Concentrations of greenhouse gases continue to accumulate in the atmosphere at increasing rates, heating the Earth's surface and destabilizing climate. Health impacts from climate change may include increased morbidity and mortality from worsening cardiopulmonary health, worsening allergies, and greater risk of infectious disease and mental illness, including anxiety, depression, and posttraumatic stress disorder from extreme weather events. Family physicians should advise patients to minimize exposure to air pollution, which is potentiated by rising temperatures. Use of self-monitoring devices, tracking local weather information, and awareness of events such as wildfires can alert patients to poor ambient air quality. Vulnerable individuals should avoid intense outdoor exercise and stay indoors or wear protective N95 masks when air quality is in the harmful range. Physicians can teach patients to recognize early symptoms of heat illness and advise adequate hydration and cooling on hot days. Physicians should become aware of the signs and symptoms of vectorborne illnesses to ensure early treatment and limit spread. Physicians should be aware of the climate and health benefits of active transport and plant-based diets when counseling their patients. Physicians can have a positive impact on climate change awareness and policy by incorporating counseling, public health precepts, and advocacy into their practice.
Concentrations of greenhouse gases continue to accumulate in the atmosphere at increasing rates, pushing Earth's climate further from the stability that has persisted since humans developed civilizations.1 The health consequences of a rapidly changing, less predictable climate are expected to be substantial.
WHAT'S NEW ON THIS TOPIC
Eighteen of the past 19 years have been the warmest on record.
The five-year average melting in west Antarctica from 2012 to 2017 was three times faster than from 1992 to 1997, putting coastal cities at increasing risk of flooding, enduring inundation, and saltwater contamination of freshwater sources.
As temperate and colder regions experience shorter, warmer winters, insect vectors can expand into new regions. The Centers for Disease Control and Prevention reported a doubling of vectorborne diseases reported from 2004 to 2016.
Air pollution is associated with increased risks of coronary heart disease, myocardial infarction, and stroke, and is associated with increased emergency department visits, chronic obstructive pulmonary disease and asthma exacerbations, and development of respiratory disease.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
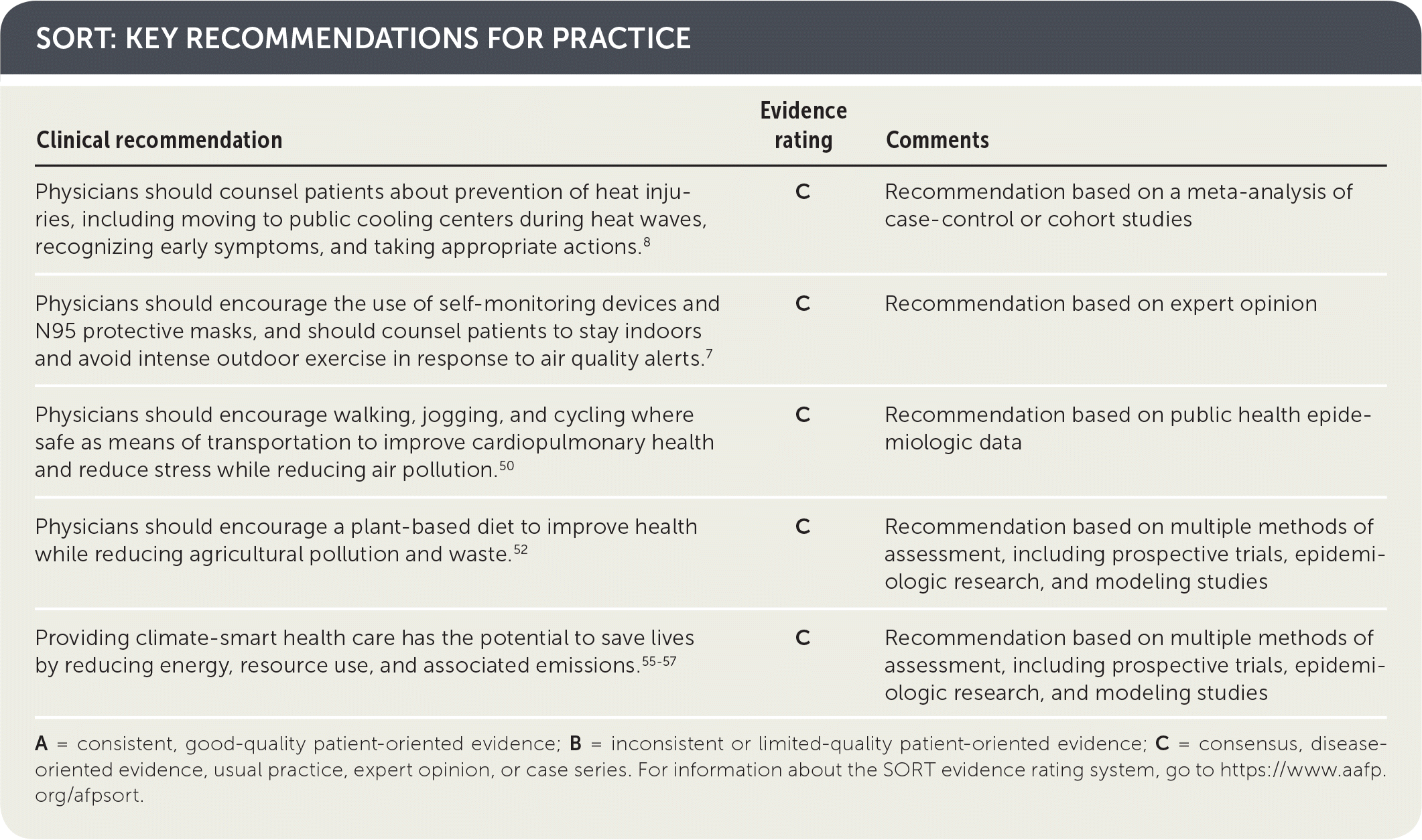
