Am Fam Physician. 2020;102(6):369-370
Author disclosure: No relevant financial affiliations.
A 27-year-old soldier deployed to Afghanistan presented with a nonresolving rash on the right upper arm that developed two months earlier. The lesion initially looked like a small pimple, so the patient tried to pop it. It subsequently ulcerated and grew slowly. The rash was nonpruritic and nonpainful. It bled and scabbed over with mild trauma, such as vigorous scrubbing in the shower. The patient did not recall any insect bites or new exposures, but he had walked around camp in short sleeves. The rash did not improve with application of an antibiotic ointment. The patient had no fevers, chills, or other symptoms.
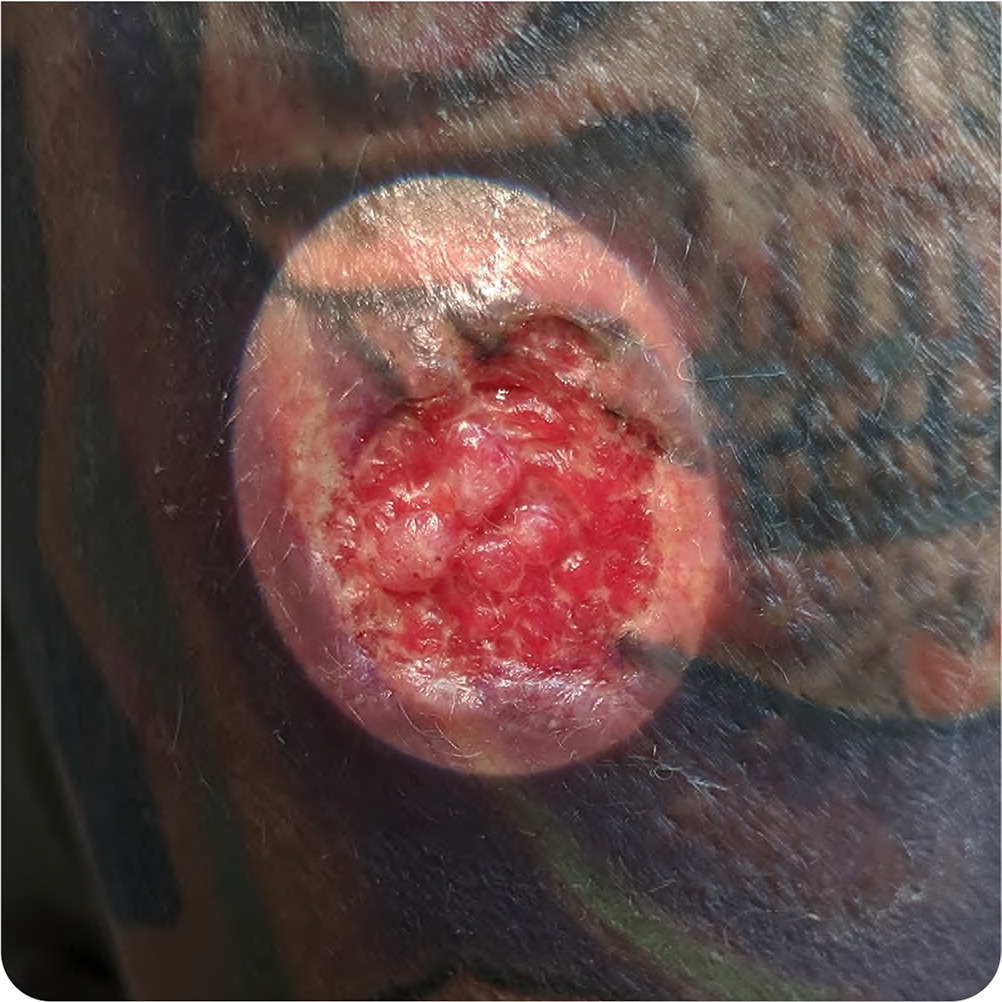
The patient's vital signs were normal. Physical examination revealed a solitary, circular, 2.4-cm, ulcerated lesion with an irregular, indurated border but no surrounding erythema (Figure 1). Physical examination findings were otherwise normal.
