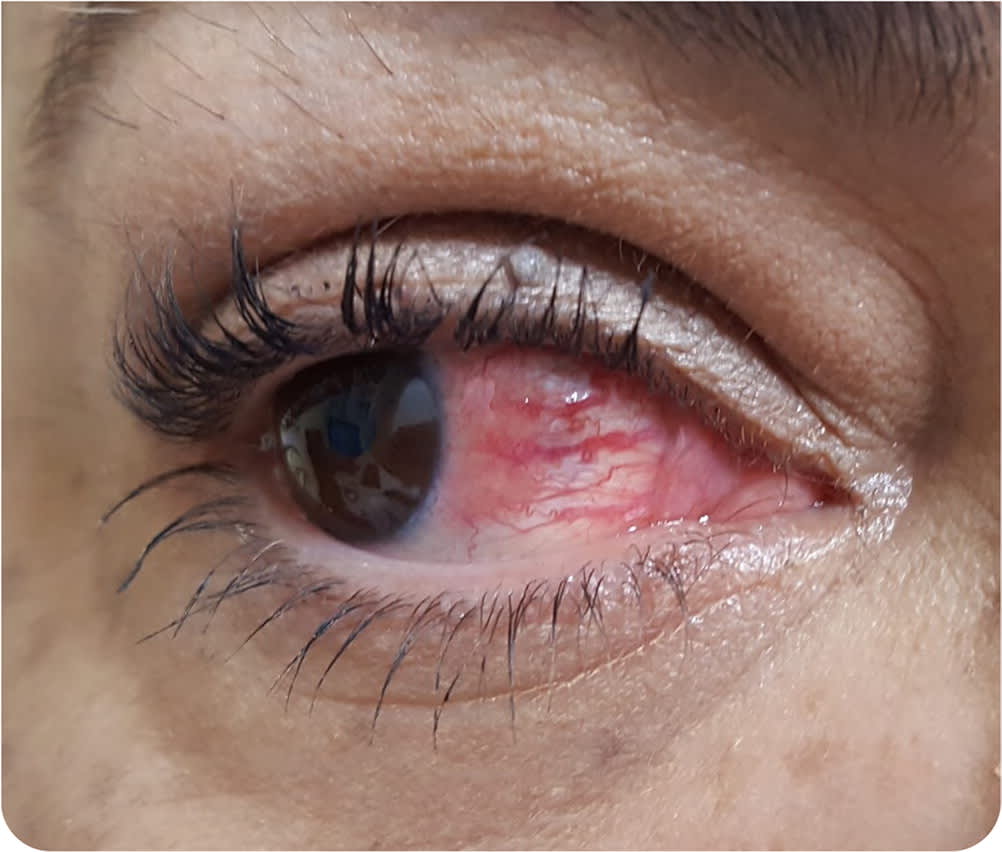
A 55-year-old woman presented with redness and pain in her right eye that had been present for one month (Figure 1). The pain began with a popping sensation, and the redness developed the next day. The pain was achy, located around the eye, and associated with watery discharge but no vision changes. One month earlier, she experienced mild achiness in her upper and lower extremities. She did not have fever, shortness of breath, skin rash, or other symptoms.
FIGURE 1
She had a history of hypertension, type 2 diabetes mellitus, mild nonproliferative diabetic retinopathy, bilateral glaucoma for which she had surgery three months earlier, and asthma. She was a former smoker. Her family history was positive for lupus erythematosus and rheumatoid arthritis
Physical examination revealed normal vital signs, upper and lower eyelids that were mildly tender to palpation, normal conjunctiva, and edema of the episcleral tissues and localized hyperemia of superficial episcleral vessels that were associated with nodular formation and clear discharge.
Question
Based on the patient’s history and physical examination findings, which one of the following is the most likely diagnosis?
A. Conjunctivitis.
B. Episcleritis.
C. Herpetic keratitis.
D. Scleritis.
E. Uveitis.
Discussion
The answer is B: episcleritis. Episcleritis is an acute, benign inflammation of the episclera, the thin vascular layer under the conjunctiva and superficial to the sclera. It presents as redness, discomfort, irritation, and watering of the eyes with preserved vision. It affects young or middle-aged women in 70% of cases.1,2 Episcleritis has simple and nodular forms. Less than one-third of cases are associated with systemic or inflammatory diseases.
Physical examination of patients with episcleritis may reveal local or diffuse dilatation of the episcleral vessels. Most cases are self-limited and resolve in two to three weeks.3 Severe symptoms may require nonsteroidal anti-inflammatory drugs or steroid eye drops.3 If episodes recur or the patient has symptoms of systemic illness, a workup should be performed to rule out rheumatoid arthritis, systemic lupus erythematosus, vasculitis, inflammatory bowel disease, or infectious diseases such as herpes or Lyme disease. It is important to differentiate benign episcleritis (no vision changes) from scleritis, which causes vision impairment and requires early aggressive treatment.2 This patient’s workup was positive for Lyme disease.
