Sexual violence is a major public health and human rights issue affecting more than 40% of women in the United States during their lifetimes. Although men and women experience sexual assault, women are at greatest risk. Populations uniquely impacted by sexual assault include adolescents; lesbian, gay, bisexual, transgender, and queer people; and active-duty military service members. Health consequences of sexual assault include sexually transmitted infections, risk of unintended pregnancy, high rates of mental health conditions (e.g., posttraumatic stress disorder), and development of chronic medical conditions (e.g., chronic pelvic pain). Family physicians care for sexual assault survivors at the time of the assault and years after, and care should follow a survivor-centered and trauma-informed framework. Multiple organizations recommend screening all women for a history of sexual violence; however, the U.S. Preventive Services Task Force recommends only universal intimate partner violence screening in women of reproductive age. A validated tool, such as the Two-Question Screening Tool, can be implemented. Initial care should include treatment of physical injuries, prophylaxis for sexually transmitted infections, immunizations, and the sensitive management of psychological issues. Clinicians must comply with state and local requirements for the use of evidence-gathering kits. Many hospitals have developed collection protocols and employ certified Sexual Assault Nurse Examiners or Sexual Assault Forensic Examiners. Prevention of sexual violence requires a comprehensive approach to address individual, relational, community, and societal factors.
Definitions and Epidemiology
Sexual violence is a broad term that encompasses all sexual acts, committed or attempted, without consent or that occur when the person is unable to consent.1 The World Health Organization recognizes sexual violence as a global public health and human rights issue with far-reaching health consequences.2 Sexual assault is a crime involving nonconsensual sexual contact or behavior, which includes rape or attempted rape, unwanted touching, and sexual coercion.1 In 2012, the Federal Bureau of Investigation developed a comprehensive definition of rape, including any penetration (i.e., with a sexual organ or object) of a body orifice (e.g., vagina, anus, mouth) without consent.3 State laws related to sex crimes differ, and state-specific information is available in the Rape, Abuse and Incest National Network database (https://apps.rainn.org/policy/).
WHAT'S NEW ON THIS TOPIC
Sexual Assault of Women
The National Intimate Partner and Sexual Violence Survey revealed that 43.6% of women experienced sexual violence in their lifetimes, with one in five women experiencing rape or attempted rape.
Approximately 6% of women in the active-duty military reported experiencing sexual assault in the past year.
Among survivors of rape, 16% to 38% report the crime to law enforcement, with similar percentages presenting for medical evaluation.
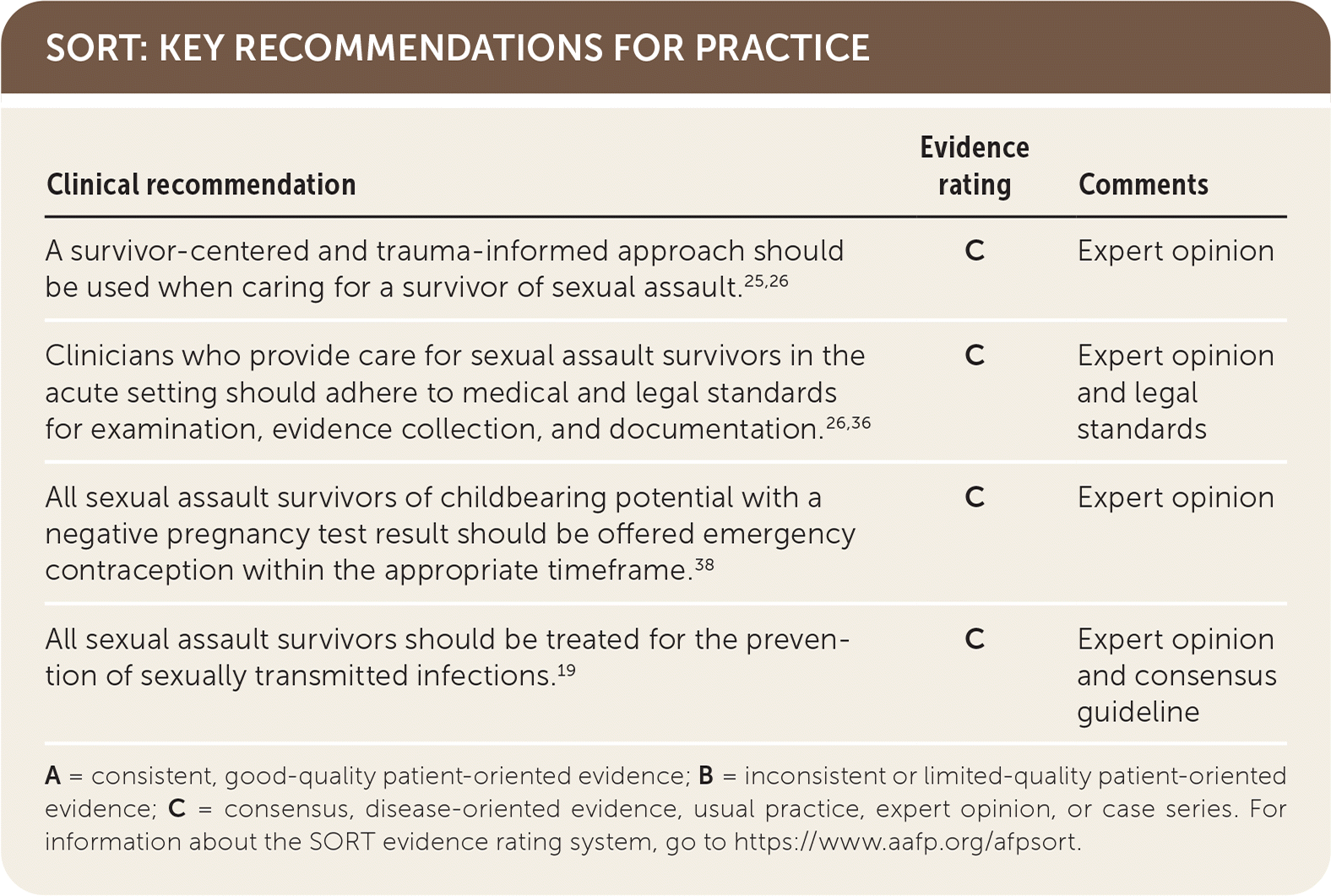
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Comments |
|---|---|---|
| A survivor-centered and trauma-informed approach should be used when caring for a survivor of sexual assault.25,26 | C | Expert opinion |
| Clinicians who provide care for sexual assault survivors in the acute setting should adhere to medical and legal standards for examination, evidence collection, and documentation.26,36 | C | Expert opinion and legal standards |
| All sexual assault survivors of childbearing potential with a negative pregnancy test result should be offered emergency contraception within the appropriate time frame.38 | C | Expert opinion |