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Our understanding of climate science and projections of how the climate is changing continue to improve: 97% of active climatologists agree that the climate is changing, that human activity and the burning of fossil fuels are primarily responsible, and that the effects will be mostly negative.2 Moreover, the climate is changing faster than anticipated. For example, the five-year average melting in west Antarctica from 2012 to 2017 was three times faster than from 1992 to 1997, putting coastal cities at increasing risk of flooding, enduring inundation, and saltwater contamination of freshwater sources.3 The most worrisome effects for Americans include more frequent and severe extreme weather events such as hurricanes, floods, droughts with resulting wildfires, and heat waves (Table 11,4); worsening air pollution affecting cardiopulmonary health; and changing seasonal characteristics that increase the risk of infectious disease spread, allergies, and asthma.4
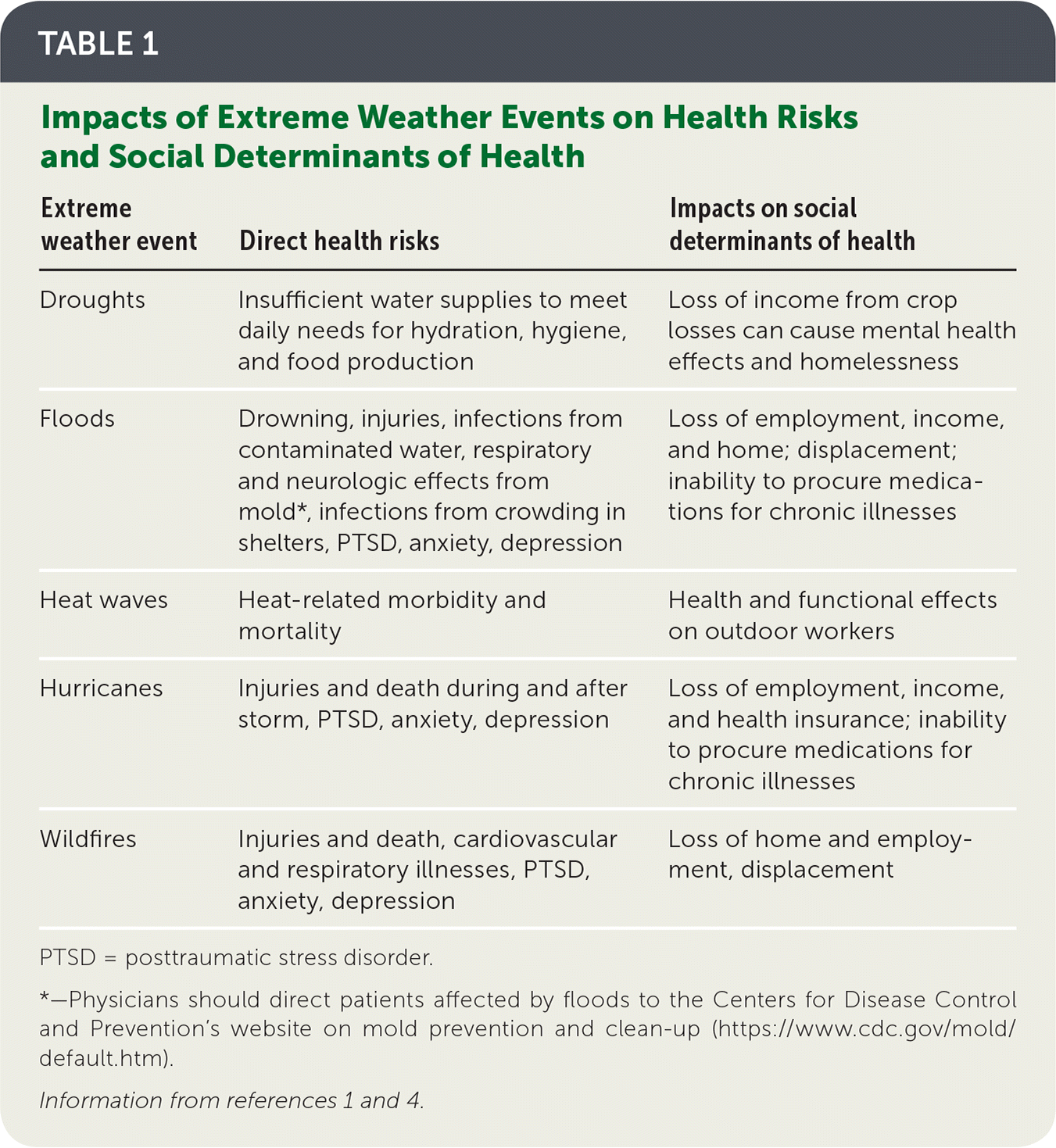
TABLE 1. Impacts of Extreme Weather Events on Health Risks and Social Determinants of Health
| Extreme weather event | Direct health risks | Impacts on social determinants of health |
|---|---|---|
| Droughts | Insufficient water supplies to meet daily needs for hydration, hygiene, and food production | Loss of income from crop losses can cause mental health effects and homelessness |
| Floods | Drowning, injuries, infections from contaminated water, respiratory and neurologic effects from mold*, infections from crowding in shelters, PTSD, anxiety, depression | Loss of employment, income, and home; displacement; inability to procure medications for chronic illnesses |
| Heat waves | Heat-related morbidity and mortality | Health and functional effects on outdoor workers |
| Hurricanes | Injuries and death during and after storm, PTSD, anxiety, depression | Loss of employment, income, and health insurance; inability to procure medications for chronic illnesses |
| Wildfires | Injuries and death, cardiovascular and respiratory illnesses, PTSD, anxiety, depression | Loss of home and employment, displacement |
PTSD = posttraumatic stress disorder.
*—Physicians should direct patients affected by floods to the Centers for Disease Control and Prevention's website on mold prevention and clean-up (https://www.cdc.gov/mold/default.htm).
Just as adapting the household environment is an essential component of asthma management, so is the need to develop climate-resilient communities and regions to provide appropriate care for patients in the setting of climate change. Family physicians have an important and timely role to counsel patients about how climate change will affect their health and what they can do about it.
Health Impacts
