Key Points for Practice
• In uncomplicated major depression, combining medications and psychotherapy is not more effective than monotherapy.
• For severe, persistent, or recurrent major depression, combining medications and psychotherapy is more effective than monotherapy.
• Continuing medications for at least six months after symptom remission will reduce relapse by nearly one-third.
• When patients with symptom remission are at high risk of relapse, cognitive behavior therapy, interpersonal therapy, or mindfulness-based cognitive therapy can reduce relapse risk.
From the AFP Editors
One in five people in the United States is diagnosed with major depression during their lifetime, and one in 10 copes with depression in any given year. Women have twice the risk of depression as men. Risk is higher in younger adults, people with lower incomes, and White and Native American ethnicities. The U.S. Department of Veterans Affairs and U.S. Department of Defense (VA/DoD) published guidelines on the management of major depressive disorder.
Screening for Depression
The U.S. Preventive Services Task Force recommends screening all patients for depression. The two-question Patient Health Questionnaire (PHQ-2) can be used, and if positive the longer PHQ-9 can be used for follow-up. These questionnaires are recommended for older adults because of similar sensitivity to geriatric-specific screening tools. Although the Edinburgh Postnatal Depression Scale is commonly used for pregnant and postpartum patients, the PHQ-2 is also effective for this population.
Diagnosis
Although screening tools can suggest major depression, diagnosis requires five or more symptoms from the Diagnostic and Statistical Manual of Mental Disorders, 5th ed. to present within the same two-week period, with one being either depressed mood or loss of interest or pleasure in almost all activities. Symptoms must cause significant distress or functional impairment. Substance misuse or a medical condition that could cause similar symptoms should be ruled out. The diagnostic evaluation is an opportunity to ask about treatment history and suicide attempts as well as current suicidal or homicidal ideation.
Treatment Setting
Collaborative care models, which include multiprofessional care, structured management, scheduled follow-up, and interprofessional communication, improve patient symptoms and satisfaction over usual care. Psychiatrist availability to recommend treatment further improves outcomes. Although collaborative care is effective in primary care settings, team-based care does not improve outcomes in specialty environments.
Interventions delivered by telehealth appear to be as effective as in-person treatment. Limited study shows similar improvements in depressive symptoms and quality of life.
Treatment of Uncomplicated Major Depression
People diagnosed with uncomplicated major depression (i.e., PHQ-9 score of 20 or less) are most often best treated with either psychotherapy or pharmacotherapy alone, although other treatments may be effective as well. Combining therapy and medication is not helpful unless depression is severe, persistent, or recurrent.
Psychotherapy
Several types of psychotherapy are effective for depression (Table 1), and all appear to have similar effectiveness. Group and individual psychotherapy improves depressive symptoms compared with the waiting list or usual care options and appear similarly effective. Guided internet-based cognitive behavior therapy appears to be beneficial for mild to moderate depression based on low-quality evidence. If patients decline medications and psychotherapy, another option is nondirective supportive therapy, which slightly improves depressive symptoms based on low-quality evidence.
