Seasonal affective disorder is a mood disorder that is a subtype or qualifier of major depressive disorder or bipolar disorder in the Diagnostic and Statistical Manual of Mental Disorders. It is characterized by depressive symptoms that occur at a specific time of year (typically fall or winter) with full remission at other times of year (typically spring or summer). Possible risk factors include family history, female sex, living at a more northern latitude, and young adulthood (18 to 30 years of age). With the temporal nature of the mood episodes, diagnosis requires full remission when the specified season ends and two consecutive years of episodes in the same season. First-line therapy for seasonal affective disorder includes light therapy, antidepressants, and cognitive behavior therapy, alone or in combination. Commercial devices are available for administering light therapy or dawn simulation. The light intensity and duration of treatment depend on the device and the patient's initial response, but 2,500 to 10,000 lux for 30 to 60 minutes at the same time every day is typically effective. Lifestyle interventions, such as increasing exercise and exposure to natural light, are also recommended. If seasonal affective disorder recurs, long-term treatment or preventive intervention is typically indicated, and bupropion appears to have the strongest evidence supporting long-term use. Continuing light therapy or other antidepressants is likely beneficial, although evidence is inconclusive. Evidence is also inconclusive for psychotherapy and vitamin D supplementation.
Seasonal affective disorder (SAD) is a mood disorder with depressive symptoms that occur at a specific time of year with full remission at other times of year. It typically occurs during fall or winter, although a less common form occurs during spring or summer.1,2 The pathophysiology is unclear, but theories include circadian rhythm disruption, dysregulation of the melanopsin signaling pathway and its impact on serotonin reuptake, and dysfunction of the hypothalamic-pituitary-adrenal axis.3–5 Studies using interviews and diagnostic criteria in the United States, Canada, and United Kingdom show a lifetime prevalence of 0.5% to 2.4% in the general population.6–8 Of patients with major depression, 10% to 20% have a seasonal pattern of symptoms consistent with SAD.9
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Comments |
|---|---|---|
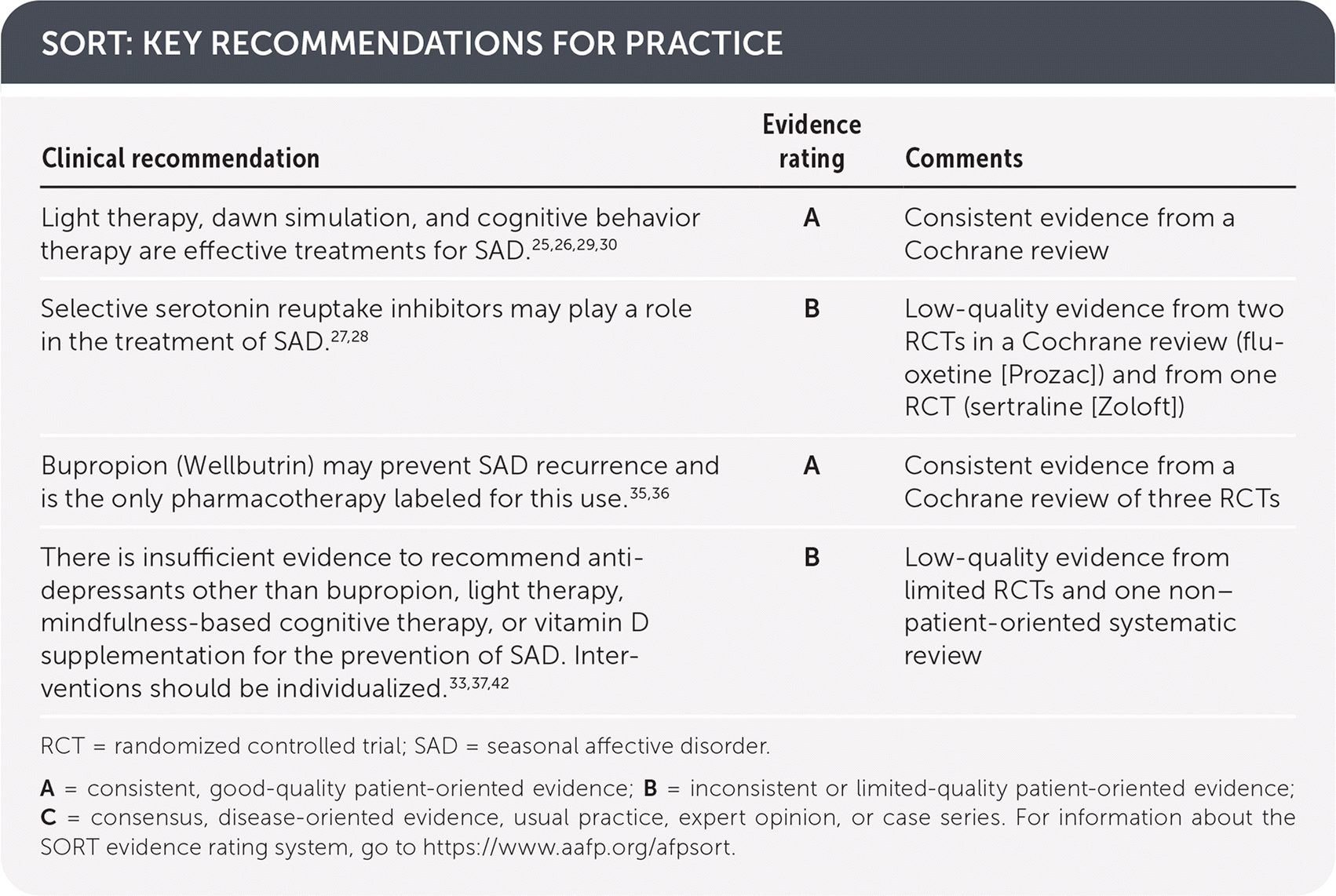
| Light therapy, dawn simulation, and cognitive behavior therapy are effective treatments for SAD.25,26,29,30 | A | Consistent evidence from a Cochrane review |
| Selective serotonin reuptake inhibitors may play a role in the treatment of SAD.27,28 | B | Low-quality evidence from two RCTs in a Cochrane review (fluoxetine [Prozac]) and from one RCT (sertraline [Zoloft]) |
| Bupropion (Wellbutrin) may prevent SAD recurrence and is the only pharmacotherapy labeled for this use.35,36 | A | Consistent evidence from a Cochrane review of three RCTs |
| There is insufficient evidence to recommend antidepressants other than bupropion, light therapy, mindfulness-based cognitive therapy, or vitamin D supplementation for the prevention of SAD. Interventions should be individualized.33,37,42 | B | Low-quality evidence from limited RCTs and one non–patient-oriented systematic review |
RCT = randomized controlled trial; SAD = seasonal affective disorder.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
