Community-acquired pneumonia (CAP) is a common condition with a hospitalization rate of about 2% in people 65 years or older and is associated with a 30-day mortality rate of 6% in hospitalized patients. In studies conducted before the COVID-19 pandemic, a bacterial pathogen was identified in 11% of patients, a viral pathogen in 23% of patients, and no organism in 62% of patients. Certain signs and symptoms can be helpful in diagnosing CAP and selecting imaging studies. Diagnosis is usually made with a combination of history, physical examination, and findings on chest radiography, lung ultrasonography, or computed tomography. Procalcitonin measurement is not recommended. CRB-65 (confusion, respiratory rate, blood pressure, 65 years of age) is a well-validated risk stratification tool in the primary care setting and does not require laboratory testing. For outpatients without comorbidities, treatment with amoxicillin, doxycycline, or a macrolide is recommended (the latter only in areas where pneumococcal resistance to macrolides is less than 25%). In outpatients with comorbidities and inpatients with nonsevere pneumonia, a combination of a beta-lactam or third-generation cephalosporin plus a macrolide, or monotherapy with a respiratory fluoroquinolone is recommended. Patients should be treated for methicillin-resistant Staphylococcus aureus or Pseudomonas infection only if they present with risk factors for those pathogens. All adults 65 years or older or those 19 to 64 with underlying conditions should receive the 20-valent pneumococcal conjugate vaccine alone or the 15-valent pneumococcal conjugate vaccine followed by 23-valent pneumococcal polysaccharide vaccine one year later. The 13-valent pneumococcal conjugate vaccine is no longer recommended for routine administration. The Centers for Disease Control and Prevention recommends vaccination against influenza and SARS-CoV-2 viruses for all adults.
This article reviews the most recent evidence for the diagnosis and treatment of community-acquired pneumonia (CAP) in adults. As knowledge about COVID-19 increases, some of the figures and recommendations presented here may change in the coming years.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
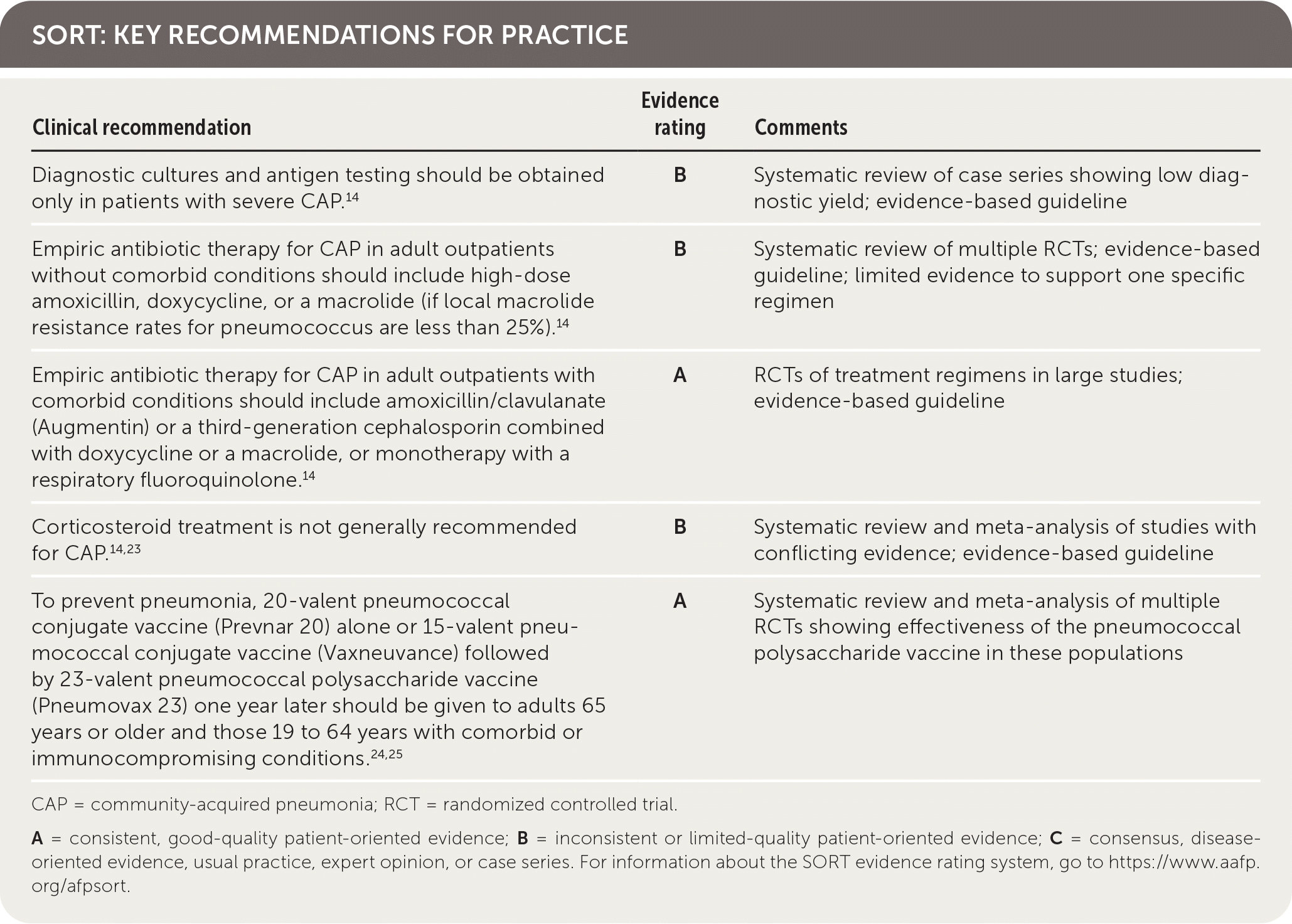
CAP = community-acquired pneumonia; RCT = randomized controlled trial.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Epidemiology
INCIDENCE
- The annual incidence of CAP is 248 cases per 100,000 adults. However, this increases to 634 cases per 100,000 in adults 65 to 79 years of age and 16,430 cases per 100,000 in adults 80 years or older.1
