A 13-year-old girl presented with a cut on her left foot that had been worsening for two weeks. The initial small scrape was immediately treated with neomycin ointment and covered. There was minimal pain at the site, but the patient had a low-grade fever the day before presentation. She had no bowel or bladder symptoms or joint pain. Her medical history included acne, seasonal allergies, and asthma.
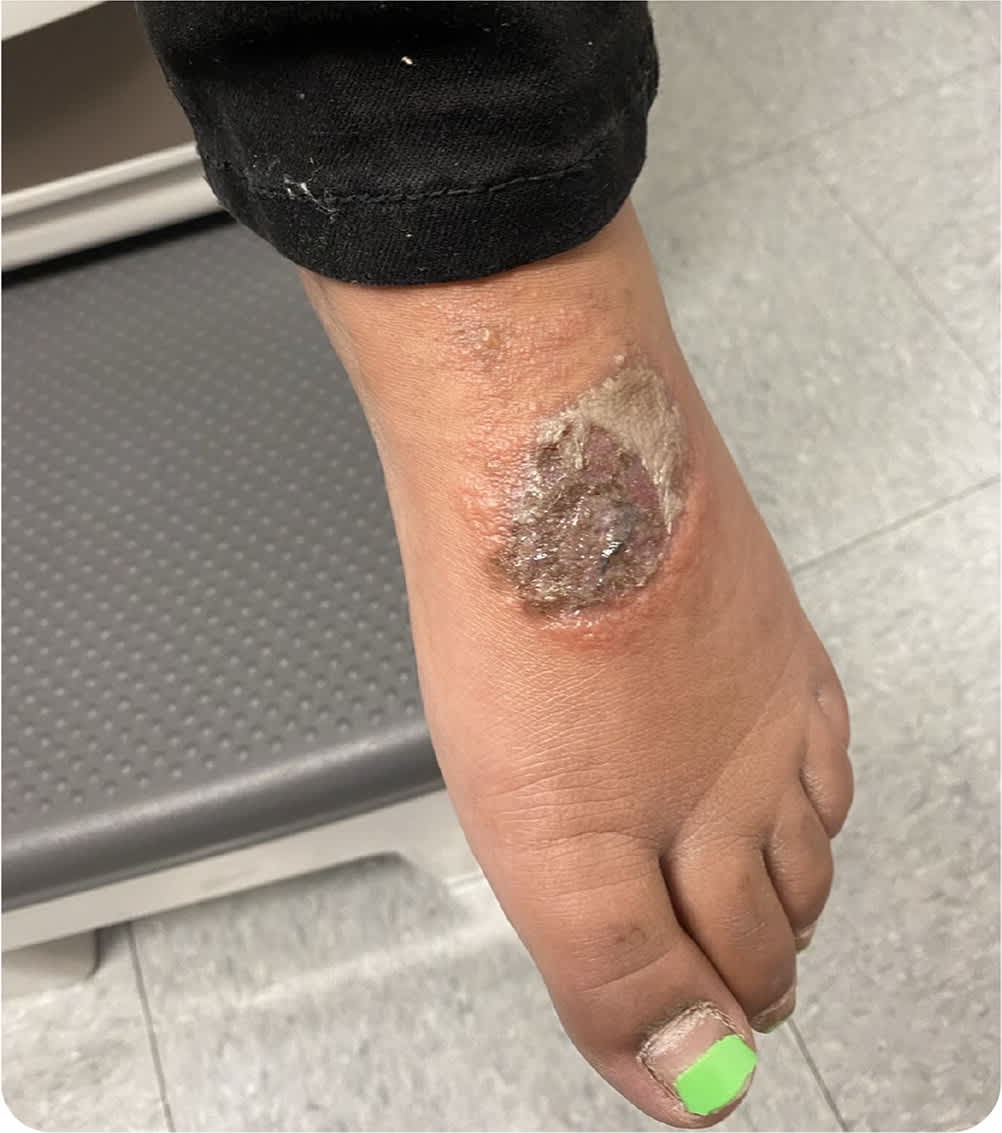
Physical examination revealed a mildly tender ulcerative lesion measuring 3 × 3 cm on the dorsal aspect of the left foot (Figure 1). The lesion had raised borders with minimal surrounding erythema and induration. It had overlying eschar but no purulent discharge. The patient was afebrile, with normal heart rate and blood pressure. Laboratory test results were normal, including complete blood count, rheumatoid factor, complete metabolic panel, antinuclear antibody, and anticyclic citrullinated antibody.
