A 20-year-old man presented with a six-month history of inflamed bumps and what appeared to be focal bruising on his legs, thighs, and arms that left persistent hyperpigmentation after resolution. The rash had been exacerbated by heat exposure and appeared worse at night. He had joint pain and paresthesia but no photosensitivity, malar rash, alopecia, or mouth ulcers. When he consulted a rheumatologist, he had an elevated antinuclear antibody titer of 1:160. The patient was taking aspirin and acetaminophen and using a topical diclofenac sodium solution. He had no relevant family, medical, or social history. He did not abuse alcohol.
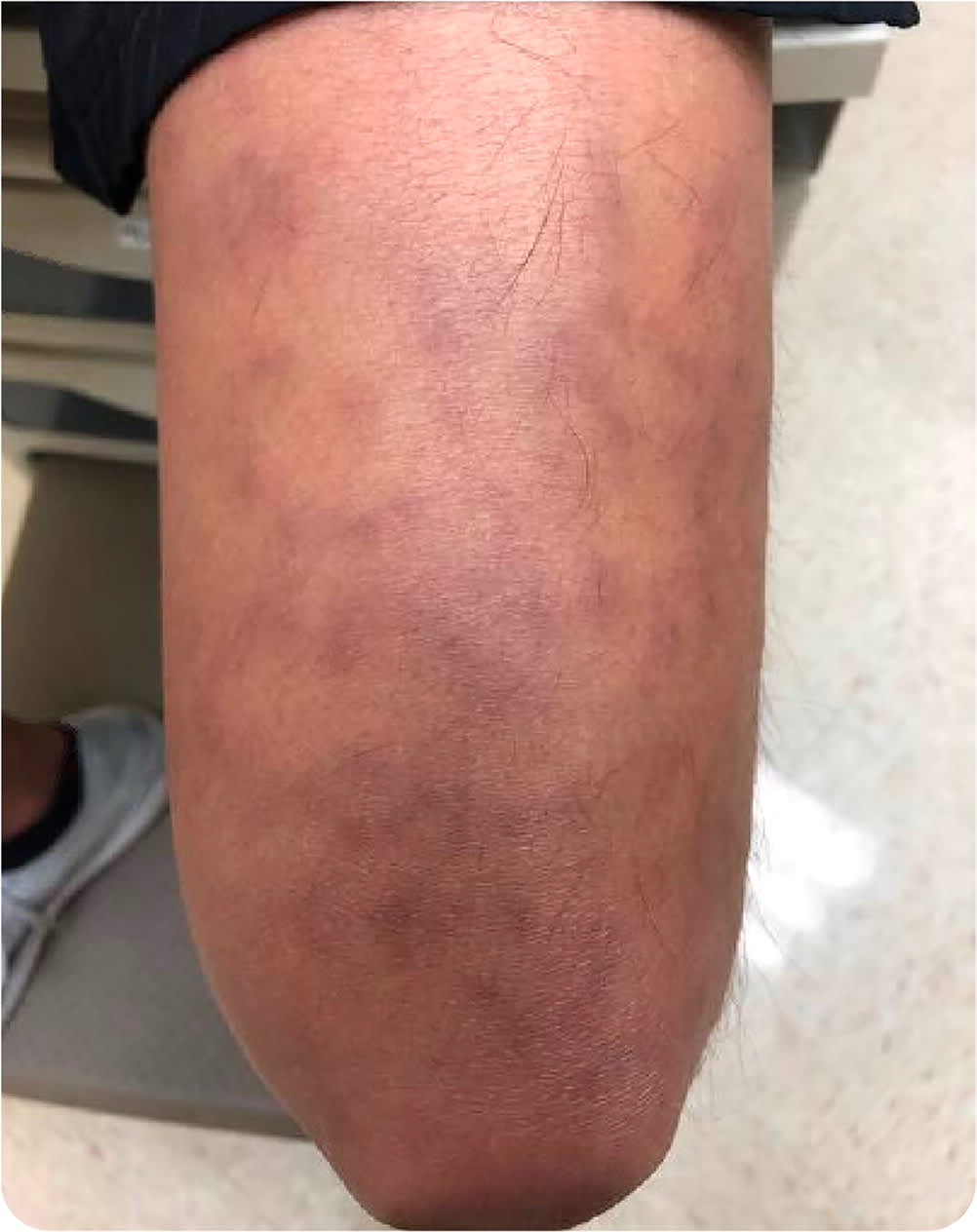
Physical examination revealed faint, dark purple, hyperpigmented patches in a reticular pattern, forming several complete rings on his dorsal thighs and a few on his lower legs and arms (Figure 1).
