A 63-year-old man presented to his family physician for a follow-up visit. He was wearing a mask, and at the end of the appointment, he asked the physician to assess a lesion on his lip. The lesion had progressively worsened over six months, during mandated use of masks. The lesion was painful with intermittent bleeding. The patient did not use chewing tobacco but was a daily smoker. He had a history of fever blisters and significant sun exposure as a child. He did not have weight loss, other skin lesions, or family history of skin conditions.
Physical examination revealed an ulcerated, crusted, erythematous plaque with well-demarcated borders on his lower lip (Figure 1). Biopsy was performed to further characterize the lesion.
FIGURE 1
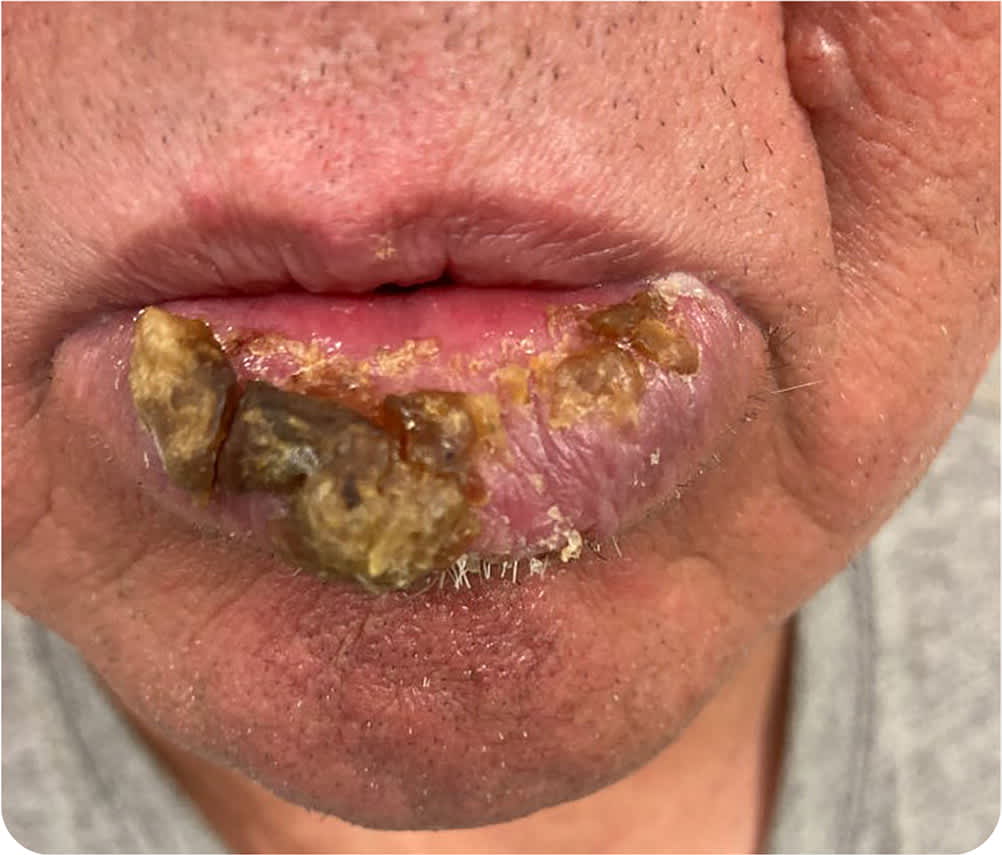
Question
Based on the patient’s history and physical examination findings, which one of the following is the most likely diagnosis?
- A. Actinic cheilitis with squamous cell carcinoma in situ.
- B. Basal cell carcinoma.
- C. Keratoacanthoma.
- D. Lichen planus.
- E. Squamous cell carcinoma.