| All sexual assault survivors should be treated for the prevention of sexually transmitted infections.19 | C | Expert opinion and consensus guideline |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Widespread underreporting of sexual assault impacts estimates of incidence and prevalence. The National Intimate Partner and Sexual Violence Survey reported that 43.6% of women experienced sexual violence in their lifetimes, with one in five women experiencing rape or attempted rape.4 Fifty to 80% of sexual assaults are committed by a person known to the survivor.5,6 This article focuses on women; however, sexual violence is increasingly reported among men, with one in four experiencing sexual violence during their lifetimes.4
Populations at increased risk include people who are physically or mentally disabled, adolescents, college students, homeless people, survivors of child maltreatment, people living in poverty, users of drugs or alcohol, people who engage in sex work, and people living in prisons, institutions, or areas of military conflict.4,7–10 Among women in the active-duty military, 6.2% surveyed reported experiencing sexual assault in the past year.11 Approximately one-half of transgender people and bisexual women experience sexual violence in their lifetimes.12,13 Lesbian, gay, bisexual, transgender, and queer populations face higher rates of hate-motivated violence, which can involve sexual assault, and are less likely to access the medical system, legal system, and support services because of discrimination and a fear of being “outed.”4,12 Children and adolescents are at risk of sexual violence, and American Family Physician has reviewed complexities unique to this population separately.14,15
Rape is the most underreported crime.4 Among survivors of rape, 16% to 38% report the crime to law enforcement, with similar percentages presenting for medical evaluation. Approximately two-thirds of survivors will disclose the assault to their primary care physician.16,17 This article reviews key aspects of clinical care for women who are sexual assault survivors. A reference to the American Academy of Family Physicians' policy statement on sexual assault and other recommended resources for clinicians are listed in Table 1.
TABLE 1. Resources for Family Physicians Treating Survivors of Sexual Assault
| American Academy of Family Physicians Policy statement on treatment of survivors of sexual assault https://www.aafp.org/about/policies/all/sexual-assault.html Policy statement on rights, protections, and support for survivors of sexual assault https://www.aafp.org/about/policies/all/sexual-assault-rights.html |
| FPM Journal Communication tips for caring for survivors of sexual assault https://www.aafp.org/fpm/2019/0700/p19.html |
| National Sexual Violence Resource Center Directory of sexual assault centers in the United States https://www.nsvrc.org/organizations or 877-739-3895 |
| Pennsylvania Coalition Against Rape Put down the chart, pick up the questions: a guide to working with survivors of sexual violence https://www.nsvrc.org/sites/default/files/2017-09/put_down_the_chart_pick_up_the_questions.pdf |
| Rape, Abuse and Incest National Sexual Assault Hotline (1-800-656-HOPE) Refers survivors to local rape crisis centers https://www.rainn.org/about-national-sexual-assault-telephone-hotline |
| Sexual Assault Forensic Examiner technical assistance Technical assistance and essential information about sexual assault medical forensic examinations https://www.safeta.org/ |
| U.S. Department of Justice, Office on Violence Against Women National protocol for sexual assault medical forensic examinations https://www.ncjrs.gov/pdffiles1/ovw/241903.pdf |
Health Sequelae of Sexual Assault
