A healthy 69-year-old patient presented with an enlarging, nonpainful, nonpruritic nodule just below his right knee that appeared eight months earlier. Twelve years earlier he sustained trauma at the site from a twig, with resulting local atrophy.
Physical examination showed a 3-cm, firm, mobile, nontender, nonpulsatile nodule (Figure 1) on the right lower leg, inferomedial to the popliteal fossa. The lesion had no appreciable punctum or comedone, and there was no surrounding warmth or erythema.
FIGURE 1

Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Atypical fibroxanthoma.
B. Benign fibrous histiocytoma.
C. Dermatofibrosarcoma protuberans.
D. Merkel cell carcinoma.
E. Pyogenic granuloma.
Discussion
The answer is C: dermatofibrosarcoma protuberans, a rare malignant soft tissue sarcoma with high rates of local recurrence. It is most often localized to the trunk (50%), proximal extremities (35%), and head and neck (15%).1 Dermatofibrosarcoma protuberans appears as a firm, nodular, or plaque-like fixated lesion of varying color, with occasional discoloration of the surrounding skin. The growth may take months or years to form, resulting in large protuberant nodules. A notable exception is dermatofibrosarcoma protuberans of the scalp, which is associated with early periosteal involvement.2
Presence of the typical lesion combined with a history of growth over an extended period is helpful in identifying dermatofibrosarcoma protuberans. The lesion may develop in the area of a previous injury.
Arising from the dermis, dermatofibrosarcoma protuberans is characterized by local aggressive growth with pseudopod-like extensions into the surrounding tissues, including fascial planes and muscle. This contributes to a high rate of recurrence (nearly 50%) following standard excision.3 However, the condition is rarely fatal because of the low risk of metastasis. Approximately 4% of patients with dermatofibrosarcoma protuberans develop distant metastases, predominantly in the lung and often after multiple local recurrences.3
More than 90% of dermatofibrosarcoma protuberans cases result from a translocation between chromosomes 17 and 22, which leads to fusion of the collagen type I alpha1 chain (COL1A1) gene with the platelet-derived growth factor subunit B (PDGFB) gene.1 This results in continuous activation of PDGFB protein tyrosine kinase and subsequent cell growth.
Surgical excision using Mohs micrographic surgery is the main treatment for dermatofibrosarcoma protuberans. If micrographic surgery is unavailable, wide local excision with 3-cm margins may be performed.4
An atypical fibroxanthoma is a malignant, nonmetastasizing tumor that presents as an erythematous plaque or sore that becomes nodular and ulcerative. It almost always develops on the head and face. It is associated with sun damage and previous radiotherapy.
Benign fibrous histiocytoma, also called dermatofibroma, is a collection of benign fibroblast-like cells presenting as a solitary, firm nodule, predominantly on the lower extremities. Lesions are normally asymptomatic but may be mildly painful or pruritic. Although typically measuring less than 1 cm, clinical variations larger than 5 cm have been reported.5
Merkel cell carcinoma is an aggressive, rapidly growing neuroendocrine tumor that typically affects patients who are older or immunosuppressed. It presents as a single asymptomatic subcutaneous nodule, often with a red or blue hue. It usually affects the face, head, or neck.
A pyogenic granuloma is a benign friable vascular papule or nodule that is red or purple. It may develop in an area of previous trauma. It typically appears abruptly and grows quickly. Although a pyogenic granuloma may develop anywhere, the fingers, face, and scalp are most common.
