Clinical Question
Should renin-angiotensin system (RAS) inhibitors be used as first-line drugs in patients with hypertension?
Evidence-Based Answer
RAS inhibitors, which include angiotensin receptor blockers, angiotensin-converting enzyme inhibitors, and renin inhibitors, should not be used as first-line agents. Patients treated with thiazide diuretics have fewer deaths related to heart failure, fewer hospitalizations from heart failure (number needed to treat [NNT] = 100), and fewer strokes (NNT = 166) than those treated with RAS inhibitors. Patients treated with RAS inhibitors have fewer deaths and hospitalizations from heart failure than those treated with calcium channel blockers (CCBs; NNT = 83), although CCBs decrease stroke risk more than RAS inhibitors (NNT = 142). Similar blood pressure control is achieved with all three classes.1 (Strength of Recommendation: B, based on inconsistent or limited-quality patient-oriented evidence.)
Practice Pointers
RAS inhibitors have been widely prescribed to treat hypertension; however, it remains unclear whether they are superior to other antihypertensive drugs in terms of clinically relevant outcomes for primary hypertension.
This Cochrane review included 45 randomized, controlled, double-blind studies involving 66,625 participants with elevated blood pressure (at least 130/85 mm Hg) and at least six months of follow-up.1 Mean duration of follow-up was 1.9 years with a range of six months to 5.6 years. The mean age of participants was 66 years and having secondary hypertension was an excluding factor. Of the 45 studies, 30 recruited patients from European countries, seven recruited from North America, and the remaining eight recruited from a combination of countries on different continents. Fifteen of the 45 studies reported ethnicity data; of these, 71% of participants were white, 23.7% were black, 1.7% were Asian, 0.3% were Hispanic, and 3.3% were “other race.” Participants with diabetes mellitus were included in 14 studies. All studies compared RAS inhibitors with other antihypertensive drug classes and reported primary outcomes of mortality and cardiovascular and renal morbidity. Secondary outcomes included degree of blood pressure control.
Moderate-certainty evidence found that, compared with thiazide diuretics, RAS inhibitors were less effective in preventing deaths or hospitalizations from heart failure and incidents of stroke. Moderate-certainty evidence also showed that RAS inhibitors and thiazides did not differ for all-cause death, total cardiovascular events, or total myocardial infarctions. When compared with CCBs, RAS inhibitors decreased deaths and hospitalizations from heart failure but were less effective in preventing strokes. [corrected] Blood pressure comparisons between patients treated with each of these classes showed no statistically significant differences. No trials reported on nonfatal serious adverse events.
This Cochrane review did not address which agent is best in patients with secondary hypertension, or with comorbidities such as diabetes. Further, it did not determine which agent should be used in those who need more than one agent. Finally, it did not address whether one class or another is best with regard to patient ethnicity, race, or age.