Climate change will have many different effects on health, specifically cardiopulmonary health, heat injuries, allergies, infectious diseases, and mental health (Table 2).1,4–17 This article reviews steps clinicians can take to lessen impacts for patients and reduce greenhouse gas emissions.
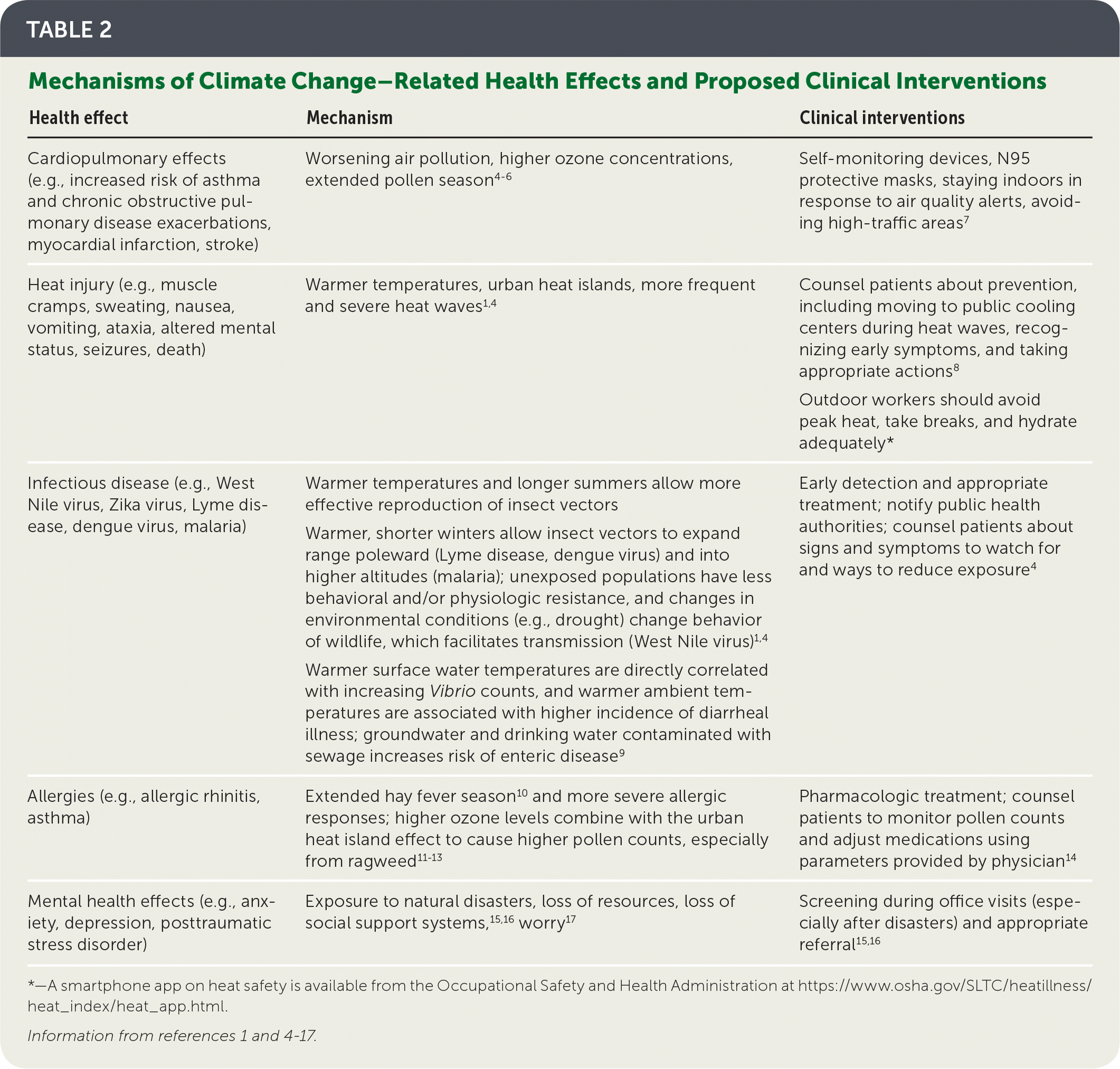
TABLE 2. Mechanisms of Climate Change–Related Health Effects and Proposed Clinical Interventions
| Health effect | Mechanism | Clinical interventions |
|---|---|---|
| Cardiopulmonary effects (e.g., increased risk of asthma and chronic obstructive pulmonary disease exacerbations, myocardial infarction, stroke) | Worsening air pollution, higher ozone concentrations, extended pollen season4–6 | Self-monitoring devices, N95 protective masks, staying indoors in response to air quality alerts, avoiding high-traffic areas7 |
| Heat injury (e.g., muscle cramps, sweating, nausea, vomiting, ataxia, altered mental status, seizures, death) | Warmer temperatures, urban heat islands, more frequent and severe heat waves1,4 | Counsel patients about prevention, including moving to public cooling centers during heat waves, recognizing early symptoms, and taking appropriate actions8 Outdoor workers should avoid peak heat, take breaks, and hydrate adequately* |
| Infectious disease (e.g., West Nile virus, Zika virus, Lyme disease, dengue virus, malaria) | Warmer temperatures and longer summers allow more effective reproduction of insect vectors Warmer, shorter winters allow insect vectors to expand range poleward (Lyme disease, dengue virus) and into higher altitudes (malaria); unexposed populations have less behavioral and/or physiologic resistance, and changes in environmental conditions (e.g., drought) change behavior of wildlife, which facilitates transmission (West Nile virus)1,4 Warmer surface water temperatures are directly correlated with increasing Vibrio counts, and warmer ambient temperatures are associated with higher incidence of diarrheal illness; groundwater and drinking water contaminated with sewage increases risk of enteric disease9 | Early detection and appropriate treatment; notify public health authorities; counsel patients about signs and symptoms to watch for and ways to reduce exposure4 |
| Allergies (e.g., allergic rhinitis, asthma) | Extended hay fever season10 and more severe allergic responses; higher ozone levels combine with the urban heat island effect to cause higher pollen counts, especially from ragweed11–13 | Pharmacologic treatment; counsel patients to monitor pollen counts and adjust medications using parameters provided by physician14 |
| Mental health effects (e.g., anxiety, depression, posttraumatic stress disorder) | Exposure to natural disasters, loss of resources, loss of social support systems,15,16 worry17 | Screening during office visits (especially after disasters) and appropriate referral15,16 |
