Am Fam Physician. 2023;107(1):90-91
Related AFP Community Blog Post: Semaglutide Shortage Highlights Inequities in Diabetic Medication Access
Author disclosure: No relevant financial relationships.
Semaglutide (Wegovy) is a glucagon-like peptide-1 (GLP-1) receptor agonist. It is labeled for use as an adjunct to diet and exercise for chronic weight management in adults classified as obese (body mass index [BMI] of 30 kg per m2 or greater) or overweight (BMI of 27 kg per m2 or greater) in the presence of one weight-related comorbidity. Semaglutide is also available in a lower-dose injectable formulation (Ozempic) and an oral formulation (Rybelsus) for the treatment of type 2 diabetes mellitus.1
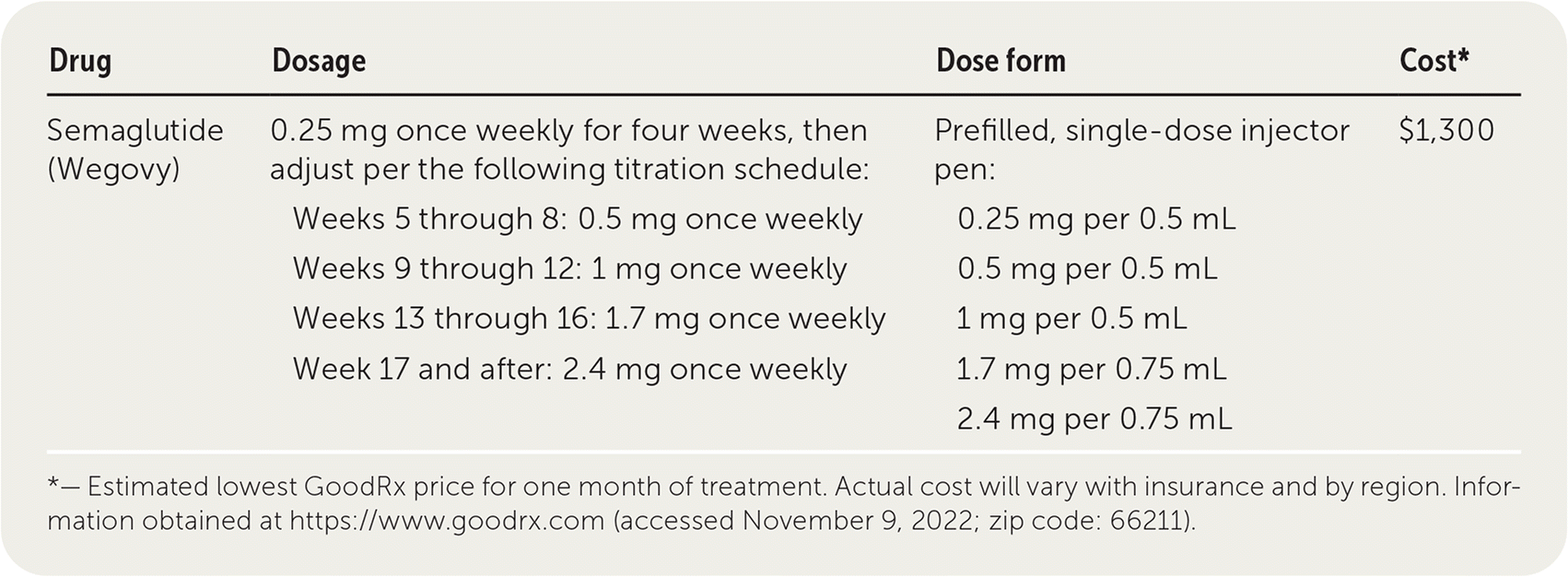
| Drug | Dosage | Dose form | Cost* |
|---|---|---|---|
| Semaglutide (Wegovy) | 0.25 mg once weekly for four weeks, then adjust per the following titration schedule: Weeks 5 through 8: 0.5 mg once weekly Weeks 9 through 12: 1 mg once weekly Weeks 13 through 16: 1.7 mg once weekly Week 17 and after: 2.4 mg once weekly | Prefilled, single-dose injector pen: 0.25 mg per 0.5 mL 0.5 mg per 0.5 mL 1 mg per 0.5 mL 1.7 mg per 0.75 mL 2.4 mg per 0.75 mL | $1,300 |
Subscribe
From $165- Immediate, unlimited access to all AFP content
- More than 130 CME credits/year
- AAFP app access
- Print delivery available
Issue Access
$59.95- Immediate, unlimited access to this issue's content
- CME credits
- AAFP app access
- Print delivery available