- Hospitalization rates for CAP increase with advancing age.1–3 A systematic review of population-based studies found that the rate was 1,830 per 100,000 adults 65 years or older and 199 per 100,000 adults younger than 65 years.2
- The hospitalization rate for CAP is nine times higher in people with comorbid chronic obstructive pulmonary disease.3
- Overall, the mortality rate for patients hospitalized with CAP is 6% at 30 days, even after initial clinical improvement. In hospitalized patients who do not improve initially or have unresolving pneumonia, the mortality rate is 34% at 30 days.4
- There are racial and ethnic disparities in the incidence of CAP. One population-based study found that the annual incidence of CAP was two to four times higher in Black adults than in White adults.5
MICROBIOLOGY
- A prospective, multicenter, population-based, active surveillance study sponsored by the Centers for Disease Control and Prevention analyzed radiograph and culture results from 2,488 inpatient adults to determine the incidence and microbiologic causes of CAP requiring hospitalization. An organism was not identified in 62% of these patients. A virus was present in 23% of patients and a bacterium in 11% of patients.1
- Another study examined the clinical and laboratory data of 323 inpatient adults with radiographically confirmed CAP and tested sputum and endotracheal aspirates to identify pathogens.6 Samples were tested for 26 bacterial and viral pathogens using culture and polymerase chain reaction analysis. A pathogen was detected in 87% of patients; 56% had bacteria alone, 25% had a combination of bacteria and viruses, and 6% had viruses alone.6 Among bacterial causes, the most common were Haemophilus influenzae (40%) and Streptococcus pneumoniae (36%). Mycoplasma and Legionella species were the most common atypical bacteria, and rhinovirus (13%) and influenza virus (7%) were the most common viral pathogens.6
- The incidence of Mycoplasma infection varies cyclically over years, and a species of Legionella is present in 3% of patients hospitalized for CAP.7
- SARS-CoV-2 infection has been a major cause of CAP during the pandemic, with data on prevalence continuing to change with emergence of disease variants and patient vaccination status; its contribution as a cause of CAP in the future is unclear.8
- False-negative results for viral pathogens are common in CAP. Samples from the lower respiratory tract have a greater diagnostic yield than nasopharyngeal or oropharyngeal samples, but obtaining lower respiratory tract samples is not usually feasible in the outpatient setting.9
Diagnosis
- The differential diagnosis of CAP includes asthma or chronic obstructive pulmonary disease exacerbation, bronchitis, congestive heart failure, gastroesophageal reflux disease, lung cancer, and pulmonary embolism.