*—A smartphone app on heat safety is available from the Occupational Safety and Health Administration at https://www.osha.gov/SLTC/heatillness/heat_index/heat_app.html.
CARDIOPULMONARY HEALTH
Climate change affects cardiopulmonary health in complex ways, mediated in large part by air pollution, which is a major cause of morbidity and mortality worldwide.18 Air pollution potentiates the effects of climate change, increasing ground-level ozone levels in hot weather, particularly in already polluted urban areas.19,20 Air pollution also drives climate change, especially through pollutants such as black carbon and methane.19,20 Climate change, in turn, affects meteorologic conditions that increasingly hamper natural clearance of pollutants through rain and wind, and expansion and severity of wildfires intensify exposure to smoke.19,20
A recent study shows an association between particle and ozone air pollution and mortality, with no lower threshold considered safe.5 Specifically, air pollution has been associated with an increased risk of coronary heart disease,21 myocardial infarction,22 and stroke,23 and is associated with increased emergency department visits, chronic obstructive pulmonary disease and asthma exacerbations, and development of respiratory disease.24 Children, older adults, people with chronic diseases, and those living in poverty are among the most vulnerable.25,26
Reducing air pollution is a recognized policy challenge.27,28 However, little is known about the effectiveness of clinical management strategies, which are typically tied to reductions in exposure. Use of self-monitoring devices, local weather information sources, and awareness of events such as wildfires can alert patients to current air quality conditions.29 People at high risk, including children, pregnant women, older adults, and those with preexisting cardiopulmonary conditions, should avoid intense outdoor exercise and stay indoors with windows closed when air quality is poor.29 N95 masks—but not ordinary surgical masks—reduce particulate inhalation and may be useful in the setting of wildfires.29,30 The AIR (ask, inform, react) mnemonic has been suggested as a potentially useful counseling tool (Table 3).7
TABLE 3. AIR Mnemonic for Patients with Pulmonary Disease

| Ask patients what they know about the effects of air pollution on their lung health |
| Inform patients about symptoms that may be related to air pollution (e.g., phlegm, shortness of breath, chest tightness) |
| React: counsel patients to monitor air quality, carry a rescue inhaler on high-risk days, limit time outdoors, and avoid intense or prolonged exertion outdoors |
Information from reference 7.