TABLE 1. Effective Psychotherapy Options in Major Depression
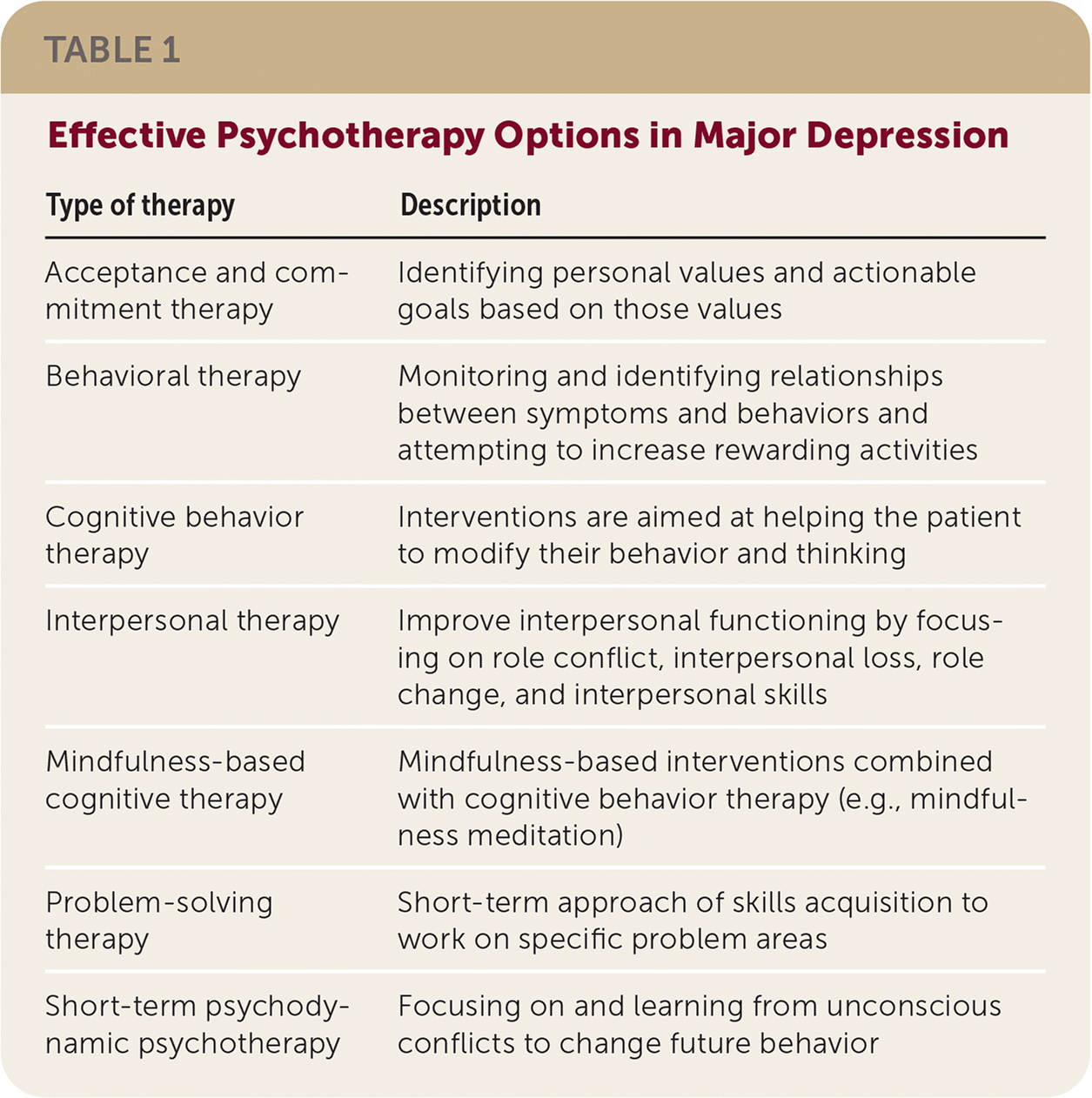
| Type of therapy | Description |
|---|---|
| Acceptance and commitment therapy | Identifying personal values and actionable goals based on those values |
| Behavioral therapy | Monitoring and identifying relationships between symptoms and behaviors and attempting to increase rewarding activities |
| Cognitive behavior therapy | Interventions are aimed at helping the patient to modify their behavior and thinking |
| Interpersonal therapy | Improve interpersonal functioning by focusing on role conflict, interpersonal loss, role change, and interpersonal skills |
| Mindfulness-based cognitive therapy | Mindfulness-based interventions combined with cognitive behavior therapy (e.g., mindfulness meditation) |
| Problem-solving therapy | Short-term approach of skills acquisition to work on specific problem areas |
| Short-term psychodynamic psychotherapy | Focusing on and learning from unconscious conflicts to change future behavior |
Medications
When choosing a medication, bupropion, mirtazapine, serotonin-norepinephrine reuptake inhibitors, selective serotonin reuptake inhibitors, and trazodone are similarly effective. Monoamine oxidase inhibitors, nefazodone, and tricyclic antidepressants are effective, but their low therapeutic indices and significant risk of toxicity limit use. Evidence for ketamine and esketamine (Spravato) is limited to patients with persistent depression.
Use of pharmacogenetic testing to guide medication choice does not appear to improve treatment outcomes.
