Case Scenario
I have a patient, K.B., with a three-year history of asthma. The patient's parent is concerned because K.B. wakes every night coughing. The family just moved to an apartment that does not have air conditioning and has received several code violations for a leaking roof and windows. The apartment is located next to two major interstate highways and is 10 miles from a cement factory. Air quality has reached the orange zone several times this month, and pollen levels have been consistently high for several months. I have provided the parent with an Asthma Action Plan and updated K.B.'s medications according to current guidelines. I believe that the environmental factors exacerbate or even cause my patient's condition, so how do I talk with the family about these issues over which they have little or no control? How do I talk with a patient about issues such as air pollution or climate change and their impacts on health?
Commentary
This case provides an example of how the environment can have significant impacts on the health of our patients. It also illustrates the complex interaction of local, regional, and global environmental harms. The wide scope of environmental threats to human health presents challenges in managing patients who are increasingly affected by climate-related changes, including severe weather events, extreme heat, worsening air quality, increasing allergens, changes in vector ecology, water quality, food and water supply, and environmental degradation.1
The effects of climate change on individual and entire population health are well established.2,3 Many of these effects, especially those related to disruption of infrastructure, heat, and air pollution, are regional.4 Health harms disproportionately affect children, pregnant people, older adults, and those with limited resources and/or populations who are marginalized who have been disproportionately exposed to unhealthy environments due to a history of discriminatory policies. When wondering whether and how these health impacts should be discussed with a patient, physicians should be knowledgeable about the daily life and circumstances of the patient and trust that patients recognize their family physicians as credible sources of information and support.
GENERAL CONSIDERATIONS BEFORE INITIATING DISCUSSIONS
Although only limited evidence is available to guide clinicians on broaching discussions about climate change with patients, it can be helpful to remember that health care professionals, including physicians and nurses, have powerful voices and are among the most trusted individuals according to populations surveyed in the United States.5,6 Physicians also have an ethical obligation to discuss climate concerns with their patients7 because climate change has been determined as a health emergency and is identified as the greatest public health threat of our century.8,9 Finally, physicians hesitant to provide advice about environment and health should take solace from data showing that more than three-fourths of the U.S. adult population would support climate solutions if they benefited personal or public health.10,11 A patient-centered approach to such discussions addresses patients' specific health concerns while exploring their receptivity to a larger, climate-informed treatment plan. Table 1 suggests approaches to common physician concerns about conducting climate change conversations in the office setting.1,3,12–17
TABLE 1. Concerns and Considerations about Climate Counseling with Patients

| Practical concerns | Counseling considerations |
|---|---|
| How does climate change impact the health of my patients? | The health effects of climate change are well documented on the Centers for Disease Control and Prevention and World Health Organization websites1,12; in a report created by the Medical Society Consortium on Climate and Health13; and by summary reports published in The Lancet, Annals of Internal Medicine, and Pediatrics.3,14,15 |
| Do I have enough time to incorporate one more topic into my visits? | Physicians should prioritize which patient counseling topics to address and how to address them effectively and efficiently for each patient. Physicians should seek resources and determine the best ways to incorporate priority topic(s) into well-visit and problem-visit workflows. Consistent, simple, clear, and tailored messaging is recommended.16 Counseling generally should be brief (less than one minute) to improve patient receptivity. |
