Kawasaki disease (KD) and multisystem inflammatory syndrome in children (MIS-C) are inflammatory conditions that present diagnostic and therapeutic challenges to the physician. Although many of their features overlap, they are two distinct conditions. KD is a febrile illness most commonly affecting children younger than five years. It manifests with prolonged fever and at least four of the following features: bilateral bulbar conjunctivitis, mucositis, diffuse maculopapular rash, extremity changes, and cervical lymphadenopathy of 1.5 cm or more in diameter. Patients with MIS-C may have many of the same manifestations but tend to have higher rates of gastrointestinal and neurocognitive symptoms and signs of shock on presentation. Both conditions are associated with cardiac sequelae, including coronary artery aneurysms, although children with MIS-C are at high risk of developing ventricular dysfunction and depressed cardiac output. Lymphocytopenia, thrombocytopenia, elevated troponin, and elevated B-type natriuretic peptide are key laboratory findings of MIS-C that can help distinguish it from KD. The use of intravenous immune globulin is well established in KD and also appears to have a role in the treatment of MIS-C. Aspirin has been used in KD for an anti-inflammatory effect, and low-dose aspirin is recommended for MIS-C to reduce the risk of thrombosis. In addition to supportive care, patients with MIS-C may benefit from immunomodulatory medications, although data on this topic are evolving.
First described in Japan in 1967, Kawasaki disease (KD) is a vasculitis affecting small- and medium-sized vessels; it is predominantly seen in children younger than five years.1 This febrile illness is characterized by systemic inflammation and is the most common cause of acquired coronary artery disease in children.2 With the emergence of multisystem inflammatory syndrome in children (MIS-C), a new inflammatory syndrome associated with COVID-19, KD has received increased attention because features of the diseases overlap.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
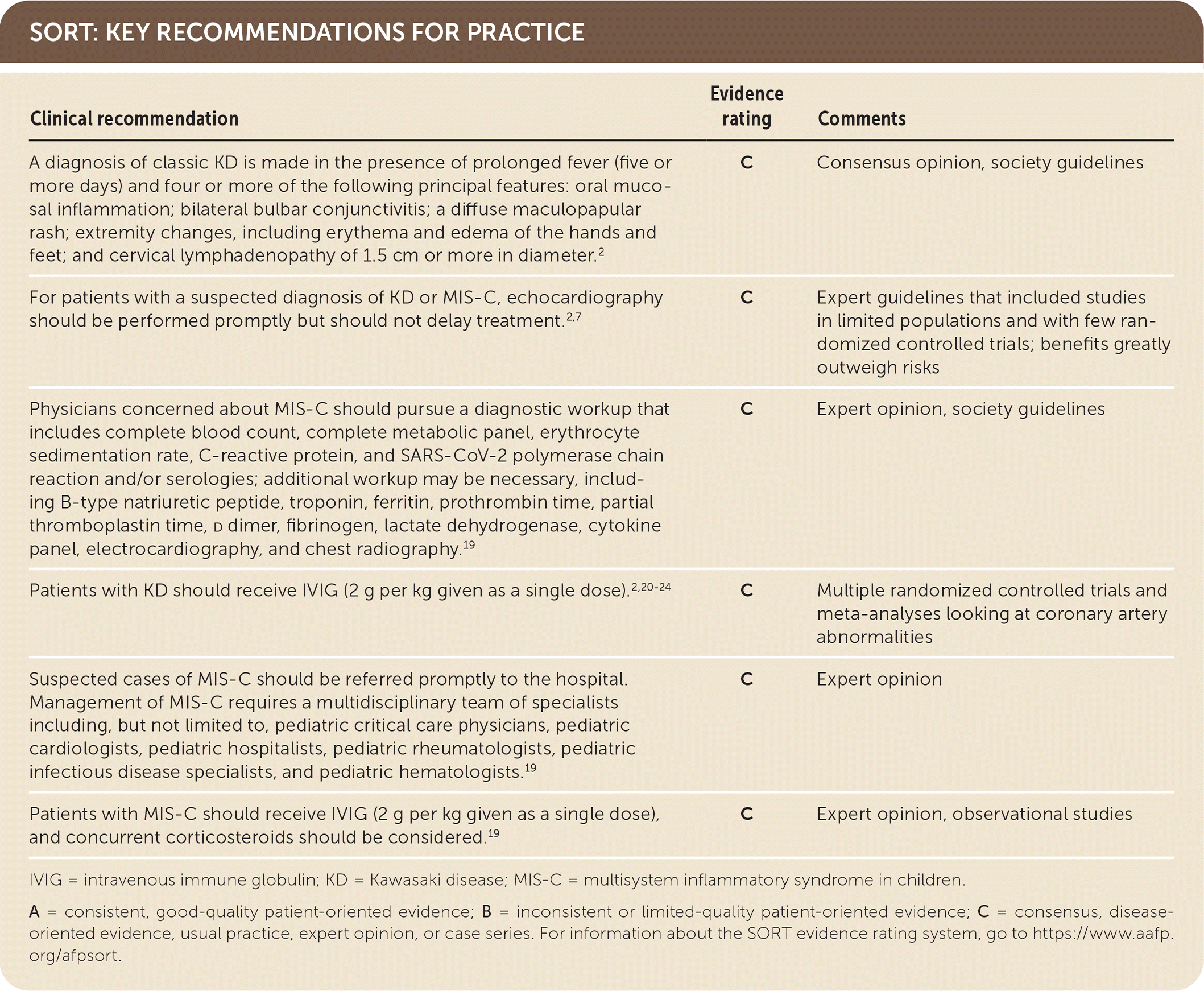
IVIG = intravenous immune globulin; KD = Kawasaki disease; MIS-C = multisystem inflammatory syndrome in children.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Epidemiology
Although the underlying cause of KD remains unknown, the epidemiology and pathophysiology suggest that it is an inflammatory response in a genetically susceptible host to an infectious or other exogenous trigger. A number of viruses have been implicated as potential triggers for KD, including coronaviruses (non–COVID-19 strains).3,4 KD is an illness predominantly occurring in toddlers, with a mean age of three years in the United States (76% of cases occur in children younger than five years).5 There is a predilection for children of Asian and Pacific Islander descent,5 and boys are affected slightly more often than girls (1.5:1).6
In contrast, MIS-C affects a wider age range, from one week to 20 years with a median age of seven to nine years.7–11 In the United States, 62% of patients are Hispanic or Latino (32%) or non-Hispanic Black (30%)—the ethnic groups disproportionately affected by COVID-19.7 Similarly to KD, MIS-C occurs more often in boys (60%) than in girls.7
Symptoms
