Clinical Question
Can a clinical prediction rule accurately identify patients at low risk of complicated acute diverticulitis, defined as diverticulitis accompanied by abscess or peritonitis?
Evidence Summary
Uncomplicated diverticulitis is defined as diverticulitis without abscess, fistula, perforation, or bleeding.1 Two randomized trials found that patients with uncomplicated diverticulitis do not benefit from antibiotics, and a systematic review concluded that most of these patients can be safely managed as outpatients.2–4 To avoid unnecessary radiation exposure and cost, it would be desirable to prioritize imaging and referral for patients at increased risk of complicated diverticulitis, with conservative outpatient management for patients at low risk of complications.
A systematic review identified 12 studies, including a total of 4,619 patients, that evaluated risk factors for complicated diverticulitis.5 The authors concluded that individual risk factors include increasing age, diffuse rather than localized abdominal pain, guarding or rebound pain, initial episode of diverticulitis, steroid use, fever, constipation, vomiting, elevated C-reactive protein (CRP) level, and elevated white blood cell (WBC) count. They proposed a clinical prediction rule based on the results of the meta-analysis but did not test it.
Another study identified 182 patients hospitalized for acute diverticulitis, of whom 24 (13%) had complicated diverticulitis defined as abscess or need for surgery.6 The mean CRP level was 10 mg per dL (100 mg per L) in patients with nonsevere diverticulitis and 25.6 mg per dL (256 mg per L) in those with complicated disease. Using a cutoff of 17 mg per dL (170 mg per L), 91% with nonsevere diverticulitis had a CRP level below that cutoff compared with only 12.5% of those with complicated disease (91% sensitive and 87.5% specific for the diagnosis of nonsevere diverticulitis).6 A second study of 99 consecutive patients, all of whom underwent computed tomography, found a sensitivity of 90.9% and specificity of 90.9% using a similar cutoff of 17.3 mg per dL (173 mg per L).7
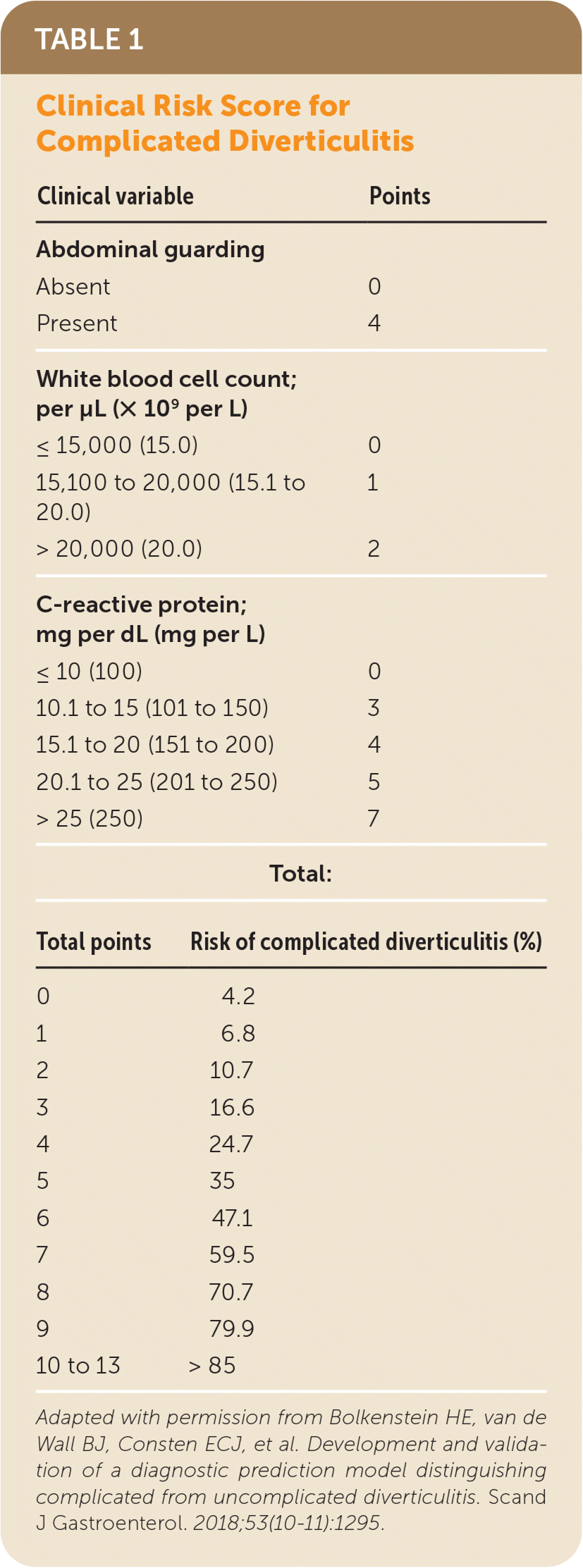
