A 20-year-old woman presented with one week of fever and throat pain. She reported progressive difficulty in swallowing and had been unable to eat or drink for 48 hours. She did not have cough, rashes, or recent sick contacts. She was otherwise healthy with no pertinent medical conditions.
On physical examination, the patient had a temperature of 103°F (39.4°C) and bilateral tender anterior cervical lymphadenopathy. Oral examination revealed vesicular lesions over the soft palate and uvula, erythema of the posterior oropharynx, and tonsillar hypertrophy without exudate (Figure 1).
FIGURE 1
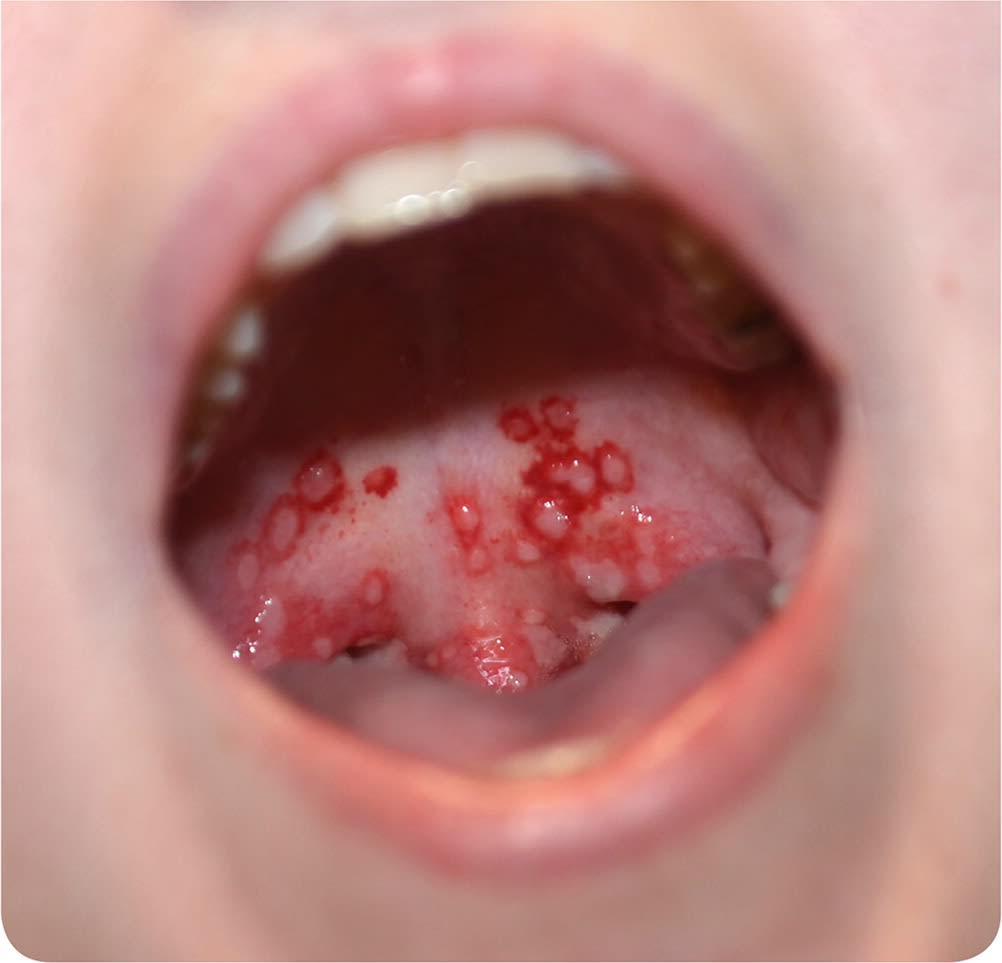
Question
Based on the patient's history and physical examination findings, which one of the following is the most appropriate treatment option?
A. Dexamethasone.
B. Observation.
C. Oral acyclovir.
D. Intravenous acyclovir.
E. Penicillin V potassium.
Discussion
The correct answer is D: intravenous acyclovir. Based on the history and examination findings, the patient was diagnosed with primary herpes simplex virus type 2 (HSV-2) infection. Traditionally, HSV-1 is implicated in oral and pharyngeal infections, and HSV-2 is implicated in genitoanal infections; however, these patterns have been blurred by evolving sexual practices.1 When HSV infection is suspected, polymerase chain reaction testing or viral culture of vesicular fluid and serum immunoglobulin G and M assays can aid in characterization. Testing for other sexually transmitted infections may also be indicated. The precise incidence of primary HSV pharyngitis is not well documented; however, a study of 613 college students with acute pharyngitis demonstrated a 5.7% prevalence of HSV, with all but two cases identified as HSV-1.2
Typically, primary HSV infections begin with a prodrome of nonspecific symptoms, including fever, headache, malaise, nausea, vomiting, and/or lymphadenopathy, with accompanying oropharyngeal erythema or petechiae, followed by the development of vesicles.1,3 This is in contrast to the prodrome of secondary (or reactivation) HSV, which is characterized by pain, pruritus, or burning, often in a previously affected distribution. 3 Given the nonspecific prodrome of primary HSV pharyngitis and its symptom overlap with group A beta-hemolytic streptococcal pharyngitis, misdiagnosis during the early stages is possible.
Antiviral therapy is indicated in patients with primary HSV-2 infection who present within 48 hours of vesicle eruption. Antivirals, such as acyclovir, are known to accelerate healing of lesions and reduce pain, fever, and viral shedding.1,3 Intravenous acyclovir is indicated when a patient has severe symptoms, regardless of duration, or is unable to take oral medications. Transition to oral acyclovir is indicated once there is sufficient mucosal healing and symptom control to allow for oral administration.
Whether dexamethasone is beneficial in patients with acute pharyngitis is controversial, even though corticosteroids are often prescribed for symptoms related to upper respiratory infections.4 Although corticosteroids may decrease overall severity and duration of pain, they do not significantly improve absenteeism from work or school or reduce analgesic use.5,6
Observation is not appropriate for patients with severe symptoms due to suspected HSV pharyngitis but may be appropriate for uncomplicated cases of acute pharyngitis.2
Penicillin V potassium is the preferred treatment for group A beta-hemolytic streptococcal pharyngitis but is not indicated for viral pharyngitis. Penicillin is recommended only for patients at high risk of group A beta-hemolytic streptococcal pharyngitis.7
We are military service members. This work was prepared as part of our official duties. Title 17 U.S.C. 105 provides that “Copyright protection under this title is not available for any work of the United States Government.” Title 17 U.S.C. 101 defines U.S. government work as a work prepared by a military service member or employee of the U.S. government as part of that person's official duties.
The views expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Department of the Navy, Department of Defense, or the U.S. government.