HEAT INJURY
Increasing greenhouse gas emissions are the primary reason that 18 of the 19 warmest years on record have occurred this century.31 Heat waves, which are longer than usual periods of hot days, are predicted to increase in the coming decades1 and have been associated with emergency department visits and increases in morbidity and mortality worldwide.32 Hot weather and heat waves are associated with increases in myocardial infarction,33 stroke,34 acute and chronic kidney injuries,34 cognitive function deficits, 35 and suicide.36 Heat-related illnesses were discussed in a previous issue of American Family Physician (https://www.aafp.org/afp/2019/0415/p482.html).
Use of certain medications can increase the risk of heat injury.37 Vulnerable populations include infants, outdoor workers, older adults, people with medical and psychiatric comorbidities, people living in poverty, and those without access to cooling.37 A meta-analysis found that poor physical or cognitive function and lack of social support increase the risk of heat injury, possibly because these conditions inhibit protective behaviors, such as proper hydration and relocation to cooler environments.8 However, except for air conditioning and moving to a cool place, no intervention could be clearly identified as protective against heat-related deaths, and some might have unintended adverse effects, such as hyponatremia in the case of excess hydration and falls in people seeking relief with frequent showers or baths.8
There have been few studies on individual measures to reduce vulnerability to heat.38 Suggested public health interventions include early heat warning systems and alerts, public cooling centers, and climate-smart projects to improve the environment and counteract the heat-trapping effects of urban heat islands.39
ALLERGIES
Increasing global temperatures and longer frost-free seasons allow for longer growing seasons, which lead to longer allergy seasons.10 Higher levels of carbon dioxide and associated air pollutants increase the production and allergenicity of pollen from certain highly allergenic plants, such as ragweed.11–13 Several studies have shown that when pollen counts are high, there is an increase in emergency department visits and hospitalizations for severe respiratory problems over the following two to five days, as well as an increase in outpatient visits for allergic rhinitis.14,39,40 Counseling patients to track their local pollen counts (using online monitoring sites such as https://weather.com/maps/health/allergies/treepollen and https://www.pollen.com) and providing instructions for medication changes to prevent flare-ups when pollen counts are high could potentially decrease visits and hospitalizations.14
Precipitation, humidity, and flooding, which are expected to worsen with climate change, enhance the growth of indoor mold.41 Compromised indoor air quality exposes vulnerable populations to allergens. Family physicians should counsel patients about the health benefits of preventing, identifying, and removing mold from inside their homes.41 The Centers for Disease Control and Prevention has an online resource on mold prevention and clean-up at https://www.cdc.gov/mold/default.htm.
INFECTIOUS DISEASES
Climate change can affect the spread of some infectious diseases. As temperate and colder regions experience shorter, warmer winters, insect vectors can expand into new regions, resulting in an increased incidence of illnesses such as malaria, Lyme disease, West Nile virus, Zika virus, dengue virus, and chikungunya virus.1,4 For example, Ixodes, the tick that transmits Lyme disease, expanded its range in the U.S. Northeast and Upper Midwest between 2001 and 2015.4 The Centers for Disease Control and Prevention reported a doubling of vectorborne diseases from 2004 to 2016.42 Vectorborne illnesses were discussed in a previous issue of American Family Physician (https://www.aafp.org/afp/2016/1001/p551.html).