What Are the Risk Factors for SAD?
Evidence for risk factors is mostly weak or limited but suggests that family history, female sex, living at a more northern latitude, and young adulthood (18 to 30 years of age) may increase risk.10–15
EVIDENCE SUMMARY
An Australian study of 4,000 twins compared symptoms in identical twins with symptoms in fraternal twins. Sets of identical twins were twice as likely to have SAD than sets of fraternal twins, suggesting a possible genetic link.10 Specific associated genes have not been identified, but a 2018 meta-analysis revealed ZBTB20 as a potential susceptibility gene for SAD.11
Two large questionnaire studies have shown that individuals living in more northern latitudes have an increased risk of developing SAD.12,13 It is suspected that prevalence increases with increasing latitude, but data are poor, and this conclusion is controversial.12,13
Two studies using the Seasonal Pattern Assessment Questionnaire (SPAQ) found that SAD has a higher prevalence in females, but this is based on poor data.14,15 A 2000 meta-analysis of population studies found that SAD appears to be most prevalent among young adults.9
What Are the Diagnostic Criteria for SAD?
In addition to meeting Diagnostic and Statistical Manual of Mental Disorders , 5th ed., (DSM-5) criteria for major depressive disorder or bipolar disorder, there must be a temporal relationship between time of year and occurrence of mood episodes. Mood episodes are discrete periods during which the patient demonstrates depressive symptoms. Full remission must occur when the specified season ends. There must be two consecutive years of mood episodes in the same season to diagnose fall/winter or spring/summer SAD. In SAD, seasonal mood episodes significantly outnumber nonseasonal mood episodes during the individual's life.1
EVIDENCE SUMMARY
The DSM-5 does not define SAD as a separate diagnosis and instead includes it as a variant of major depressive disorder or bipolar disorder.1 Typical features of depression include depressed mood, anhedonia, guilt or hopelessness, decreased energy, and impaired mood. Typical features of bipolar disorder include mania, hypomania, depression, irritability, anxiety, mood lability, sleep disturbance, and hyperactivity. SAD is a subtype or qualifier of these mood disorders with a seasonal onset and remission.
The more common fall/winter type of SAD has occasional atypical features, such as increased need for sleep, carbohydrate cravings with increased appetite and weight gain, and extreme fatigue.16 The less common spring/summer type may have the atypical symptoms of increased irritability, poor appetite with weight loss, insomnia, agitation, restlessness, anxiety, and increased violence.17
To meet the diagnostic criteria, psychosocial stressors of a specified season, such as layoffs during the winter season, must not contribute to the mood episodes. Additionally, the diagnosis requires a two-year consecutive pattern of mood episodes during a specified season.1
Although the SPAQ was developed to assess for SAD, it is typically used in the research setting and has variable sensitivity (44% to 94%) and specificity (73% to 94%).18,19 Better screening tools have not been tested or validated. Therefore, SAD should be diagnosed using DSM-5 criteria and not the SPAQ.17
What Is the Recommended Initial Treatment for SAD?