SIGNS AND SYMPTOMS
- Patient-reported symptoms often include cough, subjective fever, chills, sputum production, and dyspnea.
- A meta-analysis found that the following clinical signs and symptoms had the highest diagnostic odds ratios for pneumonia: physician's overall clinical impression (diagnostic odds ratio = 11.5), egophony (6.5), any abnormal vital sign (6.0), any abnormal lung finding (3.2), tachypnea (3.1), and measured fever (3.3).10
- A systematic review found that adults with an acute respiratory tract infection were unlikely to have CAP if they presented with normal vital signs and normal pulmonary examination findings (negative likelihood ratio = 0.1).11
- Fever is not always present in patients with bacteremia.12
- Clinicians should determine whether patients meet criteria for severe CAP (Table 113) to inform diagnostic testing and antibiotic choice.14
TABLE 1. Criteria for Severe Community-Acquired Pneumonia

| Minor criteria* |
| Respiratory rate† ≥ 30 breaths/min |
| PaO2/FiO2 ratio† ≤ 250 |
| Multilobar infiltrates |
| Confusion/disorientation |
| Uremia (BUN level ≥ 20 mg/dL) |
| Leukopenia‡ (WBC count, < 4,000 cells/mm3) |
| Thrombocytopenia (platelet count, < 100,000 cells/mm3) |
| Hypothermia (core temperature, < 36°C) |
| Hypotension requiring aggressive fluid resuscitation |
| Major criteria |
| Invasive mechanical ventilation |
| Septic shock with need for vasopressors |
Note: Severe community-acquired pneumonia is defined as the presence of one major criterion or three or more minor criteria.
BUN = blood urea nitrogen; PaO2/FiO2 = arterial oxygen pressure/fraction of inspired oxygen; WBC = white blood cell.
*—Other criteria to consider include hypoglycemia (in nondiabetic patients), acute alcoholism/alcoholic withdrawal, hyponatremia, unexplained metabolic acidosis or elevated lactate level, cirrhosis, and asplenia.
†—A need for noninvasive ventilation can substitute for a respiratory rate > 30 breaths/min or a PaO2/FiO2 ratio < 250.
‡—As a result of infection alone.
Reprinted with permission from Mandell LA, Wunderink RG, Anzueto A. et al. Infectious Diseases Society of America/American Thoracic Society consensus guidelines on the management of community-acquired pneumonia in adults. Clin Infect Dis. 2007;44(suppl 2):S38.
DIAGNOSTIC TESTING
- The aforementioned physical examination findings with high diagnostic odds ratios for pneumonia can be helpful in determining the need for imaging.10
- Previous Infectious Diseases Society of America (IDSA) guidelines recommended chest radiography as the standard method for diagnosing CAP.13
- Updated IDSA guidelines are based on studies of patients with radiographically confirmed pneumonia despite acknowledging that chest radiography is not always used in the ambulatory setting.14
- Although chest radiography has value in the evaluation of CAP, its accuracy is limited. A study of more than 3,000 patients presenting to the emergency department found that chest radiography had a positive predictive value of only 26.9% for detection of pulmonary opacities when using computed tomography as the criterion standard, whereas the negative predictive value was 96.5%.15
- Computed tomography decreases the chance of a false-positive or false-negative diagnosis, but cost and availability make this modality less useful in the outpatient setting.16
- Procalcitonin measurement is not recommended by the IDSA and has not been found to reduce antibiotic use among patients admitted to the emergency department.17
- Diagnostic cultures and antigen testing should be obtained only in patients with severe CAP.14
- In patients with CAP who have had prior respiratory isolation of methicillin-resistant Staphylococcus aureus (MRSA) or who have had recent hospitalization and treatment with parenteral antibiotics and have locally validated risk factors for MRSA infection, microbiologic testing should be performed before escalating antibiotic treatment or to allow for future de-escalation if MRSA is not detected. Similarly, in patients with severe CAP who have had prior respiratory isolation of Pseudomonas species or who have had recent hospitalization and treatment with parenteral antibiotics and have locally validated risk factors for Pseudomonas infection, microbiologic testing should be performed before escalating antibiotic treatment or to allow for future de-escalation if a species of Pseudomonas is not detected.14
- Testing for Legionella species should be reserved for cases of severe CAP or in areas where a known outbreak of Legionella infection has occurred.14
- Microbiologic testing for influenza and SARS-CoV-2 should be considered if there is any clinical suspicion for these viruses.