Sexual assault has short- and long-term consequences on women's physical, mental, sexual, and reproductive health. Short-term health implications include physical injuries, sexually transmitted infections (STIs), and pregnancy. Acute physical injuries range in severity from abrasions and bruises to concussions, fractures, and bullet wounds. The likelihood of pregnancy after sexual assault is approximately 5%, with higher rates among adolescents.18 When rape does result in pregnancy, patients are more likely to choose to terminate the pregnancy than to continue it.17 The risk of acquiring an STI after sexual assault is influenced by local prevalence rates and the type of assault.5 The most common STIs reported in sexual assault survivors are Chlamydia trachomatis, gonorrhea, and trichomoniasis. Chlamydia and gonorrhea may lead to pelvic inflammatory disease and infertility if untreated. The risk of HIV transmission from vaginal intercourse is 0.1% to 0.2% and for receptive anal intercourse is 0.5% to 3% and may be increased with mucosal trauma.19
Long-term physical sequelae of sexual assault may include chronic pelvic pain, other chronic pain syndromes, headaches, irritable bowel syndrome, and fibromyalgia. These conditions are more likely to present with sexual dysfunction, dysmenorrhea, and menorrhagia.20 Sexual assault survivors may experience more pain with speculum insertion during a routine pelvic examination.21
Posttraumatic stress disorder (PTSD) is the most common psychological sequela of sexual assault, with rates of 30% to 65%. Predictors of PTSD severity include characteristics of the assault and negative experiences related to disclosure. Ethnic minorities experienced more negative reactions related to disclosure and were more likely to experience PTSD.22,23 For military service members, military sexual trauma is directly related to developing PTSD.24 Survivors experience higher rates of depression, anxiety, substance use disorders, eating disorders, sleep disorders, contemplation of suicide, and attempted suicide.22,23
Trauma-Informed Care as a Framework
A survivor-centered and trauma-informed approach should be used when caring for a survivor of sexual assault.25,26 Clinicians must be able to recognize trauma, understand its short- and long-term health implications, and provide a safe and supportive environment when caring for sexual assault survivors. Trauma-informed services require a shift from thinking ‘What is wrong with you?’ to considering ‘What happened to you?’ The Substance Abuse and Mental Health Services Administration has outlined a framework of trauma-informed care that can be adapted to clinical settings by adhering to the four Rs: (1) Realize the effects of trauma and understand paths to recovery, (2) Recognize signs and symptoms of trauma, (3) Respond by integrating knowledge about trauma into policies and practices, and (4) actively avoid Retraumatization. The principles of this framework and examples of clinical application are listed in Table 2.25,27 Using this framework can improve the patient experience, optimize patient-clinician relationships, and improve health outcomes.27–29
TABLE 2. Substance Abuse and Mental Health Services Administration's Principles of Trauma-Informed Care

| Principle and description | Examples |
|---|---|
| Safety Physical and psychological | Always meet with the patient in a private space Knock on the door and ask permission to enter the room Meet with the patient before they disrobe and only ask them to disrobe when necessary Use empowering language such as “thank you for telling me” and “it took a lot of courage to share this with me” Ask permission before touching the patient for the examination and avoid using physical contact (e.g., hugs, hand on arm or shoulder) to express concern |