Finally, Bolkenstein and colleagues developed and validated a simple clinical risk score (Table 1) to determine the likelihood of complicated diverticulitis, defined as the presence of abscess or peritonitis and requiring intervention.8 They used data from 950 patients with acute diverticulitis, randomly dividing the patients into a derivation group, which was used to develop the risk score through multivariate analysis, and a validation group; both groups included 475 patients. The overall prevalence of complicated diverticulitis was 19% in the validation group.
TABLE 1. Clinical Risk Score for Complicated Diverticulitis
| Clinical variable | Points |
|---|---|
| Abdominal guarding | |
| Absent | 0 |
| Present | 4 |
| White blood cell count; per μL (× 109 per L) | |
| ≤ 15,000 (15.0) | 0 |
| 15,100 to 20,000 (15.1 to 20.0) | 1 |
| > 20,000 (20.0) | 2 |
| C-reactive protein; mg per dL (mg per L) | |
| ≤ 10 (100) | 0 |
| 10.1 to 15 (101 to 150) | 3 |
| 15.1 to 20 (151 to 200) | 4 |
| 20.1 to 25 (201 to 250) | 5 |
| > 25 (250) | 7 |
| Total: | |
| Total points | Risk of complicated diverticulitis (%) |
| 0 | 4.2 |
| 1 | 6.8 |
| 2 | 10.7 |
| 3 | 16.6 |
| 4 | 24.7 |
| 5 | 35 |
| 6 | 47.1 |
| 7 | 59.5 |
| 8 | 70.7 |
| 9 | 79.9 |
| 10 to 13 | > 85 |
Adapted with permission from Bolkenstein HE, van de Wall BJ, Consten ECJ, et al. Development and validation of a diagnostic prediction model distinguishing complicated from uncomplicated diverticulitis. Scand J Gastroenterol. 2018;53(10–11):1295.
The final risk score included the presence or absence of abdominal guarding, the WBC count, and the CRP level. For patients with a CRP level of 10 mg per dL or lower, WBC count of 15,000 per μL (15.0 × 109 per L) or lower, and no abdominal guarding, the risk of complicated diverticulitis decreased from 19% to 4.2%. One limitation of the study was retrospective data collection, although this would not affect reliability of ascertainment of WBC count and CRP level.8
Applying the Evidence
A 62-year-old patient presents to urgent care with acute left lower quadrant pain. The patient takes an antihypertensive and thyroid replacement therapy but is otherwise healthy. The patient does not have a history of known diverticular disease. On examination, the patient has diffuse tenderness but no abdominal guarding. The patient has a WBC count of 17,300 per μL (17.3 × 109 per L) and a CRP level of 16.80 mg per dL (168 mg per L). The patient receives 5 points using the clinical risk score, which is associated with a 35% likelihood of complicated diverticulitis. You refer the patient to the hospital for abdominal computed tomography and evaluation by a general surgeon.