| Reimbursement and federal standards | Although no International Classification of Diseases-10 (ICD-10) codes currently reimburse for environmental justice–related activities, experts are currently working with federal leaders to incorporate the topic into the Centers for Medicare and Medicaid Services standards. This may ultimately influence reimbursement by other payors, quality assurance standards, and health systems rankings. Consistent shorter messaging is likely to be more effective than attempting to meet reimbursement criteria for time spent counseling. |
| This topic is too controversial, and/or I do not have support from my peers and patients | Multiple organizations, including the American Academy of Family Physicians, American College of Physicians, American Academy of Pediatrics, American College of Obstetricians and Gynecologists, and American Psychological Association, support health care professionals and leaders as they work to address climate change locally and nationally.17 |
| Physicians are already tasked with making difficult and potentially controversial health recommendations with which colleagues and patients sometimes disagree. Pediatric clinic data suggest that the risk of a negative patient response is exceptionally low (eTable A). Physicians have an obligation to communicate concern for the patient's health and to focus on the best possible outcomes. |
MAKING RELEVANT HEALTH RECOMMENDATIONS
A useful starting point for health care professionals wanting to familiarize themselves with key components of successful climate health messaging is found in ecoAmerica's communication guide.18 The guide provides specific examples of language to use when discussing the health impacts of fossil fuel–driven pollution and climate change. It recommends using positive and locally focused phrasing (“protect our families” rather than “stop climate change”) and offers key talking points, such as, “I'm a health professional because I care about the health of everyone in our community.”18
Studies and anecdotal reports are available, with examples of physicians successfully communicating climate change–related issues—particularly in areas of pediatrics or pulmonary medicine—where specific vulnerabilities and the relationship between climate-related factors and health conditions are clearly identified.19–21
An environment-focused management strategy includes evaluating individual vulnerabilities (e.g., assessing whether the patient has air conditioning, plans a pregnancy, lives near a power plant). Exploring indoor vs. outdoor sources of air pollution is essential. Cigarette smoke, gas stoves, and cleaning compounds are common indoor pollutants and, if present, should prompt discussion of ways to limit their harms. The strategy might also include assessing the use of specific medications, such as those that exacerbate the effects of heat22 or encouraging the use of dry powder as a more environmentally friendly option to propellant inhalers.22,23
Physicians can incorporate counseling about proactive and beneficial behaviors into patient consultations, such as reminding patients with respiratory disease to check the air quality before outdoor activities or promoting the benefits of walking and biking as healthy for individuals and community air quality. Physician recommendations can incorporate aspects of motivational interviewing techniques and do not necessarily require direct mention of climate change. A helpful approach highlights clean air and healthy behaviors that also benefit individuals, families, and the local community. The ecoAmerica's guide18 and eTable A provide detailed examples of counseling points and phrasing.
eTABLE A Addressing Climate Counseling within Clinical Encounters
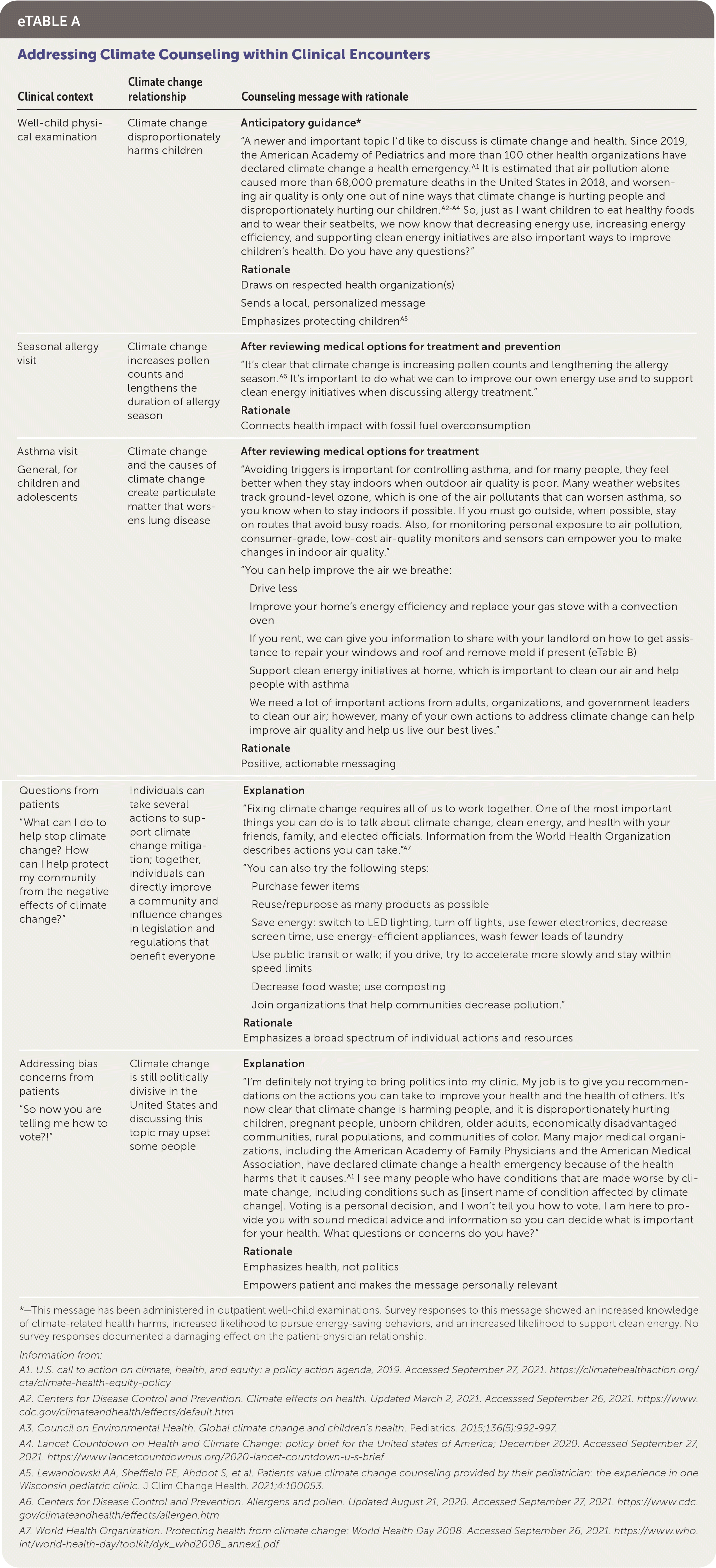
| Clinical context | Climate change relationship | Counseling message with rationale |
|---|---|---|
| Well-child physical examination | Climate change disproportionately harms children | Anticipatory guidance* “A newer and important topic I'd like to discuss is climate change and health. Since 2019, the American Academy of Pediatrics and more than 100 other health organizations have declared climate change a health emergency.A1 It is estimated that air pollution alone caused more than 68,000 premature deaths in the United States in 2018, and worsening air quality is only one out of nine ways that climate change is hurting people and disproportionately hurting our children.A2–A4 So, just as I want children to eat healthy foods and to wear their seatbelts, we now know that decreasing energy use, increasing energy efficiency, and supporting clean energy initiatives are also important ways to improve children's health. Do you have any questions?” Rationale Draws on respected health organization(s) Sends a local, personalized message Emphasizes protecting childrenA5 |
