Health maintenance for women of reproductive age includes counseling and screening tests that have been demonstrated to prevent disease and improve health. This article focuses mainly on conditions that are more common in women or have a unique impact on female patients. Family physicians should be familiar with evidence-based recommendations for contraception and preconception care and should consider screening patients for pregnancy intention. The American Academy of Family Physicians recommends against screening pelvic examinations in asymptomatic women; the U.S. Preventive Services Task Force (USPSTF) found insufficient evidence to make a recommendation for or against screening pelvic examinations. The USPSTF recommendations for women in this age group include screening for obesity and other cardiovascular risk factors, depression, intimate partner violence, cervical cancer, HIV, hepatitis C virus, tobacco use, and unhealthy alcohol and drug use as part of routine primary care. Breast cancer screening with mammography is recommended for women 50 years and older and should be individualized for women 40 to 49 years of age, although other organizations recommend earlier screening. Screening for sexually transmitted infections is based on age and risk factors; women younger than 25 years who are sexually active should be screened routinely for gonorrhea and chlamydia, whereas screening for syphilis and hepatitis B virus should be individualized. Immunizations should be recommended according to guidelines from the Centers for Disease Control and Prevention and the Advisory Committee on Immunization Practices; immunizations against influenza; tetanus; measles, mumps, and rubella; varicella; meningococcus; and human papillomavirus are of particular importance in women of reproductive age. To have the greatest impact on health, physicians should focus on USPSTF grade A and B recommendations with patients.
Health maintenance for women of reproductive age (generally defined as 15 to 44 years of age) comprises counseling and screening tests, with the goal of prevention and early detection of common diseases such as cancer, infections, and mental health issues. A systematic review found no evidence that general preventive visits (outside of condition-based screening recommendations) reduce overall mortality or deaths from conditions such as cancer or heart disease1; however, it is still important for family physicians to continue evidence-based preventive services, whether part of a routine physical examination or separately.2 This article focuses on screening and counseling for conditions that are more prevalent in women of this age or that have a unique impact on women. In most cases, recommendations from the American Academy of Family Physicians (AAFP) are aligned with those from the U.S. Preventive Services Task Force (USPSTF); this article states when recommendations differ. A full list of USPSTF recommendations is published on their website.3 Grade A and B recommendations (https://www.uspreventiveservicestaskforce.org/uspstf/grade-definitions) have the strongest evidence of benefit and are the focus of this article. Physicians can also sign up to receive regular email updates with new or draft recommendations. A list of smart-phone apps related to preventive care is provided in Table 1.
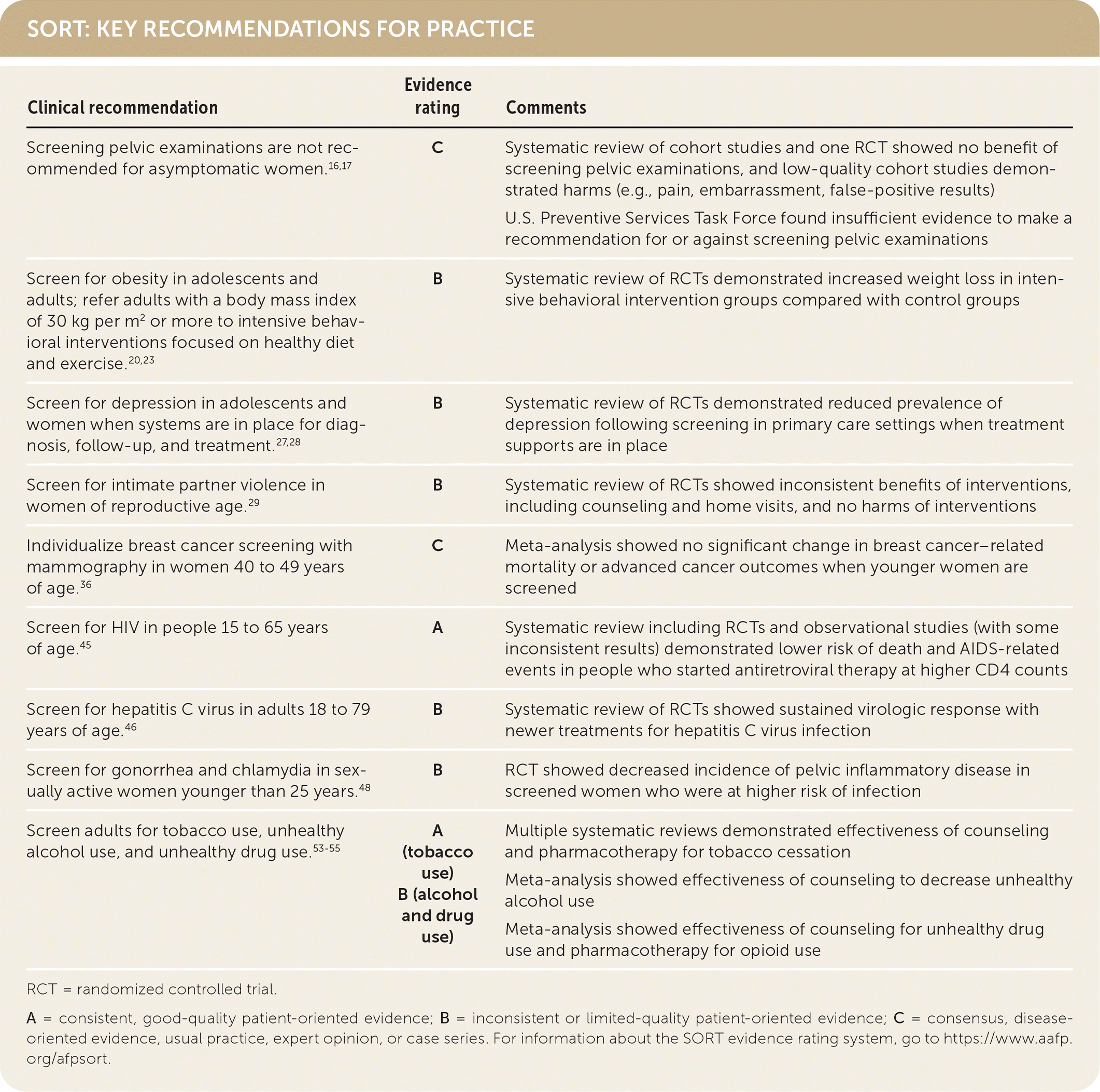
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Comments |
|---|---|---|
| Screening pelvic examinations are not recommended for asymptomatic women.16,17 | C | Systematic review of cohort studies and one RCT showed no benefit of screening pelvic examinations, and low-quality cohort studies demonstrated harms (e.g., pain, embarrassment, false-positive results) U.S. Preventive Services Task Force found insufficient evidence to make a recommendation for or against screening pelvic examinations |
| Screen for obesity in adolescents and adults; refer adults with a body mass index of 30 kg per m2 or more to intensive behavioral interventions focused on healthy diet and exercise.20,23 | B | Systematic review of RCTs demonstrated increased weight loss in intensive behavioral intervention groups compared with control groups |
| Screen for depression in adolescents and women when systems are in place for diagnosis, follow-up, and treatment.27,28 | B | Systematic review of RCTs demonstrated reduced prevalence of depression following screening in primary care settings when treatment supports are in place |
| Screen for intimate partner violence in women of reproductive age.29 | B | Systematic review of RCTs showed inconsistent benefits of interventions, including counseling and home visits, and no harms of interventions |
| Individualize breast cancer screening with mammography in women 40 to 49 years of age.36 | C | Meta-analysis showed no significant change in breast cancer–related mortality or advanced cancer outcomes when younger women are screened |
| Screen for HIV in people 15 to 65 years of age.45 | A | Systematic review including RCTs and observational studies (with some inconsistent results) demonstrated lower risk of death and AIDS-related events in people who started antiretroviral therapy at higher CD4 counts |