Discussion
The answer is A: actinic cheilitis with squamous cell carcinoma in situ. Actinic cheilitis (solar cheilitis) is a premalignant condition of the lip caused by chronic exposure to ultraviolet (UV) radiation. It most often occurs on the lower lips of individuals with light skin tones. Prevalence is 10% to 40% in those with occupational exposure to UV radiation, such as fishermen and farmers.1 Risk factors for actinic cheilitis include working outdoors for more than 25 years, age 60 years or older, light skin types, and personal history of nonmelanoma skin cancer.1 Actinic cheilitis may occur at a younger age in patients with genetic conditions that increase susceptibility to sun damage such as xeroderma pigmentosum and oculocutaneous albinism. More advanced actinic cheilitis lesions may have atrophic changes, blurred demarcation of the vermilion border, erythema, edema, hyperkeratotic plaques, ulceration, and crusting.1 Actinic cheilitis has a similar pathogenesis to actinic keratosis but has a higher risk of progression to squamous cell carcinoma.
Lip biopsy is not routinely performed in patients with a history of chronic sun exposure and early changes of actinic cheilitis (e.g., persistent dryness and scaling of the lip with a characteristic sandpaper feel, mild atrophy). Biopsy is warranted in patients presenting with hyperkeratotic or nodular areas with or without erosions or ulceration because these may suggest squamous cell carcinoma.1 Treatment of actinic cheilitis may include fluorouracil, cryotherapy, curettage, or dermabrasion.2
Squamous cell carcinoma in situ presents as an erythematous patch or plaque with hyperkeratosis and occasionally nodules or ulcerations.2,3 Histologically, squamous cell carcinoma in situ has atypical keratocytes that are limited to the epidermis and do not invade the dermis or beyond. Thin and small lesions are treated with fluorouracil, liquid nitrogen, or imiquimod.2
Basal cell carcinoma is caused by chronic UV radiation exposure. Lesions arise from the basal layer of the epidermis and are characterized by basophilic basal cells infiltrating the underlining dermis.4 Basal cell carcinoma presents as an ulcerated, nodular mass, with telangiectatic vessels visible on the sides of the crater.4 Lesions appear on the head and neck in 85% of cases and on the nose in 25% to 30% of cases.2
