Suicide rates in the United States increased from 20% to 30% between 2005 and 2015, and family physicians need evidence-based resources to address this growing clinical concern. Asking high-risk patients (e.g., patients with previous suicide attempts, substance misuse, low social support) about suicidal intent leads to better outcomes and does not increase the risk of suicide. There is insufficient evidence to support routine screening. Important elements of the patient history include the intent, plan, and means; availability of social support; previous attempts; and the presence of comorbid psychiatric illness or substance misuse. After intent has been established, inpatient and outpatient management should include ensuring patient safety and medical stabilization, activating support networks, and initiating therapy for psychiatric diseases. Care plans for patients with chronic suicidal ideation include these same steps and referral for specialty care. In the event of a completed suicide, physicians should provide support for family members who may be experiencing grief complicated by guilt, while also activating support networks and risk management systems.
National rates of suicide are increasing, and how people are attempting suicide is becoming more lethal. There have been efforts to systemically reduce suicide rates, such as the Zero Suicide model, which focuses on screening and practice guidelines.1 However, family physicians report feeling unprepared to treat patients who endorse symptoms of suicidality.2 This article presents current data and recommendations to help physicians address this challenging clinical concern.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Comments |
|---|---|---|
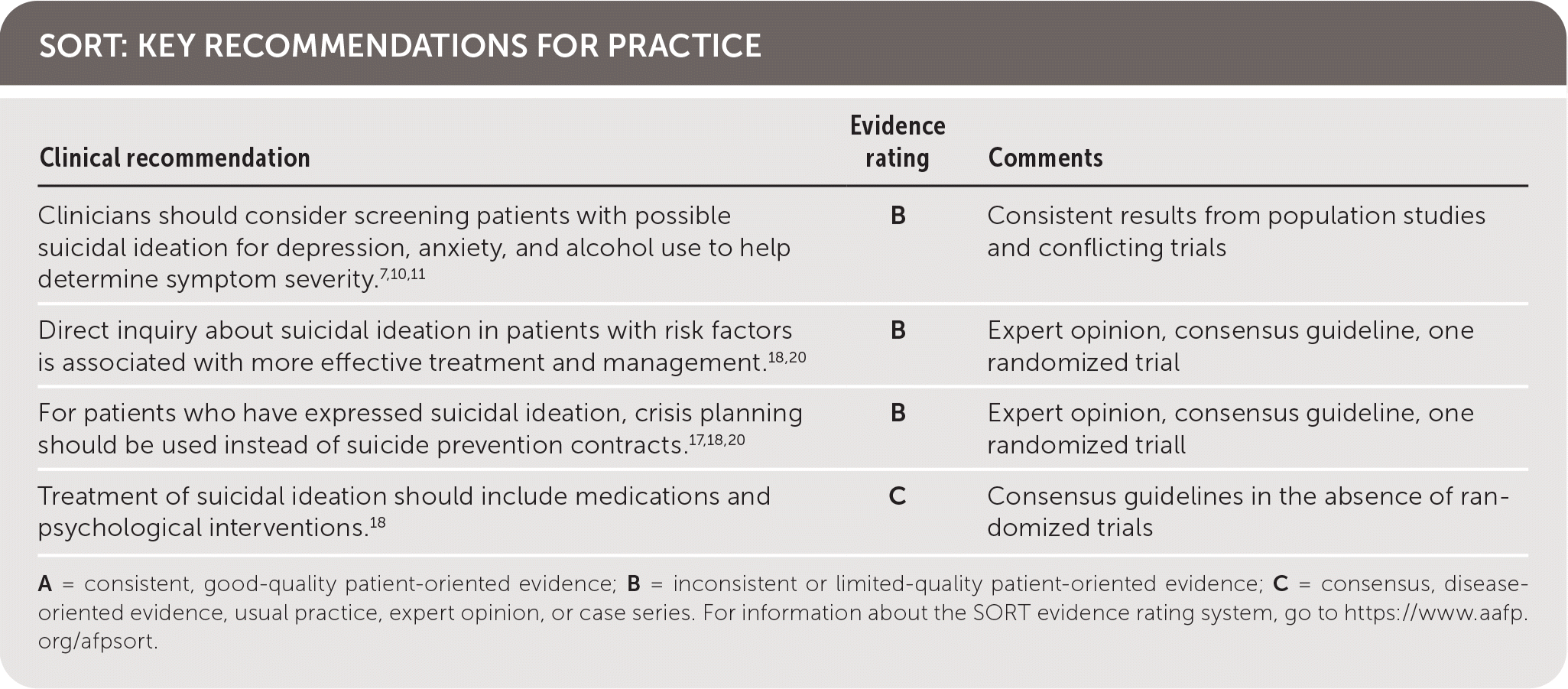
| Clinicians should consider screening patients with possible suicidal ideation for depression, anxiety, and alcohol use to help determine symptom severity.7,10,11 | B | Consistent results from population studies and conflicting trials |
| Direct inquiry about suicidal ideation in patients with risk factors is associated with more effective treatment and management.18,20 | B | Expert opinion, consensus guideline, one randomized trial |
| For patients who have expressed suicidal ideation, crisis planning should be used instead of suicide prevention contracts.17,18,20 | B | Expert opinion, consensus guideline, one randomized trial |
| Treatment of suicidal ideation should include medications and psychological interventions.18 | C | Consensus guidelines in the absence of randomized trials |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Epidemiology and Risk Factors
In 2017, suicide accounted for more than 47,000 deaths in the United States.3 Suicide is the second leading cause of death in people 10 to 34 years and the 10th leading cause of mortality among adults overall.4 Between 2005 and 2015, suicide rates increased from 20% to 30% in the United States.5 Among completed suicides, firearms are the most common means, accounting for approximately 50%, followed by hanging or suffocation (28%), and poisoning including medication overdose (14%).4
Women are twice as likely as men to attempt suicide6; however, men are nearly four times more likely to die by suicide.3 Men are more likely to use violent means, including firearms and hanging, whereas women use more passive means such as poisoning.4
People 45 to 54 years and 75 to 84 years have the highest suicide rates; however, increases in other age groups have almost eliminated the age differences. Suicidal thoughts, plans, and attempts are highest among people 18 to 25 years, compared with older age groups.7 White people are twice as likely to die by suicide as Black or Hispanic people.3 Compared with their heterosexual peers, gay men and women are twice as likely to die by suicide, and more than 40% of people who identify as transgender have attempted suicide in their lives.8,9 People living in rural areas are more likely to commit suicide and to do so by firearm. Non-Hispanic American Indian/Alaska Native people living in rural areas are also at increased risk of suicide.10