FIGURE 1
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
- A. Cutaneous polyarteritis nodosa.
- B. Drug hypersensitivity reaction.
- C. Takayasu arteritis.
- D. Urticarial vasculitis.
Discussion
The answer is A: cutaneous polyarteritis nodosa, a medium-sized vasculitis limited to the skin. It presents with tender nodules, digital infarcts, livedo reticularis, retiform purpura, ulcerations, or necrosis with or without mild systemic symptoms (e.g., headache, joint pain, paresthesia).1 Cutaneous polyarteritis nodosa typically manifests between 40 and 50 years of age; however, it may present in children and adolescents.2 Up to 60% of patients with cutaneous polyarteritis nodosa develop extracutaneous symptoms.2 Transformation of cutaneous to systemic polyarteritis nodosa is rare.
The etiology and pathogenesis of polyarteritis nodosa are unknown but are hypothesized to be multifactorial because of the varying clinical manifestations and multiorgan involvement.1 Immune complex deposition of C3 and immunoglobulin M in medium-sized arteries has been identified.1 For diagnosis, a biopsy must be of an adequate depth to ensure sampling of these arteries.1 This can be accomplished by an incisional biopsy, a deep punch biopsy, or a telescoping punch biopsy.
In this patient, a punch biopsy of the rash on his left arm showed a medium-sized, deep dermal arteriole with perivascular inflammation comprised of neutrophils, lymphocytes, and a few histiocytes and eosinophils. No necrosis was seen in the vessel wall, but an older organized thrombus was present within the arteriole. The inflammation was localized to this solitary dermal vessel.
Systemic polyarteritis nodosa affects the liver, heart, lung, and kidney. Evaluation must identify patients who have cutaneous symptoms of the systemic form of polyarteritis nodosa because symptoms are similar to the cutaneous form. The evaluation may include nerve conduction studies for paresthesia; muscle enzymes for myalgias; stool guaiac testing for abdominal pain; echocardiography to evaluate for congestive heart failure and coronary involvement; and computed tomographic or magnetic resonance angiography to identify visceral polyarteritis nodosa in patients with abdominal pain, hypertension, renal dysfunction, or other systemic symptoms.1
Treatment for cutaneous polyarteritis nodosa includes anti-inflammatory drugs such as colchicine and dapsone, with systemic glucocorticoids for acute flare-ups, which may be required long term.1 This patient was given a trial of prednisone therapy, 60 mg daily, with a taper to 6 mg daily.
Drug hypersensitivity reaction can have variable clinical presentations with or without organ dysfunction. Biopsy shows significant interface dermatitis with the presence of individual necrotic keratinocytes and a mixed dermal infiltrate. The patient would also have a history of high-risk medication use.3
Takayasu arteritis is a large vessel vasculitis that primarily affects the aorta and its branches. It presents with constitutional symptoms, arthralgia, weak peripheral pulses, skin lesions resembling erythema nodosum or pyoderma gangrenosum, and carotidynia.4 Biopsy shows inflammation in aortic tissue that consists mainly of cytotoxic lymphocytes, especially gamma delta T lymphocytes.