SUMMARY TABLE Relative Effect of Renin-Angiotensin System Inhibitors vs. Other Blood Pressure Drug Classes
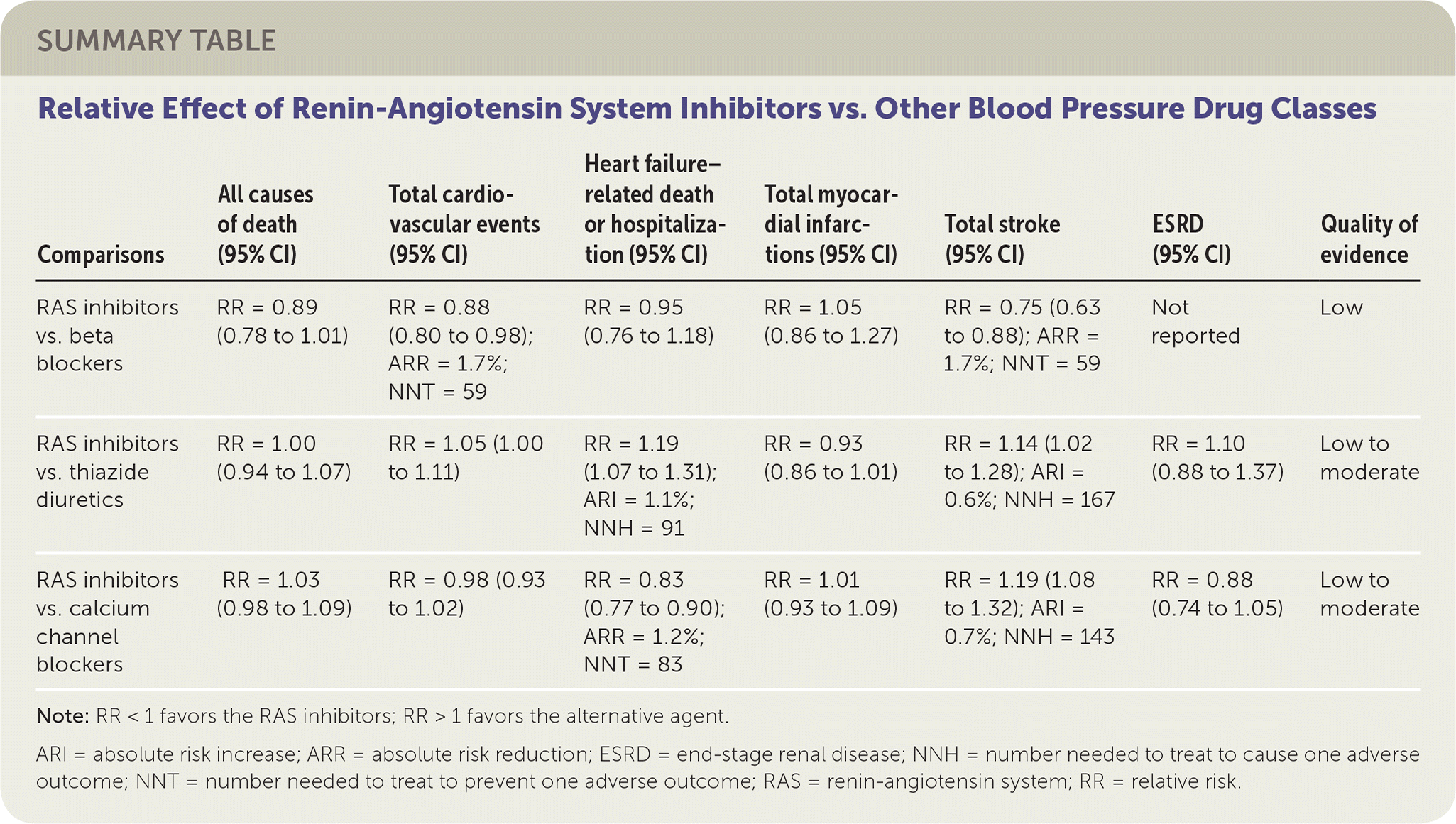
| Comparisons | All causes of death (95% CI) | Total cardiovascular events (95% CI) | Heart failure–related death or hospitalization (95% CI) | Total myocardial infarctions (95% CI) | Total stroke (95% CI) | ESRD (95% CI) | Quality of evidence |
|---|---|---|---|---|---|---|---|
| RAS inhibitors vs. beta blockers | RR = 0.89 (0.78 to 1.01) | RR = 0.88 (0.80 to 0.98); ARR = 1.7%; NNT = 59 | RR = 0.95 (0.76 to 1.18) | RR = 1.05 (0.86 to 1.27) | RR = 0.75 (0.63 to 0.88); ARR = 1.7%; NNT = 59 | Not reported | Low |
| RAS inhibitors vs. thiazide diuretics | RR = 1.00 (0.94 to 1.07) | RR = 1.05 (1.00 to 1.11) | RR = 1.19 (1.07 to 1.31); ARI = 1.1%; NNH = 91 | RR = 0.93 (0.86 to 1.01) | RR = 1.14 (1.02 to 1.28); ARI = 0.6%; NNH = 167 | RR = 1.10 (0.88 to 1.37) | Low to moderate |
| RAS inhibitors vs. calcium channel blockers | RR = 1.03 (0.98 to 1.09) | RR = 0.98 (0.93 to 1.02) | RR = 0.83 (0.77 to 0.90); ARR = 1.2%; NNT = 83 | RR = 1.01 (0.93 to 1.09) | RR = 1.19 (1.08 to 1.32); ARI = 0.7%; NNH = 143 | RR = 0.88 (0.74 to 1.05) | Low to moderate |
Note: RR < 1 favors the RAS inhibitors; RR > 1 favors the alternative agent.
ARI = absolute risk increase; ARR = absolute risk reduction; ESRD = end-stage renal disease; NNH = number needed to treat to cause one adverse outcome; NNT = number needed to treat to prevent one adverse outcome; RAS = renin-angiotensin system; RR = relative risk.
The 2017 American College of Cardiology/American Heart Association guidelines state that if a single agent is used, thiazide diuretics are considered superior, followed by CCBs and then RAS inhibitors. They also emphasize that patient comorbidities and race/ethnicity may influence pharmacologic choices (i.e., emphasizing RAS inhibitors for patients with diabetes and that black patients respond better to thiazides and CCBs than to RAS inhibitors).2 The Eighth Joint National Committee (JNC8) guidelines recommend initiating hypertension treatment in patients younger than 60 years with blood pressure readings greater than 140/90 mm Hg, and greater than 150/90 mm Hg in those 60 years and older; recommendations are further delineated by race.3 For nonblacks, JNC8 states that thiazides, CCBs, and RAS inhibitors are all appropriate first-line agents, whereas in blacks, JNC8 recommends that thiazides and CCBs be considered first-line agents.
The practice recommendations in this activity are available at http://www.cochrane.org/CD008170.
Editor's Note: The numbers needed to treat reported in this Cochrane for Clinicians were calculated by the author based on raw data provided in the original Cochrane review.
The views expressed in this article are those of the author and do not necessarily reflect the official policy or position of the Uniformed Services University of the Health Sciences, the Department of Defense, or the U.S. government.

