In 2018, two-thirds of primary care physicians in Puerto Rico were older than 55 years, compared with 43% nationwide. Meanwhile, only four out of every 10 graduates of family medicine residencies from 2011 to 2017 remained on the island in 2018, placing Puerto Rico’s new family physician retention rate among the lowest in the nation.
In the fall of 2017, Category 4 Hurricane Maria caused widespread damage in Puerto Rico. The territory has been plagued by a fleeing workforce since then, including many health care professionals who are integral to Puerto Rico’s recovery.1 Meanwhile, Puerto Rico has experienced political instability,2 and its health care system has also faced uncertainty as its 100% federal match rate for Medicaid funding was expected to expire in December 2019, alongside the temporary federal funding continuing resolution, potentially prompting severe budget cuts.3 Bills to permanently sustain funding were introduced in the U.S. House of Representatives and Senate in July 2019 but have not reached the floor vote stages.4,5
Our study presents updated data for Puerto Rico’s primary care workforce. The findings indicate that the primary care physician (PCP) workforce in Puerto Rico is aging and leaving the island more rapidly than they are being replaced.
Data for physicians in direct patient care come from the 2018 American Medical Association (AMA) Physician Masterfile, which we matched to residency information from the 2017 and 2018 AMA Historical License and Residency files.6 We supplemented osteopathic physicians using the 2016 Centers for Medicare and Medicaid Services (CMS) National Plan and Provider Enumeration System and 2016 CMS Physician Compare; identified hospitalists using 2016 CMS Provider Utilization and Payment Data; and estimated and corrected physician retirement not captured in the AMA Physician Masterfile.7–10 We identified primary care physicians as those with the self-reported specialty of family medicine, general internal medicine, general pediatrics, or general practice. We used family physicians as our study population for resident retention because internal medicine and pediatric trainees are more likely to subspecialize, thus their migration after residency can be directed by further training and not necessarily where they will practice.11
Between 2011 and 2017, Puerto Rico trained 111 family medicine residents among its four residency programs. Of those 111 graduates, only 45 were practicing on the island in 2018, a retention rate of 40.5%. Of family medicine residency graduates across the United States graduating between 2011 and 2017, only five new graduates of residency programs outside of Puerto Rico went to the island to practice. This is substantially lower than the national state-level average of 155 new graduates entering from out of state. Overall, Puerto Rico experienced a total retention and recruitment rate of only 45% (50 out of 111) of the family medicine residents it trained, the lowest rate in the nation (the next lowest was in the District of Columbia, which had a total retention and recruitment rate of 57.8%).
Meanwhile, in 2018, the median age of PCPs in Puerto Rico was 60 years, compared with 53 years nationally. The median age of family physicians in Puerto Rico was 57 years, compared with 52 years nationally. Of Puerto Rico’s PCP workforce, 66% are older than 55 years, which is much higher than the national average of 43%. The age distribution of PCPs skews much older in Puerto Rico compared with the rest of the United States (Figure 1).6–10
FIGURE 1.
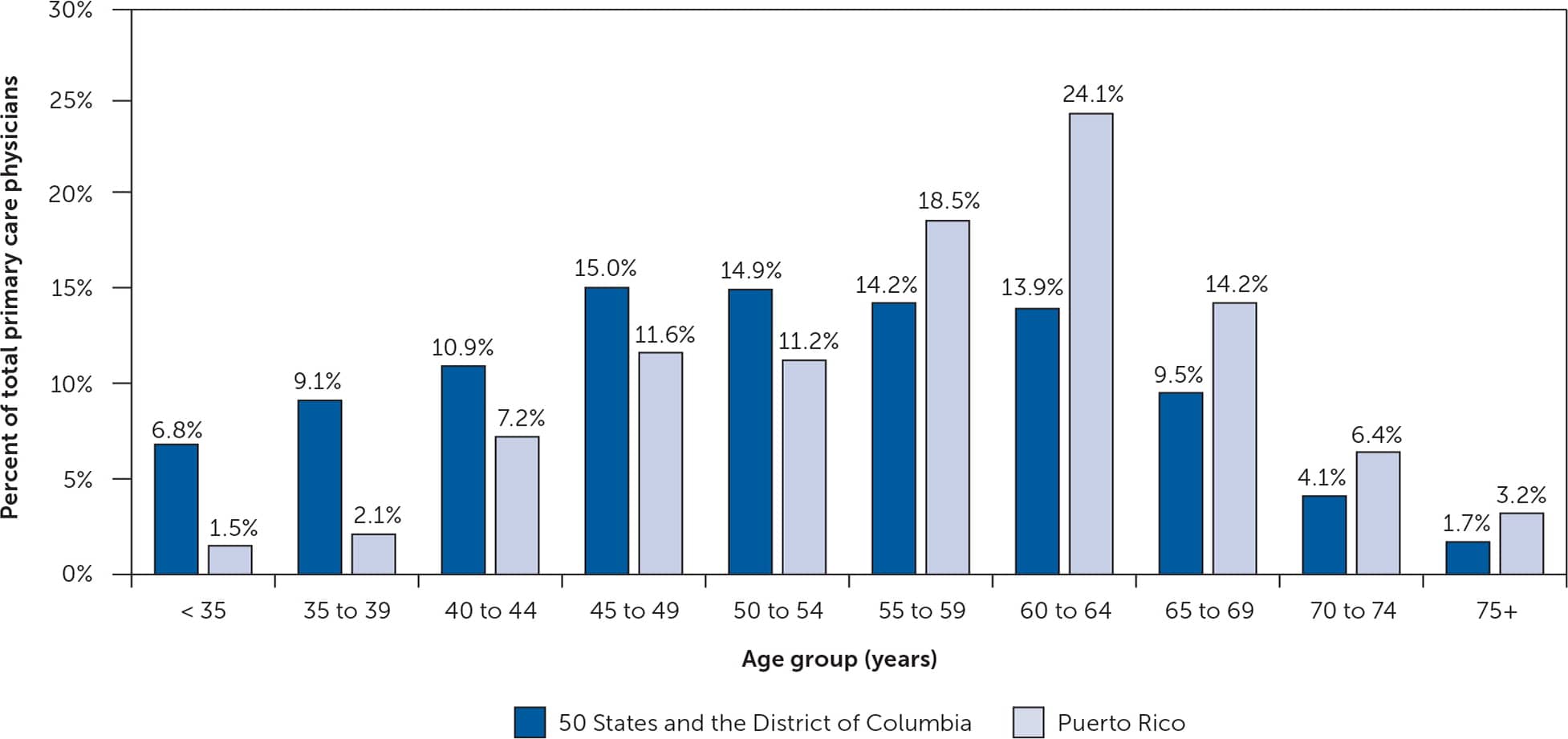
Primary care physician age distribution in Puerto Rico compared with the rest of the United States in 2018.
Puerto Rico is not attracting and retaining enough family physician trainees to replace its aging PCP workforce. Interventions to encourage family physicians to stay or migrate to Puerto Rico are necessary to address the escalating health care needs of the island. This includes funding to sustain an adequate health care infrastructure and to incentivize retention of physicians.

