Clinical Question
Do general health checks in adults reduce illness and death?
Evidence-Based Answer
General health check visits have no benefit on cardiovascular morbidity or on total, cardiovascular, or cancer-related mortality. There is also no evidence that they cause patient harm.1 (Strength of Recommendation: A, based on consistent, good-quality patient-oriented evidence.)
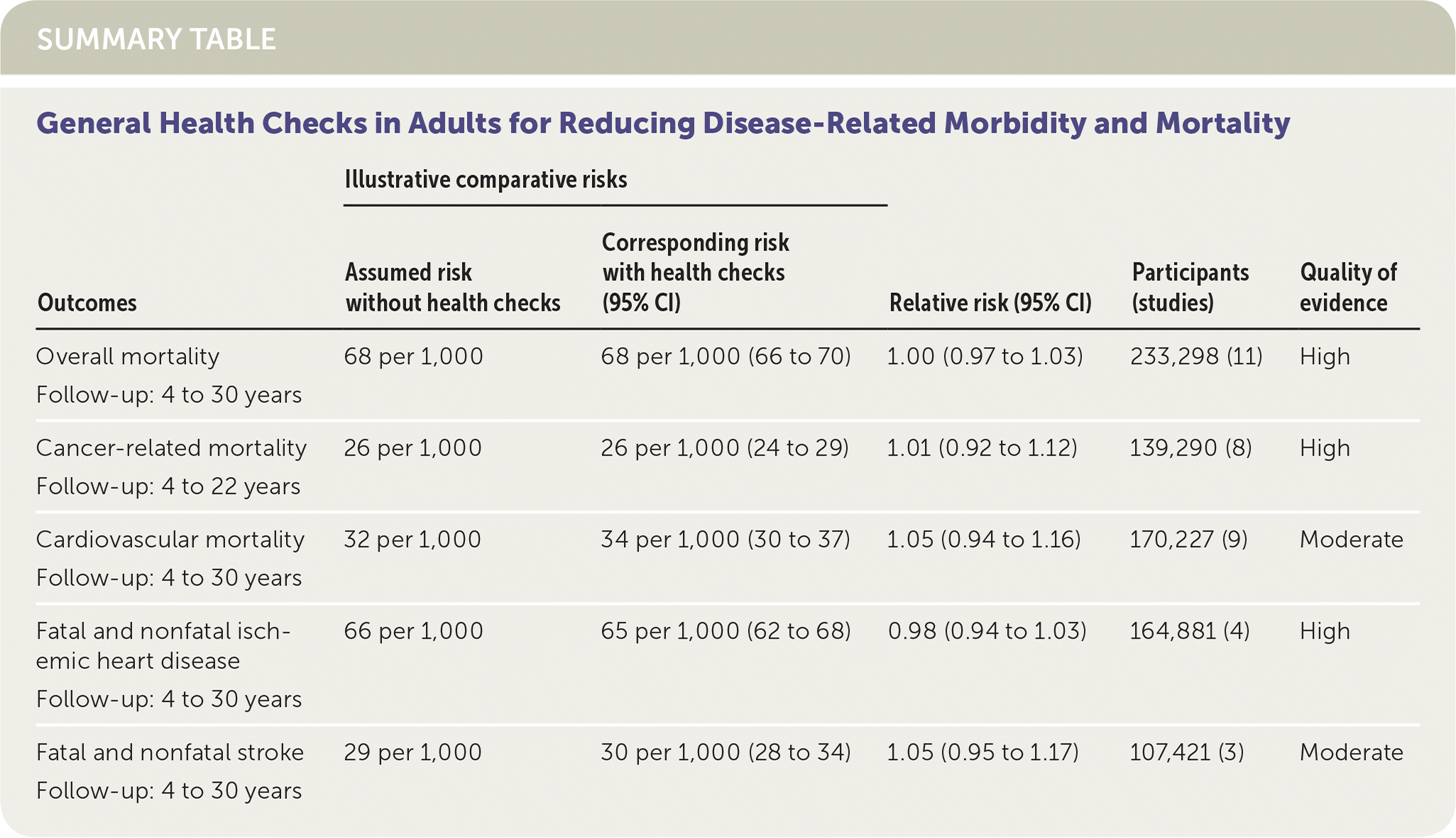
SUMMARY TABLE General Health Checks in Adults for Reducing Disease-Related Morbidity and Mortality
| Outcomes | Illustrative comparative risks | Relative risk (95% CI) | Participants (studies) | Quality of evidence | |
|---|---|---|---|---|---|
| Assumed risk without health checks | Corresponding risk with health checks (95% CI) | ||||
| Overall mortality Follow-up: 4 to 30 years | 68 per 1,000 | 68 per 1,000 (66 to 70) | 1.00 (0.97 to 1.03) | 233,298 (11) | High |
| Cancer-related mortality Follow-up: 4 to 22 years | 26 per 1,000 | 26 per 1,000 (24 to 29) | 1.01 (0.92 to 1.12) | 139,290 (8) | High |
| Cardiovascular mortality Follow-up: 4 to 30 years | 32 per 1,000 | 34 per 1,000 (30 to 37) | 1.05 (0.94 to 1.16) | 170,227 (9) | Moderate |
| Fatal and nonfatal ischemic heart disease Follow-up: 4 to 30 years | 66 per 1,000 | 65 per 1,000 (62 to 68) | 0.98 (0.94 to 1.03) | 164,881 (4) | High |
| Fatal and nonfatal stroke Follow-up: 4 to 30 years | 29 per 1,000 | 30 per 1,000 (28 to 34) | 1.05 (0.95 to 1.17) | 107,421 (3) | Moderate |
Practice Pointers
General health checks for adults 18 to 64 years of age are designed to identify patients at risk of certain diseases. The goal is early detection and prevention of associated adverse outcomes, although with screening there is always the risk of overdiagnosis. This Cochrane review was designed to evaluate the morbidity and mortality benefits and risks associated with general health checks.
This review involved 15 trials that evaluated outcomes for 251,891 patients.1 Studies included interventions such as screening for more than one disease (or risk factor) or a lifestyle intervention in more than one organ system, performed by any health care professional. In each of the studies, the control consisted of either no screenings or lifestyle interventions. Five of the study settings were in general practice, nine were in medical/research centers, and one was in the workplace. Trials were excluded if participants were 65 years and older, or if they included participants with known diseases or risk factors. Overall, the trials were judged to be at low risk of selection and allocation bias; some studies were judged to have moderate to high risk of attrition bias and outcome detection. Harms of the intervention were not reported but potentially include worry, excessive follow-up testing, and harm from subsequent treatment.
