Case Scenario
A 75-year-old patient, H.B., is having a telemedicine visit with their family physician for follow-up of end-stage chronic obstructive pulmonary disease, osteoarthritis, and chronic fatigue syndrome. H.B. is homebound because of dyspnea, chronic pain, and limited functional status and resides with a family member who is minimally involved in H.B.'s care. For three years, H.B. has rarely left home because minimal activity sets them back functionally for weeks. The COVID-19 pandemic has worsened H.B.'s isolation because they are afraid of being exposed to the virus. H.B. has refused all in-home support, although they actively participate in online chat groups. What is the impact of social isolation and loneliness on health-related outcomes in patients, and what interventions can be used by family physicians?
Commentary
Social isolation and loneliness are increasingly recognized as complex clinical and public health problems, particularly in older adults, leading to adverse mental and physical health outcomes.1 The COVID-19 pandemic has led to physical distancing policies, which have exacerbated loneliness and social isolation.2 Social isolation is an objective absence or lack of social contact with others, whereas loneliness is defined as an undesirable subjective experience of unfulfilled social contacts and/or needs.3 The terms are distinct, although they are often used interchangeably, and both have similar health implications. Social isolation and loneliness are increasingly common in older age groups. National surveys report that approximately one in four community-dwelling older adults reports social isolation,4 and 22% to 35% report feeling lonely.1 Several factors are associated with social isolation in older adults, including being unmarried, having chronic illness, and lower reported socioeconomic status.4,5
Given the high prevalence, family physicians should consider the health consequences associated with social isolation and loneliness in older adults.6 A growing body of research demonstrates a strong link between social isolation and loneliness with adverse outcomes. All-cause mortality is increased to the same extent as that for smoking or obesity. The incidence of cardiovascular disease and mental health disorders is significantly increased, and socially isolated individuals report a higher prevalence of tobacco product usage and other deleterious health behaviors.1,3,5,7 Individuals who are socially isolated and/or lonely also report higher rates of health service utilization that may be because of greater disease occurrence and/or increased outreach provided by health service agencies.1 Nevertheless, these individuals report decreased adherence with medical advice.3,8
IDENTIFYING LONELINESS AND SOCIAL ISOLATION
