Key Points for Practice
• When screening for or staging CKD, consider assessing function with urine albumin-to-creatinine ratio and serum cystatin-C measurement.
• ACE inhibitors are the best treatment for nondiabetic CKD, whereas ACE inhibitors and ARBs are beneficial in diabetic CKD. Combination ACE inhibitor and ARB therapy should be avoided.
• Treating type 2 diabetes with metformin in CKD reduces mortality and can be continued until eGFR drops to 30 mL per minute per 1.73 m2. SGLT-2 inhibitors and GLP-1 receptor agonists also improve outcomes in CKD.
From the AFP Editors
Chronic kidney disease (CKD) affects 15% of the U.S. population, although fewer than one in 10 with the disease is aware of their diagnosis. The U.S. Department of Veterans Affairs and Department of Defense (VA/DoD) have updated recommendations for evaluation and treatment of CKD.
Diagnosis
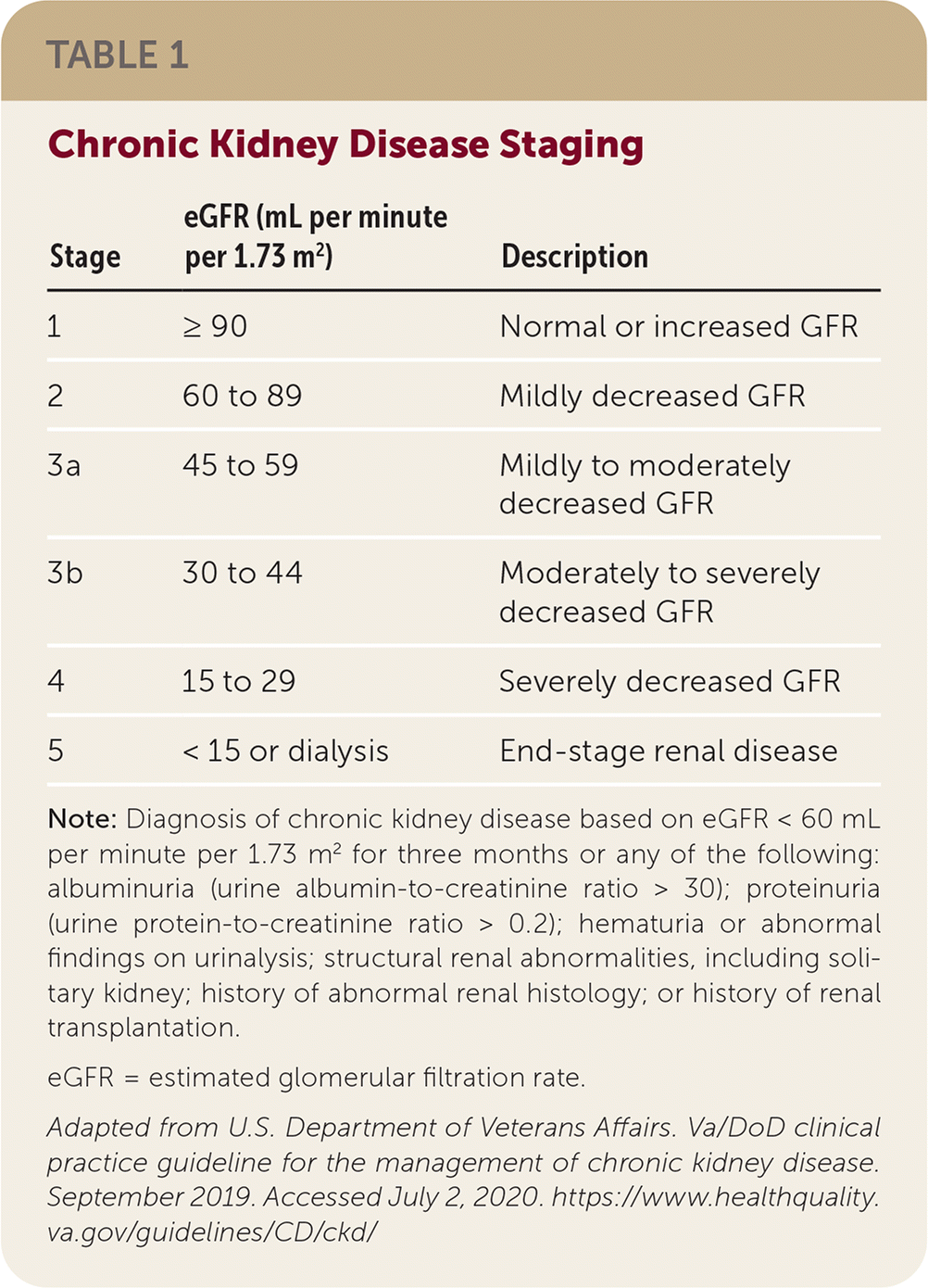
Screening for CKD does not improve outcomes in any population, and the VA/DoD recommend screening based on clinical risk and shared decision-making. CKD is staged based on estimated glomerular filtration rate (eGFR) as shown in Table 1, which is most often calculated from serum creatinine. If screening or stratifying CKD risk, physicians should use urine albumin-to-creatinine ratio testing with eGFR to improve risk prediction. The recommendations suggest a single eGFR based on a cystatin-C measurement, if available, because it is less affected by age, sex, and muscle mass than creatinine in patients with an eGFR less than 60 mL per minute per 1.73 m2. Doing so may reduce the misclassification of CKD in up to 40% of patients and may result in a higher classification stage for 25% of those with CKD.