The clinical features of classic KD are shown in Table 1.2 A diagnosis of classic KD is made in patients with prolonged fever (five or more days) and four or more of the following principal features: oral mucosal inflammation; bilateral bulbar conjunctivitis; a diffuse maculopapular rash; extremity changes, including erythema and edema of the hands and feet; and cervical lymphadenopathy of 1.5 cm or more in diameter.2 Incomplete KD is a diagnosis made when a patient has fewer than four of the major criteria but has sufficient laboratory features or suggestive changes on echocardiography. The 2017 American Heart Association KD guidelines provide a diagnostic algorithm to assist with this often challenging diagnosis2 (Table 2).
TABLE 1. American Heart Association Criteria for Diagnosing KD

| Classic KD Children with at least five days of fever and at least four of the following clinical features*: Oral mucous membrane changes, including any of the following: Erythema, dryness, and/or cracking of the lips Tongue erythema with prominent fungiform papillae (“strawberry tongue”) Diffuse oropharyngeal mucosal erythema Bilateral, nonexudative bulbar conjunctivitis, often sparing the limbus Diffuse, erythematous, maculopapular rash primarily affecting the trunk and extremities† Extremity changes: hand and foot edema, erythema, and/or painful induration of the palms and soles (acute phase) or periungual desquamation (subacute phase, two to three weeks after fever onset) Unilateral cervical lymphadenopathy (≥ 1.5 cm in diameter) | Suspected incomplete KD Children with at least five days of fever and at least two to three of the criteria for classic KD or infants with prolonged, unexplained fever (≥ 7 days)‡ who have the following findings: Elevated erythrocyte sedimentation rate (≥ 40 mm per hour) and/or elevated C-reactive protein (≥ 3 mg per dL [30 mg per L]), and A positive echocardiography§or three or more of the following laboratory findings: Anemia for age Thrombocytosis (platelet count ≥ 450,000 per μL [450 × 109 per L]) after day 7 of fever Hypoalbuminemia (albumin ≤ 3 g per dL [30 mg per L]) Elevated alanine transaminase level Leukocytosis (white blood cell count ≥ 15,000 per μL [15 × 109 per L]) Sterile pyuria (≥ 10 white blood cells per high-power field) |
| Additional comments | |
| Because the clinical features of KD are nonspecific, physicians should consider other diagnoses with similar findings; alternative diagnoses should be sought, particularly in patients with conjunctival or pharyngeal exudates, oral ulcers, a bullous or vesicular rash, generalized lymphadenopathy, or splenomegaly. Patients with KD can have a concurrent viral infection; therefore, identification of a viral pathogen does not preclude the diagnosis of KD. Given the potential for a missed KD diagnosis and/or higher risk of coronary abnormalities, physicians should consider KD in the differential diagnosis for the following: Infants younger than 6 months with prolonged, unexplained fever and irritability or with prolonged fever and unexplained aseptic meningitis Patients with prolonged fever and unexplained shock that is ultimately culture-negative Patients with prolonged fever and cervical lymphadenopathy or retro-/parapharyngeal phlegmon whose course does not respond to appropriate antibiotic treatment | |
KD = Kawasaki disease.