For patients with uncomplicated major depression who are not pregnant or breastfeeding and prefer herbal therapy, St. John’s wort, which reduces symptoms more than placebo and is comparable to antidepressant medications, is an option. Adverse effects are less common than with standard antidepressants and include gastrointestinal upset, mild sedation, restlessness, photosensitivity, and serotonin syndrome. As a cytochrome P450 3A4 enzyme inducer, St. John’s wort can reduce the effectiveness of some medications, including oral contraceptives. Dosing is three times daily, starting at 300 mg per dose. Because St. John’s wort is an herbal medication, dosing may not be consistent among formulations.
Other Treatments
All patients with uncomplicated major depression may benefit from adjunctive therapies, including exercise, bibliotherapy, and light therapy. Exercise improves symptoms in major depression compared with the waiting list or usual care options, although evidence is very low quality. Bibliotherapy, or reading literature as psychological support, is more effective than usual care. Light therapy improves symptoms whether they follow a seasonal pattern or not. Biofeedback and meditation may have slight benefit as adjunctive therapies, although evidence is very low quality.
In patients with uncomplicated major depression and relationship distress, couples-focused therapy is as effective as other therapies for reducing depressive symptoms.
Acupuncture slightly reduces symptoms compared with sham therapy. Vagus nerve stimulation and deep brain stimulation have no demonstrated benefit and significant harms. Similarly, 3,4-methylenedioxymethamphetamine (MDMA), psilocybin, and cannabis lack evidence of benefit for major depression. Vitamin D and omega fatty acids do not improve depressive symptoms.
Severe, Persistent, or Recurrent Depression
For patients with severe depression (i.e., PHQ-9 score greater than 20), major depression that persists for more than two years, or depression with at least one recurrence, combining psychotherapy and medications improves outcomes over monotherapy. Based on a single study, combining cognitive behavior therapy and medications in persistent depression increases remission of symptoms at 12 weeks with a number needed to treat of 3 (95% CI, 2 to 9).
Patients with severe major depression and incomplete response after six to 12 weeks of pharmacotherapy can add psychotherapy to medications or start a second-generation antipsychotic medication. Augmentation with psychotherapy such as cognitive behavior therapy improves depressive symptoms and increases rates of remission without increasing adverse effects. Although adding a second-generation antipsychotic medication increases remission, patients often experience adverse effects including akathisia, sedation, and weight gain.
Medication management in persistent depression can be challenging. Increasing medication doses may not improve symptoms, although adverse effects and discontinuation rates may increase. Switching patients with incomplete response to a different antidepressant does not improve symptom remission over continuing the same medication. Augmenting medical treatment with mirtazapine does not improve symptoms over placebo.
Individuals with multiple failed attempts at using pharmacotherapy may benefit from ketamine, esketamine, or transcranial magnetic stimulation. Ketamine and esketamine reduce depressive symptoms and increase remission when used as augmentation, although most trials have a high risk of bias. Transcranial magnetic stimulation may be highly effective because a systematic review of small studies shows a number needed to treat between 5 and 7 for remission compared with sham therapy. Theta burst transcranial magnetic stimulation is not better than sham therapy at 24 weeks.
Electroconvulsive therapy continues to have a role in severe major depression with catatonia, psychosis, severe suicidality, a need for a rapid response, or a history of poor response to previous treatment. Electroconvulsive therapy is more effective than sham therapy and pharmacotherapy, although this is based on very low-quality evidence from small trials. Benefits are short term, and maintenance therapy is required. The major adverse event is reduced short-term cognitive function.
Remission
Individuals who attain remission with pharmacotherapy benefit from continuing treatment for at least six months to decrease the risk of relapse. Six months of additional medical therapy reduces the relapse rate from 41% to 12%.
Patients with unstable remission or two or more episodes of major depression have a high risk of relapse. For these patients, a regimen of cognitive behavior therapy, interpersonal therapy, or mindfulness-based cognitive therapy during remission can reduce the risk of relapse.
Depression in Specific Populations
For people who are breastfeeding or pregnant, psychotherapy is recommended based on similar effectiveness and a lower risk profile than medications. For patients who become pregnant while taking effective medication, shared decision-making is required because evidence is lacking.