| Trustworthiness and transparency Build and maintain trust with the treatment team | Train all members of the team in trauma-informed care Tell the patient what to expect during and after the visit, including timing Explain all recommendations and the reasoning behind them Allow time for questions and ask the patient how they would like you to proceed Introduce all members of the team that might be involved in the patient's care (e.g., nurse chaperone, nurse calling with results after the visit) |
| Peer support Involve trauma survivors in care to help establish safety and hope for the future | Connect the patient with community-based resources |
| Collaboration and mutuality Work to level power differential; survivor and all members of the care team work as a team | Avoid using medical jargon Be mindful of body language (e.g., face the patient rather than the computer, sit when possible) Use supportive language such as “I'm here to listen and help you in any way that I can” and “How can I best support you?” Elicit the patient's concerns and worries and incorporate them into your care Share all information |
| Empowerment, voice, and choice Focus on shared decision-making | Explain rationale for all elements of the visit and obtain consent before proceeding Offer choices and respect the patient's decisions about their care Use empowering language such as “I want you to feel in control and safe. How can you let me know if you need a break or to stop?” |
| Cultural, historical, and gender issues Incorporate survivor's individual context and values into care | Elicit the patient's values and ask how they might impact care |
Screening
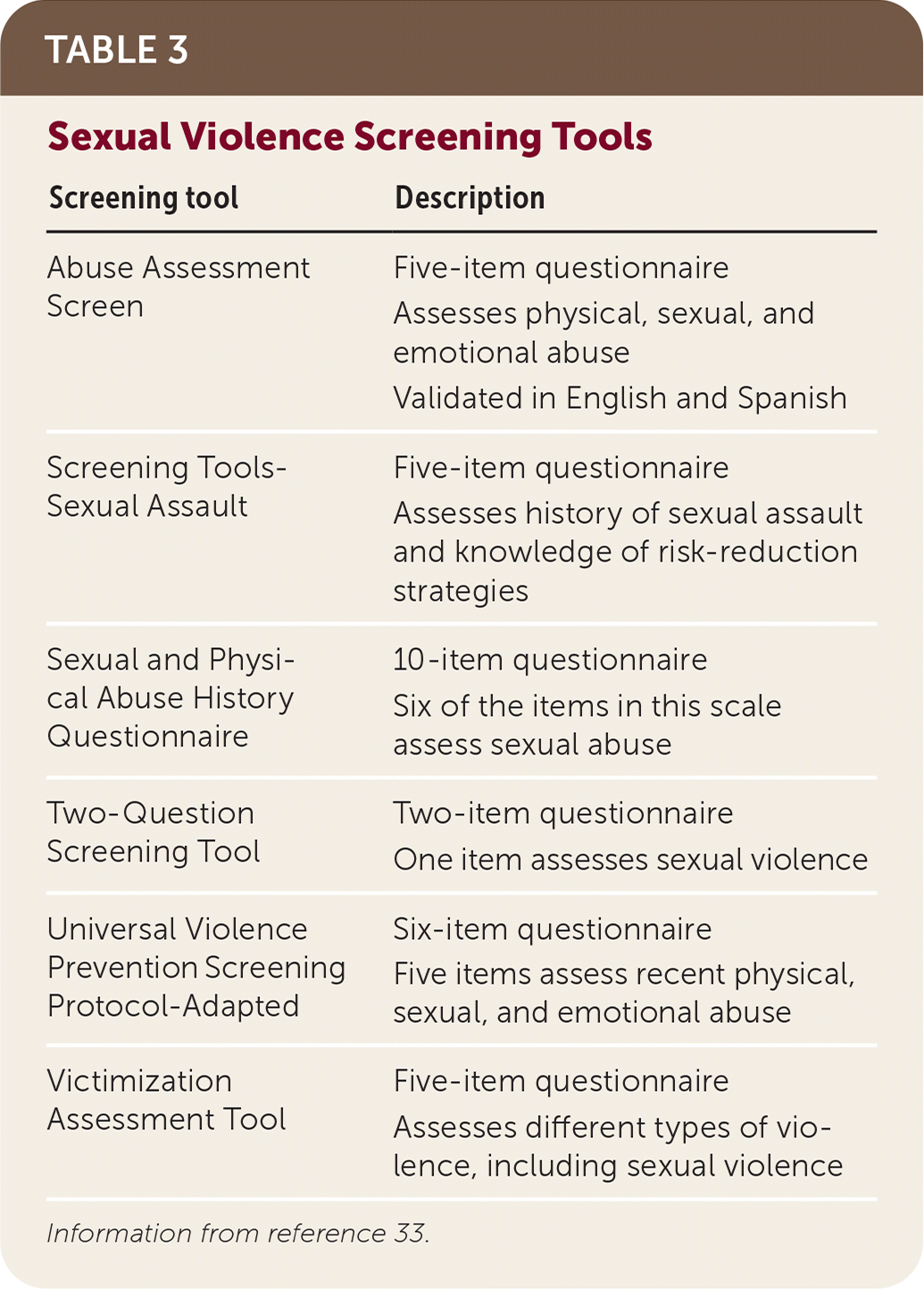
The World Health Organization, American Medical Association, and American College of Obstetricians and Gynecologists recommend screening all women for a history of sexual violence.25 Although the U.S. Preventive Services Task Force recommends universal intimate partner violence screening in women of reproductive age, they do not provide guidance on broader sexual violence screening.30 Many women are unlikely to disclose sexual assault unless asked, and most survivors would prefer for clinicians to screen for a history of sexual violence.31,32 Screening tools to identify sexual violence survivors are outlined in Table 3.33 The Two-Question Screening Tool is a validated tool that can be implemented in primary care. It includes one screening question each for intimate partner violence and sexual violence: Have you ever been hit, slapped, kicked, or otherwise physically hurt by your partner? Have you ever been forced to have sexual activities?33
TABLE 3. Sexual Violence Screening Tools
| Screening tool | Description |
|---|---|
| Abuse Assessment Screen | Five-item questionnaire Assesses physical, sexual, and emotional abuse Validated in English and Spanish |
| Screening Tools-Sexual Assault | Five-item questionnaire Assesses history of sexual assault and knowledge of risk-reduction strategies |
| Sexual and Physical Abuse History Questionnaire | 10-item questionnaire Six of the items in this scale assess sexual abuse |
| Two-Question Screening Tool | Two-item questionnaire One item assesses sexual violence |
| Universal Violence Prevention Screening Protocol-Adapted | Six-item questionnaire Five items assess recent physical, sexual, and emotional abuse |
| Victimization Assessment Tool | Five-item questionnaire Assesses different types of violence, including sexual violence |
Information from reference 33.
Screening tools are limited by the survivor's readiness for disclosure. Some survivors disclose details immediately, but others may disclose long after the event.32 Clinicians should develop consistent, effective practices for responding to disclosures of sexual victimization. The SAVE (screen, ask, validate, evaluate) method is one model protocol25,34 (Table 434).