TABLE 1. Chronic Kidney Disease Staging
| Stage | eGFR (mL per minute per 1.73 m2) | Description |
|---|---|---|
| 1 | ≥ 90 | Normal or increased GFR |
| 2 | 60 to 89 | Mildly decreased GFR |
| 3a | 45 to 59 | Mildly to moderately decreased GFR |
| 3b | 30 to 44 | Moderately to severely decreased GFR |
| 4 | 15 to 29 | Severely decreased GFR |
| 5 | < 15 or dialysis | End-stage renal disease |
Note: Diagnosis of chronic kidney disease based on eGFR < 60 mL per minute per 1.73 m2 for three months or any of the following: albuminuria (urine albumin-to-creatinine ratio > 30); proteinuria (urine protein-to-creatinine ratio > 0.2); hematuria or abnormal findings on urinalysis; structural renal abnormalities, including solitary kidney; history of abnormal renal histology; or history of renal transplantation.
eGFR = estimated glomerular filtration rate.
Adapted from U.S. Department of Veterans Affairs. Va/DoD clinical practice guideline for the management of chronic kidney disease. September 2019. Accessed July 2, 2020. https://www.healthquality.va.gov/guidelines/CD/ckd/
Nephrology Referral
Using a risk prediction model, such as the Kidney Failure Risk Calculator (https://www.mdcalc.com/kidney-failure-risk-calculator), can aid in management decisions, including when to refer patients for nephrology or transplant consultation.
Dietary Recommendations
Dietary sodium restriction to reduce proteinuria and to improve blood pressure control should be considered. Studies have evaluated various thresholds, but limiting intake to about 2,000 mg per day is generally accepted.
Limiting dietary protein intake to 0.6 to 0.8 g per kg per day to decrease CKD progression when the eGFR is below 60 mL per minute per 1.73 m2 increases malnutrition risk, which requires close monitoring.
Blood Pressure Management
One meta-analysis suggests reduced mortality in CKD when systolic blood pressure is maintained below 140 mm Hg. Angiotensin-converting enzyme (ACE) inhibitors or angiotensin II receptor blockers (ARBs) should be used to treat patients who have CKD with albuminuria and diabetes mellitus. For CKD with albuminuria but no diabetes, an ACE inhibitor is preferred because of a 31% reduction in end-stage renal disease. Both medications cause increases in potassium and creatinine levels in CKD, so monitoring is essential; combinations of ACE inhibitors and ARBs should not be used. ARBs are an appropriate alternative for ACE inhibitor–induced cough, but they are not appropriate after angioedema. No other antihypertensive medications reduce CKD progression.
Treatment of Diabetes with CKD
Metformin is considered first-line therapy to decrease mortality in type 2 diabetes with CKD. Metformin can be started above an eGFR of 45 mL per minute per 1.73 m2 and safely continued until eGFR drops to 30 mL per minute per 1.73 m2.
Consider additional treatment with sodium-glucose cotransporter-2 (SGLT-2) inhibitors and glucagon-like peptide-1 (GLP-1) receptor agonists to reduce CKD progression. SGLT-2 inhibitors slow CKD progression and reduce hospitalization for heart failure, with uncertain effect on mortality. Based on a post-hoc trial analysis, GLP-1 receptor agonists appear to reduce major cardiovascular events and mortality in CKD and may slightly reduce CKD progression. Conversely, dipeptidyl-peptidase-4 inhibitors do not improve outcomes in CKD.
Adjunctive Treatment in CKD
When CKD is complicated by metabolic acidosis, sodium bicarbonate supplementation should be used to slow progression to end-stage renal disease. Although CKD is associated with hyperuricemia, urate-lowering therapy does not slow CKD progression. Vitamin D, calcimimetics, and phosphate binders do not improve patient-oriented outcomes, even if parathyroid hormone levels are elevated.
In CKD, anemia is often associated with iron deficiency. Although intravenous iron replacement is most efficient, oral replacement is optimal when taken every other day. Erythropoiesis-stimulating agents should not be used when hemoglobin is 10 g per dL (100 g per L) or more.
Prevention of Contrast-Induced Kidney Injury
There is some evidence that intravenous isotonic saline boluses before and after iodinated contrast media administration reduce kidney injury. N-acetylcysteine has conflicting evidence, with recent studies showing no injury prevention. Prophylactic dialysis after contrast media administration does not prevent kidney injury.
Dialysis in End-Stage Renal Disease
Decisions to pursue dialysis are challenging when patients are frail or medically complex. Dialysis appears to increase survival, but at the cost of significant increases in hospitalization, invasive procedures, and death in the hospital. Patient preference for duration and control of their illness is central to this decision.
The views expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Department of the Navy, Uniformed Services University of the Health Sciences, Department of Defense, Department of Veterans Affairs, or the U.S. government.
Guideline source: U.S. Department of Veterans Affairs and Department of Defense
Evidence rating system used? Yes
Systematic literature search described? Yes
Guideline developed by participants without relevant financial ties to industry? Yes
Recommendations based on patient-oriented outcomes? Yes
Available at: https://www.healthquality.va.gov/guidelines/CD/ckd