| Screen for hepatitis C virus in adults 18 to 79 years of age.46 | B | Systematic review of RCTs showed sustained virologic response with newer treatments for hepatitis C virus infection |
| Screen for gonorrhea and chlamydia in sexually active women younger than 25 years.48 | B | RCT showed decreased incidence of pelvic inflammatory disease in screened women who were at higher risk of infection |
| Screen adults for tobacco use, unhealthy alcohol use, and unhealthy drug use.53–55 | A (tobacco use) | Multiple systematic reviews demonstrated effectiveness of counseling and pharmacotherapy for tobacco cessation |
| Meta-analysis showed effectiveness of counseling to decrease unhealthy alcohol use | ||
| Meta-analysis showed effectiveness of counseling for unhealthy drug use and pharmacotherapy for opioid use | ||
| B (alcohol and drug use) |
RCT = randomized controlled trial.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
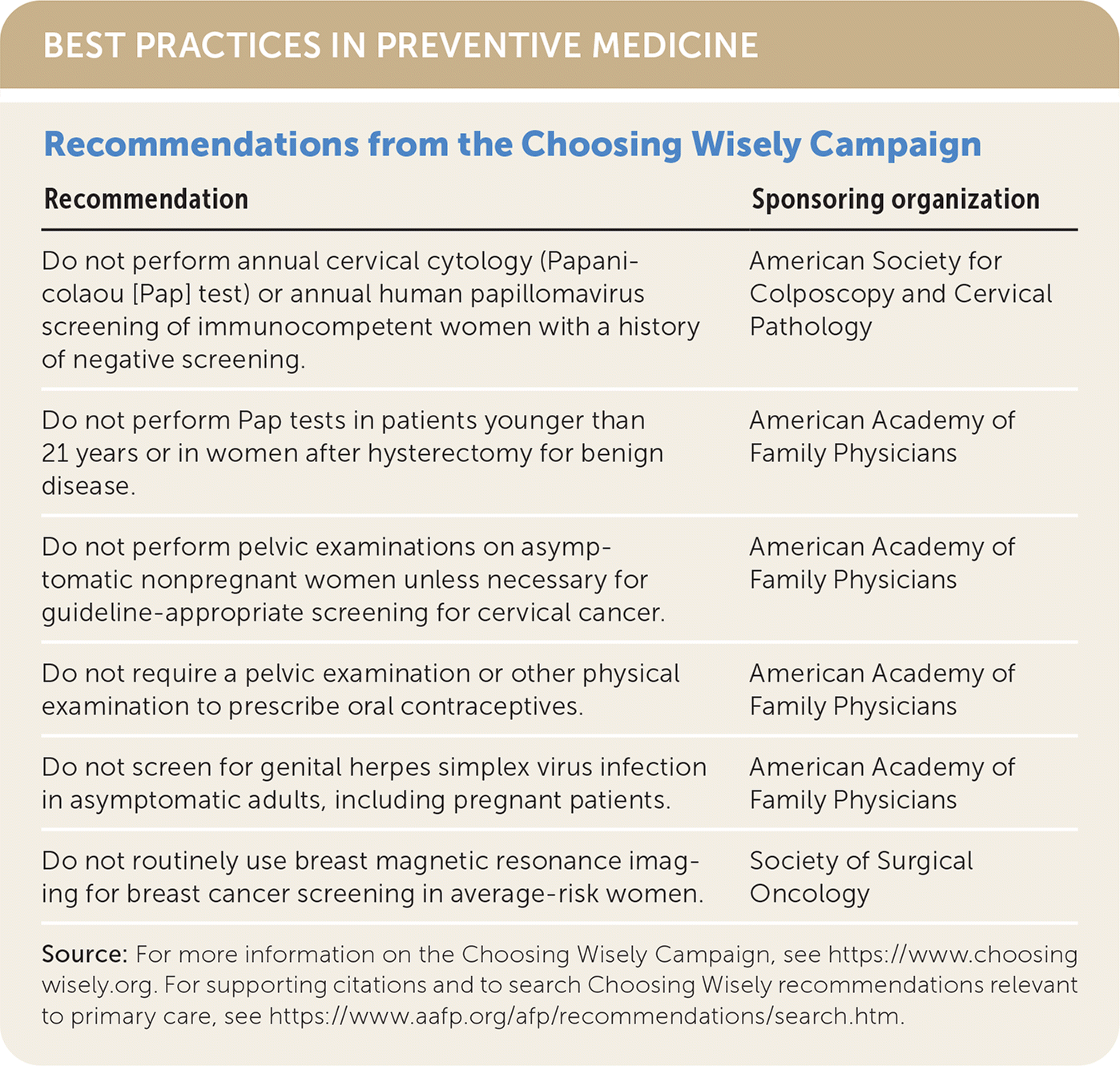
BEST PRACTICES IN PREVENTIVE MEDICINE
| Recommendation | Sponsoring organization |
|---|---|
| Do not perform annual cervical cytology (Papanicolaou [Pap] test) or annual human papillomavirus screening of immunocompetent women with a history of negative screening. | American Society for Colposcopy and Cervical Pathology |
| Do not perform Pap tests in patients younger than 21 years or in women after hysterectomy for benign disease. | American Academy of Family Physicians |
| Do not perform pelvic examinations on asymptomatic nonpregnant women unless necessary for guideline-appropriate screening for cervical cancer. | American Academy of Family Physicians |
| Do not require a pelvic examination or other physical examination to prescribe oral contraceptives. | American Academy of Family Physicians |
| Do not screen for genital herpes simplex virus infection in asymptomatic adults, including pregnant patients. | American Academy of Family Physicians |
| Do not routinely use breast magnetic resonance imaging for breast cancer screening in average-risk women. | Society of Surgical Oncology |
Source: For more information on the Choosing Wisely Campaign, see https://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
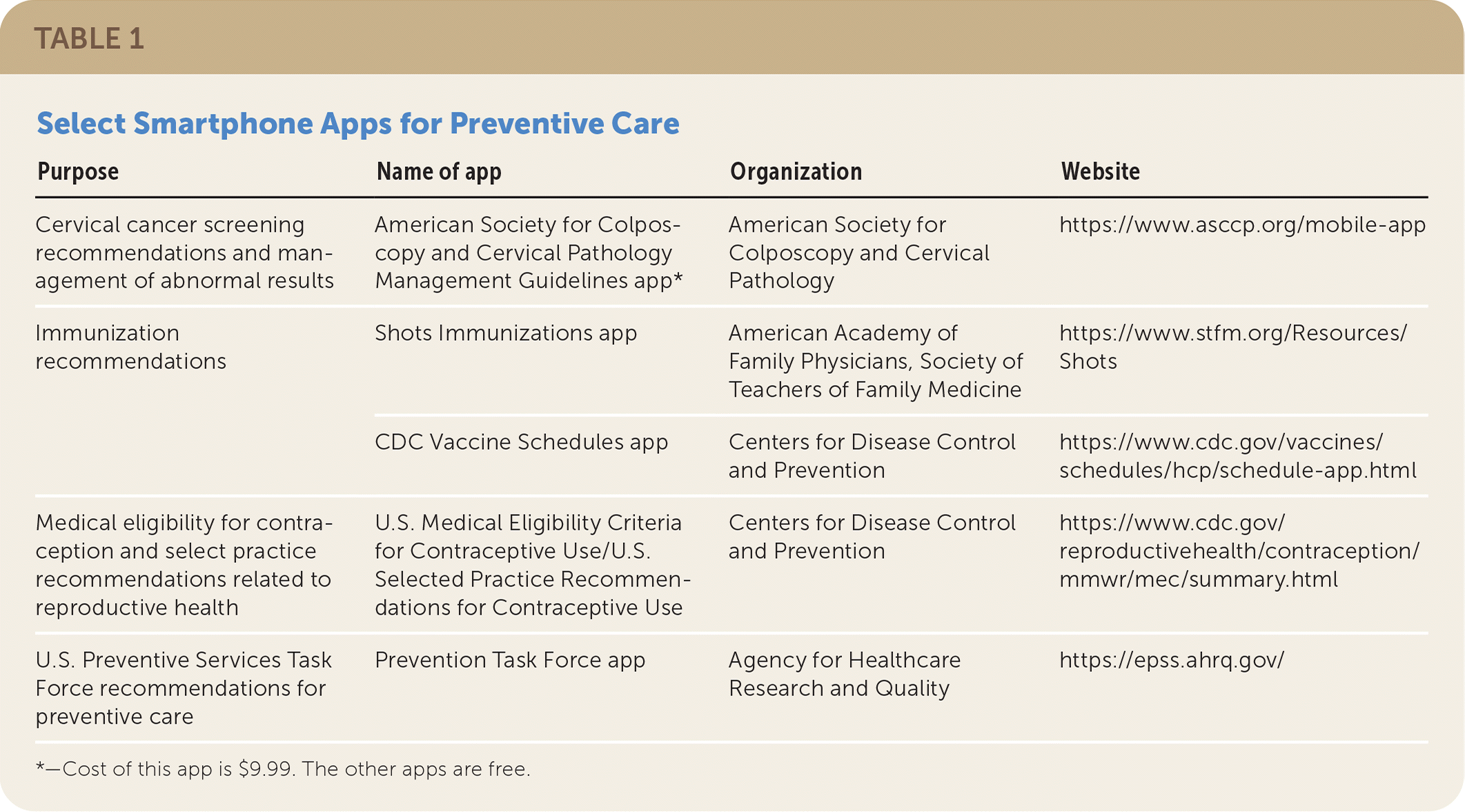
TABLE 1. Select Smartphone Apps for Preventive Care
| Purpose | Name of app | Organization | Website |
|---|---|---|---|
| Cervical cancer screening recommendations and management of abnormal results | American Society for Colposcopy and Cervical Pathology Management Guidelines app* | American Society for Colposcopy and Cervical Pathology | https://www.asccp.org/mobile-app |
| Immunization recommendations | Shots Immunizations app | American Academy of Family Physicians, Society of Teachers of Family Medicine | https://www.stfm.org/Resources/Shots |
| CDC Vaccine Schedules app | Centers for Disease Control and Prevention | https://www.cdc.gov/vaccines/schedules/hcp/schedule-app.html | |
| Medical eligibility for contraception and select practice recommendations related to reproductive health | U.S. Medical Eligibility Criteria for Contraceptive Use/U.S. Selected Practice Recommendations for Contraceptive Use | Centers for Disease Control and Prevention | https://www.cdc.gov/reproductivehealth/contraception/mmwr/mec/summary.html |
| U.S. Preventive Services Task Force recommendations for preventive care | Prevention Task Force app | Agency for Healthcare Research and Quality | https://epss.ahrq.gov/ |
*—Cost of this app is $9.99. The other apps are free.
Although this article uses the term “women” for simplicity, these recommendations apply to transgender men and nonbinary individuals as well. A previous American Family Physician article addresses health care for transgender and nonbinary patients in more detail.4 This article does not address recommendations that are specific to the antepartum or postpartum period.
Disparities exist in the provision of preventive care and are more common in people who belong to racial, ethnic, and sexual minority groups; people who are transgender; people who are uninsured; younger adults; and people who live in rural areas.5,6 Although some types of preventive care, such as breast cancer screening, have improved, disparities continue to exist, especially related to screening for sexually transmitted infections (STIs), HIV, and cervical cancer and to vaccination against human papillomavirus (HPV).7
Reproductive Planning
PREGNANCY INTENTION
