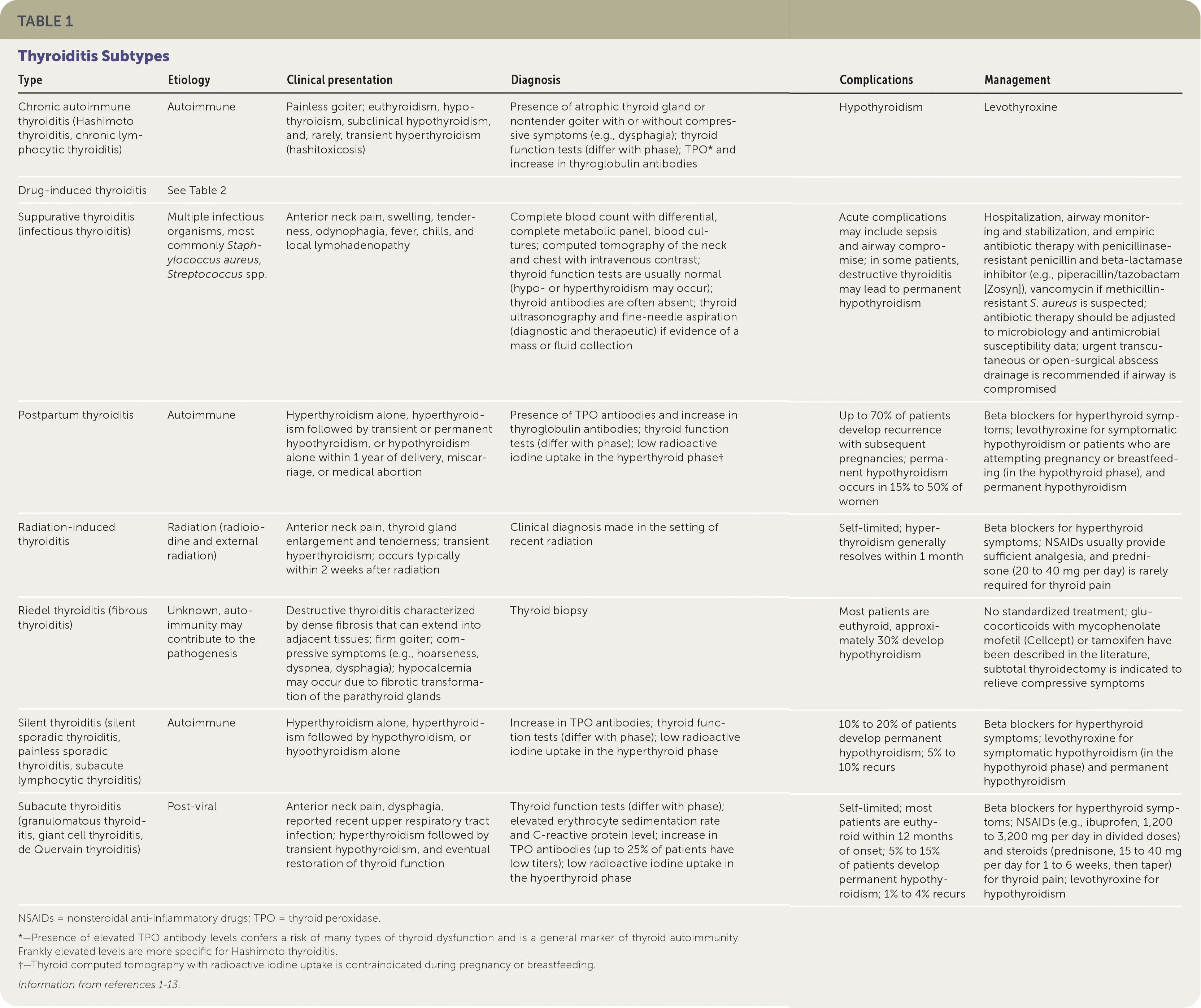
| Chronic autoimmune thyroiditis (Hashimoto thyroiditis, chronic lymphocytic thyroiditis) | Autoimmune | Painless goiter; euthyroidism, hypothyroidism, subclinical hypothyroidism, and, rarely, transient hyperthyroidism (hashitoxicosis) | Presence of atrophic thyroid gland or nontender goiter with or without compressive symptoms (e.g., dysphagia); thyroid function tests (differ with phase); TPO* and increase in thyroglobulin antibodies | Hypothyroidism | Levothyroxine |
| Drug-induced thyroiditis | See Table 2 | | | | |
| Suppurative thyroiditis (infectious thyroiditis) | Multiple infectious organisms, most commonly Staphylococcus aureus, Streptococcus spp. | Anterior neck pain, swelling, tenderness, odynophagia, fever, chills, and local lymphadenopathy | Complete blood count with differential, complete metabolic panel, blood cultures; computed tomography of the neck and chest with intravenous contrast; thyroid function tests are usually normal (hypo- or hyperthyroidism may occur); thyroid antibodies are often absent; thyroid ultrasonography and fine-needle aspiration (diagnostic and therapeutic) if evidence of a mass or fluid collection | Acute complications may include sepsis and airway compromise; in some patients, destructive thyroiditis may lead to permanent hypothyroidism | Hospitalization, airway monitoring and stabilization, and empiric antibiotic therapy with penicillinase-resistant penicillin and beta-lactamase inhibitor (e.g., piperacillin/tazobactam [Zosyn]), vancomycin if methicillin-resistant S. aureus is suspected; antibiotic therapy should be adjusted to microbiology and antimicrobial susceptibility data; urgent transcutaneous or open-surgical abscess drainage is recommended if airway is compromised |
| Postpartum thyroiditis | Autoimmune | Hyperthyroidism alone, hyperthyroidism followed by transient or permanent hypothyroidism, or hypothyroidism alone within 1 year of delivery, miscarriage, or medical abortion | Presence of TPO antibodies and increase in thyroglobulin antibodies; thyroid function tests (differ with phase); low radioactive iodine uptake in the hyperthyroid phase† | Up to 70% of patients develop recurrence with subsequent pregnancies; permanent hypothyroidism occurs in 15% to 50% of women | Beta blockers for hyperthyroid symptoms; levothyroxine for symptomatic hypothyroidism or patients who are attempting pregnancy or breastfeeding (in the hypothyroid phase), and permanent hypothyroidism |