| Seasonal allergy visit | Climate change increases pollen counts and lengthens the duration of allergy season | After reviewing medical options for treatment and prevention “It's clear that climate change is increasing pollen counts and lengthening the allergy season.A6 It's important to do what we can to improve our own energy use and to support clean energy initiatives when discussing allergy treatment.” Rationale Connects health impact with fossil fuel overconsumption |
| Asthma visit General, for children and adolescents | Climate change and the causes of climate change create particulate matter that worsens lung disease | After reviewing medical options for treatment “Avoiding triggers is important for controlling asthma, and for many people, they feel better when they stay indoors when outdoor air quality is poor. Many weather websites track ground-level ozone, which is one of the air pollutants that can worsen asthma, so you know when to stay indoors if possible. If you must go outside, when possible, stay on routes that avoid busy roads. Also, for monitoring personal exposure to air pollution, consumer-grade, low-cost air-quality monitors and sensors can empower you to make changes in indoor air quality.” “You can help improve the air we breathe: Drive less Improve your home's energy efficiency and replace your gas stove with a convection oven If you rent, we can give you information to share with your landlord on how to get assistance to repair your windows and roof and remove mold if present (eTable B) Support clean energy initiatives at home, which is important to clean our air and help people with asthma We need a lot of important actions from adults, organizations, and government leaders to clean our air; however, many of your own actions to address climate change can help improve air quality and help us live our best lives.” Rationale Positive, actionable messaging |
| Questions from patients “What can I do to help stop climate change? How can I help protect my community from the negative effects of climate change?” | Individuals can take several actions to support climate change mitigation; together, individuals can directly improve a community and influence changes in legislation and regulations that benefit everyone | Explanation “Fixing climate change requires all of us to work together. One of the most important things you can do is to talk about climate change, clean energy, and health with your friends, family, and elected officials. Information from the World Health Organization describes actions you can take.”A7 “You can also try the following steps: Purchase fewer items Reuse/repurpose as many products as possible Save energy: switch to LED lighting, turn off lights, use fewer electronics, decrease screen time, use energy-efficient appliances, wash fewer loads of laundry Use public transit or walk; if you drive, try to accelerate more slowly and stay within speed limits Decrease food waste; use composting Join organizations that help communities decrease pollution.” Rationale Emphasizes a broad spectrum of individual actions and resources |
| Addressing bias concerns from patients “So now you are telling me how to vote?!” | Climate change is still politically divisive in the United States and discussing this topic may upset some people | Explanation “I'm definitely not trying to bring politics into my clinic. My job is to give you recommendations on the actions you can take to improve your health and the health of others. It's now clear that climate change is harming people, and it is disproportionately hurting children, pregnant people, unborn children, older adults, economically disadvantaged communities, rural populations, and communities of color. Many major medical organizations, including the American Academy of Family Physicians and the American Medical Association, have declared climate change a health emergency because of the health harms that it causes.A1 I see many people who have conditions that are made worse by climate change, including conditions such as [insert name of condition affected by climate change]. Voting is a personal decision, and I won't tell you how to vote. I am here to provide you with sound medical advice and information so you can decide what is important for your health. What questions or concerns do you have?” Rationale Emphasizes health, not politics Empowers patient and makes the message personally relevant |
*—This message has been administered in outpatient well-child examinations. Survey responses to this message showed an increased knowledge of climate-related health harms, increased likelihood to pursue energy-saving behaviors, and an increased likelihood to support clean energy. No survey responses documented a damaging effect on the patient-physician relationship.
