Original Article: Evidence Lacking to Support Universal Unhealthy Drug Use Screening [Editorial]
Issue Date: January 15, 2021
Available at: https://www.aafp.org/afp/2021/0115/p72.html
To the Editor: The U.S. Preventive Services Task Force (USPSTF) recommends screening adults 18 years and older by asking about unhealthy drug use; however, the American Academy of Family Physicians (AAFP) disagrees that there is sufficient evidence to assess the benefits and harms of screening in adults except for opioid use disorder. The AAFP justifies this recommendation by noting, “Screening programs should only be implemented if services for accurate diagnosis, effective treatment, and psychosocial supports can be offered or referred.”
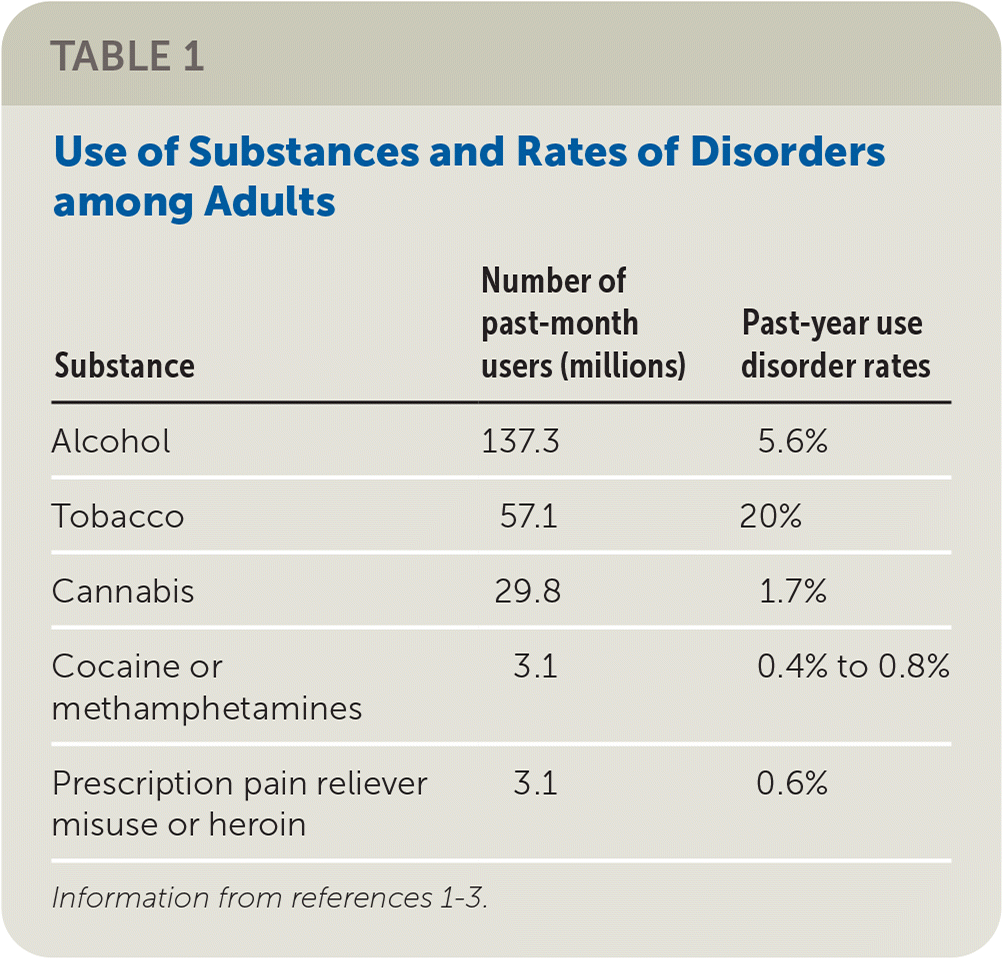
We are concerned with the AAFP's departure from the USPSTF recommendations and with the framing of Drs. Coles and Vosooney's editorial. Although opioid use disorder is of significant importance and a contributor to the prescription drug overdose epidemic, other substances are also important contributors in unhealthy drug use (Table 11–3 ). Tobacco use is the leading preventable cause of death in the United States, and more people consume alcohol than any other substance.4 Clinicians have effective modes of diagnosis, treatment, and support for the unhealthy use of these substances.
TABLE 1. Use of Substances and Rates of Disorders among Adults
Although the USPSTF does not include tobacco and alcohol in its definition of unhealthy drug use, the editorial does not clarify this point. Additionally, cannabis use and cannabis use disorder outnumber opioid-related issues; there are clear criteria for cannabis use disorder, and psychosocial approaches are helpful.5
Primary care is essential in screening, treating, and referring people for substance use disorders. The title of the editorial may send the wrong message to our colleagues and worsen public health outcomes.
The editorial also suggests that because no resources are available to treat a specific disease in a community, the community should not be screened for the disease. This argument is myopic and actively contributes to the large gaps in care found in low-income rural and urban communities. Screening for unhealthy drug use and opioid use disorders is one way to provide the leverage to bring more resources into these communities. Now is the time that we need to be more inquisitive and attentive to unhealthy drug use because of widespread impacts on public health.3,4
In Reply: Thank you for the comments on our editorial. The USPSTF recently recommended screening for unhealthy drug use by asking about use in adults 18 years and older. The AAFP disagreed and believed that there was insufficient evidence to support screening of adults, except for selective screening for opioid use disorder.1 The AAFP agrees with the USPSTF recommendations regarding tobacco and alcohol use disorders. The AAFP and USPSTF recommend that clinicians ask all adults, including pregnant people, about tobacco use and offer evidence-based treatments, including behavioral interventions and pharmacotherapy when appropriate.2 The AAFP and USPSTF agree that clinicians should screen for unhealthy alcohol use in individuals 18 years and older, including pregnant people.3
Excluding tobacco and alcohol use disorders, there are no direct studies of the risks and benefits of universal screening for substance use disorders.4 The preponderance of data about interventions for substance use disorders is obtained from treatment-seeking populations with opioid use disorder. It is inappropriate to apply these findings to screen-detected populations or patients using other substances. A systematic review commissioned by the USPSTF found that psychosocial interventions were ineffective in preventing drug use or its related consequences for cannabis use disorder in screen-detected populations.5 Effective treatments and interventions must already be in place for a screening program to benefit the screened populations.
Screening for substance use disorders does not come without risk and potential harm to the screened individual. Risks of screening include labeling, stigmatization, and medicolegal consequences. Individuals are also at greater risk of experiencing discrimination and stigma within the health care system. Health care professionals can have a negative attitude toward individuals with substance use disorders, and these attitudes directly impact a patient's care, feelings of empowerment, trust in the health care system, and clinical outcomes.6 Without evidence-based clinical care and access to community resources to positively impact the health and experience of the screened populations, screening for substance use may cause further harm rather than help. Further research in screening and investment in evidence-based substance use disorder treatment are imperative, especially in rural and urban underserved areas.
Editor's Note: Drs. Coles and Vosooney are members of the Subcommittee on Clinical Recommendation and Policies of the AAFP Commission on the Health of the Public and Science.