Case Scenario
A.F., a 71-year-old with a history of non–insulin-dependent type 2 diabetes mellitus, presents as a new patient to my family medicine clinic. A.F.’s most recent A1C level is 8.0, and they take metformin, 500 mg twice daily, and atorvastatin, 40 mg daily. A.F. reports that they check their blood glucose one to three times daily using a home glucose monitor, as recommended by their previous physician. I recommend discontinuing self-monitoring of their blood glucose because its effectiveness in achieving glycemic control is limited in patients who are not taking insulin. A.F. becomes upset by my suggestion, wondering how they can keep their diabetes under control without checking their glucose levels at home. How do I respond to my new patient?
Commentary
This case addresses a common situation in primary care that can occur when new evidence changes practices that were once taken for granted by physicians and patients as contributing to quality care. Discontinuing low-value interventions can be challenging for patients and physicians.
Until recently, self-monitoring of blood glucose was a routine recommendation for all patients with diabetes, including those not taking insulin. Among patients who do not use insulin, a growing body of evidence validates that self-monitoring of blood glucose is not effective in achieving long-term glycemic control. A 2012 Cochrane review, which compiled data from 12 randomized controlled trials, showed that patients with non–insulin-dependent diabetes who self-monitored their blood glucose levels did not have clinically significant improvements in glycemic control after one year.1 More recently, a 2017 study assigned patients with non–insulin-dependent diabetes to one of three groups: no self-monitoring, once-daily self-monitoring, and once-daily self-monitoring with enhanced patient feedback, including automatic messages about the results delivered via the glucose meter. This trial found no notable differences in A1C levels across all groups at one year and no differences in health-related quality of life.2
Routine self-monitoring of blood glucose also has potential harms. Although the exact costs are difficult to quantify, one 2012 study estimated that self-monitoring costs more than $700 annually per patient.3 In addition to cost, patients may find using a lancet painful,4 and studies indicate that stress, worry, distress, and depressive symptoms may increase with the frequency of self-monitoring.5
As a result, multiple professional societies have recommended against prescribing self-monitoring for patients with non–insulin-dependent type 2 diabetes. As part of the Choosing Wisely campaign, the American Academy of Family Physicians and the Society of General Internal Medicine have recommended against physicians prescribing self-monitoring for these patients.6,7
Nevertheless, routine self-monitoring of blood glucose in patients with non–insulin-dependent diabetes persists. The current prevalence of the practice is difficult to estimate, but in a 2012 study, approximately 75% of patients with non–insulin-dependent diabetes reported self-monitoring at least once daily.8
Barriers to Evidence-based Care
Why does this low-value practice continue? In this case scenario, both physician and patient factors influenced the situation, including a previous physician’s recommendation to self-monitor and the patient’s concerns that discontinuing the practice could cause harm.
Multiple barriers may prevent physicians from finding, interpreting, and implementing the most updated evidence-based practices.9 Although physicians have widespread online access to clinical practice guidelines, including the Choosing Wisely campaign, research demonstrates that some physicians are skeptical of clinical guidelines. One systematic review of physicians’ attitudes toward clinical practice guidelines showed that only 75% of physicians believe them to be helpful and up to 30% of physicians consider guidelines to be impractical and too rigid to apply to individual patients.10
Concerns about adapting guidelines to individual patients may explain much of the continued self-monitoring in those with non–insulin-dependent diabetes. For example, in a 2018 qualitative study based on structured interviews with 17 physicians, participants emphasized the role of self-monitoring of blood glucose in supporting patient commitment to the lifestyle changes needed for improved diabetes outcomes.11
Patients may also perceive that they derive benefit from self-monitoring and fear losing control over their condition. These concerns may explain patient resistance to physician recommendations to discontinue the practice and, perhaps, to change in general. Patients may become distressed and find it difficult to accept advice to discontinue self-monitoring because they have been told for many years that it is integral to diabetes control.
A study published in 2022 evaluated the responses from 458 patients with non–insulin-dependent diabetes about their perceptions of self-monitoring of blood glucose. Several themes emerged from the study that may help explain why some patients derive a sense of benefit from the practice.12 More than 90% of respondents stated that their physicians instructed them to self-monitor, and although one-half of those patients said that they would be willing to stop the practice if instructed to do so by their physicians, those who wished to continue cited increased quality of life, better sense of control, and decreased worry about their health.
Steps for Deprescribing Self-Monitoring
As in other situations in which physicians must de-escalate care, deprescribing self-monitoring of blood glucose requires eliciting patient goals and preferences, and, when possible, integrating those preferences with best practices based on the harms and benefits of self-monitoring.
The first step is identifying patients who may be good candidates for discontinuing self-monitoring, including those who have glycemic control at or close to the desired A1C goal using only oral agents and who are unlikely to require insulin soon. It must be determined whether the patient’s goals of treatment are aligned with a deprescribing approach. Physicians may find it helpful to categorize recommendations based on the patient’s preferences and assess whether the patient is “attached to treatment,” is interested in deintensifying care, or would rather defer their medical decisions to others. Counseling techniques tailored to each type may aid in discussions around de-escalation of self-monitoring.13
If a patient agrees to de-escalation of care, the physician should next initiate a discussion on deprescribing self-monitoring of blood glucose. This may be challenging and could require multiple visits. Tools for shared decision-making may be useful in these discussions, including examining shared review of patient data, involving the patient’s family members and other important stakeholders, and providing educational materials for review outside the clinical setting.
