Icosapent ethyl (Vascepa) is a purified ethyl ester of eicosapentaenoic acid (EPA).1 It can be used as an adjunct to maximally tolerated statin therapy to reduce the risk of myocardial infarction, stroke, coronary revascularization, and unstable angina requiring hospitalization in adult patients with elevated triglyceride levels (150 mg per dL [1.69 mmol per L] or greater) and established cardiovascular disease (CVD) or diabetes mellitus and two or more additional risk factors for CVD.1 , 2 It can also be used as an adjunct to diet and lifestyle to treat patients with severe hypertriglyceridemia (i.e., triglyceride levels greater than 500 mg per dL [5.65 mmol per L]).1
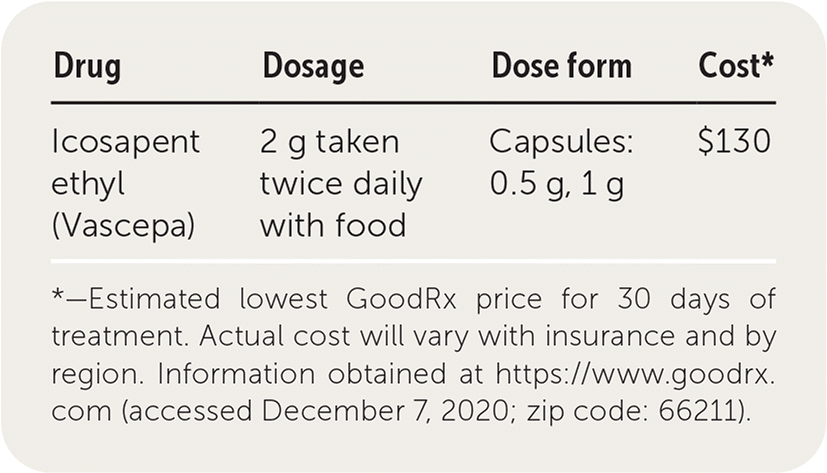
| Drug | Dosage | Dose form | Cost* |
|---|---|---|---|
| Icosapent ethyl (Vascepa) | 2 g taken twice daily with food | Capsules: 0.5 g, 1 g | $130 |
*—Estimated lowest GoodRx price for 30 days of treatment. Actual cost will vary with insurance and by region. Information obtained at https://www.goodrx.com (accessed December 7, 2020; zip code: 66211).
Safety
Atrial fibrillation occurs slightly more often in patients treated with icosapent ethyl (number needed to harm = 72) compared with placebo. Icosapent ethyl is also associated with an increased rate of hospitalization for atrial fibrillation or flutter (number needed to harm = 91).1,3 The likelihood of bleeding was slightly higher when patients taking an antithrombotic were given icosapent ethyl instead of placebo (12% vs. 10%).1,3 Because EPA is obtained from fish oil, there is a theoretical potential for allergic reaction in patients allergic to fish or shellfish.
Tolerability
Icosapent ethyl is generally well-tolerated. Adverse effects occur significantly more often with icosapent ethyl than with placebo and include musculoskeletal pain (35.9% vs. 34.4%), arthralgia (7.7% vs. 6.7%), edema (6.5% vs. 5.0%), constipation (5.4% vs. 3.6%), and gout (4.2% vs. 3.1%).1,3,4 Rates of indigestion and burping, which are common with fish oil, have not been reported.
Effectiveness
Icosapent ethyl reduces the risk of ischemic events in patients who have established CVD or who are at high risk of CVD and are on maximal statin therapy but with persistently elevated triglyceride levels (greater than 135 mg per dL [1.53 mmol per L]). Icosapent ethyl was studied in a large, randomized, double-blind, placebo-controlled trial that enrolled more than 8,000 patients.4 Participants were on statin therapy with elevated fasting triglyceride levels (i.e., 135 mg per dL to less than 500 mg per dL) and were at least 45 years of age with established CVD or at least 50 years of age and at high risk of CVD.4 Compared with placebo, treatment with icosapent ethyl, 2 g twice daily for five years, reduced fatal or nonfatal myocardial infarction (number needed to treat [NNT] = 39; 95% CI, 29 to 63), coronary revascularization (NNT = 38; 95% CI, 29 to 60), hospitalization for unstable angina (NNT = 83; 95% CI, 57 to 204), and fatal or nonfatal stroke (NNT = 111; 95% CI, 68 to 443). The risk of cardiovascular death was also reduced, although this rate is less precise because of a wide CI (NNT = 99; 95% CI, 58 to 986).5
Icosapent ethyl has not been compared directly with fibric acid derivatives, niacin, or other fish oil derivatives such as omega-3-acid ethyl esters (Lovaza). However, fibric acids, niacin, and fish oil have not demonstrated cardiovascular morbidity or mortality benefits in randomized trials.6 Icosapent ethyl has only been studied in combination with a statin. It has not been studied in patients with a lower risk of CVD..
Price
A one-month supply of icosapent ethyl costs about $130 in addition to the cost of maximal statin therapy. This is significantly more expensive than omega-3-acid ethyl esters, which is available as generic and costs about $40 for a 30-day supply.
Simplicity
The recommended dosage of icosapent ethyl is 2 g twice daily taken with food. It is available in 0.5-g or 1-g capsules. There is no titration or dose adjustment in patients with renal or hepatic failure.1
Bottom Line
Icosapent ethyl is safe, well-tolerated, and effective in preventing ischemic events, including stroke and heart attack. However, it is more expensive than other treatment options and should be considered only in adult patients treated with statins who have triglyceride levels of at least 150 mg per dL and either established CVD or type 2 diabetes with at least two additional risk factors for CVD.