| Radiation-induced thyroiditis | Radiation (radioiodine and external radiation) | Anterior neck pain, thyroid gland enlargement and tenderness; transient hyperthyroidism; occurs typically within 2 weeks after radiation | Clinical diagnosis made in the setting of recent radiation | Self-limited; hyperthyroidism generally resolves within 1 month | Beta blockers for hyperthyroid symptoms; NSAIDs usually provide sufficient analgesia, and prednisone (20 to 40 mg per day) is rarely required for thyroid pain |
| Riedel thyroiditis (fibrous thyroiditis) | Unknown, auto-immunity may contribute to the pathogenesis | Destructive thyroiditis characterized by dense fibrosis that can extend into adjacent tissues; firm goiter; compressive symptoms (e.g., hoarseness, dyspnea, dysphagia); hypocalcemia may occur due to fibrotic transformation of the parathyroid glands | Thyroid biopsy | Most patients are euthyroid, approximately 30% develop hypothyroidism | No standardized treatment; glucocorticoids with mycophenolate mofetil (Cellcept) or tamoxifen have been described in the literature, subtotal thyroidectomy is indicated to relieve compressive symptoms |
| Silent thyroiditis (silent sporadic thyroiditis, painless sporadic thyroiditis, subacute lymphocytic thyroiditis) | Autoimmune | Hyperthyroidism alone, hyperthyroidism followed by hypothyroidism, or hypothyroidism alone | Increase in TPO antibodies; thyroid function tests (differ with phase); low radioactive iodine uptake in the hyperthyroid phase | 10% to 20% of patients develop permanent hypothyroidism; 5% to 10% recurs | Beta blockers for hyperthyroid symptoms; levothyroxine for symptomatic hypothyroidism (in the hypothyroid phase) and permanent hypothyroidism |
| Subacute thyroiditis (granulomatous thyroiditis, giant cell thyroiditis, de Quervain thyroiditis) | Post-viral | Anterior neck pain, dysphagia, reported recent upper respiratory tract infection; hyperthyroidism followed by transient hypothyroidism, and eventual restoration of thyroid function | Thyroid function tests (differ with phase); elevated erythrocyte sedimentation rate and C-reactive protein level; increase in TPO antibodies (up to 25% of patients have low titers); low radioactive iodine uptake in the hyperthyroid phase | Self-limited; most patients are euthyroid within 12 months of onset; 5% to 15% of patients develop permanent hypothyroidism; 1% to 4% recurs | Beta blockers for hyperthyroid symptoms; NSAIDs (e.g., ibuprofen, 1,200 to 3,200 mg per day in divided doses) and steroids (prednisone, 15 to 40 mg per day for 1 to 6 weeks, then taper) for thyroid pain; levothyroxine for hypothyroidism |