Case Scenario
I am the family physician for a family of four and have cared for both children, currently 15 and 13 years of age, since they were born. When I recommended human papilloma-virus (HPV) vaccination for their son, the mother declined, saying that HPV is a sexually transmitted infection and that she did not believe the immunization was necessary for their son. At a later visit, the mother refused HPV immunization when their daughter reached 11 years of age. While leaving the visit, the father pulled me aside to say that he disagreed with his wife's decision and would try to change her mind.
When effective vaccines against SARS-CoV-2 became available, the father chose to be vaccinated as soon as he became eligible, but the mother did not. She explained that she was not an “anti-vaxxer” but was worried about adverse effects that might appear long after the two-month period covered in the clinical trials on which emergency authorization of these vaccines was based. The day after the U.S. Food and Drug Administration authorized the vaccine for children 12 to 15 years of age, the father asked whether he could bring his children to receive their first doses of this vaccine and the HPV vaccine. Pleasantly surprised, I agreed and asked what had prompted his wife's change of heart. After a long pause, the father said that his wife was being unreasonable and that he would prefer that she not know until after the children had been vaccinated.
From a medical perspective, the benefits of these vaccinations greatly outweigh any potential adverse effects. However, am I obligated to inform the mother and obtain her consent?
Commentary
In addressing this case, it is important to note that the dissenting parent (the mother) has not informed the family physician that she adamantly opposes giving the vaccine; this opposition would provide explicit proscription. Importantly, in a legal context, a parent (the father) who shares legal guardianship of the children is actively providing consent. This creates certain contingencies and allowances, depending on the jurisdiction. Some states (e.g., Oregon) establish that “mature minors”—specifically defined as minors determined to be mature enough by the physician to understand the purposes/effects of the vaccine—can receive the vaccine without parental consent.1 Most states without mature minor allowances require one parent to physically accompany the minor or to submit a verified, signed document certifying consent.2
In this case, one parent (the father) fulfills this role. If the child has given no indication with verbal objections to being vaccinated and the jurisdiction has the one-parent requirement, the physician is legally permitted to give the vaccine (i.e., absent the one-parent requirement, the physician would not have latitude to provide vaccination).2
The vaccines being discussed in this case are authorized by the U.S. Food and Drug Administration, so administering them is a reasonable and medically recommended course of care. Vaccination represents an intervention in the best interest of the patient and public health. Any associated burdens, risks, or potential harms have been explained and at least addressed, if not mitigated, as best as possible within common practice of provision of federally approved vaccines.3,4 Ethics generally guide decisions and actions under the scope of the law. In this case, neither ethical nor legal considerations appear to require a health care professional to contact the other parent to provide and confirm unanimous consent. The tension/conflict presented here is an interpersonal one between spouses. The caveat, as noted previously, is to ascertain and confirm the local jurisdiction's requirements.
In jurisdictions where mature minors can receive care without parental consent, the Health Insurance Portability and Accountability Act of 1996 (HIPAA) constraints restrict revealing the type of (allowed) medical care afforded to the minor. In this case, the doctor-patient privilege cannot be breached. Such breaches are permissible only under certain serious circumstances, such as in the case of a public health– reportable issue or to inform a potential victim, and possibly authorities, of impending danger or harm.5,6 In the present case, no unreasonable risk (other than those de minimis, as noted by the Centers for Disease Control and Prevention7) will occur to the health of the children or third parties.