Several different outcomes of general health checks were reported; 11 trials with 233,298 participants evaluated mortality, and the authors found no significant difference between the control and intervention groups. When the authors evaluated the impact of general health checks on cancer-related mortality, they found eight trials that demonstrated no benefit vs. control. The authors could also find no demonstrable difference in cardiovascular mortality (studied in nine trials, with varying definitions, including coronary artery disease or ischemic heart disease plus stroke) between patients undergoing general health checks and those in control groups. Further data analysis demonstrated no difference between patients evaluated with health checks and those who were not with regard to the outcomes of fatal/ nonfatal ischemic heart disease (four trials) and combined fatal/nonfatal stroke (three trials).
It is reasonable to conclude that inviting an unselected population for general health checks does not reduce illness or death. Potential reasons for finding no benefit with the studied outcomes include the possibility that people who respond to an invitation for a general health check may be more health conscious at baseline, as well as the likelihood that physicians often incorporate screening into office visits for other reasons (i.e., ordering cholesterol screening for an at-risk patient who presents with infectious symptoms).
Although no U.S. guidelines currently recommend a general health check, the U.K.'s National Health Service recommends a health check in 40- to 74-year-olds to prevent heart disease, stroke, type 2 diabetes mellitus, and kidney disease, and to raise awareness of dementia.2 Medicare patients in the United States are covered for an annual wellness visit, which is a visit to develop or update a personalized prevention plan and to perform a health risk assessment.3 Physicians should continue to use all opportunities to address disease and risk factor screening and education.
The practice recommendations in this activity are available at http://www.cochrane.org/CD009009.
The views expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Department of the Navy, the Department of Defense, or the U.S. government.
We are military service members. This work was prepared as part of our official duties. Title 17 U.S.C. 105 provides that “Copyright protection under this title is not available for any work of the United States Government.” Title 17 U.S.C. 101 defines U.S. government work as a work prepared by a military service member or employee of the U.S. government as part of that person's official duties.
Editor's Note: Although not mentioned in the practice pointers, it is worth noting that the most recent study in this review was from 1999, and all but two were published more than 25 years ago. Also, the conclusions in this meta-analysis are based largely on studies done outside of the United States/Canada. As these studies predate most modern clinical preventive service recommendations (cancer screening, lipid management, chemoprevention, behavioral counseling, screening for depression and alcohol use, etc), the evidence of this review has limited applicability to current primary care settings. We should continue evidence-based preventive services irrespective of these findings.-Corey Fogleman, MD, AFP Assistant Medical Editor