One of the key risk factors for suicide attempts and completion is a comorbid psychiatric illness, particularly in patients who have previously attempted suicide. These conditions include anxiety, mood, psychotic, and substance misuse disorders.7,10,11 Although people with depressive disorders have the highest risk, substance misuse, without comorbid psychiatric concerns, is also a significant risk factor because it may be used to mask other illnesses or it provides the decreased inhibition necessary to attempt suicide. In patients with psychotic disorders, those who have schizophrenia with hallucinations instructing them to harm themselves (i.e., command hallucinations) are at the highest risk, and those with frequent and severe exacerbations, fear of further psychiatric decline, and significant functional impairment are also at highest risk in this group.12 Medical illnesses, such as terminal health conditions, chronic obstructive pulmonary disease, chronic pain, and traumatic brain injuries also increase the risk of suicide.13 A summary of risk factors is available in Table 1.3,11,12,14–16
TABLE 1. Risk Factors Associated with Suicide

| Biologic |
| Age (45 to 54 years and 75 to 84 years) |
| Cisgender male |
| Race (White) |
| Recent illness diagnosis or chronic disease |
| Environmental/social |
| Access to means |
| Changes in future plans (e.g., changing or establishing a will; making funeral arrangements) |
| Recent suicide exposure |
| Stressful life event (e.g., death of loved one, unemployment, end of a relationship, legal issues) |
| Unmarried or limited social support |
| Psychological |
| Feelings of social isolation (including members of the lesbian, gay, bisexual, transgender, queer+ community) |
| History of suicide attempts (personal or family) |
| Hopelessness |
| Insomnia |
| Irritability |
| Psychiatric history (personal or family), such as anxiety, mood disorders, schizophrenia, borderline personality disorder |
| Substance (including ethanol) misuse disorder |
Evaluation
The U.S. Preventive Services Task Force concluded that there is insufficient evidence to demonstrate that routine screening for suicide risk in adolescents, adults, and older adults reduces attempts or mortality from suicide.17 Tools such as the nine-item Patient Health Questionnaire (PHQ-9; https://www.mdcalc.com/phq-9-patient-health-questionnaire-9) are available to screen for suicidal ideation. There is support for using item 9 (i.e., in the past two weeks have you had “Thoughts that you would be better off dead, or thoughts of hurting yourself in some way?”) of the PHQ-9 as a component of screening during a clinical interview.18
There are no agreed-upon recommendations to stratify suicide risk, and risk stratification is a source of controversy in research.14,19 Recent meta-analyses found that approximately one-half of patients who were categorized as low risk ultimately died by suicide.14 Current recommendations focus on the individualized assessment of the seriousness of suicidal ideation, including the incorporation of known risk factors and understanding factors that are exacerbating thoughts of self-harm for the patient.14,15 Family physicians who engage in patient-centered care by incorporating the patient's history, current stressors, and current data on risk factors for suicide, and by reducing access to means of self-harm such as firearms are following standards of care for patients expressing suicidal ideation.16 Evidence demonstrates that asking patients at high risk about suicide does not increase suicidal ideation or attempts and leads to better outcomes.15 In a review of practice guidelines from the U.S. Department of Veterans Affairs and the U.S. Department of Defense, no studies found an increased risk of harm from screening or from asking the patient about suicide.18 Key questions to ask patients who are suicidal are provided in Table 2.12