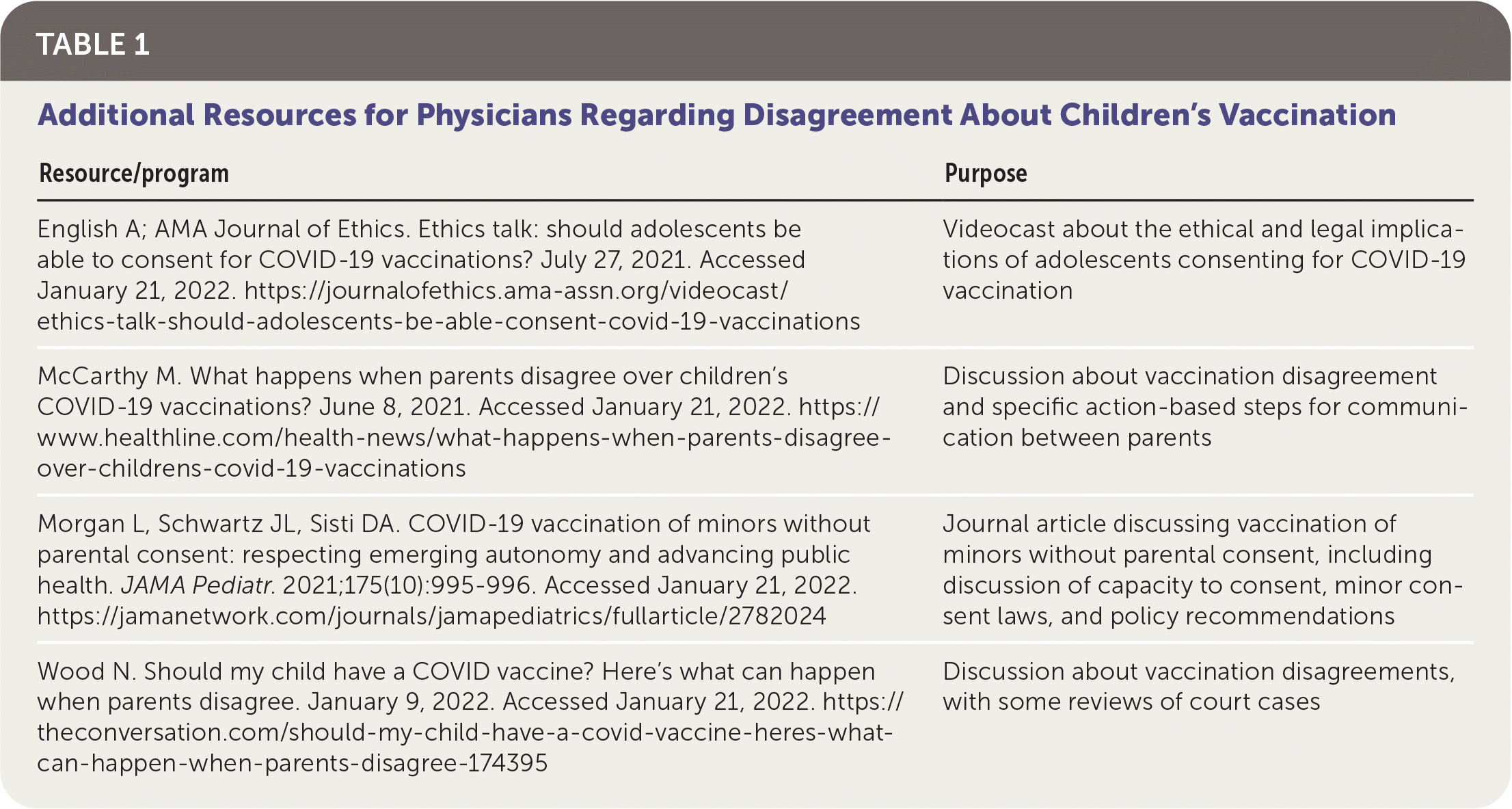
Regarding the discussion of the value of vaccination with the mother, health education and promotion are important (if not arguably obligate) aspects of clinical care. Such education requires effective, respectful, and tactful discussion of information. In the best interests of everyone involved, a conversation with both parents is warranted. In a real-time discussion, the necessary information should be provided in ways that avoid exacerbating the existing domestic conflict. This could be achieved by focusing on the positive effects of vaccination, including on the mother's health, and noting that her being vaccinated would also be of benefit to those with whom she has close contact. The conversation could acknowledge her previous concerns and provide updated information on vaccine safety from the latest long-term follow-up studies. Table 1 provides resources for physicians when speaking about childhood vaccination disagreement with parents.