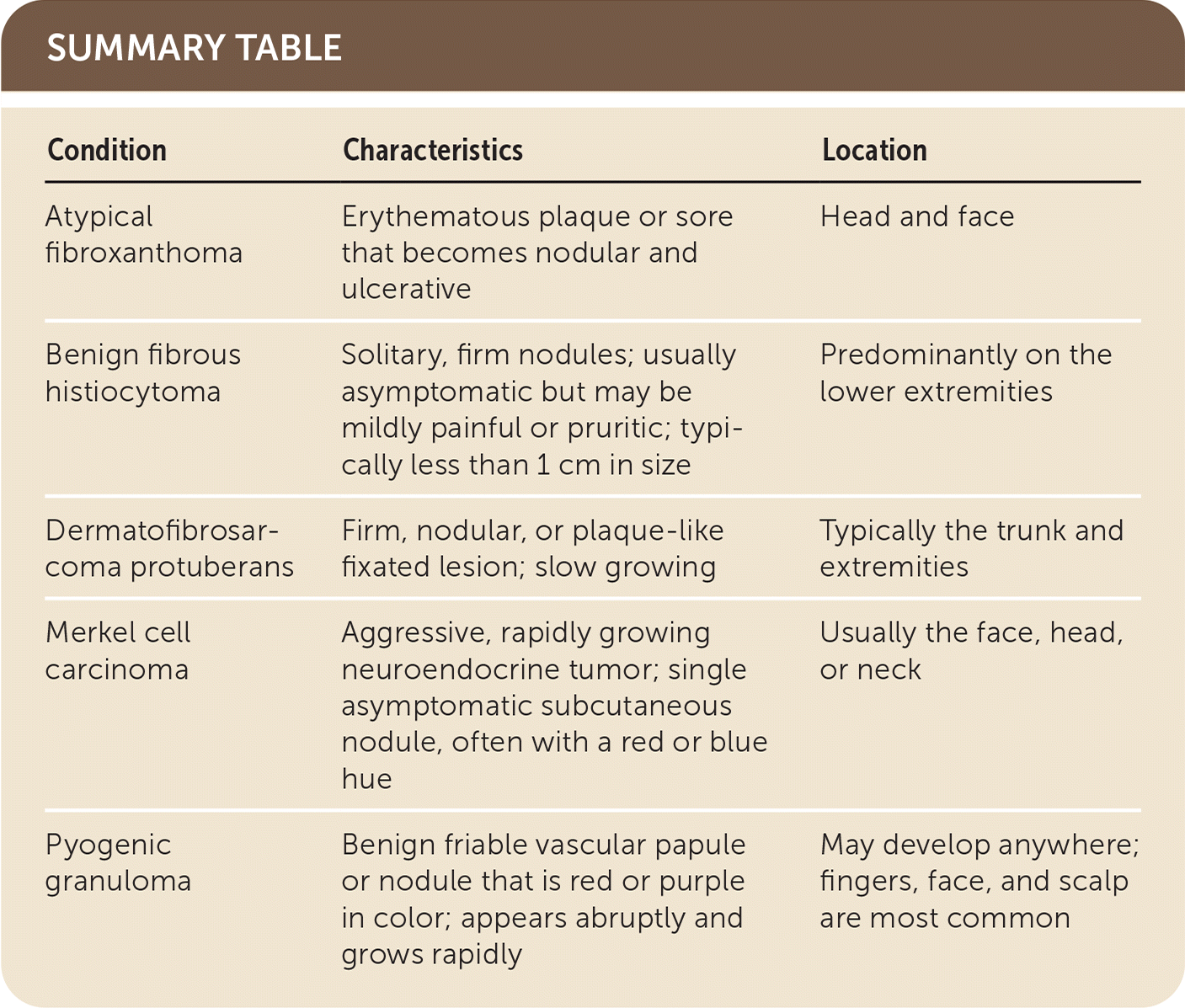
SUMMARY TABLE
| Condition | Characteristics | Location |
|---|---|---|
| Atypical fibroxanthoma | Erythematous plaque or sore that becomes nodular and ulcerative | Head and face |
| Benign fibrous histiocytoma | Solitary, firm nodules; usually asymptomatic but may be mildly painful or pruritic; typically less than 1 cm in size | Predominantly on the lower extremities |
| Dermatofibrosarcoma protuberans | Firm, nodular, or plaque-like fixated lesion; slow growing | Typically the trunk and extremities |
| Merkel cell carcinoma | Aggressive, rapidly growing neuroendocrine tumor; single asymptomatic subcutaneous nodule, often with a red or blue hue | Usually the face, head, or neck |
| Pyogenic granuloma | Benign friable vascular papule or nodule that is red or purple in color; appears abruptly and grows rapidly | May develop anywhere; fingers, face, and scalp are most common |
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Navy, U.S. Air Force, Department of Defense, or the U.S. government.