In 2011, 45% of pregnancies in the United States were unintended at the time of conception.8 The Centers for Disease Control and Prevention (CDC) and the American College of Obstetricians and Gynecologists recommend screening for pregnancy intention as part of primary care visits.9,10 One method of screening that has been studied is the One Key Question.11 Patients are asked whether they would like to become pregnant in the next year. Those who answer yes should be offered preconception counseling. For those who answer no, physicians should initiate a contraceptive options discussion. For patients who are okay either way or are unsure, physicians should initiate further discussion of the patient's goals and preferences. Pilot studies have demonstrated the feasibility of using One Key Question in the primary care setting and found that its use leads to higher rates of contraception use and preconception counseling11; however, more evidence is needed to support this intervention as a population-based screening recommendation.
CONTRACEPTION
Women who want to have children often wish to plan the timing of their pregnancies. This makes the availability of effective contraception an important factor in achieving a person's goals.9 The CDC has developed a tool called the U.S. Medical Eligibility Criteria for Contraceptive Use, available as an app and on the CDC website; it allows physicians to easily determine eligibility or contraindications to various contraceptive methods based on the patient's health status.12
PRECONCEPTION AND INTERCONCEPTION CARE
If a woman desires pregnancy or is not actively trying to avoid pregnancy, preconception care is appropriate to try to reduce health risks and to maximize the chances of a healthy pregnancy, delivery, and infant. Interpregnancy or interconception care extends the concept of preconception care to maintain a woman's health across her reproductive life span. The AAFP has a position paper with evidence-based recommendations addressing preconception care.13 The American College of Obstetricians and Gynecologists and the Society for Maternal-Fetal Medicine have published a guideline that includes topics such as avoiding interpregnancy intervals of less than six months, breastfeeding recommendations, counseling about family planning, and screening for and prevention of other medical conditions, as recommended in this article.14 The USPSTF recommends prescription of folic acid for people who may become pregnant.15
Screening Pelvic Examinations
The AAFP recommends against screening pelvic examinations in asymptomatic women because there are potential harms of overtreatment and unnecessary testing and no known benefits from screening asymptomatic patients.16 The USPSTF found insufficient evidence to make a recommendation for or against screening pelvic examinations.17 The USPSTF recommends against screening for ovarian cancer, and screening pelvic examinations have been studied primarily for the purpose of ovarian cancer screening.18 The Prostate, Lung, Colorectal, and Ovarian cancer screening trial dropped pelvic examinations from its ovarian cancer screening algorithm after no cases of ovarian cancer were detected by pelvic examination.19
Obesity and Cardiovascular Risk
Obesity, defined as a body mass index (BMI) of 30 kg per m2 or higher, is more prevalent among women (40%) than men (35%) in the United States.20 Studies show a correlation between increased BMI in women 30 to 55 years of age and increased risk of mortality, as well as morbidities such as cardiovascular disease later in life.21 In women, obesity affects the reproductive cycle and is associated with an increased risk of infertility and polycystic ovary syndrome.22 Current USPSTF guidelines recommend that adults with a BMI of 30 kg per m2 or higher be provided with or referred for intensive multicomponent behavioral interventions.20 The USPSTF also recommends screening for obesity in adolescents.23
The USPSTF addresses screening recommendations for other cardiovascular disease risk factors, including hypertension, diabetes mellitus, and overall cardiovascular risk. These recommendations are summarized in eTable A.
eTABLE A USPSTF Recommendations on Screening for CVD Risk Factors

| Risk factor | USPSTF recommendation | Comments |
|---|---|---|
| Diabetes mellitus | Screen adults 40 to 70 years of age who are overweight or obese (B recommendation)A1 | Screening can be done with A1C level, fasting plasma glucose, or glucose tolerance test |
| Hypertension | Screen adults ≥ 18 years (A recommendation)A2 | Initial screening with office blood pressure measurement should be confirmed with ambulatory blood pressure measurement before starting treatment |
| Obesity | Refer adults with body mass index ≥ 30 kg per m2 for intensive behavioral intervention to promote healthy diet and exercise (B recommendation)A3 Screen adolescents for obesity (B recommendation)A4 | Adults who are overweight or obese with additional CVD risk factors should be referred for intensive behavioral counseling to promote healthy diet and exercise |
| Statin use | Prescribe statin therapy for primary prevention in adults 40 to 75 years of age with at least one CVD risk factor and a 10-year CVD event risk of 10% or higher (B recommendation)A5 | Risk stratification includes measurement of lipid levels Use the American College of Cardiology/American Heart Association pooled cohort equations to calculate CVD risk (http://tools.acc.org/ASCVD-Risk-Estimator-Plus/#!/calculate.estimate) |
CVD = cardiovascular disease; USPSTF = U.S. Preventive Services Task Force.