Conjunctivitis is the most common cause of red eye and is usually a result of bacterial infection, viral infection, or allergies. Conjunctivitis presents as morning crusting and daytime discharge. Physical examination shows diffuse erythema of bulbar and palpebral conjunctiva.
Herpetic keratitis is caused by the herpes simplex virus (HSV). It presents as acute onset of pain, watery discharge, and blurred vision. HSV 1 and 2 can be transmitted through hand-eye contact from primary oral or genital lesions. HSV has high prevalence in the United States and may cause corneal blindness.4
Scleritis causes red eye associated with intense ocular pain, photophobia, and vision impairment that can lead to vision loss. More than 50% of cases are associated with systemic inflammatory diseases.5 Scleritis is caused by severe ocular inflammation.6
Uveitis is inflammation of the uvea that can damage the vascular portion of the eye leading to permanent vision loss. It can be acute, recurrent, or chronic. Uveitis presents as decreased vision, floaters, eye pain, and photophobia. It is caused by infections or systemic inflammatory diseases.5
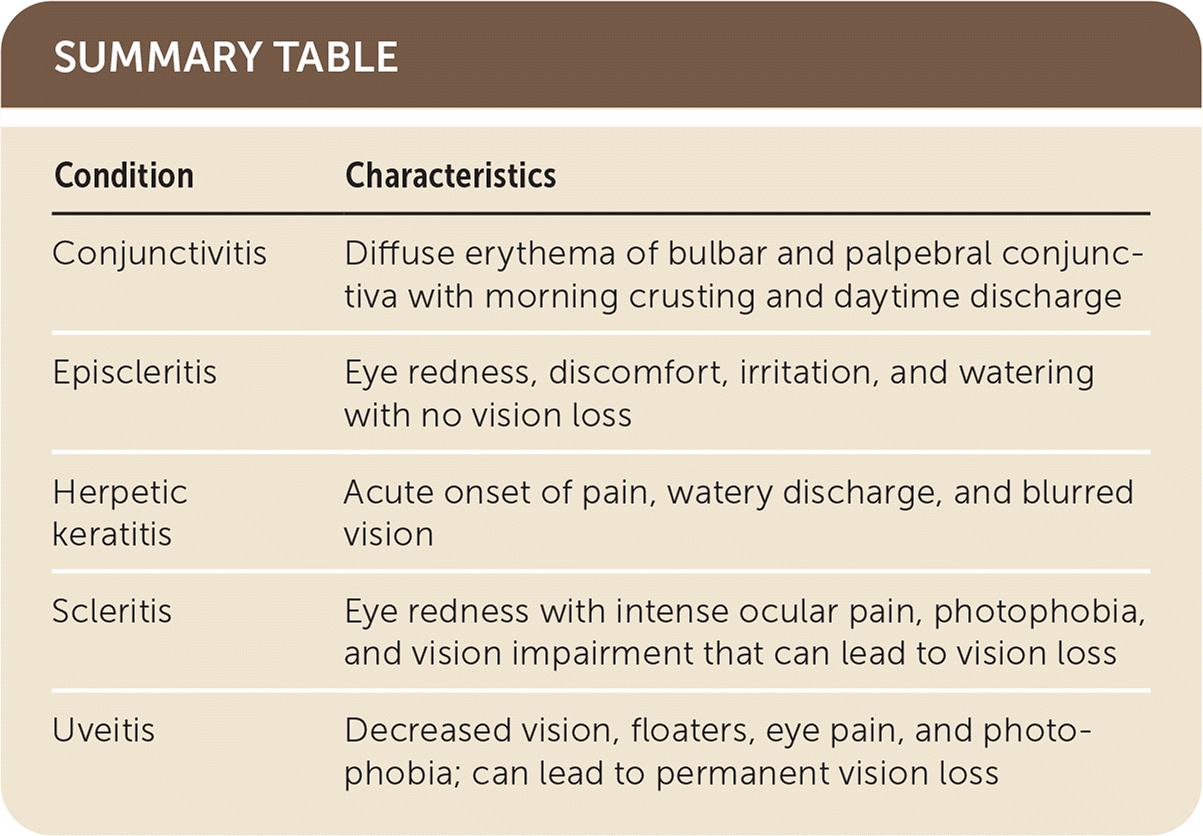
SUMMARY TABLE
| Condition | Characteristics |
|---|---|
| Conjunctivitis | Diffuse erythema of bulbar and palpebral conjunctiva with morning crusting and daytime discharge |
| Episcleritis | Eye redness, discomfort, irritation, and watering with no vision loss |
| Herpetic keratitis | Acute onset of pain, watery discharge, and blurred vision |
| Scleritis | Eye redness with intense ocular pain, photophobia, and vision impairment that can lead to vision loss |
| Uveitis | Decreased vision, floaters, eye pain, and photophobia; can lead to permanent vision loss |