FIGURE 1
Question
Based on the patient’s history and physical examination findings, which one of the following is the most likely diagnosis?
- A. Allergic contact dermatitis.
- B. Nummular dermatitis.
- C. Pyoderma gangrenosum.
- D. Squamous cell carcinoma.
Discussion
The answer is A: allergic contact dermatitis. This form of contact dermatitis can be caused by secondary allergen transfer. Neomycin is one such allergen, and exposure can result in a type IV hypersensitivity reaction. Neomycin is used in many antibacterials, such as topical creams, eye preparations, and eardrop solutions.1 The prevalence of antibacterial hypersensitivity reactions is increasing, accounting for 4.17% of dermatitis cases.2
Type IV (delayed-type) hypersensitivity reactions involve T-cell antigen interactions, T-cell activation, and cytokine secretion. The overreaction of cytokines and T-cell activation lead to tissue damage, inflammation, and cell death. With a delayed-type hypersensitivity reaction, symptoms of allergic contact dermatitis develop one or two days after exposure. Acute allergic contact dermatitis typically starts with a rash or skin lesion at the site of exposure that is often associated with oozing, drainage, or crusting. The lesions may then become raw, scaled, or thickened, with the formation of papules, blisters, or vesicles. Chronic allergic contact dermatitis can lead to further breakdown of the skin barrier, causing atrophy.1
The patch test is the preferred diagnostic test for allergic contact dermatitis. Histopathology shows epidermal spongiosis and spongiotic vesicles. Infiltrating lymphocytes can also be seen in the epidermis, contributing to the cell-mediated delayed hypersensitivity reaction. Lack of recurrence with avoidance of the allergen can aid in clinical diagnosis.2
Treatment of allergic contact dermatitis begins with avoidance of the allergen. Topical steroids and topical tacrolimus are first-line therapy for acute localized allergic contact dermatitis. For chronic disease, intermittent use of topical corticosteroids and topical tacrolimus is standard treatment. Second-line therapies include phototherapy and systemic immunosuppressive agents such as methotrexate and cyclosporine.3