Information from:
A1. Siu AL. Screening for abnormal blood glucose and type 2 diabetes mellitus: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med. 2015;163(11):861–868.
A2. Siu AL. Screening for high blood pressure in adults: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med. 2015;163(10):778–786.
A3. Curry SJ, Krist AH, Owens DK, et al. Behavioral weight loss interventions to prevent obesity-related morbidity and mortality in adults: U.S. Preventive Services Task Force recommendation statement. JAMA. 2018;320(11):1163–1171.
A4. Grossman DC, Bibbins-Domingo K, Curry SJ, et al. Screening for obesity in children and adolescents: U.S. Preventive Services Task Force recommendation statement. JAMA. 2017;317(23):2417–2426.
A5. Bibbins-Domingo K, Grossman DC, Curry SJ, et al. Statin use for the primary prevention of cardiovascular disease in adults: U.S. Preventive Services Task Force recommendation statement [published corrections appear in JAMA. 2020;323(7):669–670]. JAMA. 2016;316(19):1997–2007.
Depression
Major depressive disorder is the leading cause of disability in women.24 The prevalence of depression in women is approximately two times higher than in men.25,26 This difference holds true among adults 20 years of age to older than 60 years, with the highest prevalence of depression occurring in women 40 to 59 years of age.26 The reasons for higher risk and prevalence of depression in women are not fully understood and are hypothesized to involve multiple biologic and environmental factors that are simultaneously at play.24,26 Current USPSTF guidelines recommend screening for depression in adults and adolescents when systems are in place to ensure follow-up, such as case management, direct depression care or coordination of care, and mental health treatment.27–29 Screening tests recommended by the USPSTF are the Patient Health Questionnaire for adults and the Geriatric Depression Scale for older adults.
Intimate Partner Violence
Intimate partner violence (IPV) is defined by the USPSTF as physical or sexual violence, psychological aggression, or stalking by a person with whom one has a close personal relationship (e.g., a spouse).29 In the 2015 National Intimate Partner and Sexual Violence Survey, 4.7% of women were found to have experienced sexual violence, physical violence, and/or stalking in the past year, and 43.6% of women had experienced sexual violence during their lifetime.30 The prevalence of IPV is highest among women of reproductive age. Current USPSTF guidelines recommend screening for IPV in all women of reproductive age and provision or referral of ongoing support services for those who screen positive.29 Validated screening instruments for IPV include the HARK (Humiliation, Afraid, Rape, Kick), HITS (Hurt, Insult, Threaten, Scream), E-HITS (Extended HITS), PVS (Partner Violence Screen), and WAST (Woman Abuse Screen Tool).29 Examples of the screening tools are reviewed in a previous American Family Physician article on IPV (https://www.aafp.org/afp/2016/1015/p646.html). The recommendations for screening were based predominantly on limited evidence showing benefit of interventions for pregnant and postpartum women29 but have been generalized to apply to nonpregnant women given the potential benefits of screening and the absence of harms.
Cancer Screening
CERVICAL CANCER
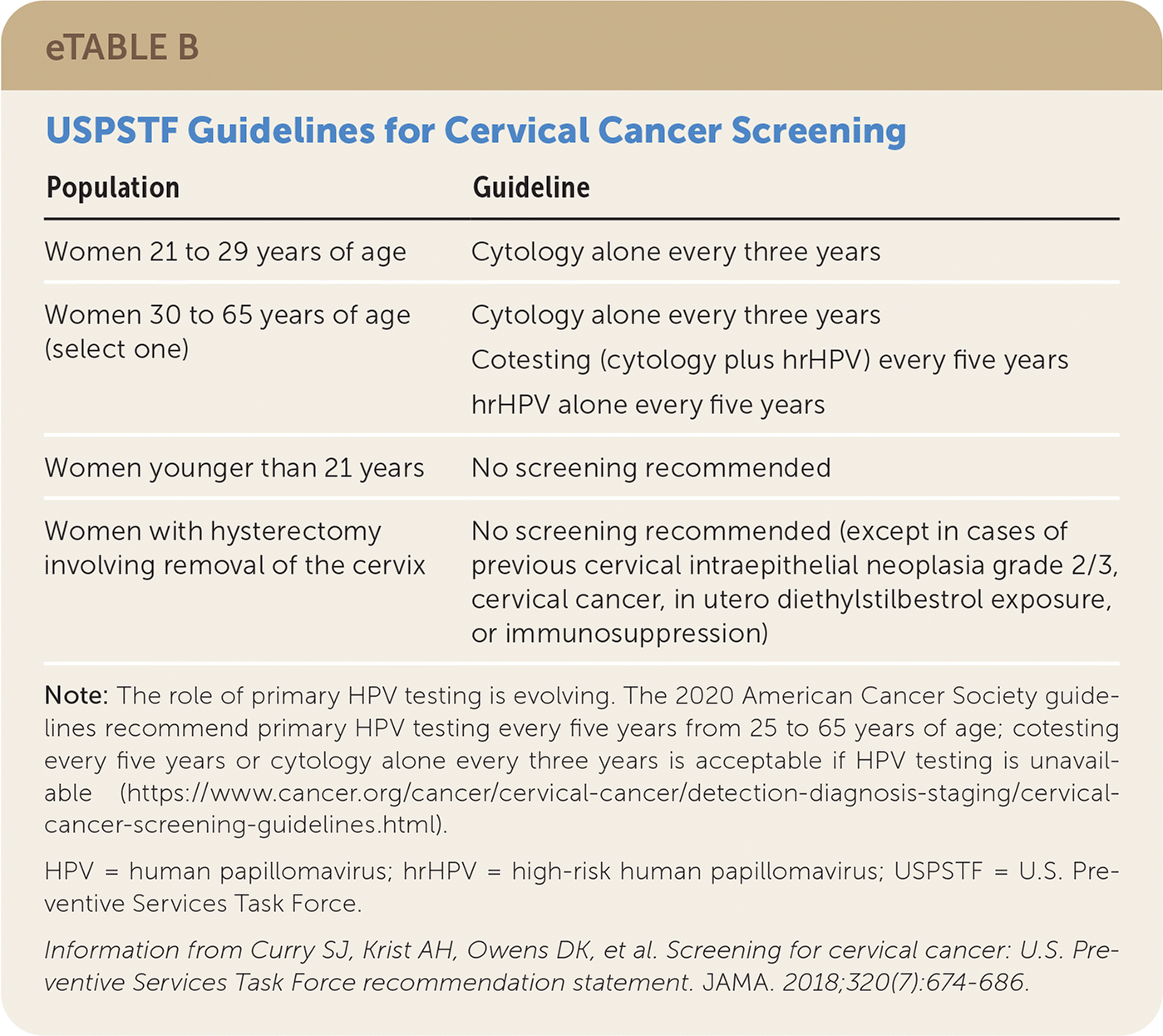
The CDC estimates that 93% of cervical cancers could be prevented by vaccination and screening.31 As of 2015, however, an estimated 14 million women 21 to 65 years of age had not been screened for cervical cancer within the past three years.32 Evidence suggests that in women 30 years and older, HPV infection is a better predictor of cervical cancer than cytology. In women younger than 30 years, HPV tends to be more transient, and the cervix has a greater potential for regeneration, making cytology more appropriate for screening. This difference is reflected in the USPSTF cervical cancer screening recommendations as well as recent interim clinical guidance from the American Society for Colposcopy and Cervical Pathology.33,34 The inclusion of primary HPV testing without cytology for women 30 years and older is a change from previous guidelines. USPSTF guidelines34 for cervical cancer screening are summarized in eTable B.