- Lung ultrasonography is an alternative imaging modality if the clinician has appropriate training and equipment. A meta-analysis using computed tomography as the criterion standard showed that ultrasonography was more accurate than chest radiography at diagnosing CAP.18
Treatment
INPATIENT VS. OUTPATIENT CARE
- When determining if a patient should be treated for CAP as an inpatient or outpatient, the IDSA recommends using the Pneumonia Severity Index (https://www.mdcalc.com/psi-port-score-pneumonia-severity-index-cap) as an adjunct to clinical judgment.14 However, its use may be limited because it requires more than 20 variables, including imaging and several blood tests.
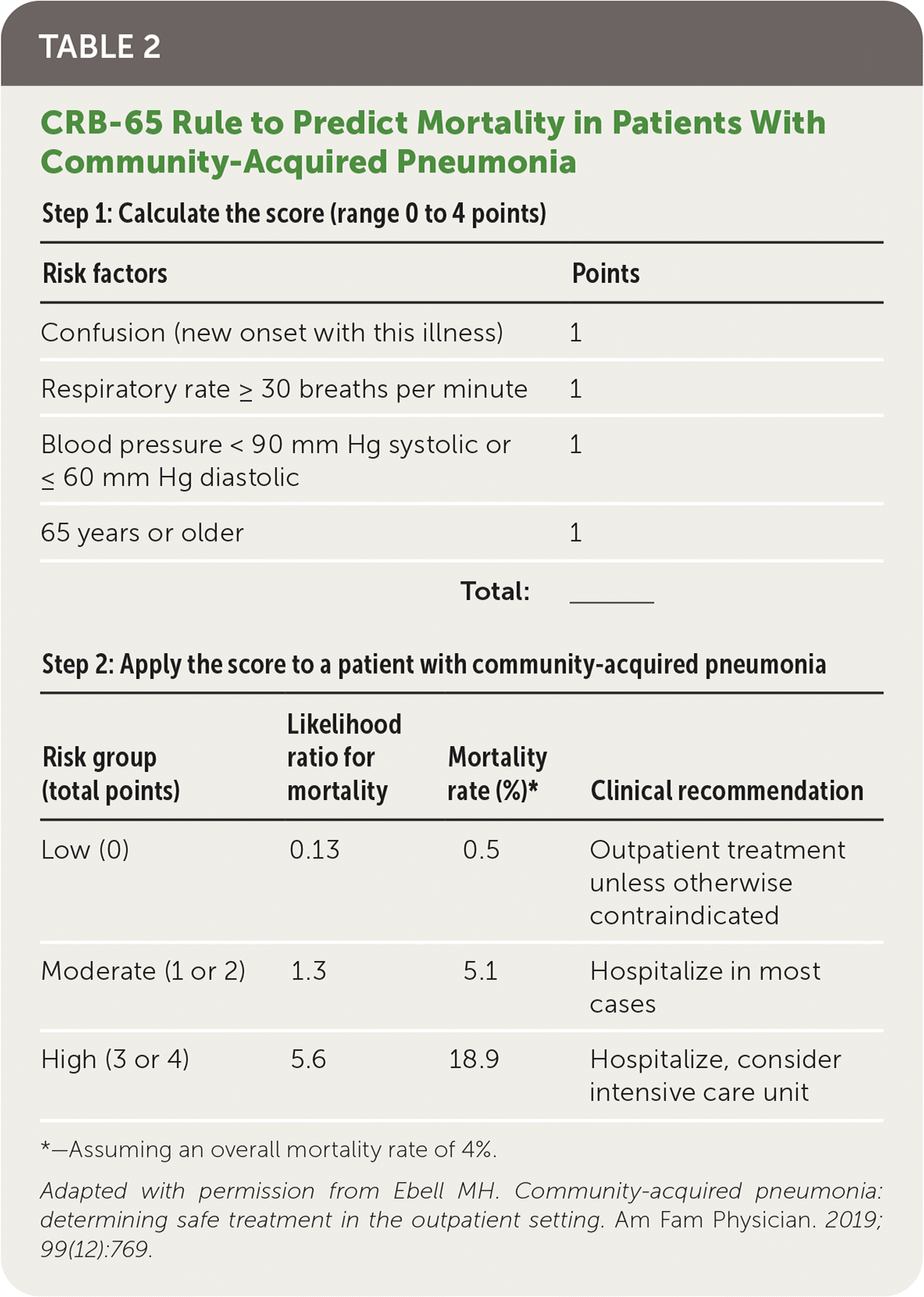
- The British Thoracic Society recommends using CURB-65 (confusion, urea nitrogen, respiratory rate, blood pressure, 65 years of age; https://www.mdcalc.com/curb-65-score-pneumonia-severity) or CRB-65 for risk stratification.19 The CRB-65 tool (Table 220) is easier to use in the outpatient setting because it requires no laboratory testing and has been well validated in primary care settings.21
TABLE 2. CRB-65 Rule to Predict Mortality in Patients With Community-Acquired Pneumonia
| Step 1: Calculate the score (range 0 to 4 points) | ||||
| Risk factors | Points | |||
| Confusion (new onset with this illness) | 1 | |||
| Respiratory rate ≥ 30 breaths per minute | 1 | |||
| Blood pressure < 90 mm Hg systolic or ≤ 60 mm Hg diastolic | 1 | |||
| 65 years or older | 1 | |||
| Total: | ________ | |||
| Step 2: Apply the score to a patient with community-acquired pneumonia | ||||
| Risk group (total points) | Likelihood ratio for mortality | Mortality rate (%)* | Clinical recommendation | |
| Low (0) | 0.13 | 0.5 | Outpatient treatment unless otherwise contraindicated | |
| Moderate (1 or 2) | 1.3 | 5.1 | Hospitalize in most cases | |
| High (3 or 4) | 5.6 | 18.9 | Hospitalize, consider intensive care unit | |
*—Assuming an overall mortality rate of 4%.
Adapted with permission from Ebell MH. Community-acquired pneumonia: determining safe treatment in the outpatient setting. Am Fam Physician. 2019; 99(12):769.
