A 59-year-old man presented with a progressive full-body rash. The pruritic rash began on his extremities approximately six months earlier and was initially diagnosed as drug-related exanthem secondary to a calcium channel blocker. The patient was prescribed topical and oral steroids. Soon after finishing the steroids, his rash became progressively more widespread, involving the face, trunk, and all extremities. He also reported generalized weakness, small joint arthritis, and neuropathy. The patient did not have known contact allergens or exposures. His medical history included hypertension and hypothyroidism.
Physical examination revealed confluent erythroderma of the scalp, face, trunk, back, extremities, and groin (Figure 1). He had pitting edema and fissuring over both lower extremities with serous drainage. No nail involvement was observed. Two 4-mm punch biopsies were performed.
FIGURE 1
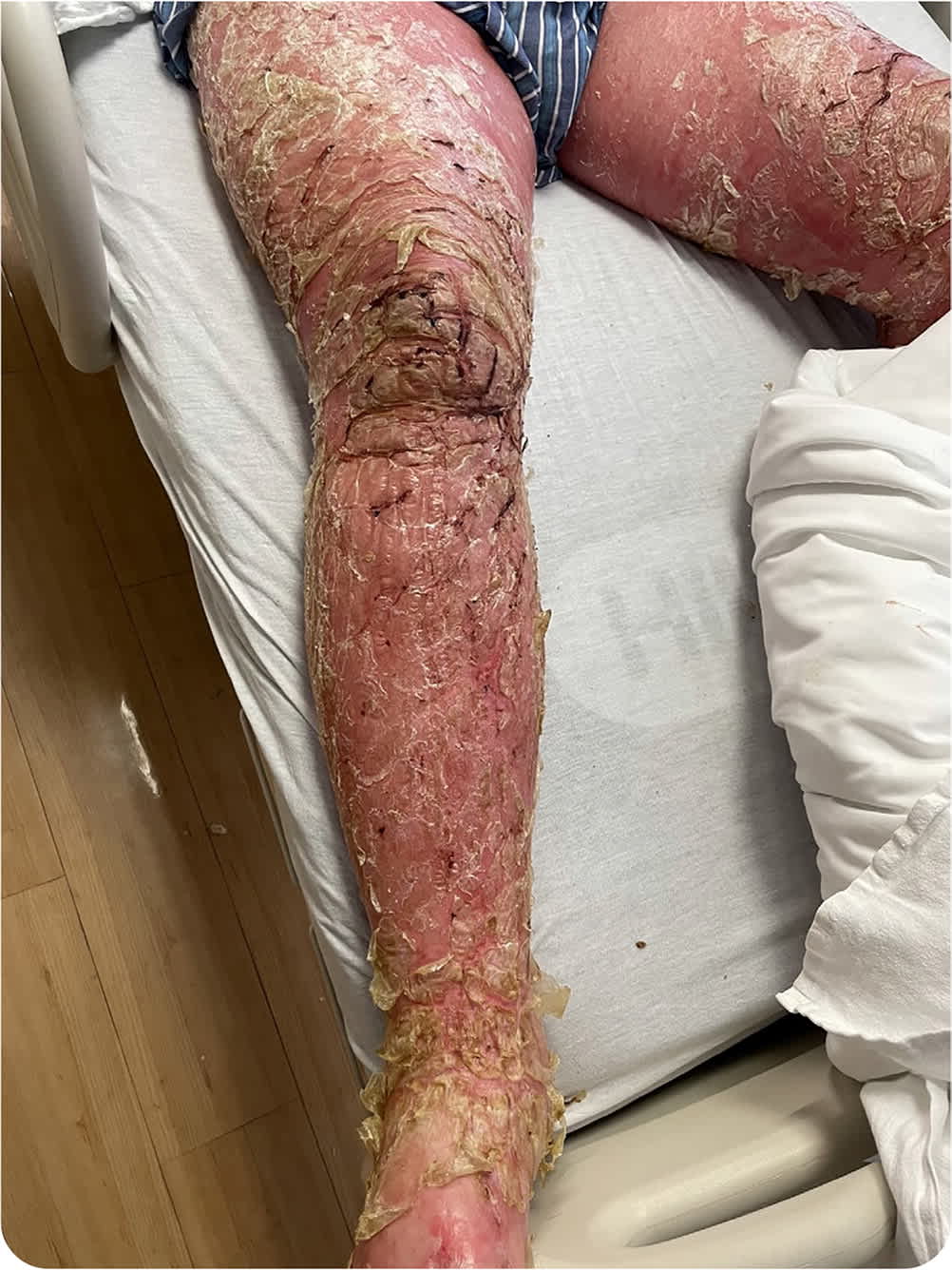
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
- A. Atopic dermatitis.