Urticarial vasculitis presents with recalcitrant pruritic, erythematous papules and plaques that resemble urticaria but persist for more than 24 hours and bruising. Biopsy shows signs of leukocytoclastic vasculitis with injury and enlargement of endothelial cells, extravasation of red blood cells, leukocytoclasis, fibrin deposition in and surrounding vessels, and perivascular infiltrate of neutrophils.5
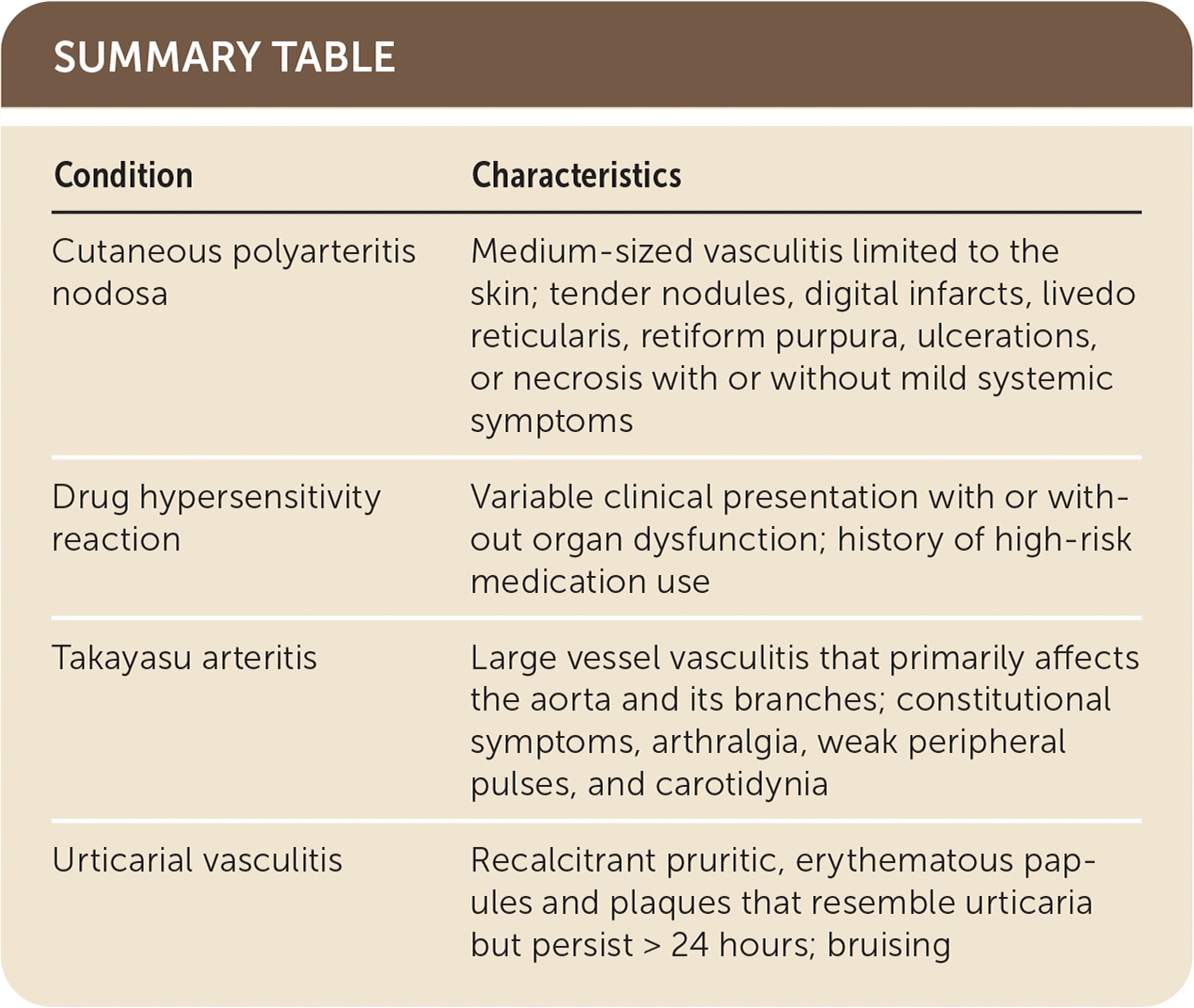
SUMMARY TABLE
| Condition | Characteristics |
|---|---|
| Cutaneous polyarteritis nodosa | Medium-sized vasculitis limited to the skin; tender nodules, digital infarcts, livedo reticularis, retiform purpura, ulcerations, or necrosis with or without mild systemic symptoms |
| Drug hypersensitivity reaction | Variable clinical presentation with or without organ dysfunction; history of high-risk medication use |
| Takayasu arteritis | Large vessel vasculitis that primarily affects the aorta and its branches; constitutional symptoms, arthralgia, weak peripheral pulses, and carotidynia |
| Urticarial vasculitis | Recalcitrant pruritic, erythematous papules and plaques that resemble urticaria but persist > 24 hours; bruising |

