Key Points for Practice
• Outside the hospital, hypothermia is diagnosed by presentation, not core temperature. Movement is impaired in mild hypothermia, and alertness lost and shivering slowed or stopped in moderate hypothermia.
• Insulation and vapor barrier from the ground and elements are key to all hypothermia treatment.
• Moderate and severe hypothermia require active warming and gentle handling to prevent dysrhythmia.
From the AFP Editors
Accidental hypothermia occurs when core temperature reaches 95°F (35°C) or lower outside of medical therapy. Hypothermia is common in wilderness environments and among urban homeless, especially with the use of alcohol or other intoxicating substances. Shivering slows around 89.6°F (32°C) and ceases by 86°F (30°C). Brain activity begins to decline around 93.2°F (34°C). Below 86°F, decreased cardiac output and bradycardia predispose the patient to dysrhythmia.
The Wilderness Medical Society has published an updated guideline on treating accidental hypothermia outside of hospitals, including a staging classification system based on clinical observation.
Evaluation
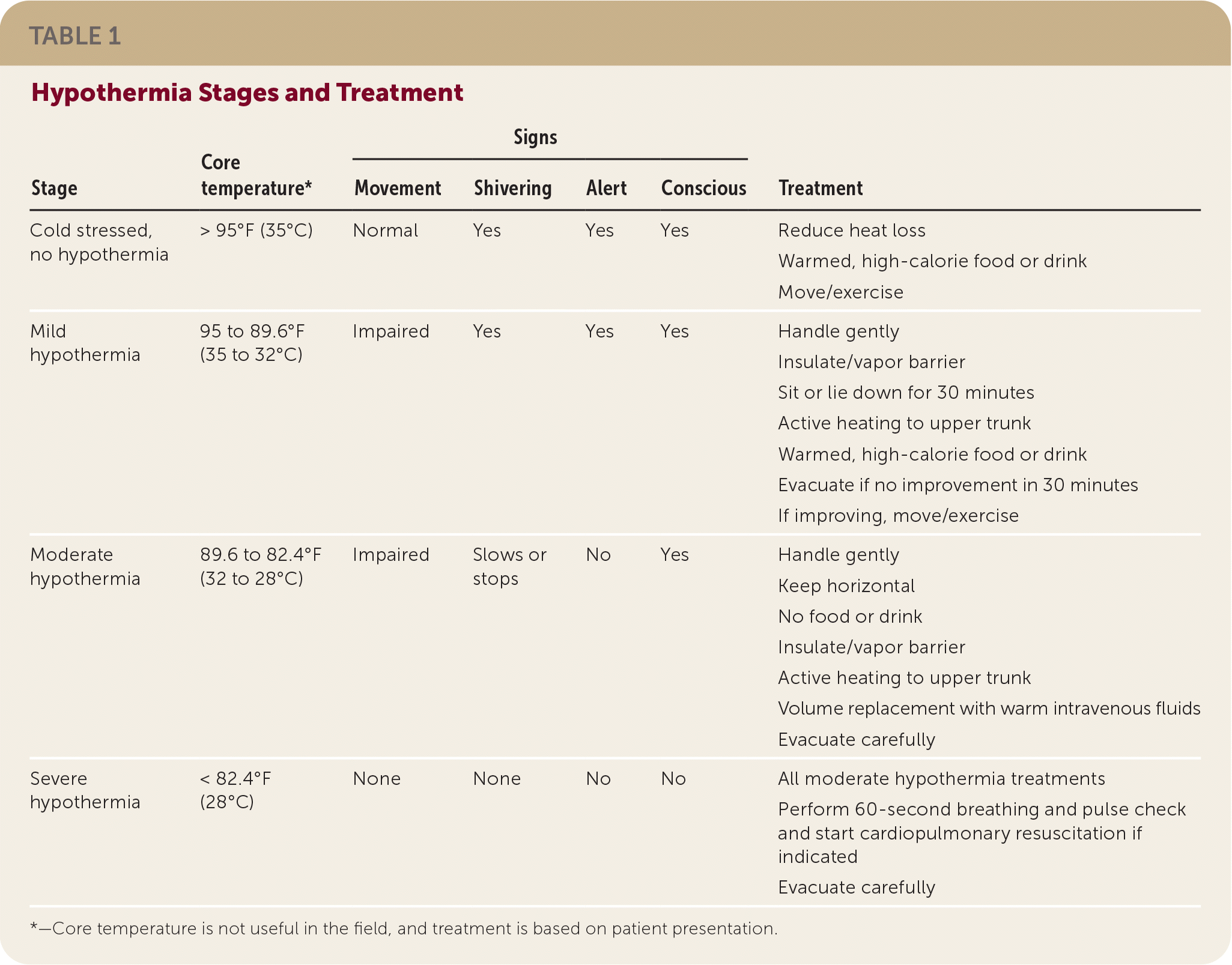
Hypothermia first affects movement when mild, followed by declining alertness and loss of shivering in moderate hypothermia before a person becomes unconscious. Hypothermia should be considered in people who feel cold and are shivering and who are incapacitated or having difficulty caring for themselves. Table 1 shows how presentation changes with each stage of hypothermia. Outside a hospital, the diagnosis of hypothermia and treatment is guided by patient assessment because core temperature readings are difficult and inaccurate.