Family physicians recognize the importance of loneliness as a condition that affects their patients but are often limited in their ability to reliably identify affected patients.9 The U.S. Preventive Services Task Force does not have a recommendation about screening for loneliness and social isolation; however, a recent report from the National Academy of Medicine provides guidance.1 Universal screening is not currently indicated because of the paucity of evidence-based interventions; however, physicians may consider assessments using validated tools, such as the Berkman-Syme10 or UCLA Loneliness Scale.1,11 Screening may be indicated in at-risk patients, for example, in those who have experienced a challenging life event such as the loss of a loved one, those who disclose limited social networks, or those who have frequent health care use.1 When patients at risk have been identified, physicians should consider discussing the adverse health outcomes associated with social isolation and loneliness with their patients and caregivers and investigate for underlying health or functional limitations that may be contributing factors.1
There is growing interest in information technology as a platform for assessing social isolation and loneliness.1 Several technologies are being explored as tools to identify or predict patterns of social isolation, including home-based activity monitoring, tracking of online and electronic usage patterns, and wearable devices that record sleep and physical activity.1
STRATEGIES TO MITIGATE LONELINESS AND SOCIAL ISOLATION
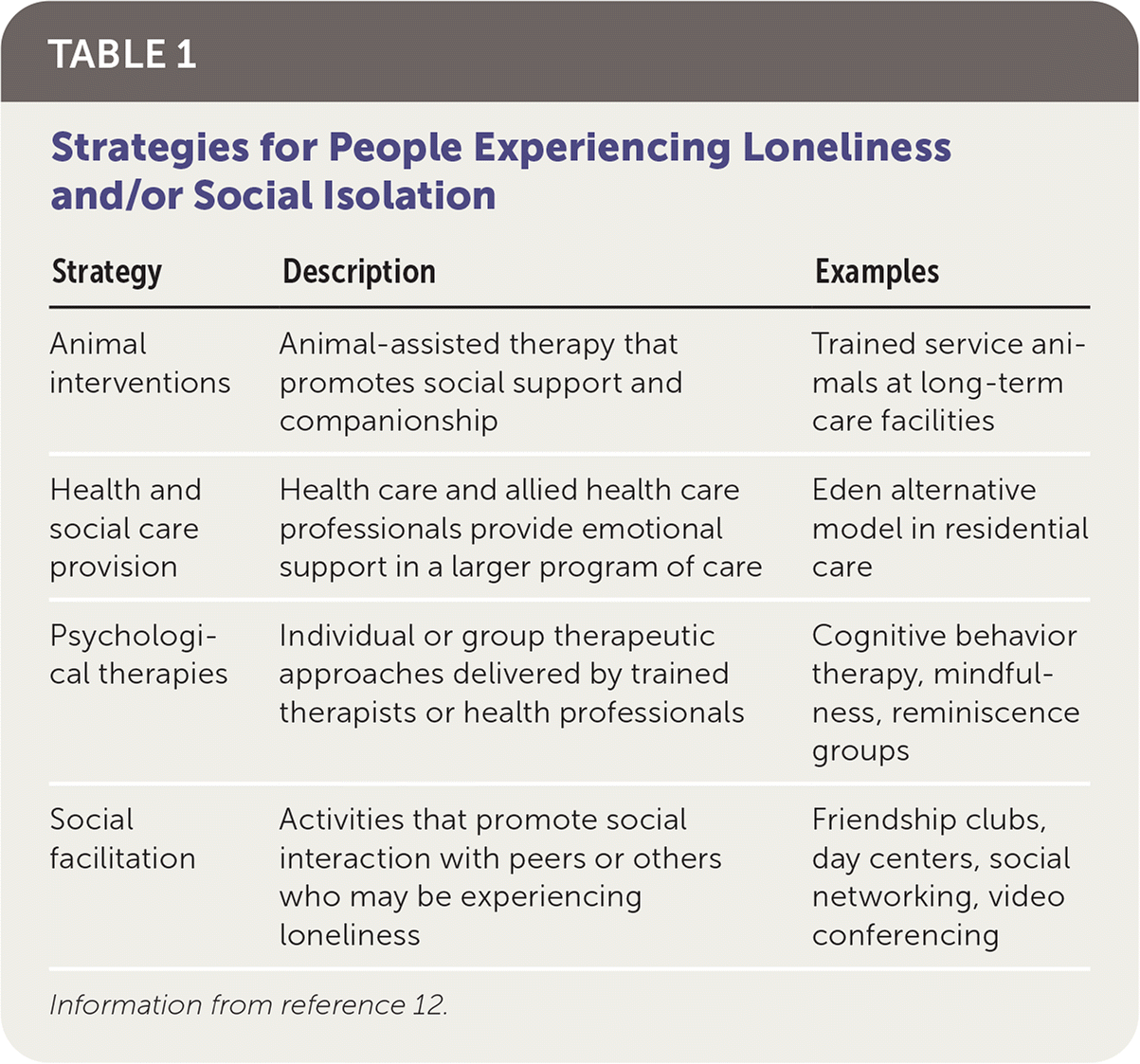
There is currently limited evidence to support specific interventions to mitigate the health effects of social isolation and loneliness. An integrative review categorizing several strategies, such as social facilitation and psychological therapies, has highlighted activities that promote active engagement.12 Table 1 provides strategies, descriptions, and examples for patients.12 A subsequent review from the Agency for Healthcare Research and Quality corroborated the lack of quality evidence but pointed to promising interventions that promote group physical activity and strategies that connect socially isolated older adults to health services.13
TABLE 1. Strategies for People Experiencing Loneliness and/or Social Isolation
| Strategy | Description | Examples |
|---|---|---|
| Animal interventions | Animal-assisted therapy that promotes social support and companionship | Trained service animals at long-term care facilities |
| Health and social care provision | Health care and allied health care professionals provide emotional support in a larger program of care | Eden alternative model in residential care |
| Psychological therapies | Individual or group therapeutic approaches delivered by trained therapists or health professionals | Cognitive behavior therapy, mindfulness, reminiscence groups |
| Social facilitation | Activities that promote social interaction with peers or others who may be experiencing loneliness | Friendship clubs, day centers, social networking, video conferencing |
Information from reference 12.