Waterborne diarrheal diseases are also occurring more frequently, especially outside the United States, and typically involve enteric viruses, parasites, and bacteria, most notably Vibrio.4 Physicians should be familiar with the signs and symptoms of diseases involving these organisms to ensure early treatment and prevent transmission, and should stay up to date on new and emerging infectious diseases in their communities and other locales where their patients may travel.4
Prevention of insect- and waterborne diseases includes counseling patients about appropriate clothing and use of insect repellent, ensuring that household windows have screens, checking for ticks after spending time outside, and use of insect netting.43,44
MENTAL HEALTH
The mental health effects of climate change depend on the degree of exposure and perceived threat. Weather-related disasters can produce anxiety, depression, and posttraumatic stress disorder.15,16 These effects may be transient, or they can persist in people who experience significant losses as a result of the disaster and in at-risk groups, including children, people living in poverty, and first responders.15,16 Physicians should be prepared to connect patients with appropriate community resources and mental health professionals. Extrapolating from the trauma literature, psychological therapies may be particularly helpful in reducing the likelihood of posttraumatic stress disorder in children and adolescents exposed to weather-related disasters.45
Although much research has focused on the mental health effects of catastrophic events such as storms or floods, less is known about the effects from “slow” events such as droughts or rising sea levels. These events affect land use, agricultural yield, and infrastructure and can lead to interpersonal or economic stress, displacement, or other existential conditions with concomitant mental health impacts.46 However, anxiety and worry about potential impacts of climate change can be constructive and adaptive, and may support pro-environmental attitudes and actions.17 Positive engagement behaviors may serve as effective mental health interventions. A Cochrane review of studies on outdoor environmental enhancement and conservation activities found qualitative evidence for improved well-being among participants.47 Although further study is needed, the idea of local environmental interventions to enhance well-being (e.g., via social connections) suggests that engagement in community-based pro-environmental behaviors may have benefits for both health and the environment.
The Role of Physicians
The consequences of failing to stabilize the climate at a global average surface temperature below 2.5°F (1.5°C) above pre-industrial levels48 are so detrimental for human health and well-being that a compelling argument can be made that physicians have a moral obligation to educate their patients and support policies to reduce greenhouse gas emissions.49 One approach is for physicians to counsel patients on the personal and environmental benefits of transitioning to active transport (e.g., walking, jogging, bicycling) and a plant-based diet. In healthy individuals and in safe settings, active transport confers cardiopulmonary benefits, may reduce stress, and reduces ambient air pollution.50 Although recent reviews have found few health risks associated with consumption of red meat,51 diets that emphasize the intake of fruits, vegetables, nuts, and legumes (e.g., the Mediterranean diet) are associated with a multitude of health benefits while also reducing agricultural carbon dioxide emissions and waste.52,53 Although no studies have shown that emphasizing these environmental cobenefits in the clinical setting results in more significant behavioral change compared with counseling about the personal health benefits of diet and exercise alone, one ongoing study is researching the effects of incorporating behavioral counseling, mindfulness, and climate change education.54 Such studies are important for gauging patient receptivity to counseling that explicitly addresses climate change as a health concern.
The U.S. health care sector is responsible for 10% of all greenhouse gas emissions, 10% of smog formation, 12% of air pollution emissions, and smaller but significant amounts of ozone-depleting substances and other air toxicants.55 The health effects of these emissions and resource use in 2013 were equivalent to the loss of 470,000 years of healthy life (in disability-adjusted life years).55 The use of climate-smart practices in the health care sector has the potential to save lives by reducing energy and resource use, thereby safeguarding the environment, demonstrating leadership in the community, and saving money.56 Physicians can work with hospitals, the most resource-intensive institutions in the health care sector, to reduce energy use. Efforts to reduce hospital emissions, increase employees' active transportation, and educate physicians about the health impacts of air pollution were successful in one health care system.57 Multiple resources exist to assist clinicians and hospitals in providing climate-smart health care (Table 4).
TABLE 4. Climate Change Actions and Resources for Health Care Professionals
| Actions | Resources |
|---|---|
| Encourage the facilities where you work to lead by example by adopting measures to reduce their carbon footprint | Health Care Without Harm (https://noharm-uscanada.org/content/us-canada/join-our-physician-network) |
| My Green Doctor (https://www.mygreendoctor.org) | |
| Encourage professional associations to explore and address the issue of climate change and the role the health care sector has in mitigation | American Academy of Family Physicians position statement on environmental health and climate change (https://www.aafp.org/about/policies/all/climate-pollution.html) |
| American Academy of Pediatrics policy statement on global climate change and children's health (http://pediatrics.aappublications.org/content/136/5/992) | |