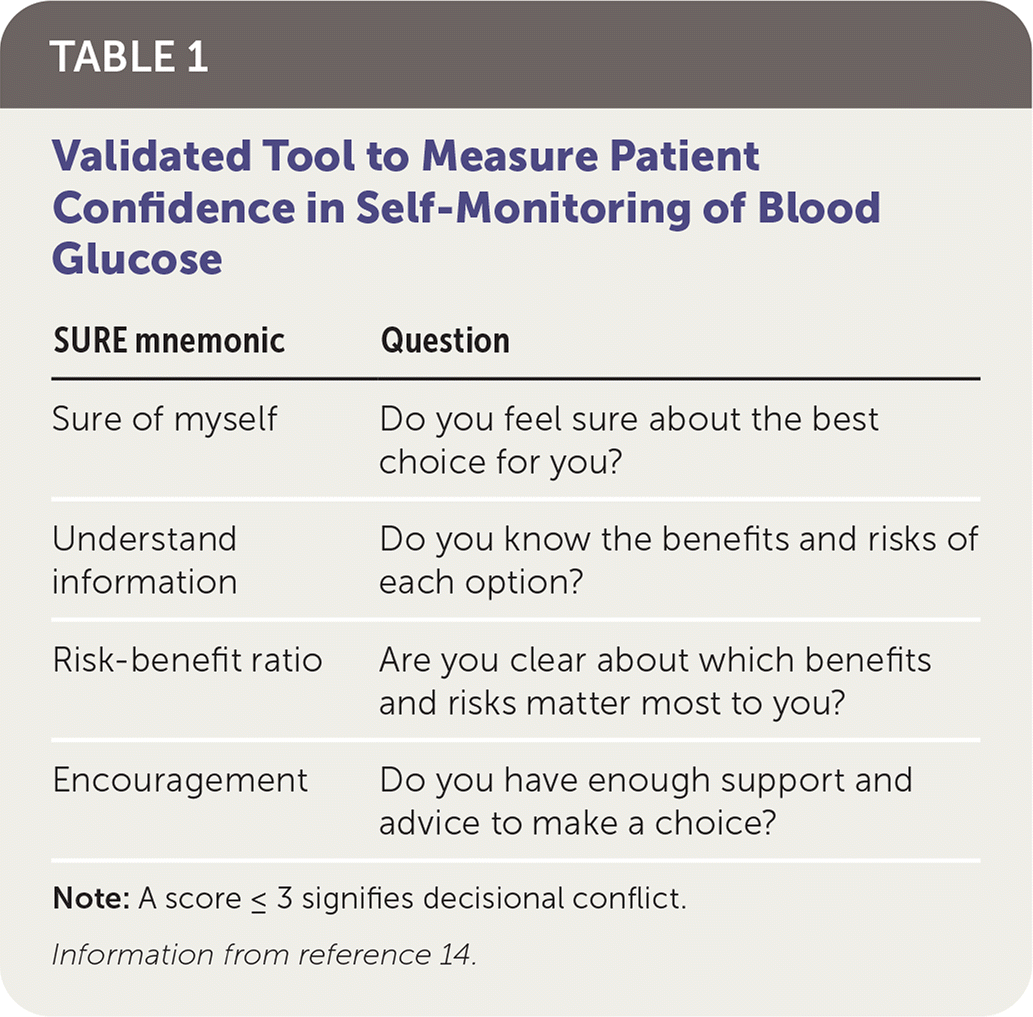
Physicians may also find helpful a validated tool to test patient confidence in their decision, such as the SURE questionnaire (Table 114 ), when developing individualized strategies. The SURE questionnaire can facilitate structured counseling to ensure that patients understand the risks and benefits of self-monitoring while keeping the physician on track to fully engage with patients’ concerns.14 Physicians should expect that patients’ decisions about de-escalation of their self-monitoring of blood glucose will change over time; decisions about their diabetes management goals and preferences will also change, especially because of the ever-evolving landscape of diabetes care. Physicians should follow up periodically to revisit this conversation.
TABLE 1. Validated Tool to Measure Patient Confidence in Self-Monitoring of Blood Glucose
| SURE mnemonic | Question |
|---|---|
| Sure of myself | Do you feel sure about the best choice for you? |
| Understand information | Do you know the benefits and risks of each option? |
| Risk-benefit ratio | Are you clear about which benefits and risks matter most to you? |
| Encouragement | Do you have enough support and advice to make a choice? |
Note: A score ≤ 3 signifies decisional conflict.
Information from reference 14.
Case Resolution
The patient is expressing discomfort with the new physician’s proposed change in their diabetes management. The physician in this scenario, who is seeing A.F. for the first time, should begin by acknowledging their commitment to patient care, as well as eliciting A.F.’s concerns and fears, involving their family and caretakers as appropriate. The physician should explain concepts with which A.F. may not be familiar, while providing a rationale for de-escalating self-monitoring of blood glucose given the most recent evidence and practice guidelines. Nonetheless, some patients will naturally require more time than others to decide about de-escalation of self-monitoring, and the physician should expect to follow up and continue the conversation at future visits as needed.