TABLE 2. Questions to Ask in the Assessment of Suicidal Intent

| Are you currently thinking about or have you recently thought about death or harming yourself? Do you have access to the method (e.g., gun, bullets, poison, pills)? Do you have any intention of following through with the thoughts of self-harm? Have you or a family member ever attempted suicide in the past? Are you currently using alcohol or drugs (illicit or prescription)? Do you have friends or family with whom you are close? Have you told them about these thoughts? Have you thought about how you would harm yourself? What is your plan? What has kept you from acting on these thoughts? What are your plans for the future? Have you or a family member ever been diagnosed with or treated for anxiety, depression, or other mental health problems? Have there been any changes in your employment, social life, or family? Do you tend to be impulsive with your decisions or behavior? |
Information from reference 12.
Management
ACUTE MANAGEMENT
Patients who have expressed suicidal ideation but deny current suicidal intent, have no plan or means in place, and have good social support may be treated as an outpatient or referred for outpatient therapy. With the patient's permission, close family or friends should be involved to ensure patient safety and adherence to follow-up care instructions. Crisis planning, including educating patients on coping skills, locating social support, and identifying crisis resources, effectively reduces suicidal ideation and number of days spent in the hospital.18,20 However, suicide contracts, in which patients agree to not engage in self-harm behaviors, are not an effective means of reducing suicide.18,20
Inpatient admission should be offered to patients with specific plans for suicide who have the means to complete their plan. Where available, treatment options may also include intensive outpatient treatment or partial hospitalization programs. When in doubt about the need for admission, inpatient care is the prudent option. If a patient is referred for admission but not placed in the hospital, they may experience additional stress and increased feelings of helplessness. Ensuring patient safety is a primary concern regardless of the treatment setting. Therefore, arranging for appropriate follow-up and enlisting help from social support resources can be beneficial. Caregivers should remove weapons and medications that could be used for deliberate self-harm and monitor the patient frequently. During inpatient admissions, patients may need to stay in a locked unit where they do not have access to stairwells, light fixtures, and other installations that could be used for hanging. Frequent contact with staff can provide early identification of and stabilization after additional suicide attempts. If a patient were to refuse treatment, involuntary hospitalization might be required, and physicians should review individual state legislation related to involuntary treatment.18
PHARMACOTHERAPY
For patients who are suicidal and have unipolar and bipolar mood disorders, lithium has been proven to decrease suicide attempts and all-cause mortality. In patients with underlying psychotic disorders, clozapine (Clozaril) has been shown to reduce suicidal behaviors but is typically reserved until other treatments have been used. The use of clozapine is restricted because of the potential for agranulocytosis.11 Antidepressants are often the first-line treatment for mood disorders, but unique concerns need to be addressed when using these medications with individuals expressing suicidal ideation. A U.S. Food and Drug Administration boxed warning has been issued because of increased risk of suicidality among adolescents and young adults in the early months after starting selective serotonin reuptake inhibitor therapy.21 There can also be a concern for overdose with antidepressants and other types of pharmacotherapy. Citalopram (Celexa) and venlafaxine were of most concern among the antidepressants