| The American College of Emergency Physicians policy statement on climate change and public health (http://bit.ly/2JoqJoi) | |
| Additional associations with policy statements: American Academy of Dermatology (http://bit.ly/2J5J5uS) American College of Physicians (http://bit.ly/2HaCLyK) American College of Preventive Medicine (http://bit.ly/31z8hik) American Congress of Obstetricians and Gynecologists (http://bit.ly/2ZZDsnb) American Medical Association (http://bit.ly/2WtLUJt) American Psychiatric Association (http://bit.ly/35Wg11i) American Thoracic Society (http://bit.ly/33Q26I7) National Medical Association (http://bit.ly/2YfGXUZ) | |
| Work with professional associations and teaching institutions to make climate literacy a mandatory requirement for all clinical education programs | Global Consortium on Climate and Health Education (http://bit.ly/2DUF9sK) |
| Medical Society Consortium on Climate and Health (https://medsocietiesforclimatehealth.org) | |
| Become an informed advocate for climate mitigation and adaptation efforts | Many professional and evidence-based advocacy organizations are providing useful information, such as the American Academy of Family Physicians, American Public Health Association, and Physicians for Social Responsibility |
| Set an example: do your part to understand and minimize your own carbon footprint | Carbon footprint calculators are available at: http://bit.ly/2Wsi9Zb https://www3.epa.gov/carbon-footprint-calculator https://www.conservation.org/act/carboncalculator/calculate-your-carbon-footprint.aspx |
Physicians also have an important role as advocates. The American Academy of Family Physicians recognizes “serious adverse health consequences resulting from pollution, greenhouse gas emissions from human activities, climate change and ozone layer depletion,” and recommends “strong action on the part of all public and private institutions to reduce pollution of our land, atmosphere, and water.”58 Physicians can strengthen and support public health and community initiatives (e.g., heat wave warning systems) by increasing public awareness and helping patients locate community-based resources (Table 5). Clear disaster preparedness guidelines are emerging for patients with chronic diseases. Physicians can assist patients with planning and preparedness activities for likely disasters, such as possible early evacuation, procurement of supplies of critical medication and equipment, and arrangements to receive critical treatments outside of the disaster area59,60 (Table 659–63 ). Advocacy tools that are broadly applicable to other physician concerns are also useful for taking action to combat the health impacts of climate change.64
TABLE 5. Public Health Resources for Natural Disasters
| Preparedness | Emergency responders |
| CDC natural disasters and severe weather resource: https://www.cdc.gov/disasters/index.html CDC disaster preparedness educational materials for people with chronic diseases: https://www.cdc.gov/disasters/hurricanes/educationalmaterials.html EPA: https://www.epa.gov/natural-disasters Federal Emergency Management Agency climate change resource: https://www.fema.gov/climate-change National Center for Disaster Preparedness: https://ncdp.columbia.edu U.S. Department of Homeland Security disaster preparedness resource: https://www.ready.gov WHO resource on preventing heat-related illness: http://www.euro.who.int/__data/assets/pdf_file/0007/147265/Heat_information_sheet.pdf | National Institute for Occupational Safety and Health emergency response resources: https://www.cdc.gov/niosh/topics/emres/natural.html OSHA hurricane preparedness and response resource: https://www.osha.gov/dts/weather/hurricane/index.html OSHA indoor air quality resource: https://www.osha.gov/SLTC/indoorairquality/index.html OSHA occupational heat exposure resource: https://www.osha.gov/SLTC/heatstress OSHA wildfire resource: https://www.osha.gov/dts/wildfires/index.html |
| Public health organizations | |
| American Public Health Association: https://www.apha.org/topics-and-issues/climate-change CDC: https://www.cdc.gov/climateandhealth Center for Climate Change and Health: http://climatehealthconnect.org National Institute of Environmental Health Sciences: https://www.niehs.nih.gov/research/programs/geh/climatechange/index.cfm U.S. Global Change Research Program: https://www.globalchange.gov WHO: http://www.who.int/health-topics/climate-change | |
| Building resiliency | |
| APA resource for flood victims: http://www.apa.org/helpcenter/flood-distress.aspx APA resource for hurricane victims: https://www.apa.org/helpcenter/hurricane-stress.aspx EPA Climate Change Adaptation Resource Center: https://www.epa.gov/arc-x EPA resource on climate change and heat islands: https://www.epa.gov/heat-islands/climate-change-and-heat-islands EPA resource on indoor air quality: https://www.epa.gov/indoor-air-quality-iaq/adapting-buildings-indoor-air-quality-changing-climate Indiana University Environmental Resilience Institute: https://eri.iu.edu/erit/implications/public-health.html Substance Abuse and Mental Health Services Administration disaster behavioral health resources: https://www.samhsa.gov/dtac/disaster-behavioral-health-resources U.S. Climate Resilience Toolkit: https://toolkit.climate.gov | |
| Health care resources | |
| CDC mold prevention and clean-up resource: https://www.cdc.gov/mold/default.htm Climate for Health: http://climateforhealth.org Health Care Without Harm: https://noharm.org National Association of County and City Health Officials climate change resource: https://www.naccho.org/programs/environmental-health/hazards/climate-change Practice Greenhealth: https://practicegreenhealth.org |
APA = American Psychological Association; CDC = Centers for Disease Control and Prevention; EPA = U.S. Environmental Protection Agency; OSHA = Occupational Safety and Health Administration; WHO = World Health Organization.