Keratoacanthoma occurs in sun-exposed areas and has a male predominance. It can grow rapidly within four to six weeks as a crateriform tumor with a central keratin plug. It may regress spontaneously with scarring within six months.4
Lichen planus on the lip typically presents as white lines in a reticular pattern (Wickham striae) and is associated with lesions on the buccal mucosa. On histologic examination, there is damage to the basal keratinocytes and a bandlike lymphocytic infiltrate in the upper dermis.1 Women are more commonly affected than men, and there is a slight risk of these lesions evolving into squamous cell carcinoma.4
Squamous cell carcinoma is an invasive malignancy arising from keratinocytes that may develop de novo or from precursor actinic keratosis or squamous cell carcinoma in situ.3 Invasive squamous cell carcinoma typically shows dysplastic keratinocytes involving the full thickness of the epidermis and dermal invasion, differentiating it from in situ.1 Physical examination may show scaly to nodular lesions with ulceration, often on the ears, lower lips, or dorsum of the hands.4
SUMMARY TABLE
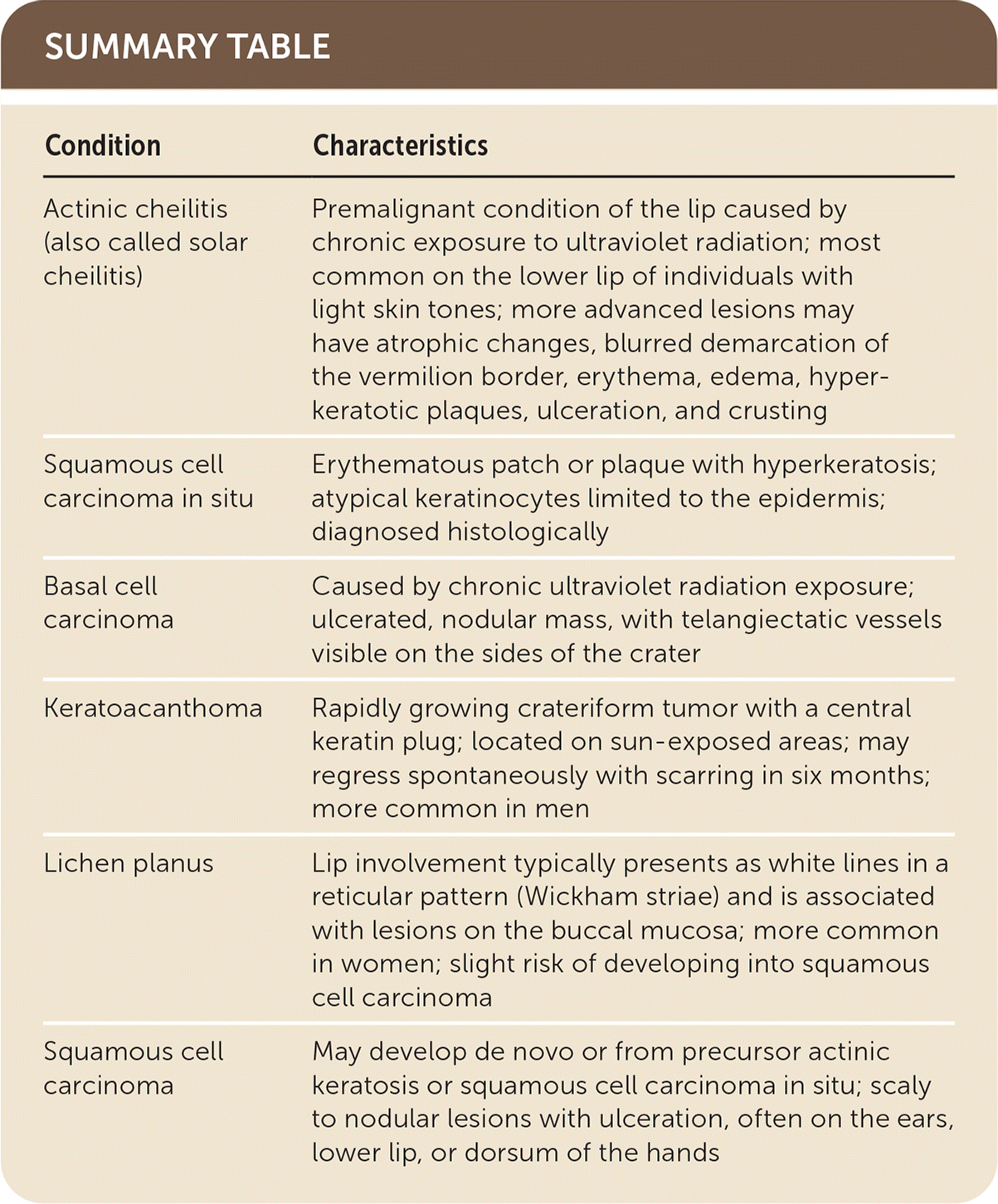
| Condition | Characteristics |
|---|---|
| Actinic cheilitis (also called solar cheilitis) | Premalignant condition of the lip caused by chronic exposure to ultraviolet radiation; most common on the lower lip of individuals with light skin tones; more advanced lesions may have atrophic changes, blurred demarcation of the vermilion border, erythema, edema, hyperkeratotic plaques, ulceration, and crusting |
| Squamous cell carcinoma in situ | Erythematous patch or plaque with hyperkeratosis; atypical keratinocytes limited to the epidermis; diagnosed histologically |
| Basal cell carcinoma | Caused by chronic ultraviolet radiation exposure; ulcerated, nodular mass, with telangiectatic vessels visible on the sides of the crater |
| Keratoacanthoma | Rapidly growing crateriform tumor with a central keratin plug; located on sun-exposed areas; may regress spontaneously with scarring in six months; more common in men |
| Lichen planus | Lip involvement typically presents as white lines in a reticular pattern (Wickham striae) and is associated with lesions on the buccal mucosa; more common in women; slight risk of developing into squamous cell carcinoma |
| Squamous cell carcinoma | May develop de novo or from precursor actinic keratosis or squamous cell carcinoma in situ; scaly to nodular lesions with ulceration, often on the ears, lower lip, or dorsum of the hands |