EMPIRIC ANTIBIOTIC THERAPY
- Antibiotics should be prescribed for outpatients if there is clinical suspicion for CAP without performing imaging studies, unless the diagnosis is in doubt.22
- For patients being treated in the outpatient setting, the British Thoracic Society recommends initiating antibiotics based on clinical suspicion without microbiologic testing.22
- Antibiotic therapy for outpatients is summarized in Table 3.14
- In patients with severe CAP (Table 113), combination therapy with a beta-lactam antibiotic plus a macrolide or a beta-lactam plus a respiratory fluoroquinolone is recommended.14
- In patients with severe CAP who have had prior respiratory isolation of MRSA or were recently hospitalized and treated with parenteral antibiotics and have locally validated risk factors for MRSA infection, vancomycin or linezolid (Zyvox) should be added to cover for MRSA infection.14
- In patients with severe CAP who have had prior respiratory isolation of a Pseudomonas species or who have had recent hospitalization and treatment with parenteral antibiotics and have locally validated risk factors for Pseudomonas infection, piperacillin/tazobactam (Zosyn), cefepime, ceftazidime (Fortaz), imipenem/cilastatin (Primaxin IV), meropenem (Merrem), or aztreonam (Azactam) should be added to cover for Pseudomonas infection.14
- When MRSA or Pseudomonas coverage is added, blood and sputum cultures should be obtained to allow for de-escalation of this coverage if the pathogen is ruled out.14
- Antibiotics should be continued for a minimum of five days, and discontinued after the patient improves and remains clinically stable.14
- The IDSA recommends treating adults with oseltamivir (Tamiflu) when influenza virus is isolated in the inpatient setting, regardless of the duration of illness before CAP diagnosis. In the outpatient setting, oseltamivir should be initiated regardless of duration of illness.14
- Research is ongoing to develop protocols and new drugs to treat pneumonia caused by SARS-CoV-2.