Information from:
A1. U.S. call to action on climate, health, and equity: a policy action agenda, 2019. Accessed September 27, 2021. https://climatehealthaction.org/cta/climate-health-equity-policy
A2. Centers for Disease Control and Prevention. Climate effects on health. Updated March 2, 2021. Accessed September 26, 2021. https://www.cdc.gov/climateandhealth/effects/default.htm
A3. Council on Environmental Health. Global climate change and children's health. Pediatrics. 2015;136(5):992–997.
A4. Lancet Countdown on Health and Climate Change: policy brief for the United states of America; December 2020. Accessed September 27, 2021. https://www.lancetcountdownus.org/2020-lancet-countdown-u-s-brief
A5. Lewandowski AA, Sheffield PE, Ahdoot S, et al. Patients value climate change counseling provided by their pediatrician: the experience in one Wisconsin pediatric clinic. J Clim Change Health. 2021;4:100053.
A6. Centers for Disease Control and Prevention. Allergens and pollen. Updated August 21, 2020. Accessed September 27, 2021. https://www.cdc.gov/climateandhealth/effects/allergen.htm
A7. World Health Organization. Protecting health from climate change: World Health Day 2008. Accessed September 26, 2021. https://www.who.int/world-health-day/toolkit/dyk_whd2008_annex1.pdf
Finally, the clinical environment can model a strategy of climate-friendly practices and offer resources such as office-based posters and materials to engage, inform, and encourage patients about practical climate-friendly interventions (https://climatehealthconnect.org/resources/posters). By making these educational materials available, health messages become integral to the office culture and encourage staff and colleagues to incorporate climate-aware approaches into their personal and professional interactions.
INTEGRATING ENVIRONMENTAL JUSTICE CONCERNS INTO COMMUNITY PRACTICE
Globally and locally, climate disasters and environmental pollutants disproportionately affect Black, Indigenous, and other communities of color.8,24 Because of structural discriminatory practices, Black and Hispanic individuals are more likely than other population groups to live in heat islands, flood zones, and contaminated environments.25 These health disparities highlight the need to address socioeconomic and racial equality issues as an integral part of environmental equity. For instance, White individuals in the United States consume more air-polluting goods and services than Black and Hispanic individuals, but White individuals experience 17% less air-pollution exposure. Black and Hispanic individuals experience 56% and 63%, respectively, greater exposure to pollutants than is caused by their consumption.25,26 Physicians should be ready to combat local policies that penalize marginalized communities (e.g., gentrification, which displaces lower-income residents), while supporting those that will improve environmental conditions without adverse socioeconomic consequences. Engagement on a policy level might include staying informed of local climate-related legislation and responding to opportunities for the public to give comments and feedback to officials. Physicians should integrate racial and environmental equity into discussions with patients and use concrete examples of specific vulnerabilities relevant to their community (Table 2). Information about asthma rates in a patient's zip code or county is available from County Health Rankings & Roadmaps (https://www.countyhealthrankings.org/explore-health-rankings) and Places: Local Data for Better Health (https://www.cdc.gov/places/index.html). Specific examples and patient stories are also among the most effective strategies for advocacy to groups and decision makers.18,27 Physicians who are a part of communities of color or marginalized communities can have an especially significant impact as trusted voices and respected leaders within a community.