eTABLE B USPSTF Guidelines for Cervical Cancer Screening
| Population | Guideline |
|---|---|
| Women 21 to 29 years of age | Cytology alone every three years |
| Women 30 to 65 years of age (select one) | Cytology alone every three years |
| Cotesting (cytology plus hrHPV) every five years | |
| hrHPV alone every five years | |
| Women younger than 21 years | No screening recommended |
| Women with hysterectomy involving removal of the cervix | No screening recommended (except in cases of previous cervical intraepithelial neoplasia grade 2/3, cervical cancer, in utero diethylstilbestrol exposure, or immunosuppression) |
Note: The role of primary HPV testing is evolving. The 2020 American Cancer Society guidelines recommend primary HPV testing every five years from 25 to 65 years of age; cotesting every five years or cytology alone every three years is acceptable if HPV testing is unavailable (https://www.cancer.org/cancer/cervical-cancer/detection-diagnosis-staging/cervical-cancer-screening-guidelines.html).
HPV = human papillomavirus; hrHPV = high-risk human papillomavirus; USPSTF = U.S. Preventive Services Task Force.
Information from Curry SJ, Krist AH, Owens DK, et al. Screening for cervical cancer: U.S. Preventive Services Task Force recommendation statement. JAMA. 2018;320(7):674–686.
Emerging research shows that using patient self-collection of samples for HPV testing may be equally effective and increase screening rates compared with samples collected by a health care professional.35 However, at this time, neither the USPSTF nor the American Society for Colposcopy and Cervical Pathology recommends self-sampling until more data are available.
BREAST CANCER
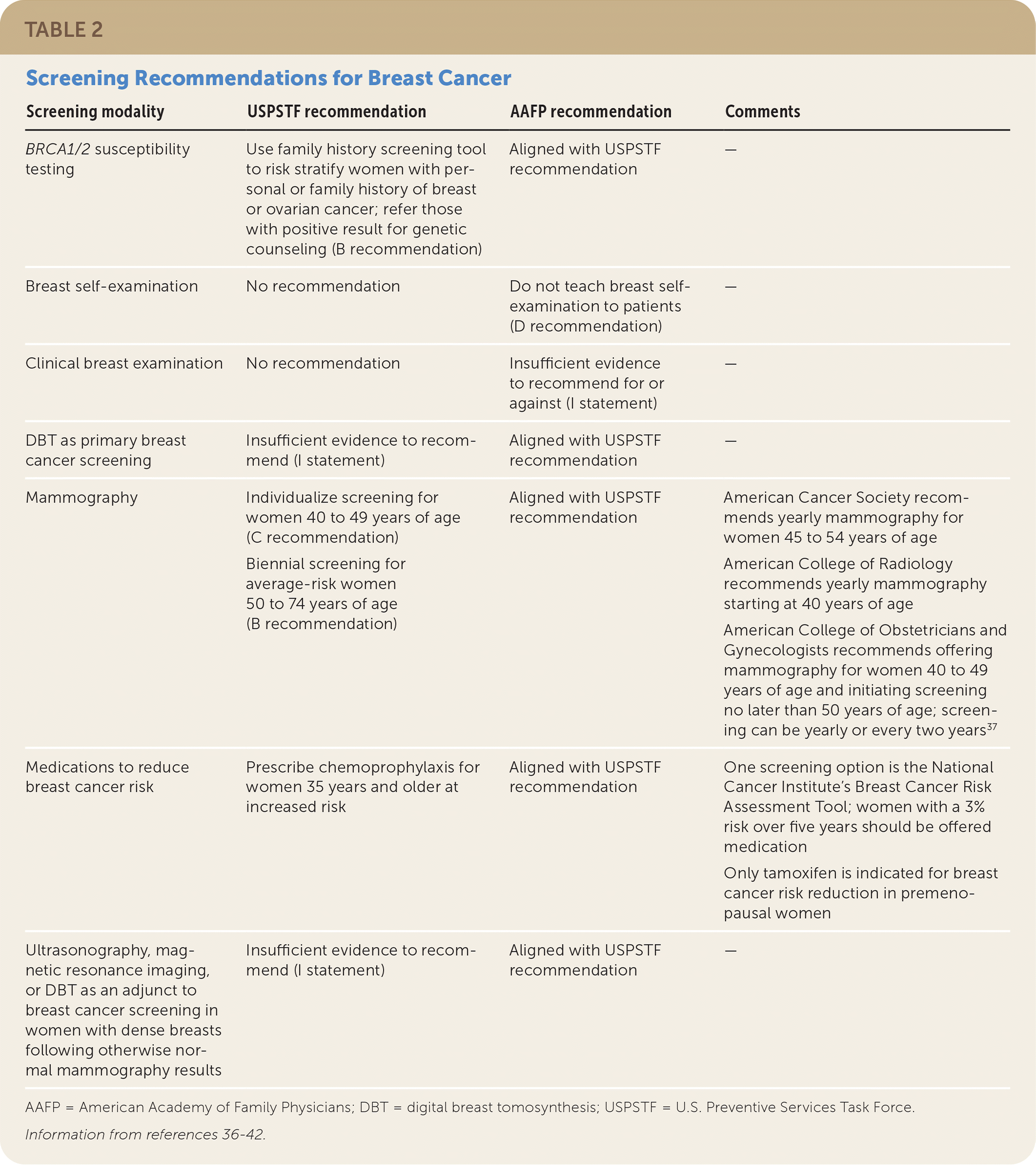
According to the USPSTF, the greatest benefit from breast cancer screening occurs from biennial screening with mammography between 50 and 74 years of age for women at average risk.36 The decision to start screening before 50 years of age should be a shared one, weighing the small chance of avoiding breast cancer–related death against the relatively more common risks of overdiagnosis, false-positive results, unnecessary biopsies, and radiation-induced breast cancer. USPSTF and AAFP recommendations for breast cancer screening are summarized in Table 2.36–42
TABLE 2. Screening Recommendations for Breast Cancer
| Screening modality | USPSTF recommendation | AAFP recommendation | Comments |
|---|---|---|---|
| BRCA1/2 susceptibility testing | Use family history screening tool to risk stratify women with personal or family history of breast or ovarian cancer; refer those with positive result for genetic counseling (B recommendation) | Aligned with USPSTF recommendation | — |
| Breast self-examination | No recommendation | Do not teach breast self-examination to patients (D recommendation) | — |
| Clinical breast examination | No recommendation | Insufficient evidence to recommend for or against (I statement) | — |
| DBT as primary breast cancer screening | Insufficient evidence to recommend (I statement) | Aligned with USPSTF recommendation | — |
| Mammography | Individualize screening for women 40 to 49 years of age (C recommendation) Biennial screening for average-risk women 50 to 74 years of age (B recommendation) | Aligned with USPSTF recommendation | American Cancer Society recommends yearly mammography for women 45 to 54 years of age American College of Radiology recommends yearly mammography starting at 40 years of age American College of Obstetricians and Gynecologists recommends offering mammography for women 40 to 49 years of age and initiating screening no later than 50 years of age; screening can be yearly or every two years37 |
| Medications to reduce breast cancer risk | Prescribe chemoprophylaxis for women 35 years and older at increased risk | Aligned with USPSTF recommendation | One screening option is the National Cancer Institute's Breast Cancer Risk Assessment Tool; women with a 3% risk over five years should be offered medication Only tamoxifen is indicated for breast cancer risk reduction in premenopausal women |
| Ultrasonography, magnetic resonance imaging, or DBT as an adjunct to breast cancer screening in women with dense breasts following otherwise normal mammography results | Insufficient evidence to recommend (I statement) | Aligned with USPSTF recommendation | — |
AAFP = American Academy of Family Physicians; DBT = digital breast tomosynthesis; USPSTF = U.S. Preventive Services Task Force.
