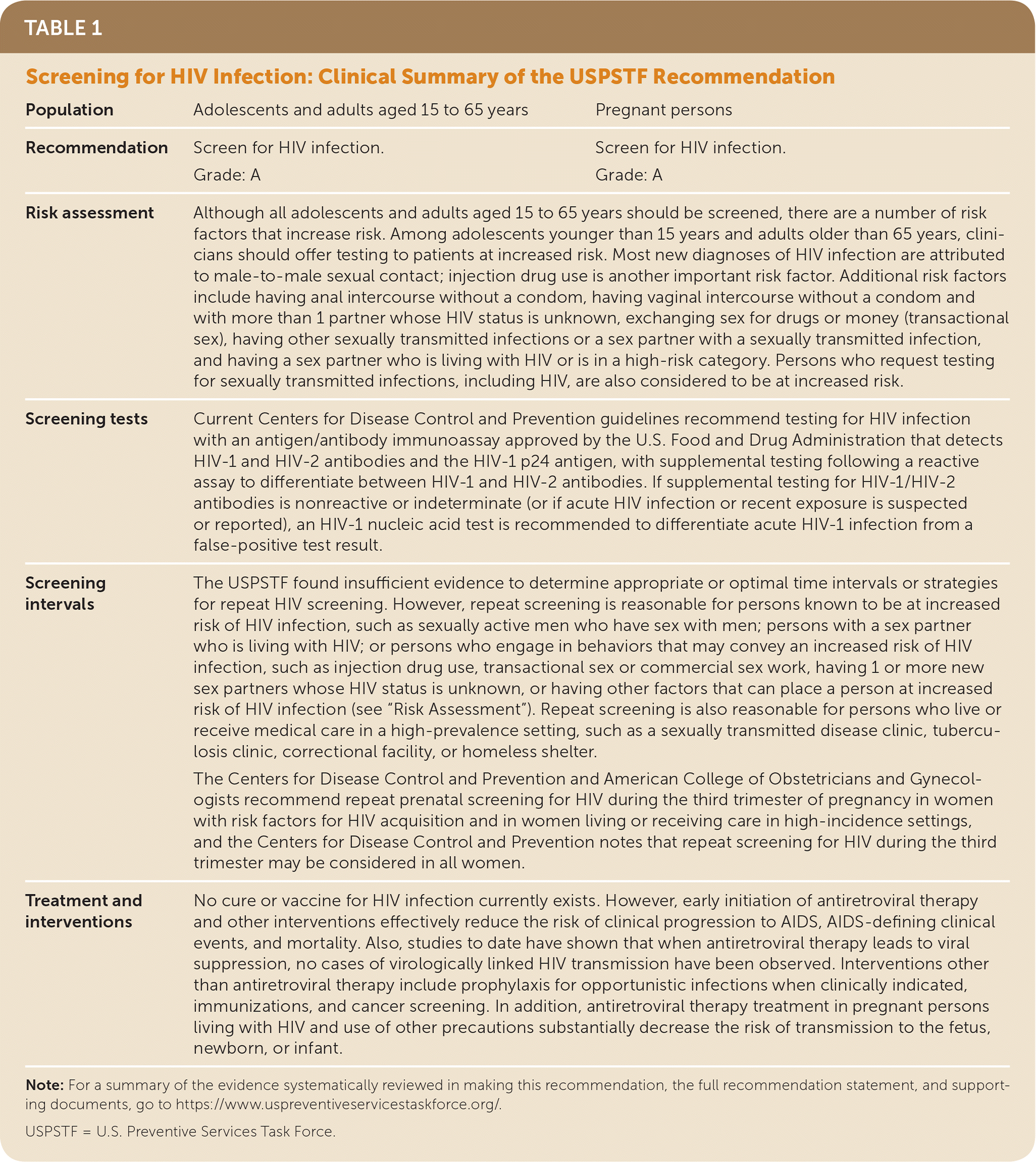
| Population | Adolescents and adults aged 15 to 65 years | Pregnant persons |
| Recommendation | Screen for HIV infection. Grade: A | Screen for HIV infection. Grade: A |
| Risk assessment | Although all adolescents and adults aged 15 to 65 years should be screened, there are a number of risk factors that increase risk. Among adolescents younger than 15 years and adults older than 65 years, clinicians should offer testing to patients at increased risk. Most new diagnoses of HIV infection are attributed to male-to-male sexual contact; injection drug use is another important risk factor. Additional risk factors include having anal intercourse without a condom, having vaginal intercourse without a condom and with more than 1 partner whose HIV status is unknown, exchanging sex for drugs or money (transactional sex), having other sexually transmitted infections or a sex partner with a sexually transmitted infection, and having a sex partner who is living with HIV or is in a high-risk category. Persons who request testing for sexually transmitted infections, including HIV, are also considered to be at increased risk. | |
| Screening tests | Current Centers for Disease Control and Prevention guidelines recommend testing for HIV infection with an antigen/antibody immunoassay approved by the U.S. Food and Drug Administration that detects HIV-1 and HIV-2 antibodies and the HIV-1 p24 antigen, with supplemental testing following a reactive assay to differentiate between HIV-1 and HIV-2 antibodies. If supplemental testing for HIV-1/HIV-2 antibodies is nonreactive or indeterminate (or if acute HIV infection or recent exposure is suspected or reported), an HIV-1 nucleic acid test is recommended to differentiate acute HIV-1 infection from a false-positive test result. | |
| Screening intervals | The USPSTF found insufficient evidence to determine appropriate or optimal time intervals or strategies for repeat HIV screening. However, repeat screening is reasonable for persons known to be at increased risk of HIV infection, such as sexually active men who have sex with men; persons with a sex partner who is living with HIV; or persons who engage in behaviors that may convey an increased risk of HIV infection, such as injection drug use, transactional sex or commercial sex work, having 1 or more new sex partners whose HIV status is unknown, or having other factors that can place a person at increased risk of HIV infection (see “Risk Assessment”). Repeat screening is also reasonable for persons who live or receive medical care in a high-prevalence setting, such as a sexually transmitted disease clinic, tuberculosis clinic, correctional facility, or homeless shelter. The Centers for Disease Control and Prevention and American College of Obstetricians and Gynecologists recommend repeat prenatal screening for HIV during the third trimester of pregnancy in women with risk factors for HIV acquisition and in women living or receiving care in high-incidence settings, and the Centers for Disease Control and Prevention notes that repeat screening for HIV during the third trimester may be considered in all women. | |
| Treatment andinterventions | No cure or vaccine for HIV infection currently exists. However, early initiation of antiretroviral therapy and other interventions effectively reduce the risk of clinical progression to AIDS, AIDS-defining clinical events, and mortality. Also, studies to date have shown that when antiretroviral therapy leads to viral suppression, no cases of virologically linked HIV transmission have been observed. Interventions other than antiretroviral therapy include prophylaxis for opportunistic infections when clinically indicated, immunizations, and cancer screening. In addition, antiretroviral therapy treatment in pregnant persons living with HIV and use of other precautions substantially decrease the risk of transmission to the fetus, newborn, or infant. | |