TABLE 2. Discussing Climate Change and Equity with Patients

| Patient questions about equity “I didn't know that climate change was hurting some people more than others. Who does climate change harm the most?” | Climate change disproportionately harms vulnerable individuals and those living in socioeconomically and racially marginalized communities | Explanation “Although climate change harms all of us, its health burdens do not fall on everyone equally. Some people, such as children, older adults, people with chronic medical conditions, and pregnant people, are more likely to be harmed because of differences in how their bodies respond to their environment and because of a comparatively greater reliance on their community to support them. The lifestyle, lack of community-shared infrastructure, and work environments make rural communities more vulnerable to extreme heat, income loss, insect-spread diseases, and water contamination. Black, Indigenous, and other communities of color are disproportionately harmed by extreme heat, poor air quality, and flooding because of a legacy of policies that have not been adequately addressed, leading to continued and lasting effects on those communities today. As a result, we all need to know how individuals and communities are harmed by climate change if we are going to create fair, justice-informed solutions.” Rationale Improving conditions for disproportionately affected individuals invites allyship and supports development of better climate solutions. It also incorporates moral standards of responsibility and care. |
Ultimately, climate-aware physicians should look beyond their practices.28 According to a recently updated conceptual model outlining defining principles for primary care, practices should “seek out the impact of social determinants of health and social inequities.”29 This model recommends that primary care practices develop partnerships with health and community-based organizations to be able to address the broader context of their patients' lives, including the environment. Conversations about the environmental determinants of health should take place in the patients' communities—where they live, work, and play.
Case Scenario Resolution
The physician and parent in the case scenario should discuss the relationship between the asthma exacerbation and environmental factors. In this case, clarifying the significance of highway proximity, factory emissions, and housing is a priority. Together, they should identify and initiate practical interventions for those factors that can be addressed, develop clinically appropriate creative solutions for more intractable issues, and explore community-focused efforts to improve local conditions overall. The physician's team can assist the family in accessing the AirNow website (https://www.airnow.gov/) or in downloading the free Daily Breath app (https://www.dailybreathforecast.com/) to check daily air quality and advise the family on how to adjust outdoor exposure accordingly. The preferential use of dry-powder inhalers should be discussed if applicable. The health care team can help the family explore transportation options, especially daily journeys to and from school, to reduce pollution exposure. Team members should investigate resources to repair leaks and install fans (lower carbon output) and/or air conditioning, air filters, or dehumidifiers to improve indoor air quality and to protect against the impact of higher ambient temperatures. Other beneficial installations include air purifiers; indoor air-quality monitors; and MERV-13 heating, ventilation, and air-conditioning (HVAC) filters (upkeep and replacement of soiled filters are also crucial; eTable B). Participation in local organizations and activities promoting better air quality and housing conditions should be encouraged. The physician can also commit to supporting such efforts, for instance, by speaking publicly on behalf of the community or accessing, compiling, and preparing in lay terms relevant data and results and recommendations from scientific reports.