OTHER CANCERS
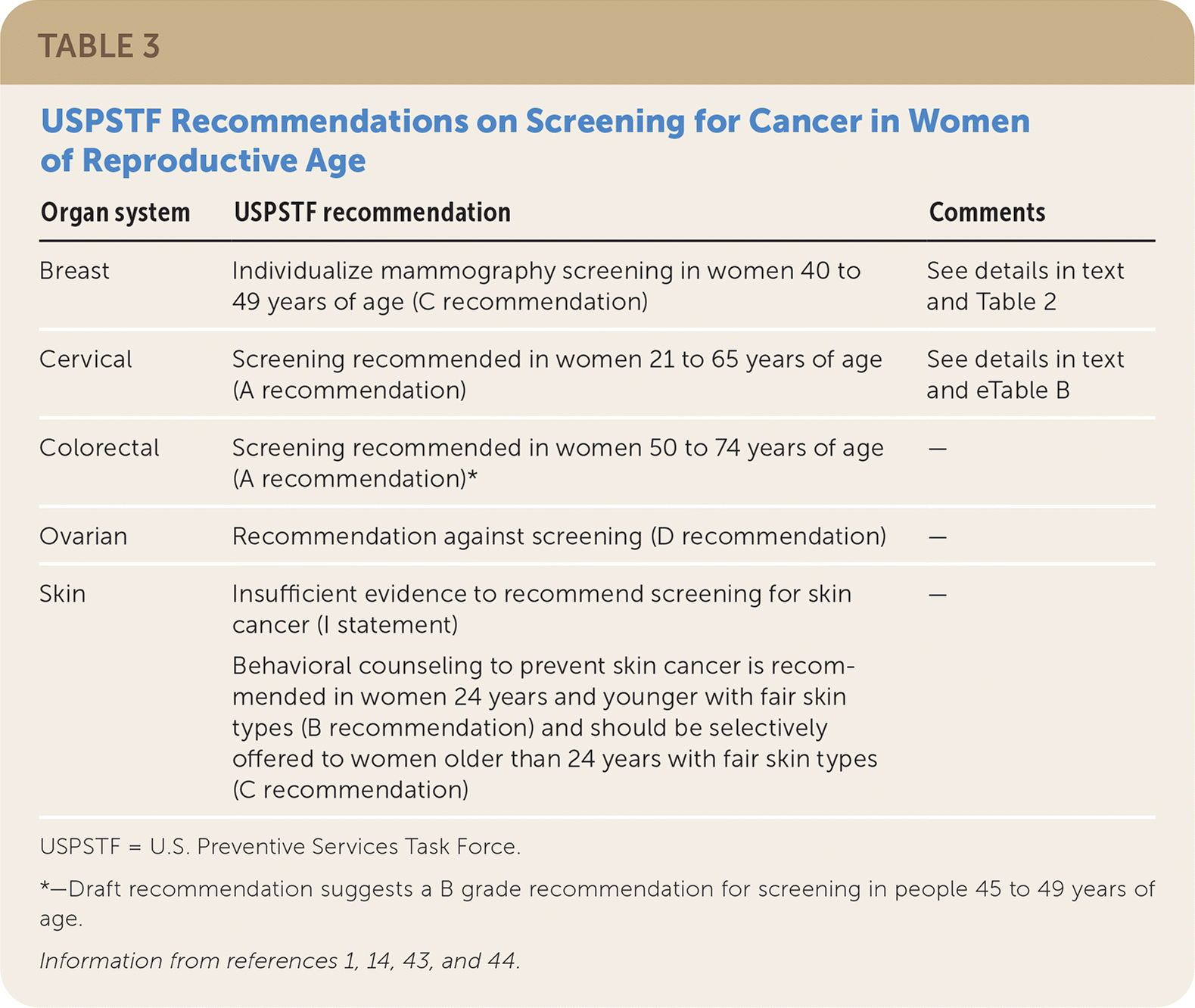
Recommendations on screening for and counseling about skin cancer and colorectal cancer are the same for women as for men. Table 3 summarizes recommendations for cancer screening in women of reproductive age.1,14,43,44
TABLE 3. USPSTF Recommendations on Screening for Cancer in Women of Reproductive Age
| Organ system | USPSTF recommendation | Comments |
|---|---|---|
| Breast | Individualize mammography screening in women 40 to 49 years of age (C recommendation) | See details in text and Table 2 |
| Cervical | Screening recommended in women 21 to 65 years of age (A recommendation) | See details in text and eTable B |
| Colorectal | Screening recommended in women 50 to 74 years of age (A recommendation)* | — |
| Ovarian | Recommendation against screening (D recommendation) | — |
| Skin | Insufficient evidence to recommend screening for skin cancer (I statement) Behavioral counseling to prevent skin cancer is recommended in women 24 years and younger with fair skin types (B recommendation) and should be selectively offered to women older than 24 years with fair skin types (C recommendation) | — |
USPSTF = U.S. Preventive Services Task Force.
*—Draft recommendation suggests a B grade recommendation for screening in people 45 to 49 years of age.