*—Clinical features may not be present simultaneously.
†—Accentuation of the rash in the groin with early desquamation is suggestive of KD; erythema multiforme–like rash is also common in patients with KD.
‡—In young infants, prolonged fever may be the sole clinical finding of KD.
§—The classic finding of coronary artery aneurysms typically does not present until after the first week of illness in patients with KD; positive echocardiography is characterized by any one of the following three findings:
• Left anterior descending coronary artery or right coronary artery diameter z score ≥ 2.5;
• Coronary artery aneurysms present;
• Three or more other suggestive features: decreased left ventricular function, mitral regurgitation, pericardial effusion, or z scores between 2 and 2.5 in the left anterior descending coronary artery or right coronary artery.
Information from reference 2.
TABLE 2. Additional Resources on Kawasaki Disease and Multisystem Inflammatory Syndrome in Children

| American Heart Association guidelines on Kawasaki disease https://www.ahajournals.org/doi/10.1161/CIR.0000000000000484 |
| Centers for Disease Control and Prevention: Multisystem Inflammatory Syndrome in Children https://www.cdc.gov/mis/hcp/index.html |
| American College of Rheumatology: Multisystem Inflammatory Syndrome in Children https://www.rheumatology.org/Portals/0/Files/ACR-COVID-19-Clinical-Guidance-Summary-MIS-C-Hyperinflammation.pdf |
When diagnosing KD, physicians must have a strong understanding of the features of each major symptom. The conjunctivitis of KD is bilateral, nonexudative, and affects the bulbar conjunctiva but classically spares the limbus (Figure 1). The rash of KD is typically diffuse and maculopapular, often accentuated in the perineal region (Figure 2). The oral mucous membrane changes of KD can manifest as erythema of the oropharyngeal mucosa or lips; dryness, cracking, and/or peeling of the lips (Figure 3); or a “strawberry” appearance of the tongue. Anterior cervical lymphadenopathy is typically unilateral and involves at least one node larger than 1.5 cm in diameter. In contrast to bacterial lymphadenitis, the lymphadenopathy of KD is typically not associated with marked erythema of the overlying skin and is not exquisitely painful to palpation. Rarely, painful lymphadenopathy is the presenting feature of KD and may be misdiagnosed as bacterial lymphadenitis.12 The extremity changes of KD manifest as erythema and edema of the palms and soles and, at times, refusal to walk because of painful induration. Subacute extremity changes include periungual desquamation and deep transverse grooves across the nail lines, termed Beau lines. Outside of the major diagnostic criteria, profound irritability is commonly described. Children may also have arthritis or arthralgia, gastrointestinal complaints such as diarrhea and vomiting, or rhinorrhea and cough. Symptoms, physical examination findings, and laboratory evidence of viral infection should not exclude the diagnosis of KD because studies have reported that 30% to 40% of children who meet the diagnostic criteria of KD are also positive for at least one respiratory virus.3,13
FIGURE 1.
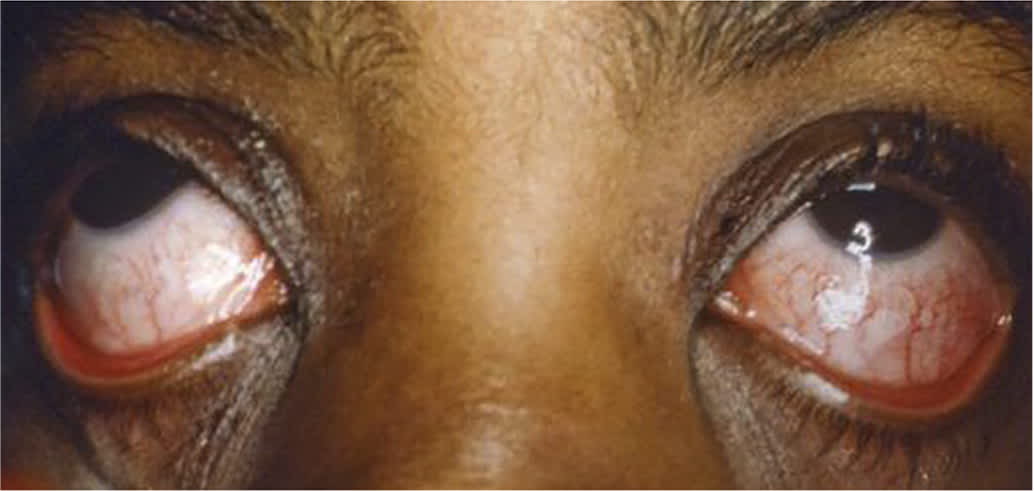
Bilateral, nonexudative conjunctivitis in a patient with Kawasaki disease; note the limbus is spared.
Copyright © Wake Forest School of Medicine Graham Archives Library.
FIGURE 2.