TABLE 4. SAVE Model

| Components | Tips for implementation into practice |
|---|---|
| SCREEN all patients for sexual assault | Assure confidentiality Assure patients that sexual violence will not be reported unless a dependent person is currently at risk or the survivor wishes to report it |
| ASK direct questions in a nonjudgmental way | Normalize the topic of sexual violence Avoid formal or technical language Make eye contact Do not minimize the experience Never blame a patient for sexual violence they have experienced, even if they blame themselves |
| VALIDATE the patient | Use language that validates, supports and empowers such as: Thank you for telling me. It took a lot of courage to share this with me. I am really sorry that happened to you. It is not your fault. You did not do anything to deserve this. You are not alone. I care about you. I am here to listen or help in any way I can. You decide what you think is best for you. |
| EVALUATE, educate, and refer | Evaluate for present danger from the assailant Evaluate for how this is impacting the patient physically and psychologically Evaluate for psychological safety and suicidal ideations Refer the patient to survivor advocacy and crisis support agencies Offer referral to counseling and mental health services based on the patients' needs |
Information from reference 34.
Evaluation of Acute Presentation
Most sexual assault survivors who present acutely will go to an urgent care center or emergency department. If patients contact their physician before visiting their office, the patients' concerns must be heard, and their autonomy supported. Patients should receive information on where to report for care and be advised that bathing, changing clothes, urinating, defecating, douching, and delays in seeking care could alter evidence collection.35
On presentation, informed consent should always be obtained before evaluation or evidence collection.35 Initial assessment includes evaluation for life-threatening conditions, serious injuries, or psychiatric emergencies. Patients may require urgent stabilization and hospitalization or surgery. When assessing and treating injuries, precautions should be taken to prevent destruction or contamination of evidence (e.g., wear nonpowdered gloves, avoid obtaining urine specimens, avoid giving oral or rectal medications unless needed for stabilization).26
Family physicians may be the first point of contact for sexual assault survivors presenting to care. Clinicians who evaluate survivors acutely must adhere to medical and legal requirements, and those with limited or no experience should request assistance from trained personnel. The medical forensic examination, collection of evidence, and documentation should be performed by a health care professional trained in the medical and legal requirements for evidence collection whenever possible because improper collection can lead to the inability to prosecute a case.35–37 Many hospitals have developed protocols and employed certified Sexual Assault Nurse Examiners or Sexual Assault Forensic Examiners to ensure survivors receive trauma-informed care while meeting these requirements. If trained personnel are unavailable, clinicians can seek technical assistance by calling the SAFE Technical Assistance program and accessing a detailed protocol from the U.S. Department of Justice's Office on Violence Against Women.35–37 If a transfer of care is indicated, efforts should be made to minimize delay and loss of evidence. Family physicians can offer to stay with the survivor to provide support in the transfer process.
