
Am Fam Physician. 2020;102(3):181-182
Author disclosure: No relevant financial affiliations.
A 45-year-old woman with a 10-year history of primary adrenal insufficiency was admitted to the hospital for treatment of pyelonephritis caused by Escherichia coli infection, for which she was given intravenous antibiotics and fluids.
On physical examination, her heart rate was 120 beats per minute, and her blood pressure was 90/58 mm Hg. Oral examination revealed hyperpigmentation of her tongue, the vermilion border of her lips, and the buccal mucosa (Figure 1).
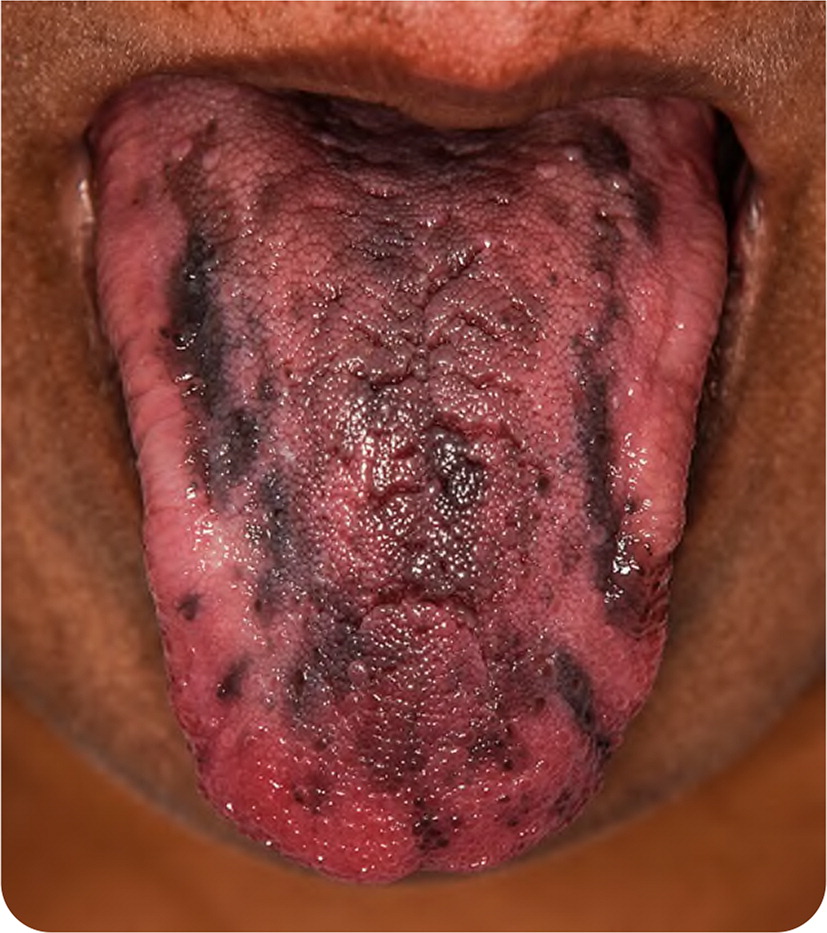
Question
Discussion
The correct answer is A: check adherence to glucocorticoid therapy. Hyperpigmentation is a characteristic clinical finding of primary adrenal insufficiency. Successful treatment of adrenal insufficiency depends on taking the correct dosage of the glucocorticoid for the prescribed period.
Hyperpigmentation is caused by an increase in adrenocorticotropic hormone, which acts as an agonist of the melanocortin-1 receptor. This receptor is highly expressed on the surface of melanocytes.1 The hyperpigmentation is most prominent at flexures, sites of pressure and friction, palmar and plantar creases, and sun-exposed areas. However, it can also affect scars and buccal, vaginal, and anal mucous membranes.
Primary adrenal insufficiency hyperpigmentation usually resolves when the excess secretion of adrenocorticotropic hormone is blocked by replacement doses of glucocorticoid. Persistence of hyperpigmentation in a patient with primary adrenal insufficiency is suggestive of medication nonadherence or inadequate dosing. Defining the appropriate dosage can be challenging because of the individual variability of glucocorticoid secretion.2 Suboptimal replacement therapy increases the risk of mortality from several conditions, including cardiovascular disease, infectious disease, and cancer.3,4 Conversely, overreplacement can result in impaired glucose tolerance, insulin resistance, obesity, and hypertension.5
Glucocorticoid replacement therapy in primary adrenal insufficiency requires continuous monitoring and adjustment. In the absence of reliable biomarkers to monitor treatment, the glucocorticoid dosage should be based on the clinical assessment. Patients must adhere to the optimal regimen and understand the necessity of monitoring and dosage adjustments, including awareness of situations that may require adjustments, especially stress dosing in cases of concurrent illness.
In this patient, adherence should be verified before increasing the dose of glucocorticoids. Dosing adjustments may be needed if treatment is inadequate despite adherence to the regimen.
Increasing the dosage of fludrocortisone, another treatment for primary adrenal insufficiency, is not indicated because mineralocorticoids are not involved in feedback inhibition of excess adrenocorticotropic hormone secretion.
Clinical observation alone may be harmful to the patient if she is not taking optimal replacement doses of glucocorticoids.