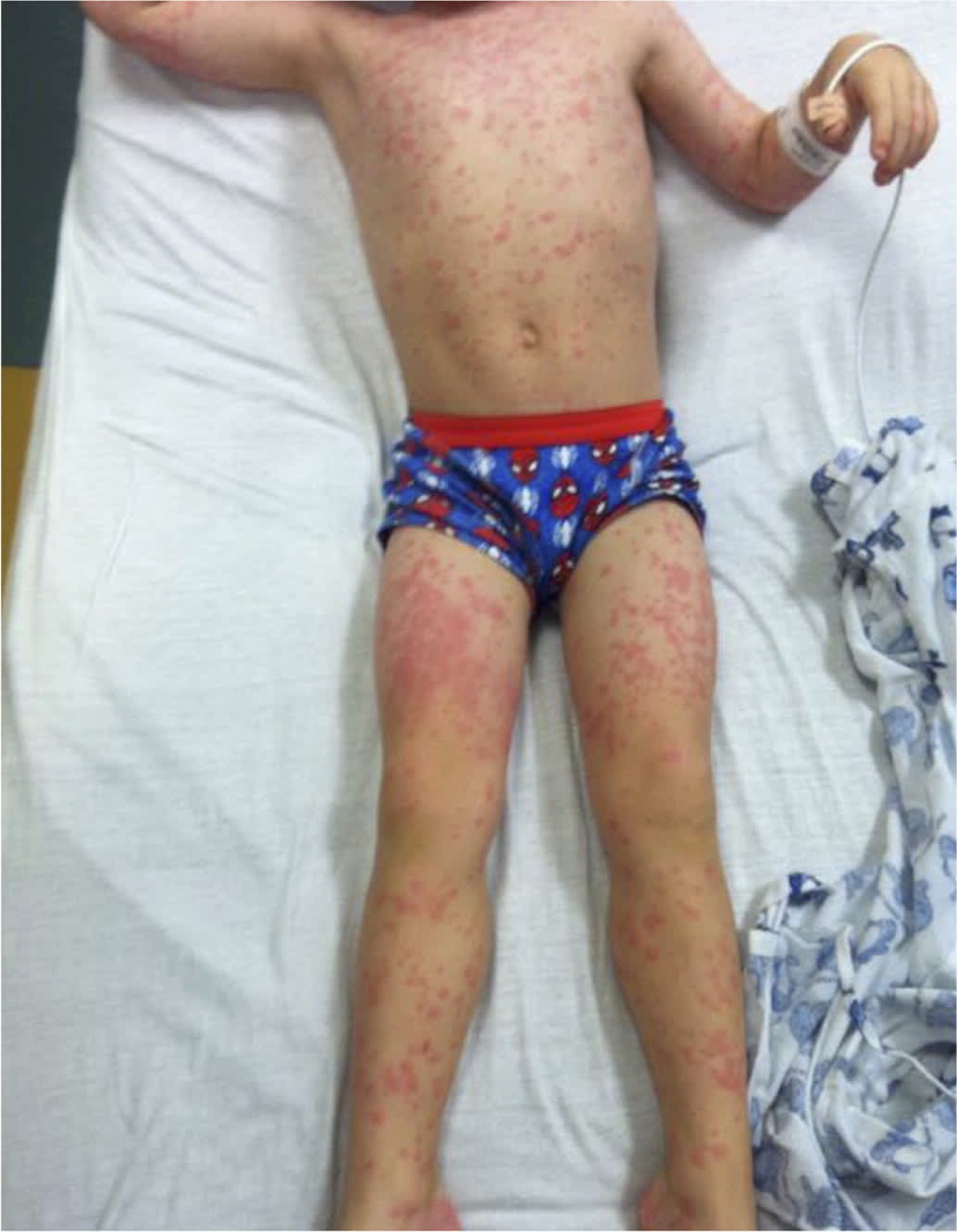
Diffuse, erythematous, maculopapular rash in a patient with Kawasaki disease.
Copyright © Dr. Lindsay Strowd.
FIGURE 3.