Question
Discussion
The answer is A: cutaneous leishmaniasis. This patient has a typical presentation of cutaneous leishmaniasis: chronic painless lesion with a central lobular appearance and interwoven granulation tissue. The mildly indurated border is sometimes described as having a volcanic appearance.1 Leishmaniasis is a protozoal infection transmitted through a sand fly bite.2 Because the sand fly is very small, many patients do not recall being bitten.2
The spectrum of leishmaniasis ranges from isolated skin involvement to mucocutaneous and systemic involvement, depending on the causative species of Leishmania.3 Isolated cutaneous leishmaniasis usually begins as a small papule and evolves into an ulcerated lesion.1 The lesion can persist for six or more months before resolving with or without treatment.3
Although not common in the United States, leishmaniasis is endemic in many regions, including North Africa, the Middle East, the Mediterranean, Mexico, Central America, and northern parts of South America.3 Worldwide, approximately 1 million cases of leishmaniasis are diagnosed every year.4 The diagnosis is made clinically based on history and physical examination findings but can be confirmed by culture and histopathologic examination of a full-thickness skin biopsy from the lesion's border.2
Cutaneous malignancy has a variable appearance, and a biopsy is required to differentiate it from lesions with a similar appearance. Cutaneous malignancy is not common in healthy young people.5
Cutaneous tuberculosis is a rare form of extrapulmonary tuberculosis. Direct inoculation results in a tuberculous chancre, which presents as a shallow, painless ulceration with a granular base, typically without a raised border.6
Pyoderma gangrenosum is an inflammatory disorder of the skin that results in painful ulcers, most commonly affecting the legs. More than 50% of patients with the condition have an underlying systemic inflammatory disease, such as ulcerative colitis, Crohn disease, or rheumatoid arthritis. Lesions typically begin as a painful papule or pustule, progressing to an ulcer with a purulent base and bluish edges.7
Tertiary syphilis can cause destructive granulomatous tumors (gummas) that affect the skin and so tissues, bone, and central nervous system. These typically develop three to 10 years after the initial infection. Tertiary syphilis is often accompanied by cardiovascular or neurologic symptoms, most commonly difficulty with coordination and balance, paralysis, blindness, and dementia. Biopsy may be indicated to differentiate gummas from lesions with a similar appearance.5
| Conditions | Characteristics |
|---|---|
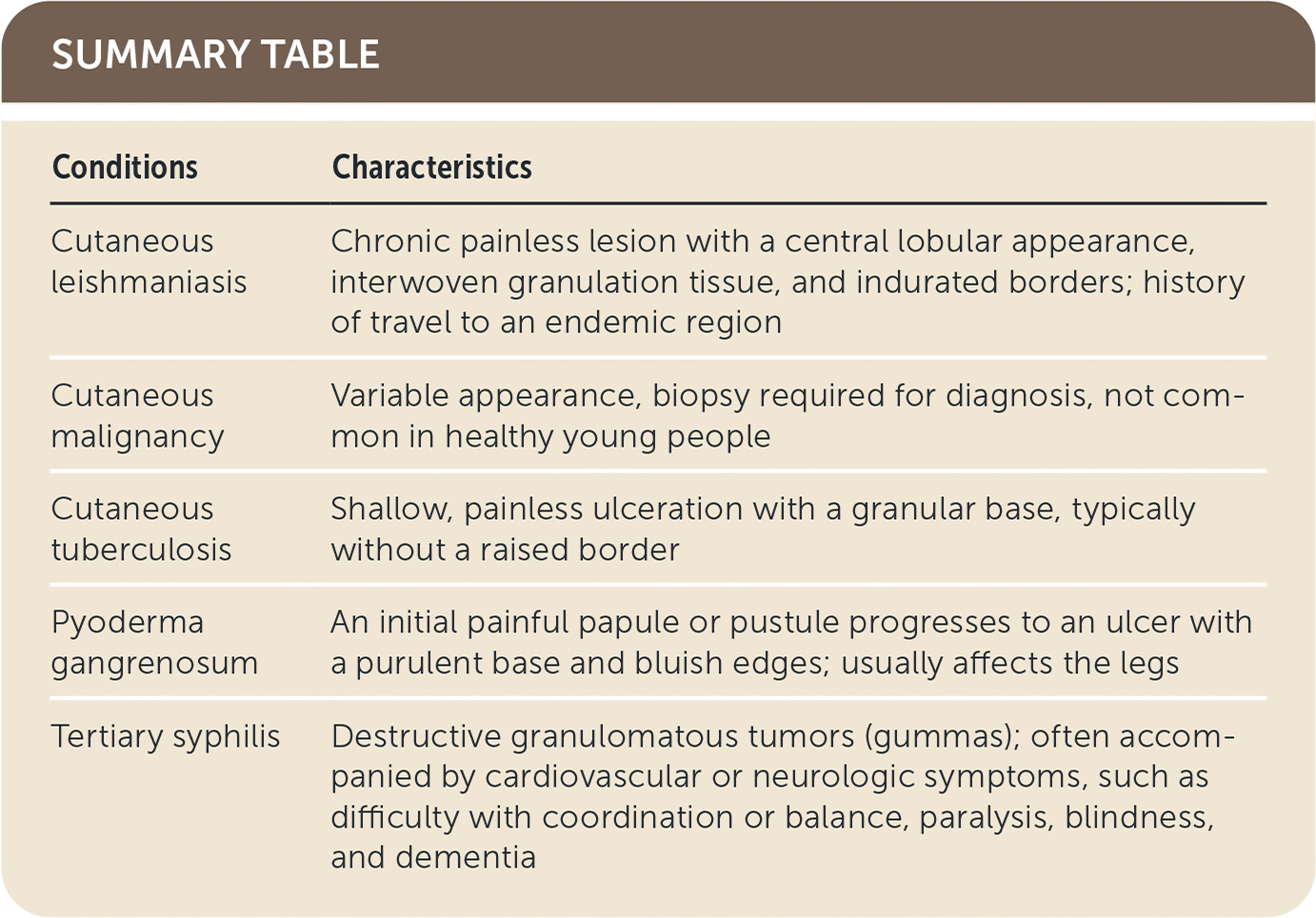
| Cutaneous leishmaniasis | Chronic painless lesion with a central lobular appearance, interwoven granulation tissue, and indurated borders; history of travel to an endemic region |
| Cutaneous malignancy | Variable appearance, biopsy required for diagnosis, not common in healthy young people |
| Cutaneous tuberculosis | Shallow, painless ulceration with a granular base, typically without a raised border |
| Pyoderma gangrenosum | An initial painful papule or pustule progresses to an ulcer with a purulent base and bluish edges; usually affects the legs |
| Tertiary syphilis | Destructive granulomatous tumors (gummas); often accompanied by cardiovascular or neurologic symptoms, such as difficulty with coordination or balance, paralysis, blindness, and dementia |
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Air Force, the Department of Defense, or the U.S. government.