A complete history is crucial. The clinician should use a supportive and nonjudgmental approach, and documentation should include the patient's own words. Details of the assault, including about sexual contact and exposure to bodily fluids, should be documented. A gynecologic history is pertinent, including disclosure of last consensual sex.
The physical examination begins with an assessment of injuries. Physical injuries are noted in approximately one-half of all reported sexual assaults, with nongenital injuries more common than genital ones.17 The clinician should perform a detailed examination of the entire body and photograph or draw injuries. In the absence of major trauma, evidence collection is done concurrently with the physical examination.26
Collection of Evidence
Sexual assault evidence kits, or rape kits, are packages used to collect evidence from a survivor during a medical forensic examination. These kits are standardized and contain forms for documentation, bags and paper sheets for evidence collection, a comb, envelopes, materials for blood samples, swabs, and instructions. Clinicians should document what evidence is collected, when, and by whom.36
Diagnosis and Treatment
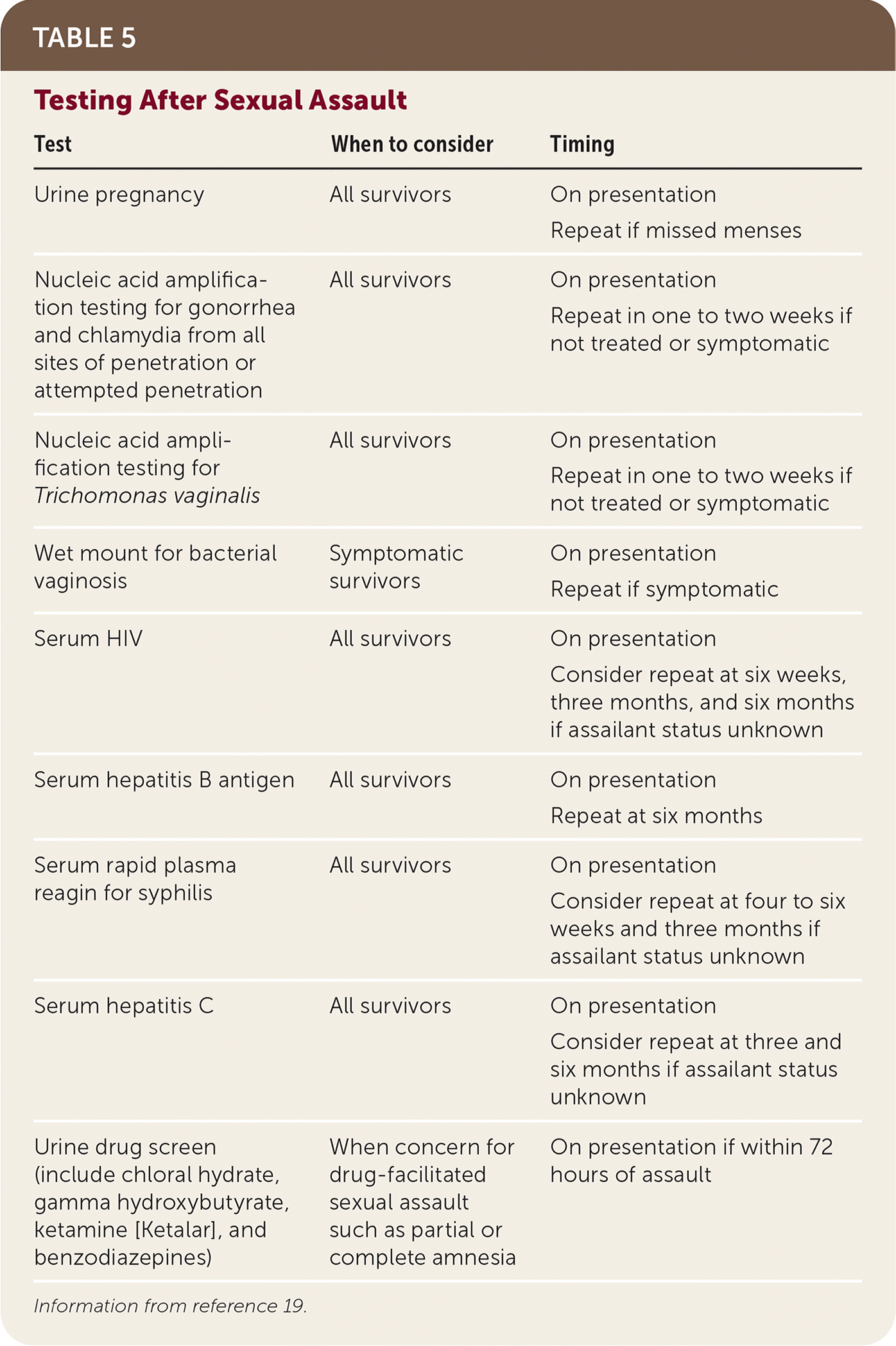
Diagnostic testing should be based on the nature of an assault and possible exposures.35 Table 5 includes diagnostic testing pertinent to the medical evaluation of sexual assault survivors.19
TABLE 5. Testing After Sexual Assault
| Test | When to consider | Timing |
|---|---|---|
| Urine pregnancy | All survivors | On presentation Repeat if missed menses |
| Nucleic acid amplification testing for gonorrhea and chlamydia from all sites of penetration or attempted penetration | All survivors | On presentation Repeat in one to two weeks if not treated or symptomatic |
| Nucleic acid amplification testing for Trichomonas vaginalis | All survivors | On presentation Repeat in one to two weeks if not treated or symptomatic |
| Wet mount for bacterial vaginosis | Symptomatic survivors | On presentation Repeat if symptomatic |
| Serum HIV | All survivors | On presentation Consider repeat at six weeks, three months, and six months if assailant status unknown |
| Serum hepatitis B antigen | All survivors | On presentation Repeat at six months |
| Serum rapid plasma reagin for syphilis | All survivors | On presentation Consider repeat at four to six weeks and three months if assailant status unknown |
| Serum hepatitis C | All survivors | On presentation Consider repeat at three and six months if assailant status unknown |
| Urine drug screen (include chloral hydrate, gamma hydroxybutyrate, ketamine [Ketalar], and benzodiazepines) | When concern for drug-facilitated sexual assault such as partial or complete amnesia | On presentation if within 72 hours of assault |
Information from reference 19.