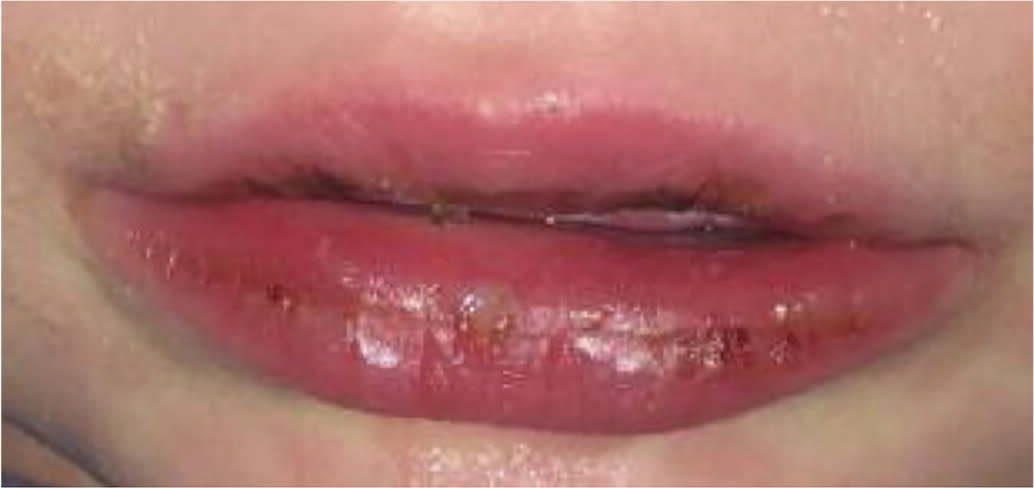
Oral mucous membrane changes in a patient with Kawasaki disease.
Copyright © Dr. Lindsay Strowd.
The Centers for Disease Control and Prevention case definition of MIS-C is presented in Table 3.7 Similarly to KD, fever is the principal diagnostic finding of MIS-C. A shorter duration of fever (24 hours or longer) is used to diagnose MIS-C, which is a significant distinction from KD. Gastrointestinal symptoms, including vomiting, diarrhea, and abdominal pain, are the second most common set of symptoms reported in MIS-C, present in about 80% of cases.8 Neurocognitive symptoms have been described in approximately one-fifth of patients and include headache, irritability, lethargy, altered mental status, or features of aseptic meningitis.8 Respiratory symptoms, including cough, congestion, dyspnea, and sore throat, are less common but have also been reported.8
TABLE 3. Multisystem Inflammatory Syndrome in Children: Case Definition

| Centers for Disease Control and Prevention Case Definition, May 14, 2020 Individuals younger than 21 years presenting with fever,* laboratory evidence of inflammation,† and evidence of clinically severe illness requiring hospitalization, with multisystem (≥ 2) organ involvement (cardiac, renal, respiratory, hematologic, gastrointestinal, dermatologic, or neurologic); and No alternative plausible diagnoses; and Positive for current or recent SARS-CoV-2 (COVID-19) infection by reverse transcriptase polymerase chain reaction, serology, or antigen test or exposure to a suspected or confirmed COVID-19 case within 4 weeks before the onset of symptoms. |
| Additional comments Some individuals may fulfill partial or full criteria for Kawasaki disease but should be reported if they meet the case definition for multisystem inflammatory syndrome in children. Consider multisystem inflammatory syndrome in children in any childhood death with evidence of SARS-CoV-2 infection. |
*—Fever ≥ 100.4°F (38.0°C) for ≥ 24 hours or report of subjective fever lasting ≥ 24 hours.
†—Including, but not limited to, one or more of the following: elevated C-reactive protein, erythrocyte sedimentation rate, fibrinogen, procalcitonin, d dimer, ferritin, lactic acid dehydrogenase, or interleukin 6; elevated neutrophils; reduced lymphocytes; and low albumin.
Information from reference 7.
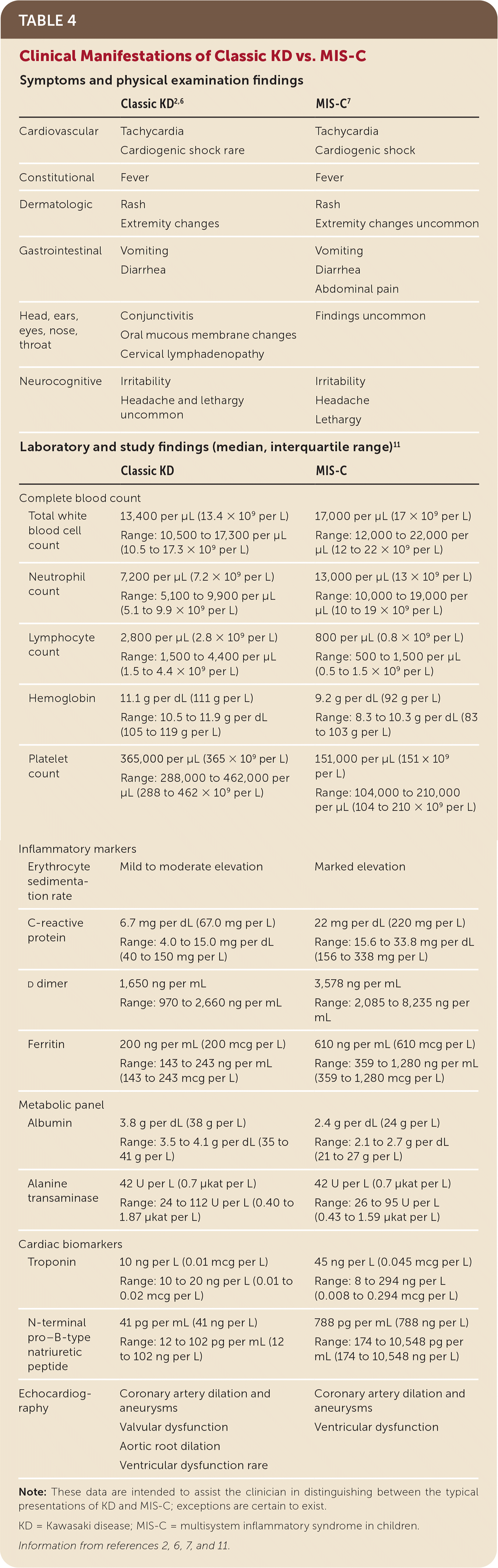
Of note, the clinical manifestations of MIS-C may have tremendous overlap with those of KD (Table 42,6,7,11 ). A recent systematic review reported that 36% of patients with MIS-C had symptoms consistent with KD (6% with classic KD and 30% with incomplete KD).8 The individual symptoms of KD were present with varying frequency in patients with MIS-C: 58% had rash; 40% had conjunctival injection; 23% had red, cracked lips; 4.5% had a strawberry tongue; and 4% had cervical lymphadenopathy.8
TABLE 4. Clinical Manifestations of Classic KD vs. MIS-C
| Symptoms and physical examination findings | ||
| Classic KD2,6 | MIS-C7 | |
| Cardiovascular | Tachycardia | Tachycardia |
| Cardiogenic shock rare | Cardiogenic shock | |
| Constitutional | Fever | Fever |
| Dermatologic | Rash | Rash |
| Extremity changes | Extremity changes uncommon | |