TABLE 1. Additional Resources for Physicians Regarding Disagreement About Children's Vaccination
| Resource/program | Purpose |
|---|---|
| English A; AMA Journal of Ethics. Ethics talk: should adolescents be able to consent for COVID-19 vaccinations? July 27, 2021. Accessed January 21, 2022. https://journalofethics.ama-assn.org/videocast/ethics-talk-should-adolescents-be-able-consent-covid-19-vaccinations | Videocast about the ethical and legal implications of adolescents consenting for COVID-19 vaccination |
| McCarthy M. What happens when parents disagree over children's COVID-19 vaccinations? June 8, 2021. Accessed January 21, 2022. https://www.healthline.com/health-news/what-happens-when-parents-disagree-over-childrens-covid-19-vaccinations | Discussion about vaccination disagreement and specific action-based steps for communication between parents |
| Morgan L, Schwartz JL, Sisti DA. COVID-19 vaccination of minors without parental consent: respecting emerging autonomy and advancing public health. JAMA Pediatr. 2021;175(10):995–996. Accessed January 21, 2022. https://jamanetwork.com/journals/jamapediatrics/fullarticle/2782024 | Journal article discussing vaccination of minors without parental consent, including discussion of capacity to consent, minor consent laws, and policy recommendations |
| Wood N. Should my child have a COVID vaccine? Here's what can happen when parents disagree. January 9, 2022. Accessed January 21, 2022. https://theconversation.com/should-my-child-have-a-covid-vaccine-heres-what-can-happen-when-parents-disagree-174395 | Discussion about vaccination disagreements, with some reviews of court cases |
If the children have already been vaccinated without the mother's knowledge, however, the physician may, depending on state law and regulation, have no legal requirement to proactively communicate the vaccination status of her children, unless the mother raises the question directly, in which case ethical and legal precepts dictate truthful responses to her questions.8
It is reasonable to assume that the mother may react negatively if she learns that the physician has administered the vaccine. However, the physician may be well within ethical probity and legal rights to assert, as noted previously, that they were acting on the basis of one parent giving permission, depending on the laws and policy of the jurisdiction.4,8
The physician's future relationship with the mother, if not the entire family, may be affected; however, in a balance of interests, the physician could feel comfortable that the benefit of giving the vaccine outweighed the negative effect on the relationship with the mother and family.
Although the letter of the law may provide for consent of only one parent, if the physician's relationship with this family is particularly close and the physician is especially concerned about potential damage to the family and trust from all family members from this conflict, an alternative might be to refer the father to another colleague or facility to provide the vaccinations. However, this might not necessarily protect the ongoing relationship because the referral may be interpreted as being complicit in the husband's surreptitious actions. Another option would be that, if the physician believes that the historic hesitancy of the mother to take the vaccine with the husband's candid comment regarding the wife's “unreasonableness” equates to not wanting her children to be vaccinated, it may be appropriate to delay vaccination unless and until some unified decision from both parents is given. Finally, it is important to remember that the legal and ethical tenets presented here apply only to cases where parents are legally married. Different rules apply for those in other situations, such as in situations where couples are divorced, and would in most circumstances disallow one parent to choose vaccination against the wishes of the other.9
Case Resolution
In this scenario, ethical principles of beneficence, nonmaleficence, respect for patients' autonomy (even as minors), and constructs of confidentiality guide the decision to provide vaccinations to the children based on the children's assent and their father's explicit informed consent. The precepts of “one-parent consent” and/or mature minor status and capacity—as determined within the particular jurisdiction—provide the legal basis and grounds within which ethical considerations for the scope of care can and should be rendered. However, from ethical and legal perspectives, individual issues such as the physician's tolerance for conflict, concern for the family's harmony, and the relationship with patients may be grounds for differing, and somewhat more nuanced, courses of action. Thus, there are times when these decisions must be made on a case-by-case basis.
The opinions and assertions contained herein are the private views of the author and are not to be construed as official or as reflecting the views of the Department of Defense or the U.S. government.