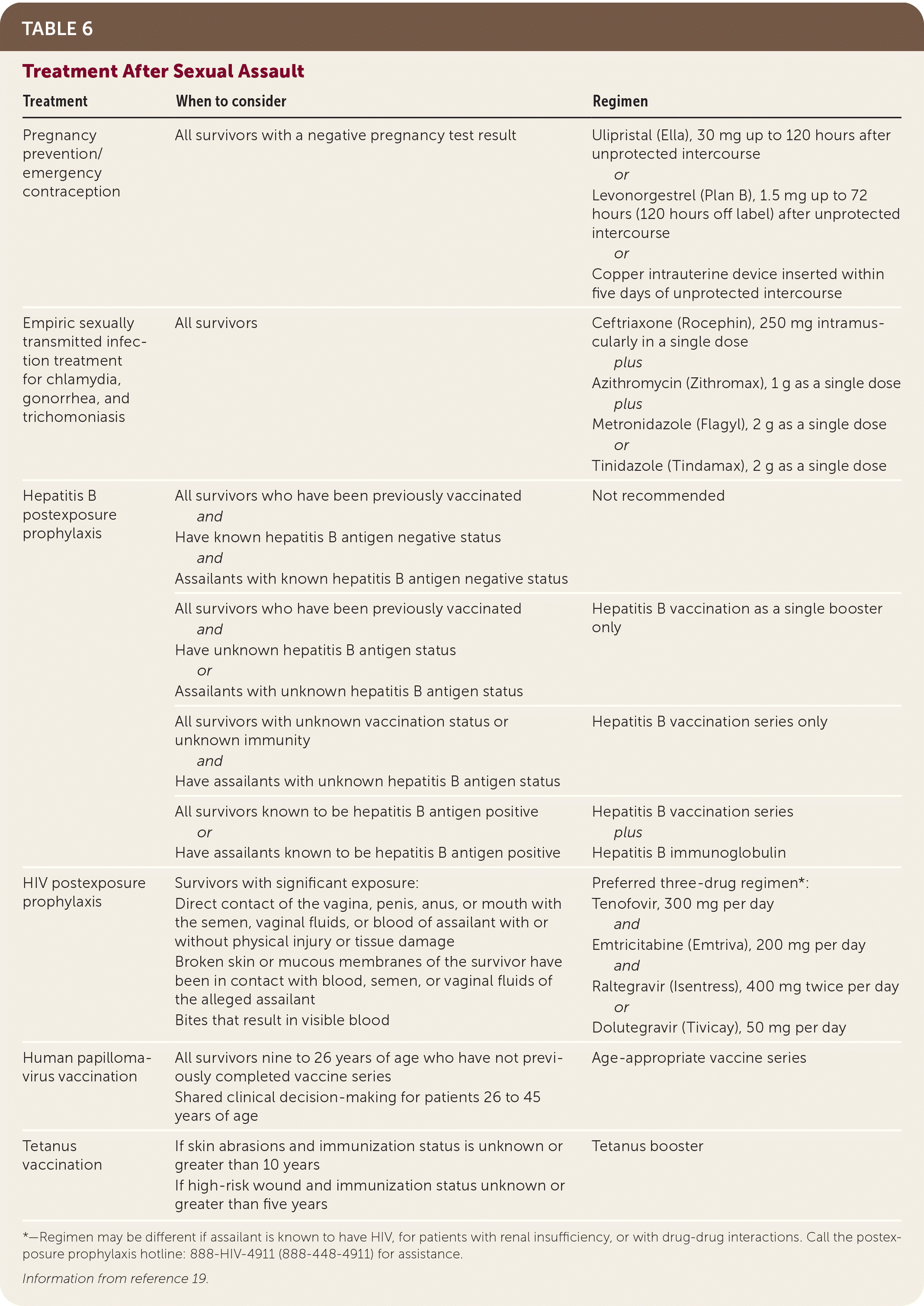
All sexual assault survivors should receive timely treatment for pregnancy and disease prevention, as indicated (Table 6).19 All sexual assault survivors of childbearing age with a negative urine pregnancy test at the time of presentation should be offered emergency contraception within the appropriate time frame.38 The Centers for Disease Control and Prevention released guidelines for the prevention and treatment of STIs for survivors of sexual assault. Empiric treatment against chlamydia, gonorrhea, and trichomoniasis is recommended for all survivors.19 Postexposure prophylaxis against HIV should be recommended based on the type of exposure and HIV status of the assailant (if known). Postexposure prophylaxis against hepatitis B with hepatitis B vaccine, with or without hepatitis B immunoglobulin, may be indicated depending on the assailant's hepatitis status and the survivor's vaccination status. Human papillomavirus vaccination is recommended for female survivors nine to 26 years of age who have not previously received the vaccination and for some survivors (ages 26 to 45 years) based on shared clinical decision-making.19,39 Tetanus vaccination is recommended for patients with breaks in the skin or mucosa based on vaccination status (Table 6).19
TABLE 6. Treatment After Sexual Assault
| Treatment | When to consider | Regimen |
|---|---|---|
| Pregnancy prevention/emergency contraception | All survivors with a negative pregnancy test result | Ulipristal (Ella), 30 mg up to 120 hours after unprotected intercourse or Levonorgestrel (Plan B), 1.5 mg up to 72 hours (120 hours off label) after unprotected intercourse or Copper intrauterine device inserted within five days of unprotected intercourse |
| Empiric sexually transmitted infection treatment for chlamydia, gonorrhea, and trichomoniasis | All survivors | Ceftriaxone (Rocephin), 500 mg intramuscularly in a single dose plus Doxycycline, 100 mg orally twice daily for 7 days plus Metronidazole (Flagyl), 2 g as a single dose or Tinidazole (Tindamax), 2 g as a single dose |
| Hepatitis B postexposure prophylaxis | All survivors who have been previously vaccinated and Have known hepatitis B antigen negative status and Assailants with known hepatitis B antigen negative status | Not recommended |
| All survivors who have been previously vaccinated and Have unknown hepatitis B antigen status or Assailants with unknown hepatitis B antigen status | Hepatitis B vaccination as a single booster only | |
| All survivors with unknown vaccination status or unknown immunity and Have assailants with unknown hepatitis B antigen status | Hepatitis B vaccination series only | |
| All survivors known to be hepatitis B antigen positive or Have assailants known to be hepatitis B antigen positive | Hepatitis B vaccination series plus Hepatitis B immunoglobulin | |
| HIV postexposure prophylaxis | Survivors with significant exposure: Direct contact of the vagina, penis, anus, or mouth with the semen, vaginal fluids, or blood of assailant with or without physical injury or tissue damage Broken skin or mucous membranes of the survivor have been in contact with blood, semen, or vaginal fluids of the alleged assailant Bites that result in visible blood | Preferred three-drug regimen*: Tenofovir, 300 mg per day and Emtricitabine (Emtriva), 200 mg per day and Raltegravir (Isentress), 400 mg twice per day or Dolutegravir (Tivicay), 50 mg per day |
| Human papillomavirus vaccination | All survivors nine to 26 years of age who have not previously completed vaccine series Shared clinical decision-making for patients 26 to 45 years of age | Age-appropriate vaccine series |
| Tetanus vaccination | If skin abrasions and immunization status is unknown or greater than 10 years If high-risk wound and immunization status unknown or greater than five years | Tetanus booster |
*—Regimen may be different if assailant is known to have HIV, for patients with renal insufficiency, or with drug-drug interactions. Call the postexposure prophylaxis hotline: 888-HIV-4911 (888-448-4911) for assistance.