for overdose toxicity. Despite these risks, there is evidence to support the benefit and use of antidepressants to reduce overall suicidal ideation and suicide attempts.11 In these patients, pharmacotherapy should be accompanied by patient education, additional monitoring (e.g., scheduled visits, telephone calls), and limited supplies (e.g., a 30-day supply of medication). There is emerging evidence to support ketamine as a pharmacologic intervention because it rapidly reduces depressive symptoms in the acute treatment phase. However, more studies are needed to address dosing, administration concerns, and long-term implications.11 Research has demonstrated that a combination of psychological therapy and pharmacotherapy is more effective than either alone for the treatment of suicidal ideation.18
LONG-TERM MANAGEMENT
After initial stabilization and improvement of suicidal ideation, patients will need follow-up care.11 Follow-up with community mental health care programs and mental health clinicians has reduced suicide rates in many countries. In patients with personality disorders, predominantly borderline, histrionic, and narcissistic disorders, suicidal gestures and intent may become common and chronic. The physician must be vigilant about taking each threat seriously because gestures may become lethal. An expert consensus practice guideline suggests that physicians evaluate for suicide risk and coping resources, and help patients identify problem-solving techniques.22 If the patient is at high risk of self-harm, referrals to emergency services and specialty care are recommended.22
Coping with a Completed Suicide
A completed suicide causes stress for the patient's loved ones and physician. These stressors may include personal and legal ramifications. Bereavement after suicide is similar to that after other causes of death; however, survivors are more likely to feel shame and to blame themselves for the loss.23 The physician should be prepared to empathetically support the family members through this difficult transition. Survivors need the opportunity to ask questions, an understanding of the underlying causes of suicide, an opportunity to say goodbye, and follow-up contact with the health care system.24 Support groups may also be of benefit and may be found through the resources listed in Table 3.25
TABLE 3. Resources for Suicide Prevention and Survivors

| American Foundation for Suicide Prevention https://afsp.org |
| National Suicide Prevention Lifeline 1-800-273-TALK (8255) https://suicidepreventionlifeline.org |
| Suicide Prevention Resource Center https://www.sprc.org |
Adapted with permission from Norris D, Clark MS. Evaluation and treatment of the suicidal patient. Am Fam Physician. 2012;85(6):604.
In situations in which the physician must face an angry family member, prudent steps include careful documentation; hospital notification, managed care, and malpractice risk management teams; and taking care to give condolences compassionately to the family without assigning blame.26
Some physicians who have had a patient commit suicide report feelings of guilt, personal responsibility, and descent into a mood disorder.27,28 This is most common among physicians who think they missed warning signs or could have done more to protect their patient.29 Physicians who develop suicidal ideation may be at increased risk of a suicide attempt because of their advanced medical knowledge and access to lethal means. To cope with this stress, physicians should have access to social support and medical and psychological care.26
This article updates previous articles on this topic by Norris and Clark25; Stovall and Domino30; and Gliatto and Rai.31
Data Sources: A PubMed search was completed using the key terms suicide, suicide risk factors, suicide prevent, suicide treatment, and suicide interventions. Also searched were Essential Evidence Plus, the Cochrane database, and the National Guideline Clearinghouse. Search dates: January 10, 2020, and November 13, 2020.