Prognosis is favorable with topical agents and avoidance of the allergen.3 This patient’s wound almost completely resolved after four weeks of treatment with triamcinolone cream.
Nummular dermatitis (nummular eczema) is characterized by multiple coin-sized, round or oval-shaped, red, pruritic plaques, most commonly on the upper and lower extremities. Lesions may have central clearing with raised edges, resembling an annular rash over time. This idiopathic condition affects men more often than women. A patch test distinguishes allergic contact dermatitis from nummular dermatitis.4
Pyoderma gangrenosum presents as an inflammatory papule or pustule that progresses to a painful, nonpruritic ulcer with an indeterminate border and purulent base. Neutrophils are important in the development of these lesions. Pyoderma gangrenosum is differentiated from allergic contact dermatitis by minimal pain and lack of pruritus.5
Squamous cell carcinoma is a malignant lesion arising from epidermal keratinocytes, usually in areas exposed to sunlight or with chronic irritation. Presentation varies, including papules, plaques, or nodules that can be smooth, hyperkeratotic, or ulcerated. It is typically not pruritic.6
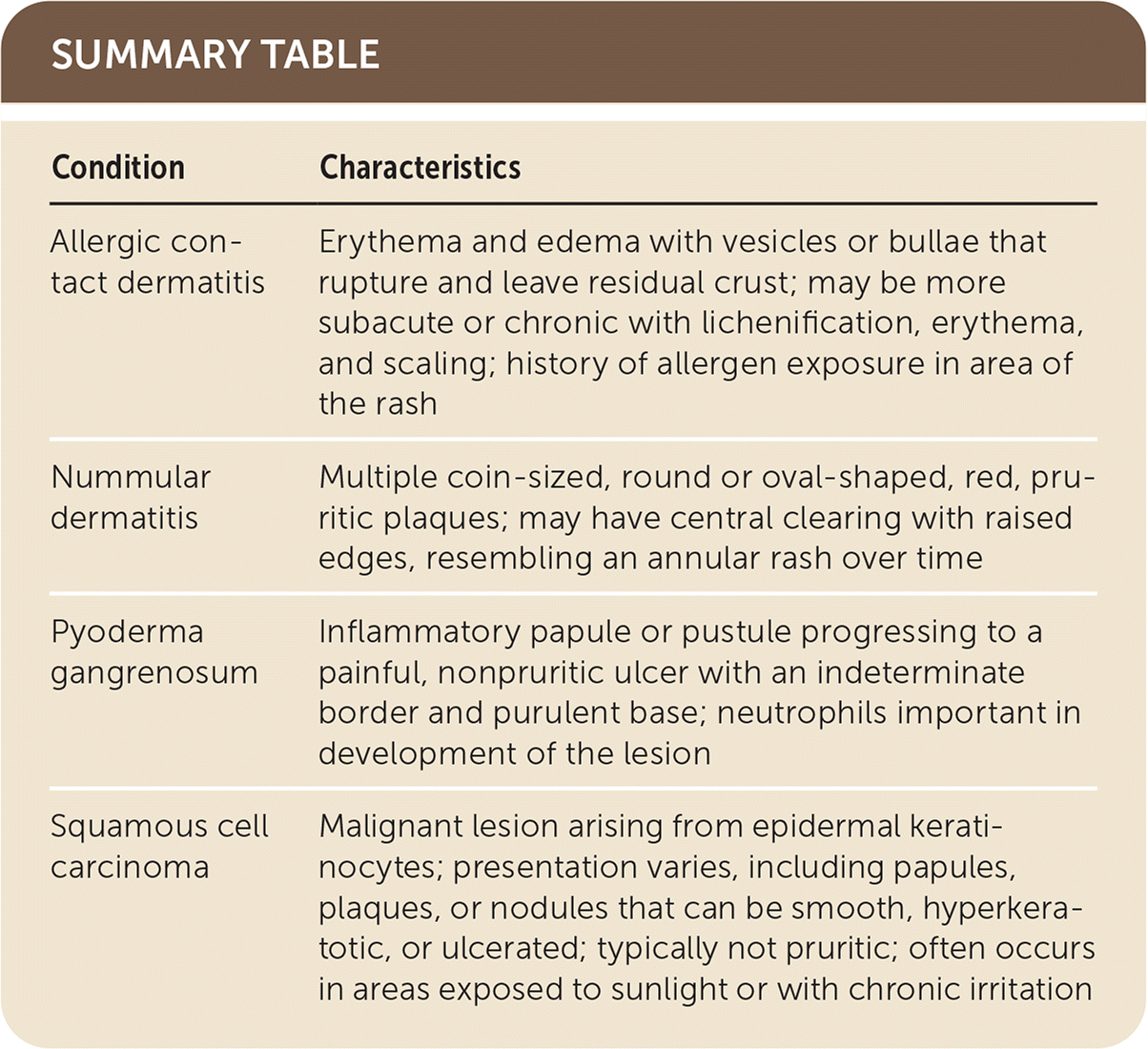
SUMMARY TABLE
| Condition | Characteristics |
|---|---|
| Allergic contact dermatitis | Erythema and edema with vesicles or bullae that rupture and leave residual crust; may be more subacute or chronic with lichenification, erythema, and scaling; history of allergen exposure in area of the rash |
| Nummular dermatitis | Multiple coin-sized, round or oval-shaped, red, pruritic plaques; may have central clearing with raised edges, resembling an annular rash over time |
| Pyoderma gangrenosum | Inflammatory papule or pustule progressing to a painful, nonpruritic ulcer with an indeterminate border and purulent base; neutrophils important in development of the lesion |
| Squamous cell carcinoma | Malignant lesion arising from epidermal keratinocytes; presentation varies, including papules, plaques, or nodules that can be smooth, hyperkeratotic, or ulcerated; typically not pruritic; often occurs in areas exposed to sunlight or with chronic irritation |