| Gastrointestinal | Vomiting | Vomiting |
| Diarrhea | Diarrhea | |
| Abdominal pain | ||
| Head, ears, eyes, nose, throat | Conjunctivitis | Findings uncommon |
| Oral mucous membrane changes | ||
| Cervical lymphadenopathy | ||
| Neurocognitive | Irritability | Irritability |
| Headache and lethargy uncommon | Headache | |
| Lethargy | ||
| Laboratory and study findings (median, interquartile range)11 | ||
| Classic KD | MIS-C | |
| Complete blood count | ||
| Total white blood cell count | 13,400 per μL (13.4 × 109 per L) | 17,000 per μL (17 × 109 per L) |
| Range: 10,500 to 17,300 per μL (10.5 to 17.3 × 109 per L) | Range: 12,000 to 22,000 per μL (12 to 22 × 109 per L) | |
| Neutrophil count | 7,200 per μL (7.2 × 109 per L) | 13,000 per μL (13 × 109 per L) |
| Range: 5,100 to 9,900 per μL (5.1 to 9.9 × 109 per L) | Range: 10,000 to 19,000 per μL (10 to 19 × 109 per L) | |
| Lymphocyte count | 2,800 per μL (2.8 × 109 per L) | 800 per μL (0.8 × 109 per L) |
| Range: 1,500 to 4,400 per μL (1.5 to 4.4 × 109 per L) | Range: 500 to 1,500 per μL (0.5 to 1.5 × 109 per L) | |
| Hemoglobin | 11.1 g per dL (111 g per L) | 9.2 g per dL (92 g per L) |
| Range: 10.5 to 11.9 g per dL (105 to 119 g per L) | Range: 8.3 to 10.3 g per dL (83 to 103 g per L) | |
| Platelet count | 365,000 per μL (365 × 109 per L) | 151,000 per μL (151 × 109 per L) |
| Range: 288,000 to 462,000 per μL (288 to 462 × 109 per L) | Range: 104,000 to 210,000 per μL (104 to 210 × 109 per L) | |
| Inflammatory markers | ||
| Erythrocyte sedimentation rate | Mild to moderate elevation | Marked elevation |
| C-reactive protein | 6.7 mg per dL (67.0 mg per L) | 22 mg per dL (220 mg per L) |
| Range: 4.0 to 15.0 mg per dL (40 to 150 mg per L) | Range: 15.6 to 33.8 mg per dL (156 to 338 mg per L) | |
| | 1,650 ng per mL | 3,578 ng per mL |
| Range: 970 to 2,660 ng per mL | Range: 2,085 to 8,235 ng per mL | |
| Ferritin | 200 ng per mL (200 mcg per L) | 610 ng per mL (610 mcg per L) |
| Range: 143 to 243 ng per mL (143 to 243 mcg per L) | Range: 359 to 1,280 ng per mL (359 to 1,280 mcg per L) | |
| Metabolic panel | ||
| Albumin | 3.8 g per dL (38 g per L) | 2.4 g per dL (24 g per L) |
| Range: 3.5 to 4.1 g per dL (35 to 41 g per L) | Range: 2.1 to 2.7 g per dL (21 to 27 g per L) | |
| Alanine transaminase | 42 U per L (0.7 μkat per L) | 42 U per L (0.7 μkat per L) |
| Range: 24 to 112 U per L (0.40 to 1.87 μkat per L) | Range: 26 to 95 U per L (0.43 to 1.59 μkat per L) | |
| Cardiac biomarkers | ||
| Troponin | 10 ng per L (0.01 mcg per L) | 45 ng per L (0.045 mcg per L) |
| Range: 10 to 20 ng per L (0.01 to 0.02 mcg per L) | Range: 8 to 294 ng per L (0.008 to 0.294 mcg per L) | |
| N-terminal pro–B-type natriuretic peptide | 41 pg per mL (41 ng per L) | 788 pg per mL (788 ng per L) |
| Range: 12 to 102 pg per mL (12 to 102 ng per L) | Range: 174 to 10,548 pg per mL (174 to 10,548 ng per L) | |
| Echocardiography | Coronary artery dilation and aneurysms | Coronary artery dilation and aneurysms |
| Valvular dysfunction | Ventricular dysfunction | |
| Aortic root dilation | ||
| Ventricular dysfunction rare | ||
Note: These data are intended to assist the clinician in distinguishing between the typical presentations of KD and MIS-C; exceptions are certain to exist.