TABLE 1. Hypothermia Stages and Treatment
| Stage | Core temperature* | Signs | Treatment | |||
|---|---|---|---|---|---|---|
| Movement | Shivering | Alert | Conscious | |||
| Cold stressed, no hypothermia | > 95°F (35°C) | Normal | Yes | Yes | Yes | Reduce heat loss Warmed, high-calorie food or drink Move/exercise |
| Mild hypothermia | 95 to 89.6°F (35 to 32°C) | Impaired | Yes | Yes | Yes | Handle gently Insulate/vapor barrier Sit or lie down for 30 minutes Active heating to upper trunk Warmed, high-calorie food or drink Evacuate if no improvement in 30 minutes If improving, move/exercise |
| Moderate hypothermia | 89.6 to 82.4°F (32 to 28°C) | Impaired | Slows or stops | No | Yes | Handle gently Keep horizontal No food or drink Insulate/vapor barrier Active heating to upper trunk Volume replacement with warm intravenous fluids Evacuate carefully |
| Severe hypothermia | < 82.4°F (28°C) | None | None | No | No | All moderate hypothermia treatments Perform 60-second breathing and pulse check and start cardiopulmonary resuscitation if indicated Evacuate carefully |
*—Core temperature is not useful in the field, and treatment is based on patient presentation.
Treatment
MILD HYPOTHERMIA
In mild hypothermia, shivering can effectively produce heat if patients are insulated from the elements. Protection from further cooling should include using insulation and a vapor barrier, especially for the head and neck and between the patient and the ground. Wet clothes should not be removed until the patient is in a warm environment.
An alert patient with effective shivering and no increased aspiration risk can benefit from warmed, high-calorie liquid or food. The patient should remain seated or horizontal for at least 30 minutes and be carefully observed after that. After a period of warming, calorie replacement, and observation, allowing the patient to increase exercise slowly to generate additional heat may be considered. Active external heat sources should be applied to the axillae, chest, and back. Use of insulation with vapor barriers with active heat sources will maximize heat absorption. Cold injured skin should be rechecked every 20 to 30 minutes to decrease burn risk.
MODERATE AND SEVERE HYPOTHERMIA
For patients with moderate or severe hypothermia, peripheral rewarming can increase cold blood return to the heart, leading to a drop in core temperature that increases risk of dysrhythmia. This afterdrop can be caused by patient movement, warm water immersion, or other heat applied to extremities. Patients with moderate hypothermia should be kept horizontal to prevent afterdrop. After cold water rescues, decreased catecholamines can worsen afterdrop and cause life-threatening hypotension or sudden onset cardiac dysrhythmia. This process is known as circumrescue collapse.
Active rewarming is essential for treating moderate to severe hypothermia. Large heat packs cover more surface area; small chemical packs provide insufficient heat for core rewarming but may be used on hands and feet during transport. Heated humidified oxygen and fluid resuscitation with normal saline warmed to 104 to 107.6°F (40 to 42°C) may be used with active rewarming, if available.
During transport, forced air warming or increasing the transportation compartment to at least 75.2°F (24°C) is most effective for heat retention.
RESUSCITATION
Because hypothermia decreases metabolism, traditional signs of futility do not apply in hypothermia. Fixed, dilated pupils, rigor mortis, and apparent dependent lividity may occur in patients who can be resuscitated. One-minute carotid pulse checks may be necessary to palpate a bradycardic pulse through cold skin. If high-quality cardiopulmonary resuscitation must be interrupted by rescue, compressions should be performed for five minutes with no more than five-minute breaks in between. All defibrillations should be at maximum power. If core temperature is below 86°F and an initial defibrillation is unsuccessful, further shocks should be delayed until core temperature exceeds 86°F. Atrial dysrhythmias are common during rewarming and often resolve spontaneously. End tidal carbon dioxide monitoring is used, if available, to prevent hyperventilation with decreased metabolic load; otherwise, one-half the normal ventilation rate should be delivered.
Editor's Note: The current guideline simplifies staging of hypothermia compared with a recent AFP article discussing hypothermia (https://www.aafp.org/afp/2019/1201/p680.html).
The article references the previous edition of this guideline but also includes discussion of frostbite and nonfreezing injuries such as frostnip, pernio, and immersion foot. AFP also published a summary of the 2019 Wilderness Medical Society guideline on frostbite (https://www.aafp.org/afp/2020/0401/p440.html).—Michael J. Arnold, MD, AFP Contributing Editor
Guideline source: Wilderness Medical Society
Evidence rating system used? Yes
Systematic literature search described? Yes
Guideline developed by participants without relevant financial ties to industry? Yes
Recommendations based on patient-oriented outcomes? Yes
Published source: Wilderness Environ Med. December 2019; 30(4S):S47–S69