Sexually Transmitted Infections
The USPSTF recommends routine screening for HIV in people 15 to 65 years of age and for hepatitis C virus infection in people 18 to 79 years of age.45,46 Patients at higher risk of contracting HIV should be offered preexposure prophylaxis.47 All women 24 years and younger and older women at increased risk should be screened for gonorrhea and chlamydia; screening for syphilis and hepatitis B virus is recommended only in women at elevated risk.48–50 Local prevalence data and risk factors are important when deciding which women to screen for syphilis because 90.8% of all cases of primary and secondary syphilis in 2014 occurred in men.49
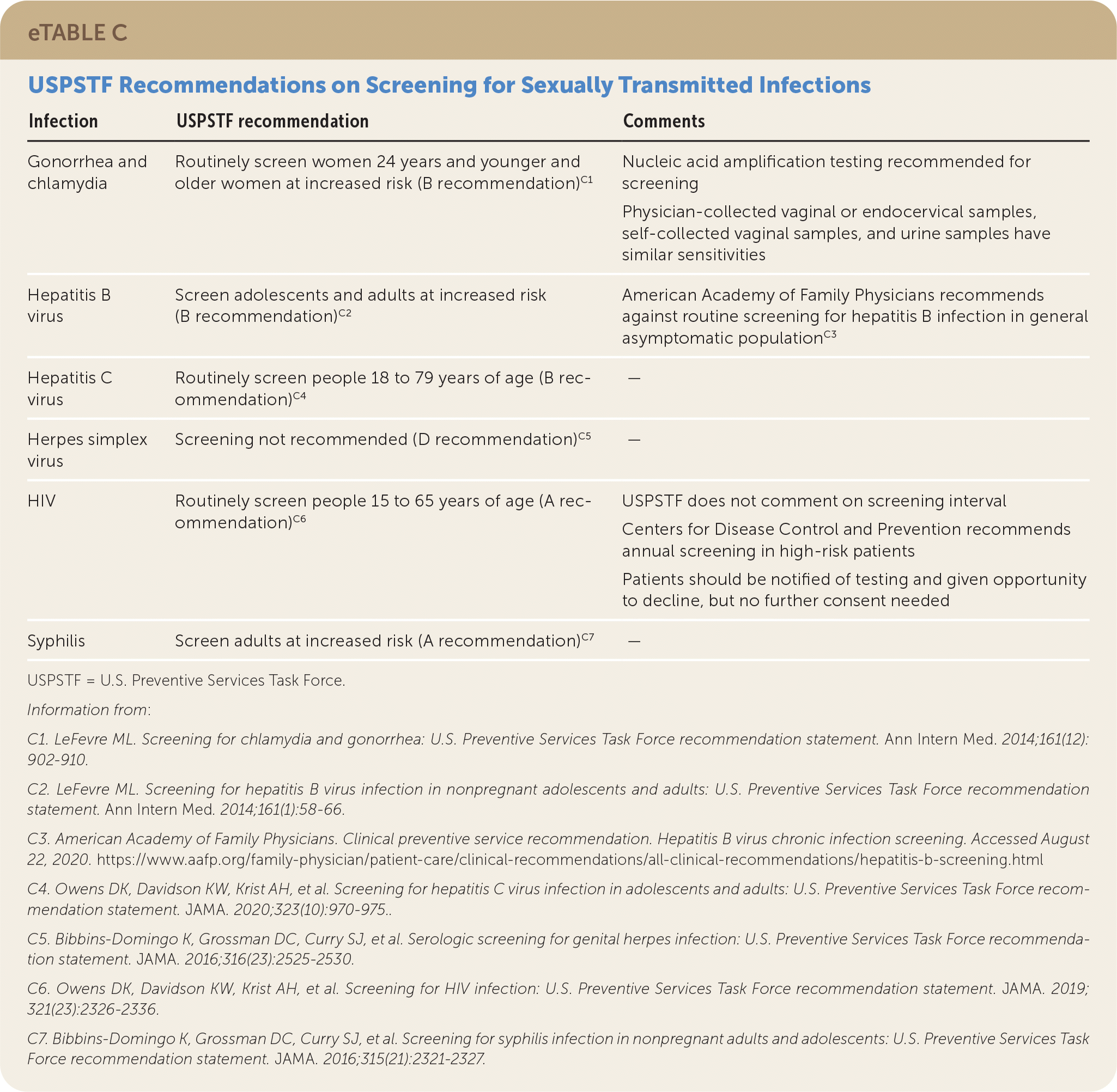
Risk factors for STI acquisition include multiple sex partners; history of incarceration; current or past STIs, including HIV infection; injection drug use; and engaging in transactional sex. People initiating treatment for tuberculosis and those presenting for care at STI clinics are also more likely to have STIs, and race (Black, Hispanic, Native American, and Alaska or Hawaii Native) is a marker for elevated risk because of social and health inequities.51 The USPSTF recommends against routine serologic screening for herpes simplex virus.52 eTable C summarizes USPSTF recommendations for STI screening.
eTABLE C USPSTF Recommendations on Screening for Sexually Transmitted Infections
| Infection | USPSTF recommendation | Comments |
|---|---|---|
| Gonorrhea and chlamydia | Routinely screen women 24 years and younger and older women at increased risk (B recommendation)C1 | Nucleic acid amplification testing recommended for screening Physician-collected vaginal or endocervical samples, self-collected vaginal samples, and urine samples have similar sensitivities |
| Hepatitis B virus | Screen adolescents and adults at increased risk (B recommendation)C2 | American Academy of Family Physicians recommends against routine screening for hepatitis B infection in general asymptomatic populationC3 |
| Hepatitis C virus | Routinely screen people 18 to 79 years of age (B recommendation)C4 | — |
| Herpes simplex virus | Screening not recommended (D recommendation)C5 | — |
| HIV | Routinely screen people 15 to 65 years of age (A recommendation)C6 | USPSTF does not comment on screening interval Centers for Disease Control and Prevention recommends annual screening in high-risk patients Patients should be notified of testing and given opportunity to decline, but no further consent needed |
| Syphilis | Screen adults at increased risk (A recommendation)C7 | — |
USPSTF = U.S. Preventive Services Task Force.
Information from:
C1. LeFevre ML. Screening for chlamydia and gonorrhea: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med. 2014;161(12):902–910.
C2. LeFevre ML. Screening for hepatitis B virus infection in nonpregnant adolescents and adults: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med. 2014;161(1):58–66.
C3. American Academy of Family Physicians. Clinical preventive service recommendation. Hepatitis B virus chronic infection screening. Accessed August 22, 2020. https://www.aafp.org/family-physician/patient-care/clinical-recommendations/all-clinical-recommendations/hepatitis-b-screening.html
C4. Owens DK, Davidson KW, Krist AH, et al. Screening for hepatitis C virus infection in adolescents and adults: U.S. Preventive Services Task Force recommendation statement. JAMA. 2020;323(10):970–975..
C5. Bibbins-Domingo K, Grossman DC, Curry SJ, et al. Serologic screening for genital herpes infection: U.S. Preventive Services Task Force recommendation statement. JAMA. 2016;316(23):2525–2530.
C6. Owens DK, Davidson KW, Krist AH, et al. Screening for HIV infection: U.S. Preventive Services Task Force recommendation statement. JAMA. 2019; 321(23):2326–2336.
C7. Bibbins-Domingo K, Grossman DC, Curry SJ, et al. Screening for syphilis infection in nonpregnant adults and adolescents: U.S. Preventive Services Task Force recommendation statement. JAMA. 2016;315(21):2321–2327.
Substance Use
The USPSTF recommends screening for the use of tobacco and the unhealthy use of alcohol and drugs and providing interventions to help users quit.53–55 These recommendations are the same in women and men of the same age; however, there are some differences in susceptibility to and treatment of these conditions. In terms of smoking cessation, although women are less likely to smoke cigarettes than men, women who use tobacco have more difficulty quitting and have higher relapse rates.56 Women may not respond as well to nicotine replacement therapy and may be more affected by concerns about weight gain and by lack of social support; these factors should be taken into consideration when counseling patients.57 Women are considered to be engaging in risky alcohol use at lower levels of consumption compared with men. In women, risky alcohol use is defined as more than three drinks in a day or more than seven drinks in a week.58 Behavioral counseling interventions are effective for tobacco use, unhealthy alcohol use, and unhealthy drug use. Pharmacotherapy is also recommended as an option for tobacco and opioid use. Substance use screening recommendations are summarized in Table 4, including the AAFP's differing position on unhealthy drug use screening.56,57,59–64
TABLE 4. USPSTF Recommendations on Screening for Substance Use

| Substance | USPSTF recommendation | Comments |
|---|---|---|
| Alcohol | Screen adults and provide behavioral counseling for unhealthy alcohol use | More than one-half of women of reproductive age drink monthly, and 18.2% meet the definition of risky alcohol use (at least four drinks on one occasion) Women are more prone to health problems from alcohol because of slower metabolism |
| Tobacco | Screen adults and provide advice and assistance to quit | 14.1% of women use tobacco, primarily cigarettes Highest rates are in people 25 to 44 years of age Tobacco use associated with higher incidence of breast cancer, progression of cervical intraepithelial neoplasia, premature menopause, and low bone mineral density |
| Unhealthy drug use (including marijuana) | Screen adults for unhealthy drug use | 15% of women report substance use (including marijuana) within the past year Substance use may progress to addiction more quickly in women than in men The AAFP finds insufficient evidence to recommend screening adults and adolescents for unhealthy drug use (I statement) but recommends selective screening of adults for opioid use disorder after considering risks and benefits (C recommendation) |
AAFP = American Academy of Family Physicians; USPSTF = U.S. Preventive Services Task Force.