eTABLE B Additional Resources on Climate Counseling with Patients
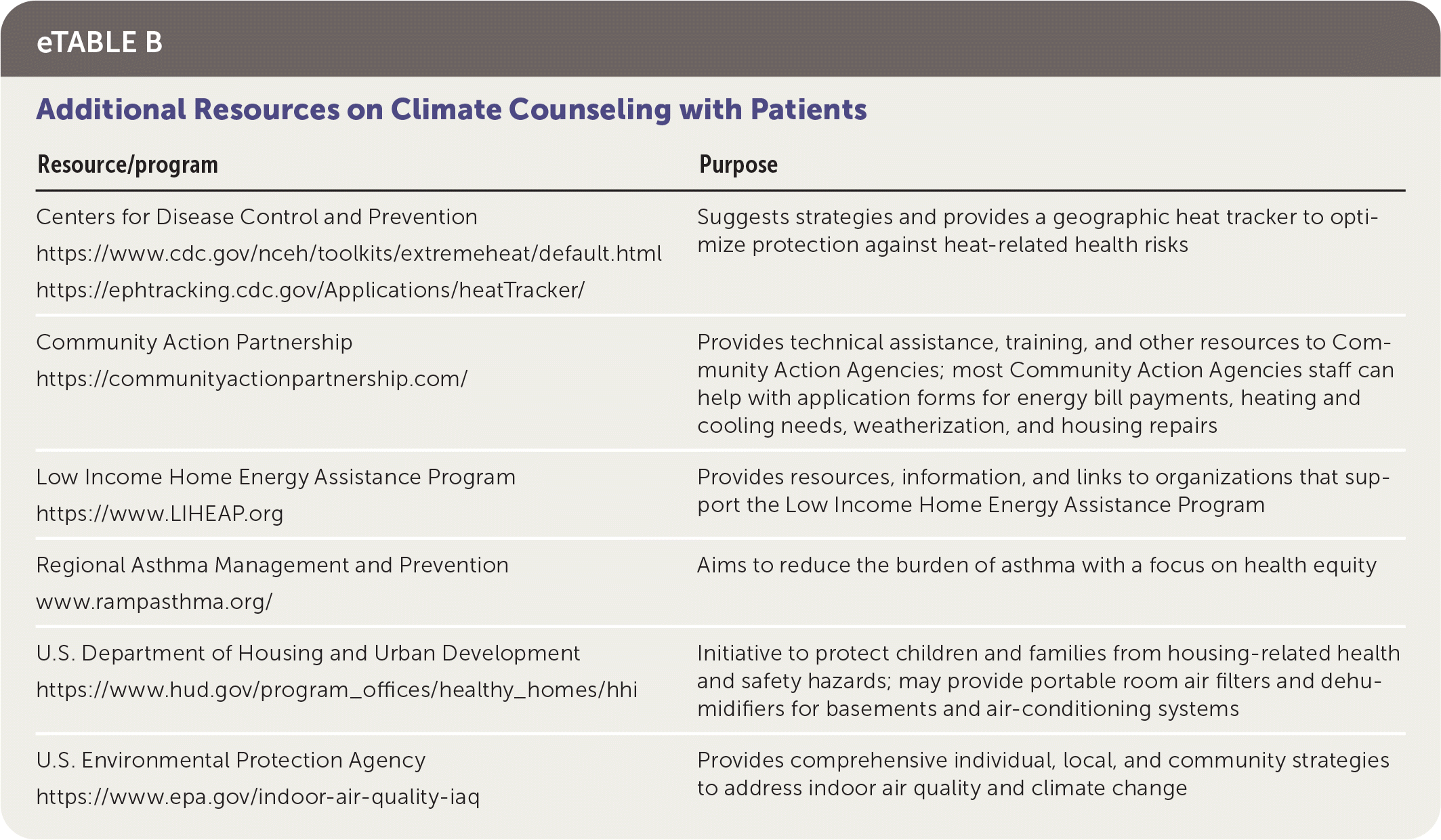
| Resource/program | Purpose |
|---|---|
| Centers for Disease Control and Prevention https://www.cdc.gov/nceh/toolkits/extremeheat/default.html https://ephtracking.cdc.gov/Applications/heatTracker/ | Suggests strategies and provides a geographic heat tracker to optimize protection against heat-related health risks |
| Community Action Partnership https://communityactionpartnership.com/ | Provides technical assistance, training, and other resources to Community Action Agencies; most Community Action Agencies staff can help with application forms for energy bill payments, heating and cooling needs, weatherization, and housing repairs |
| Low Income Home Energy Assistance Program https://www.LIHEAP.org | Provides resources, information, and links to organizations that support the Low Income Home Energy Assistance Program |
| Regional Asthma Management and Prevention www.rampasthma.org/ | Aims to reduce the burden of asthma with a focus on health equity |
| U.S. Department of Housing and Urban Development https://www.hud.gov/program_offices/healthy_homes/hhi | Initiative to protect children and families from housing-related health and safety hazards; may provide portable room air filters and dehumidifiers for basements and air-conditioning systems |
| U.S. Environmental Protection Agency https://www.epa.gov/indoor-air-quality-iaq | Provides comprehensive individual, local, and community strategies to address indoor air quality and climate change |
The authors thank Jan-Michael Archer for his review.
Editor's Note: Dr. Wellbery is associate deputy editor for AFP.