TABLE 3. Antibiotic Options for Outpatients With Community-Acquired Pneumonia

| Healthy adults without comorbid conditions Amoxicillin, 1 g three times daily Doxycycline, 100 mg twice daily Macrolide (if local resistance rates for pneumococcus are less than 25%) Azithromycin (Zithromax), 500 mg on day 1 and 250 mg on days 2 to 5 Clarithromycin, 500 mg twice daily |
| Adults with comorbid conditions (heart, lung, liver, or renal disease; diabetes mellitus; alcoholism; malignancy; asplenia) Amoxicillin/clavulanate (Augmentin), 875 mg/125 mg or 2,000 mg/125 mg twice daily, or a third-generation cephalosporin And Macrolide or doxycycline (as dosed above) OR Respiratory fluoroquinolone Levofloxacin, 750 mg once daily Moxifloxacin (Avelox), 400 mg once daily Gemifloxacin (Factive), 320 mg once daily |
Adapted with permission from Metlay JP, Waterer GW, Long AC, et al. Diagnosis and treatment of adults with community-acquired pneumonia. An official clinical practice guideline of the American Thoracic Society and Infectious Diseases Society of America. Am J Respir Crit Care Med. 2019;200(7):e48.
SYSTEMIC CORTICOSTEROIDS
- The IDSA does not recommend corticosteroids for treatment of CAP in the inpatient or outpatient setting, regardless of illness severity.14
- A systematic review and meta-analysis of corticosteroid use in adults with CAP found that short-term use may reduce the risk of acute respiratory distress syndrome in severe CAP. However, all of the studies included in the analysis had significant limitations, and overall mortality was not improved with corticosteroid use.23
- Steroids may be used in patients with CAP if they are needed to treat a comorbid condition such as asthma, chronic obstructive pulmonary disease, or autoimmune disease.
- Steroids may be used to treat CAP-related septic shock that is refractory to fluid resuscitation and vasopressor support.14
Prevention
- Updated guidelines published in January 2022 recommend vaccinating adults 65 years or older or those 19 to 64 years with underlying conditions with 20-valent pneumococcal conjugate vaccine (PCV20; Prevnar 20) alone or the 15-valent pneumococcal conjugate vaccine (PCV15; Vaxneuvance) followed by 23-valent pneumococcal polysaccharide vaccine (PPSV23; Pneumovax 23) one year later.24
- PPSV23 decreases the relative risk of CAP by 13%.25 The risk is reduced by 28% in adults 65 years or older and in younger adults with comorbid or immunocompromising conditions.25 Updated guidelines are believed to provide broader coverage and be cost-effective.
- The 13-valent pneumococcal conjugate vaccine (PCV13; Prevnar 13) is no longer recommended for routine use in immunocompetent adults 65 years or older.
- Adults previously vaccinated with both PCV13 and PPSV23 do not require PCV20 or PCV15 vaccination at this time.
- Adults vaccinated only with PPSV23 should receive a single dose of PCV15 or PCV20 one year after receiving PPSV23.
- The Centers for Disease Control and Prevention recommends that all adults be immunized against influenza and SARS-CoV-2 viruses.26
This article updates previous articles on this topic by Kaysin and Viera27; Watkins and Lemonovich28; Lutfiyya, et al.29; and Thibodeau and Viera.30
Data Sources: PubMed and OVID Medline searches were completed in Clinical Queries using the key term community-acquired pneumonia. The searches included randomized controlled trials, practice guidelines, and reviews. Essential Evidence Plus was also searched for data using the key terms acute lower respiratory tract infection, community-acquired pneumonia, and pneumonia. Search dates: March 2021 through January 2022.