KD = Kawasaki disease; MIS-C = multisystem inflammatory syndrome in children.
Exposure to or a history of COVID-19 is often noted among patients with MIS-C; however, because COVID-19 can present asymptomatically, this may not be apparent from the history in these patients. Therefore, testing for evidence of COVID-19 is included in the Centers for Disease Control and Prevention's case definition. Among patients with MIS-C, 94% to 99% have tested positive for SARSCoV-2 by reverse transcriptase polymerase chain reaction or for antibodies against this virus.7,8
Cardiac Manifestations
Coronary artery dilation and aneurysm formation are well-known complications of KD. If untreated, 15% to 25% of patients with KD will develop coronary artery abnormalities; the percentage drops to around 5% with prompt treatment.14 Therefore, echocardiography is important for patients suspected of having KD but should not delay treatment.2,7 For risk stratification, coronary artery lumen diameter is compared with the child's body surface area and normalized as a z score. Scores of at least 2.5 in the left anterior descending branch and proximal right coronary artery are highly specific for KD.2 Some patients with mild dilation will experience spontaneous resolution, whereas others will develop giant aneurysms (z score of 10 or more) and can experience significant morbidity, including arterial stenosis, clot formation, and cardiac ischemia or infarction, sometimes requiring cardiac bypass surgery or transplant.2
Coronary artery changes in KD are not typically symptomatic in the acute phase, and physicians should remain cognizant that the myocardium and endocardium may become inflamed, which could manifest as tachycardia, a hyperdynamic precordium, a gallop rhythm, and accentuation of flow murmurs.2 Valvular dysfunction has been reported in about 25% of patients with KD (with the mitral valve being the most commonly affected), whereas aortic root dilation has been reported in about 10% of cases.15 In about 5% of children with KD in the continental United States, intracardiac inflammation can lead to severe tachycardia, hypotension, and cardiovascular collapse, also known as KD shock syndrome.2
Similarly to KD, MIS-C can have profound cardiac manifestations, the principal of which is shock, which can lead to death.8 Although shock is rare in KD, most patients with reported MIS-C develop hypotension, likely because of a combination of cardiac dysfunction and systemic vasodilation,16 and require admission to an intensive care unit.17 Echocardiography is used to visualize the coronary arteries and to establish the degree of cardiac dysfunction, which has been noted in about 30% of patients with MIS-C in the United States.16,17 Reports have cited a range of rates of coronary artery dilation or aneurysms in MIS-C; one large cohort of 1,733 patients in the United States reported that 16.5% of those with MIS-C developed coronary artery changes, similar to the rate in untreated KD.17 In addition to echocardiography, electrocardiography has an important diagnostic role in MIS-C because electrocardiographic changes and cardiac arrhythmias, including ST segment changes, premature beats, QTc prolongation, atrioventricular block, and sustained life-threatening arrhythmias, have been well described.16,18
Laboratory Findings
The laboratory findings of KD and MIS-C indicate systemic inflammation; however, some key differences exist. Table 4 provides a comparison of the laboratory values found in an early cohort of patients with MIS-C in England and a large cohort of patients with KD in San Diego, Calif.2,6,7,11 Diagnostic workup for children with suspected MIS-C should include complete blood count, complete metabolic panel, erythrocyte sedimentation rate, C-reactive protein, and SARS-CoV-2 polymerase chain reaction and/or serologies. Additional workup includes B-type natriuretic peptide, troponin, ferritin, prothrombin time, partial thromboplastin time, d dimer, fibrinogen, lactate dehydrogenase, cytokine panel, electrocardiography, and chest radiography.19 In KD, inflammatory markers, including erythrocyte sedimentation rate, C-reactive protein, ferritin, and d dimer, are most often mildly to moderately elevated. Patients with MIS-C tend to have very high markers of inflammation, especially C-reactive protein values.11
In complete blood count values, patients with KD typically demonstrate elevated white blood cell counts.2 Patients with MIS-C present with a low absolute lymphocyte count and frank lymphocytopenia. Both illnesses manifest with mild to moderate anemia, although it tends to be more profound in MIS-C.11 The platelet count is another area of divergence: Patients with KD classically develop thrombocytosis, with platelet counts of more than 450,000 per μL (450 × 109 per L) after seven days of illness, whereas patients with MIS-C tend to develop mild to severe thrombocytopenia.11
Elevated transaminase and decreased albumin levels can occur in patients with both illnesses.11 The hypoalbuminemia in KD tends to be mild, but it can be severe in patients with MIS-C and lead to complications, such as pulmonary edema, especially in the setting of aggressive fluid resuscitation.