Immunizations
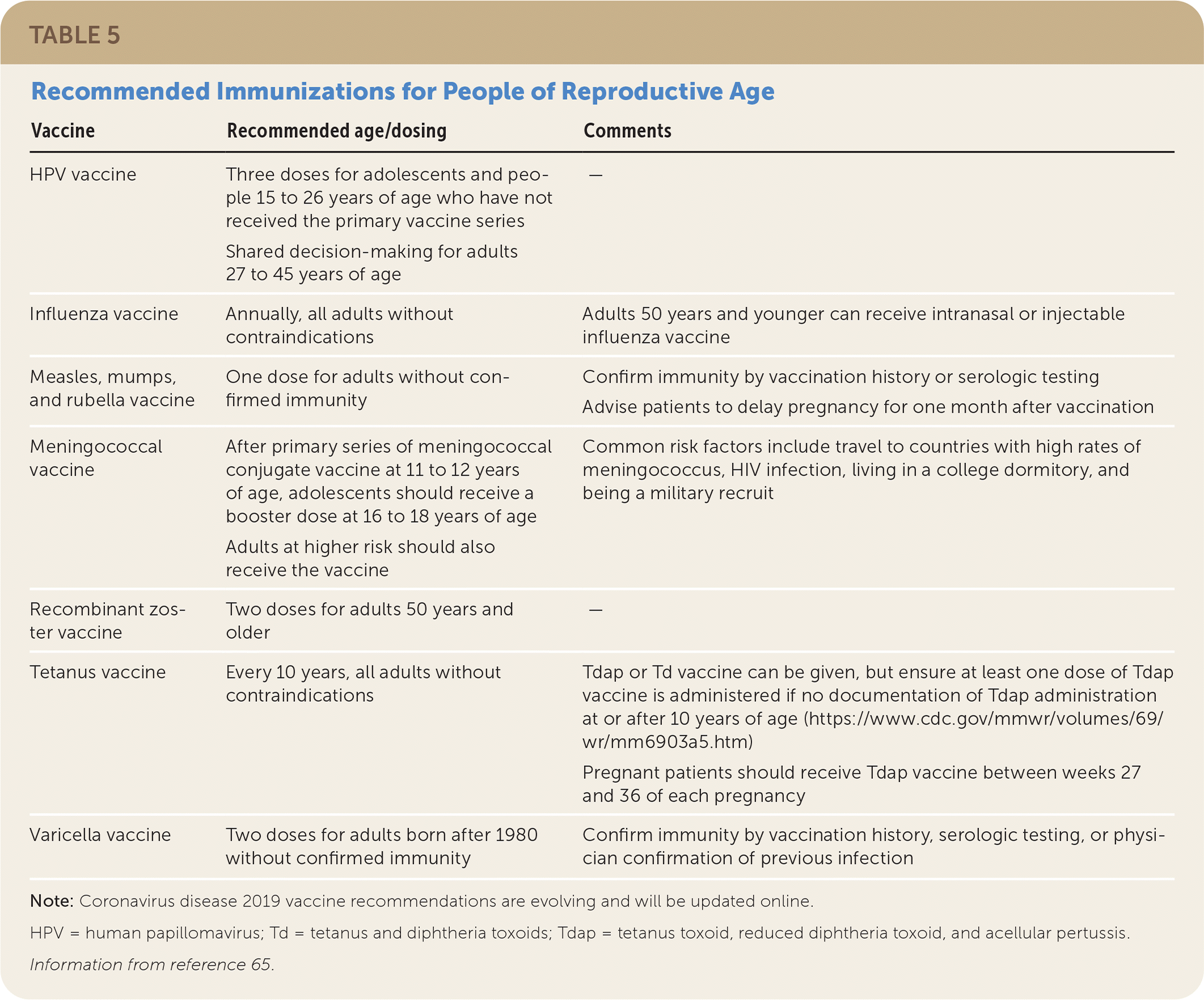
Immunization recommendations are the same for men and nonpregnant women of the same age.65 Table 5 lists immunization recommendations in adults.65 A summary of vaccine recommendations is available on the CDC website at https://www.cdc.gov/vaccines/adults/index.html and is also available via the smartphone apps listed in Table 1.
TABLE 5. Recommended Immunizations for People of Reproductive Age
| Vaccine | Recommended age/dosing | Comments |
|---|---|---|
| HPV vaccine | Three doses for adolescents and people 15 to 26 years of age who have not received the primary vaccine series Shared decision-making for adults 27 to 45 years of age | — |
| Influenza vaccine | Annually, all adults without contraindications | Adults 50 years and younger can receive intranasal or injectable influenza vaccine |
| Measles, mumps, and rubella vaccine | One dose for adults without confirmed immunity | Confirm immunity by vaccination history or serologic testing Advise patients to delay pregnancy for one month after vaccination |
| Meningococcal vaccine | After primary series of meningococcal conjugate vaccine at 11 to 12 years of age, adolescents should receive a booster dose at 16 to 18 years of age Adults at higher risk should also receive the vaccine | Common risk factors include travel to countries with high rates of meningococcus, HIV infection, living in a college dormitory, and being a military recruit |
| Recombinant zoster vaccine | Two doses for adults 50 years and older | — |
| Tetanus vaccine | Every 10 years, all adults without contraindications | Tdap or Td vaccine can be given, but ensure at least one dose of Tdap vaccine is administered if no documentation of Tdap administration at or after 10 years of age (https://www.cdc.gov/mmwr/volumes/69/wr/mm6903a5.htm) Pregnant patients should receive Tdap vaccine between weeks 27 and 36 of each pregnancy |
| Varicella vaccine | Two doses for adults born after 1980 without confirmed immunity | Confirm immunity by vaccination history, serologic testing, or physician confirmation of previous infection |
Note: Coronavirus disease 2019 vaccine recommendations are evolving and will be updated online.
HPV = human papillomavirus; Td = tetanus and diphtheria toxoids; Tdap = tetanus toxoid, reduced diphtheria toxoid, and acellular pertussis.
Information from reference 65.
The CDC does not recommend routine or catch-up vaccination for HPV in adults 27 to 45 years of age; rather, it recommends HPV vaccination based on shared clinical decision-making in this age group.65
This article updates a previous article on this topic by Riley, et al.66
Data Sources: We searched the Agency for Healthcare Research and Quality, American Academy of Family Physicians (AAFP) website, Cochrane Library, Essential Evidence Plus, American College of Obstetricians and Gynecologists, Centers for Disease Control and Prevention, and Women's Preventive Services Initiative for recommendations on the following terms: preventive care, health maintenance, screening recommendations, reproductive health, reproductive age, obesity, depression, intimate partner violence, substance use, cervical cancer screening, sexually transmitted infections, immunizations, and substance use. We also searched the Choosing Wisely website for recommendations from the AAFP. Search dates: December 1, 2019, through January 9, 2020; June 2020; and January 4, 2021.
Editor's Note: This article was finalized prior to FDA Emergency Use Authorization for vaccines for the prevention of COVID-19. For information about these vaccines, see this article on Outpatient Management of COVID-19.—Kenny Lin, MD, Deputy Editor