- B. Drug-induced erythroderma.
- C. Erythrodermic pityriasis rubra pilaris.
- D. Psoriasis.
- E. Staphylococcal scalded skin syndrome.
Discussion
The answer is D: psoriasis. Psoriasis is the most common cause of erythroderma in adults.1 Erythroderma, also known as exfoliative dermatitis, is defined as erythema and scaling that comprise more than 80% of the body surface area.2 Erythroderma has numerous potential causes, making treatment difficult. About 50% of cases arise from a preexisting skin condition. Erythroderma can also be due to drug reactions or cutaneous T cell lymphoma.2,3 Because of the rapid cell turnover in erythroderma, many of the cell contents (e.g., nucleic acids, amino acids) are lost as the skin sloughs. This can lead to complications such as hypoalbuminemia, peripheral edema, high-output heart failure, anemia, lymphadenopathy, and hypo- or hyperthermia.2
Features of psoriatic erythroderma include preexisting psoriatic plaques, sparing of the central face, and nail changes (e.g., onycholysis, oil drop sign, pitting, subungual hyperkeratosis). The typical features of psoriasis can fade as the erythrodermic reaction becomes more widespread, with disseminated, sterile subcorneal pustules taking the place of plaques. This is commonly precipitated by the withdrawal of medications such as corticosteroids, methotrexate, or cyclosporine (Sandimmune).1,2
Atopic dermatitis erythroderma presents as a widespread intensely pruritic, erythematous rash. Lichenification with white scaling can occur, along with the preexisting eczematous lesions. Increased serum immunoglobulin E and eosinophils are nonspecific findings that may be present.2,3
Drug-induced erythroderma presents as fever, possible peripheral eosinophilia, lymphadenopathy, and hepatitis. Drug reactions caused by systemic medications usually begin as a morbilliform or scarlatiniform exanthem.2,4 A drug reaction with eosinophilia and systemic symptoms (DRESS) is one type of reaction that can lead to erythroderma. DRESS develops two to six weeks after initiation of the inducing medication.2
Erythrodermic pityriasis rubra pilaris presents as salmon-colored to orange-red lesions with varying scales. Follicular keratotic papules on the elbows, knees, and dorsal aspects of the fingers are often present. Islands of sparing within the erythroderma, along with the follicular keratotic papules, make the diagnosis more likely.2,5
Staphylococcal scalded skin syndrome, an acute skin condition that typically occurs in infants and young children, often becomes erythrodermic. Painful areas of erythema develop on the skin 24 to 48 hours following infection with exfoliative toxin–positive Staphylococcus aureus. Soon after, flaccid subcorneal blisters appear and then slough off to expose underlying skin that is moist and red. Mucous membranes are spared.2
SUMMARY TABLE
| Condition | Characteristics |
|---|---|
| Atopic dermatitis | Widespread intensely pruritic, erythematous rash; eczematous lesions; lichenification |
| Drug-induced erythroderma | Morbilliform or scarlatiniform exanthem; facial edema |
| Erythrodermic pityriasis rubra pilaris | Salmon-colored to orange-red lesions with varying scales; follicular keratotic papules; islands of sparing within the erythroderma |
| Psoriasis | Preexisting psoriatic plaques, sparing of the central face; nail changes (e.g., onycholysis, oil drop sign, pitting, subungual hyperkeratosis) |
| Staphylococcal scalded skin syndrome | Painful erythema followed by flaccid subcorneal blisters that slough off; mucous membranes are spared; most common in infants and young children |