The recent National Academy of Medicine report also noted the limited evidence base supporting interventions; however, the report provided approaches that could be implemented by family physicians caring for patients who are experiencing social isolation and loneliness.1 Social prescribing is an approach involving the activities that health care professionals can suggest to link patients with nonclinical support services, which are often found in the community.1 Primary care physicians can implement social prescribing in multiple ways, including a direct referral to community-based agencies through the use of a practice-based care manager for assessing needs and tailoring the referral or by providing access to a directory of support services for patients and family caregivers.1 Peer support groups, particularly for patients with a shared illness or condition, have an extensive evidence base in chronic disease self-management and may benefit those who are socially isolated or lonely.1,14 Although cognitive behavior therapy and interpersonal psychotherapy have the potential to mitigate the negative perceptions of social interactions, the evidence demonstrating effectiveness is limited.1
In addition to its role in assessment, information technology may offer new tools to deliver individual or group interventions to this population.1 Social media virtual communities and video-assisted friendly visits are among these intervention strategies that are currently being researched.1
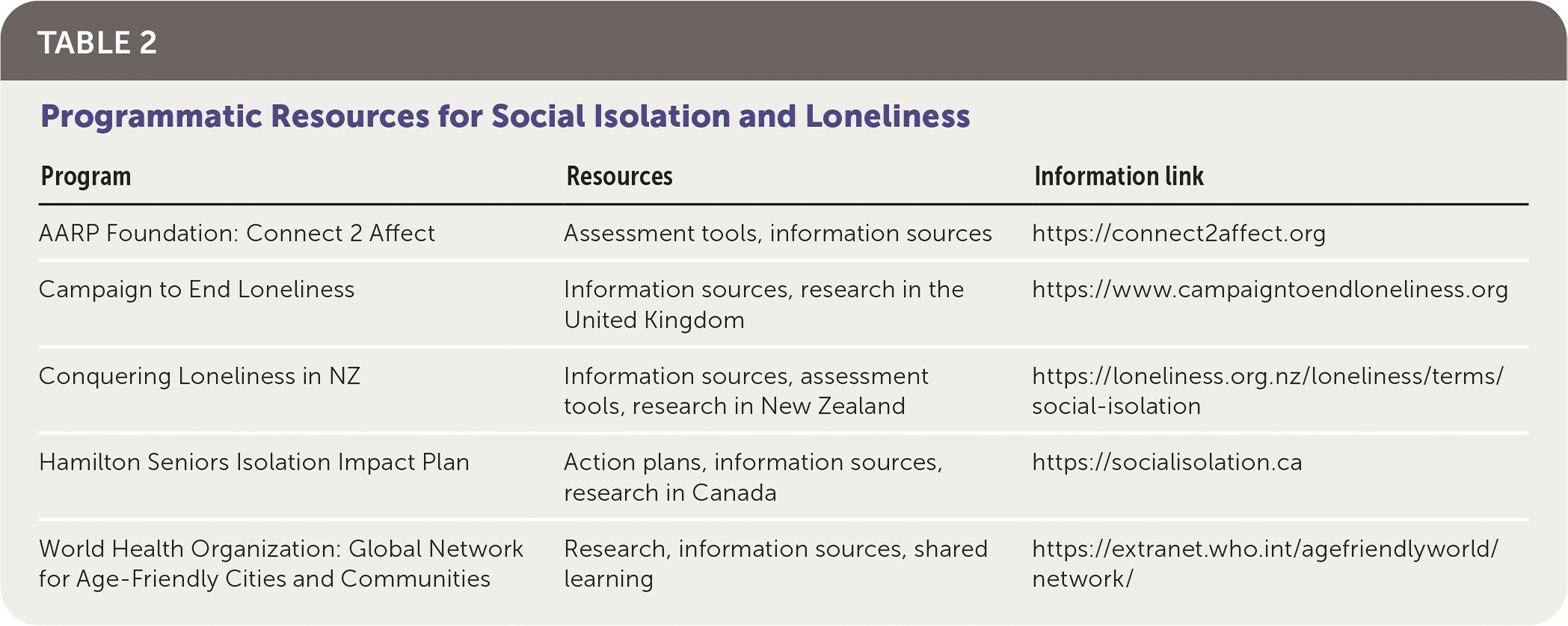
The National Academy of Medicine recommends that physicians, clinical practices, and health care systems partner with community-based providers to promote care that includes and facilitates the use of tailored social services in addressing social isolation and loneliness in older adults.1 Many countries, having identified the public health implications of social isolation and loneliness, have launched initiatives to support systems-level interventions, and regional organizations have created directories of resources (Table 2).
TABLE 2. Programmatic Resources for Social Isolation and Loneliness
| Program | Resources | Information link |
|---|---|---|
| AARP Foundation: Connect 2 Affect | Assessment tools, information sources | https://connect2affect.org |
| Campaign to End Loneliness | Information sources, research in the United Kingdom | https://www.campaigntoendloneliness.org |
| Conquering Loneliness in NZ | Information sources, assessment tools, research in New Zealand | https://loneliness.org.nz/loneliness/terms/social-isolation |
| Hamilton Seniors Isolation Impact Plan | Action plans, information sources, research in Canada | https://socialisolation.ca |
| World Health Organization: Global Network for Age-Friendly Cities and Communities | Research, information sources, shared learning | https://extranet.who.int/agefriendlyworld/network/ |
For the patient in the case scenario, the physician could consider using a screening tool to better assess H.B.'s feelings of loneliness. To promote greater social contact, H.B. could be linked with existing social services, either through existing care management services in the clinic or through referral to a care manager for comprehensive assessment and access to tailored services. By acknowledging H.B.'s limited mobility and highlighting H.B.'s existing information technology skills, the physician could recommend participation in a virtual peer support group or services such as a gentle yoga/breathing class for people with chronic obstructive pulmonary disease. Finally, screening for comorbid mood disorders may provide an opportunity to offer a more directed intervention, such as cognitive behavior therapy.