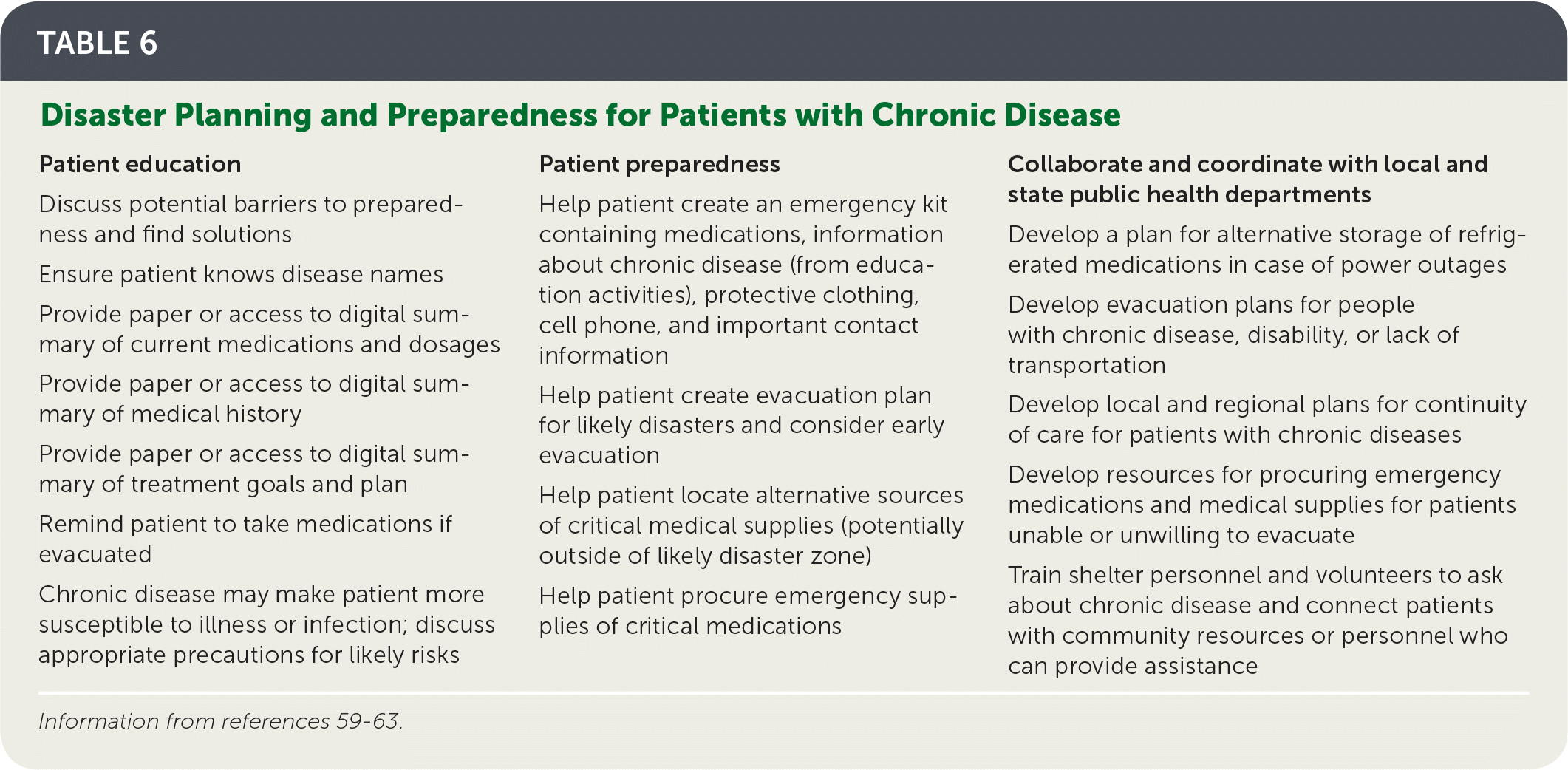
TABLE 6. Disaster Planning and Preparedness for Patients with Chronic Disease
| Patient education | Patient preparedness | Collaborate and coordinate with local and state public health departments |
|---|---|---|
| Discuss potential barriers to preparedness and find solutions Ensure patient knows disease names Provide paper or access to digital summary of current medications and dosages Provide paper or access to digital summary of medical history Provide paper or access to digital summary of treatment goals and plan Remind patient to take medications if evacuated Chronic disease may make patient more susceptible to illness or infection; discuss appropriate precautions for likely risks | Help patient create an emergency kit containing medications, information about chronic disease (from education activities), protective clothing, cell phone, and important contact information Help patient create evacuation plan for likely disasters and consider early evacuation Help patient locate alternative sources of critical medical supplies (potentially outside of likely disaster zone) Help patient procure emergency supplies of critical medications | Develop a plan for alternative storage of refrigerated medications in case of power outages Develop evacuation plans for people with chronic disease, disability, or lack of transportation Develop local and regional plans for continuity of care for patients with chronic diseases Develop resources for procuring emergency medications and medical supplies for patients unable or unwilling to evacuate Train shelter personnel and volunteers to ask about chronic disease and connect patients with community resources or personnel who can provide assistance |
Data Sources: A PubMed search was completed in Clinical Queries using the key terms climate change AND asthma, allergies, vector-borne disease, air pollution, mental health, psychological impacts, disaster psychology, and psychological adaptation. The search included meta-analyses, clinical trials, original research on mechanisms, and reviews. Also searched were UpToDate, OVID, and the Cochrane database. Search dates: June 17, 2018, and March 11, 2019.
Editor's Note: Dr. Wellbery is associate deputy editor of American Family Physician.