Delayed Presentation
Delayed presentation is common, particularly when the initial disclosure is in the primary care setting.40 One study of women receiving mental health services for childhood sexual assault reported an average time to disclosure of 16 years.31 A systematic review of health care professionals' responses to delayed sexual assault disclosures characterized helpful and unhelpful responses. Helpful responses included validating the disclosure, providing emotional support, and providing tangible aid and informational support. Unhelpful responses included blaming the survivor, minimizing or dismissing the experience, and treating the survivor differently after disclosure.40
Prevention
Primary prevention of sexual violence requires a comprehensive approach with interventions to address individual, relational, community, and societal factors. The Centers for Disease Control and Prevention has developed STOP SV, a technical package highlighting effective strategies for prevention (Table 7).41 Effective programs confront public attitudes about love and sexuality and teach conflict resolution skills. Programs mobilizing boys and men as allies and focusing on bystander approaches can prevent sexual violence. Empowerment-based training for college-aged women has been shown to decrease the risk of victimization. Transportation policies, campus safety programs, and crime prevention programs have been shown to decrease the incidence of sexual assault.41
TABLE 7. Sexual Assault Prevention Strategies: STOP SV Mnemonic
| Strategy | Examples of an evidence-based approach | |
|---|---|---|
| S | Promote social norms that protect against violence | Bystander approaches can empower young people to intervene in peer groups Mobilizing boys and men as allies |
| T | Teach skills to prevent sexual violence | Implementing social-emotional learning to change the way children and adolescents think and feel about violence Promoting healthy sexuality through comprehensive sex education that includes consent and respect Teaching healthy safe dating and relationship skills to adolescents through effective programs like Safe Dates Empowerment-based training to increase participants' ability to identify and reduce exposure to risky situations |
| O | Provide opportunities to empower girls and women | Strengthening economic supports for women and families Strengthening opportunities for leadership and empowerment for girls |
| P | Create protective environments | Improving safe physical spaces and increasing staff monitoring in schools Establishing safe workplace policies and taking proactive measures to reduce harassment and violence in the workplace |
| SV | Support victims to lessen harms | Survivor-centered services like rape crisis centers Comprehensive treatment for sexual violence survivors, including mental health services Treatment for children who were exposed to violence in their homes and communities and are at risk of violence perpetration |
Adapted from Basile KC, DeGue S, Jones K, et al. STOP SV: a technical package to prevent sexual violence. Atlanta: National Center for Injury Prevention and Control; Centers for Disease Control and Prevention; 2016:11. Accessed August 26, 2020. https://www.cdc.gov/violenceprevention/pdf/sv-prevention-technical-package.pdf
Early recognition by clinicians after sexual assault and effective support and care for survivors can help prevent adverse health sequelae and revictimization. Survivor-centered services such as rape crisis centers provide a healing environment and allow patients to connect to advocates and resources. Survivors who work with advocates report more positive experiences with the medical and legal systems.41 Clinicians can connect survivors to advocates through the National Sexual Assault Hotline (1-800-656-4673), which provides referrals to local rape crisis centers, and the National Sexual Violence Resource Center (https://www.nsvrc.org/), which maintains a directory of support organizations.
This article updates previous articles on this topic by Luce, et al.,42 and Petter and Whitehill.43
Data Sources: A PubMed search was completed on August 29, 2019, September 21, 2019, March 2, 2020, and August 26, 2020 using the key words sexual assault, sexual violence, and rape. On June 28, 2019 and August 26, 2020 we searched using an evidence summary generated by Essential Evidence Plus and the key words abuse, violence, sexual assault, and rape. Also searched were the Cochrane database and the U.S. Preventive Services Task Force using the key words sexual assault, sexual violence, and rape on September 21, 2019 and August 26, 2020.