Clinical guidelines recommend light therapy, antidepressants, cognitive behavior therapy (CBT), and/or lifestyle interventions (e.g., increasing exercise and exposure to natural light), alone or in combination.20–24
EVIDENCE SUMMARY
Light therapy uses exposure to a high illuminating fluorescent bulb. Intensity of light is generally 2,500 to 10,000 lux. Light therapy devices are typically commercially available as “light boxes” that disperse light and filter out ultraviolet rays. Patient positioning and distance from the device and length of daily exposure depend on the manufacturer's specifications and the patient's response to therapy. However, light therapy typically occurs for 30 to 60 minutes at the same time every day, shortly after waking. Patients should face the light but may do other activities, such as reading or exercising, during therapy. Light therapy is considered very low risk (the bright midday sun is equivalent to about 50,000 to 100,000 lux of light), but patients with diseases involving the eyes or who are taking medications that sensitize the eyes to light may benefit from ophthalmology clearance before initiation of therapy. Dawn simulation is an alternative to light therapy that uses a much weaker light (e.g., 250 lux) that is gradually applied at the end of a patient's sleep cycle and as they wake.24
A 2005 meta-analysis of eight randomized controlled trials (RCTs) with 228 total patients demonstrated that bright light therapy and dawn simulation are effective treatments for SAD with an effect size of 0.84, which is similar to antidepressant therapy.25 A recent meta-analysis of 19 studies including 610 total patients showed that bright light therapy was effective compared with placebo, with an improvement in depression scores (95% CI, −0.63 to −0.12) and a risk ratio (RR) of 1.42 (95% CI, 1.08 to 1.85) for response to active treatment.26
Selective serotonin reuptake inhibitors (SSRIs) are typically first-line therapy for unipolar depression and have been shown to improve depression subtypes such as SAD. In a 2011 Cochrane review, fluoxetine (Prozac) was statistically similar to light therapy in effectiveness and safety (RR = 0.98; 95% CI, 0.77 to 1.24).27 A 2004 RCT including 204 patients with SAD reported significantly greater improvements in depression scores and a greater treatment response rate with sertraline (Zoloft) compared with placebo (62% vs. 42%; P = .04).28
In 2015 and 2016, RCTs compared CBT with light therapy over subsequent winter seasons. The first study found that CBT and light therapy both significantly improved depression severity with similar remission rates after the first winter. However, in the follow-up study, the CBT group had less recurrence and higher rates of remission after the second winter compared with the light therapy group, suggesting that CBT was statistically superior for acute and recurrent SAD.29,30
Sleep hygiene and exercise may positively impact SAD, and although evidence is lacking from well-designed clinical trials, harm is minimal, and they have other benefits. Avoiding prolonged screen time before bed, having a regular sleep-wake cycle, walking outside or adjusting the work environment to increase natural light, or doing aerobic exercise can improve mood symptoms.31,32
What Are the Recommended Methods for Preventing Recurrence of SAD?
Light therapy and antidepressants, such as SSRIs, are likely beneficial in preventing recurrence, but evidence on long-term prevention is inconclusive. Bupropion (Wellbutrin) has been shown to prevent recurrence in patients with a history of SAD. Evidence is inconclusive for other therapies, such as psychotherapy and vitamin D supplementation.33–42
EVIDENCE SUMMARY
Because a SAD diagnosis requires at least two years of recurrent episodes, patients with the disorder will likely need long-term treatment in future seasons. Although it is appropriate to continue effective treatments for acute SAD, such as light therapy and SSRIs, studies investigating long-term preventive strategies (i.e., treatment beyond one season) are less conclusive. For example, a 2019 Cochrane review compared infrared light therapy with bright white light therapy performed from October to April for the prevention of SAD. Compared with no light therapy, the incidence of subsequent depressive episodes was similar for patients treated with infrared light therapy (RR = 0.50; 95% CI, 0.21 to 1.17) and bright light therapy (RR = 0.64; 95% CI, 0.30 to 1.38).33,34
Although SSRIs are appropriate first-line agents, alone or in combination with light therapy, bupropion is the only medication specifically labeled for preventing SAD. A 2019 Cochrane review showed that fewer patients experienced recurrent major depressive episodes during winter months when starting bupropion between September and November, before recurrence of symptoms (RR = 0.56; 95% CI, 0.44 to 0.72).35,36
Mindfulness-based cognitive therapy combines CBT with mindfulness and meditation as treatment for depression. A 2019 Cochrane review comparing preventive mindfulness-based cognitive therapy (administered in summer months before the next episode) with light therapy found similar incidence of SAD in both groups. Notably, there is little evidence to assess the effectiveness of these and other psychological treatments, such as psychodynamic and integrative therapies.37,38
Vitamin D deficiency is thought to be associated with depressive disorders, and systematic reviews have shown that supplementation may improve depression. However, the use of vitamin D supplementation has not been well studied in SAD, and only one meta-analysis, limited to a subset of women 70 years and older with SAD, did not find positive mood improvement.39–42
This article updates previous articles on this topic by Kurlansik and Ibay43; Lurie, et al.44; and Saeed and Bruce.45
Data Sources: A PubMed search was conducted using the key term seasonal affective disorder. The search included systematic and clinical reviews, meta-analyses, reviews of clinical trials and other primary sources, and evidence-based guidelines. Also searched were the Cochrane database, National Guideline Clearinghouse, Essential Evidence Plus, and Ovid database. References from these sources were consulted to clarify the statements made in publications. Search dates: September to November 2019 and August 2020.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as the official policy or position of the U.S. Army, the Department of Defense, or the U.S. government.