Finally, the elevation of troponin and B-type natriuretic peptide is a notable difference between patients with MIS-C and those with KD. Troponin and B-type natriuretic peptide levels are not routinely evaluated in KD, but in children with KD whose levels were measured, elevations were minimal.11
Treatment
The fundamental goal of treatment for patients with KD and MIS-C is to rapidly reduce systemic inflammation. Intravenous immune globulin (IVIG), 2 g per kg in a single dose, has been a long-established therapy for KD and is an effective way to reduce vascular inflammation, improve symptoms, and reduce risk of coronary artery abnormalities.2,20–24 High-dose aspirin (80 to 100 mg per kg per day) has been used for decades for anti-inflammatory effect; however, no evidence supports a reduction in coronary artery abnormalities.25,26 Many clinicians have begun to use medium-dose aspirin (30 to 50 mg per kg per day) or low-dose aspirin (3 to 5 mg per kg per day) during the acute phase to avoid the potential toxicity of high-dose aspirin.27 Low-dose aspirin provides an antiplatelet effect, given the risk of clotting in patients who develop aneurysms.2 Systemic corticosteroids for the treatment of KD have been a subject of controversy, but a landmark randomized controlled trial published in 2012 (RAISE study) demonstrated a clear benefit in Japanese children who were at high risk.28 A subsequent meta-analysis of 16 trials supported the role of corticosteroids as well, especially in early, severe KD.29 Most of the trials were conducted in Japan, where validated scoring tools are available to identify high-risk patients; thus, results may not be generalizable to other populations, and large practice variation exists. Some centers and KD experts have advocated for the addition of corticosteroids in the treatment of North American patients at high risk of IVIG resistance, including those with coronary artery aneurysms at diagnosis, those younger than 12 months, those with KD shock syndrome, and those who have KD presenting with macrophage activation syndrome.30,31 There is no universally accepted dosing regimen, but corticosteroid courses similar to those used in the RAISE study have been proposed (methylprednisolone or prednisone in a dosage of 2 mg per kg per day for five days, followed by a two-week taper).31
Treatment for MIS-C is a topic of ongoing research and is based largely on expert opinion and therapies used in KD and other childhood inflammatory conditions. Given the severity of disease, patients with suspected MIS-C in the clinic setting should be quickly referred to the hospital, where a multidisciplinary and multispecialty team can assist with treatment recommendations.19 Supportive measures, including respiratory support and judicious fluid resuscitation, are critical to prevent patient morbidity and mortality. Many patients also require inotropic support.8 As in patients with KD, IVIG given at 2 g per kg has been a consensus first-line therapy for those with MIS-C.19,32 Low-dose aspirin is recommended to reduce the risk of thrombosis associated with coronary artery aneurysms.19 Corticosteroid use to improve outcomes in MIS-C is a topic of ongoing research. Early observational data have suggested that adjunctive systemic corticosteroids can reduce the course of fever in patients with MIS-C.33 Additional observational studies published in July 2021 had seemingly conflicting results, however, indicating a need for prospective trials using a standardized treatment approach.34–36 Immunomodulators such as anakinra (Kineret), an interleukin-1 receptor antagonist, have been recommended in severe cases, although no robust published data are available on their use.19
This article updates a previous article on this topic by Saguil, et al.37
Data Sources: Our review of the literature was conducted by searching PubMed Clinical Queries using the following key terms: pediatric multisystem inflammatory syndrome, SARSCoV-2 related, multisystem inflammatory syndrome in children, Kawasaki disease, mucocutaneous lymph node syndrome. The PubMed MeSH database was also used to search related terms. The search included meta-analyses, randomized controlled trials, clinical trials, reviews, letters to the editor, and case reports. Government disease-tracking websites, such as the Centers for Disease for Control and Prevention website on multisystem inflammatory syndrome in children, were also important sources of information and references. Search dates: January 19 and July 19, 2021.
The authors thank Dr. Lindsay Strowd and the Wake Forest School of Medicine Graham Archives Library for contributing the images included in this work.

