To the Editor: Scalp dermatitis with scaling can be challenging to diagnose in children. Tinea capitis, the most common cause of hair loss among children, should be excluded.
A 10-year-old patient presented with a seven-year history of scalp scaling, beginning with a quarter-sized, well-demarcated scaly plaque of hair loss, previously diagnosed as seborrheic dermatitis and treated with topical antifungals and corticosteroids. Two months earlier, the patient developed fluctuance, purulent drainage, and alopecia.
The patient had an erythematous, boggy patch of alopecia involving more than 50% of the scalp and clinically consistent with a kerion (Figure 1), an inflammatory subtype characterized by tender, erythematous, boggy plaques with thick crusting, often with pustules and purulent drainage.1,2 The patient had no cervical lymphadenopathy. A potassium hydroxide scraping test and Wood lamp examination were negative. A punch biopsy found hyphae and spores within the hair shaft. The fungal culture grew Trichophyton tonsurans. The patient was treated with griseofulvin, 20 to 25 mg per kg per day, and ketoconazole 2% shampoo applied to the scalp for five minutes, rinsed daily for two weeks, and then rinsed twice a week for six weeks. The kerion resolved after eight weeks, leaving patchy alopecia with permanent scarring. Tinea capitis can mimic seborrheic dermatitis, atopic dermatitis, contact dermatitis, scalp psoriasis, sebopsoriasis, and discoid lupus. It can develop into a kerion.1,2 It is caused by advanced disease and an exaggerated immune response, predominantly found in children five to 10 years of age.3 More than 20 misdiagnosed cases have been reported, usually as bacterial abscesses or dissecting cellulitis.4 Delayed treatment increases risk of permanent hair loss.
FIGURE 1.
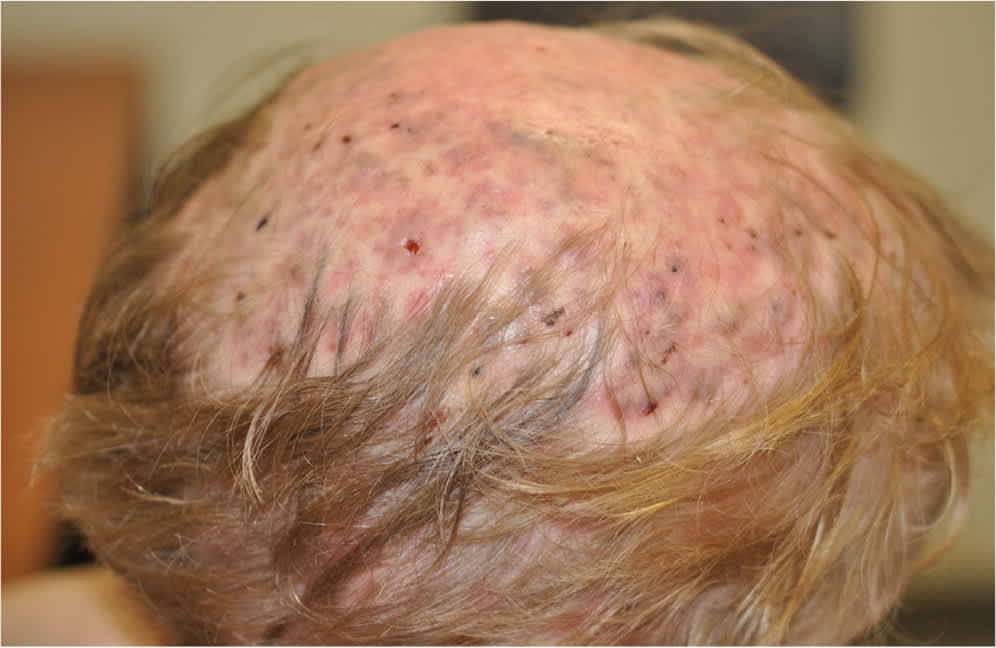
Tender, erythematous, boggy plaque with scattered purulent drainage on the scalp.
Tinea capitis should be treated with systemic antifungals because topical medications inadequately penetrate the hair follicle.2 Oral griseofulvin is the first-line treatment.5 A systematic review found that griseofulvin was more effective for Microsporum species, whereas terbinafine (Lamisil) was equally or slightly more effective for Trichophyton dermatophytes.1,5 Some clinicians treat kerion with prednisone, although combination treatment may not be superior to antifungals alone.6 Antibiotics are unnecessary unless a secondary bacterial infection is identified.6
Topical antifungal shampoos as an adjunctive scalp treatment can decrease infectivity and be used in family members to decrease risk of reinfection from asymptomatic carriers. Ketoconazole 2% shampoo should be applied to the scalp for five to 10 minutes, two to three times per week for at least two weeks or until the infection has cleared. Fomites should be disinfected or discarded because dermatophytes can stay viable for prolonged periods.1
The authors thank Dr. Wendi E. Wohltmann for her expertise as the dermatopathologist for this case and article review.
The views expressed are those of the authors and do not reflect the official views or policy of the U.S. Department of Defense or its components.