Although adults 65 years and older benefit equally from pharmacotherapy and psychotherapies, an initial trial of psychotherapy is preferred to avoid risks from polypharmacy. Bibliotherapy is effective as an adjunct for major depression in older adults.
G-TRUST GUIDELINE SCORECARD
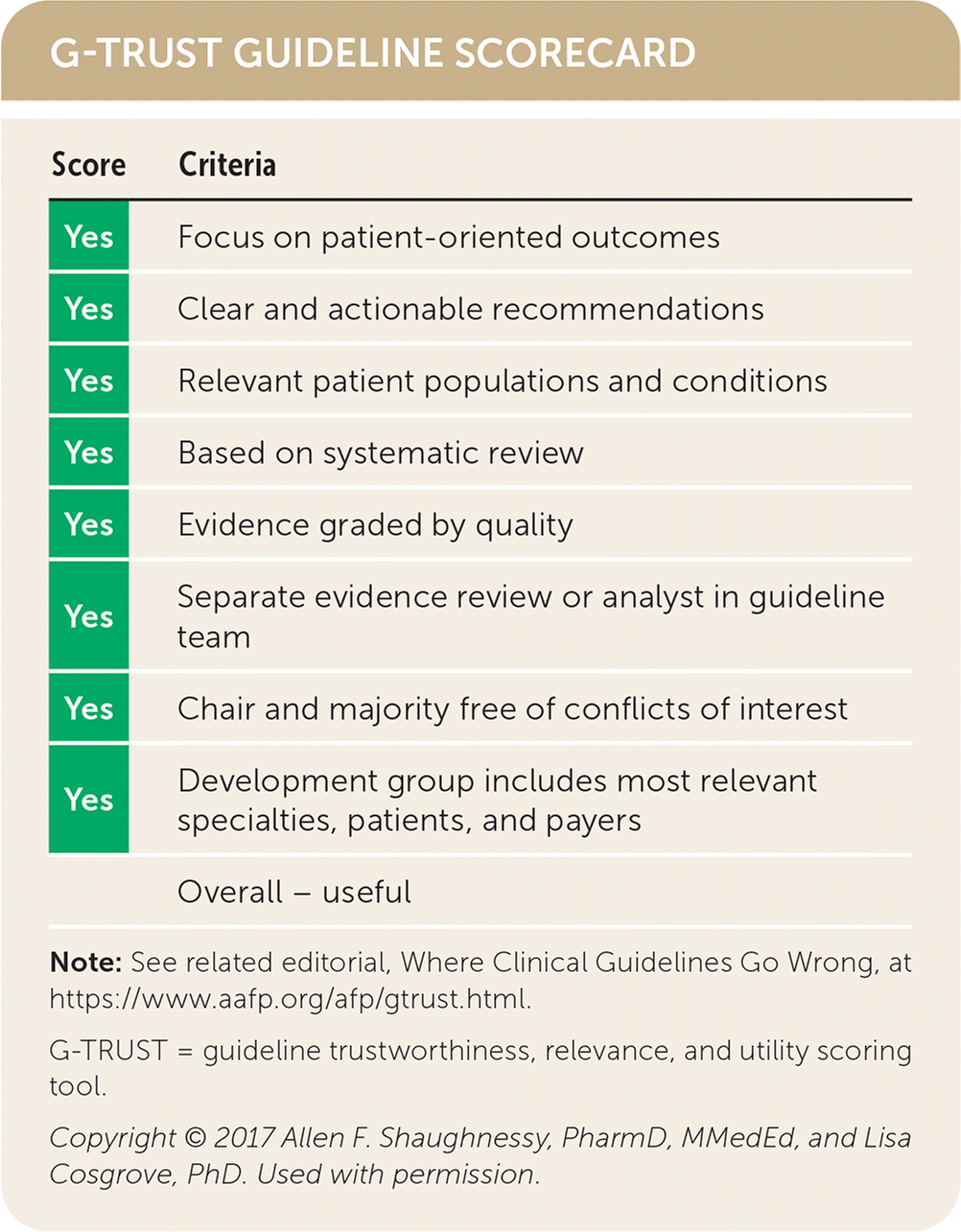
| Score | Criteria |
|---|---|
| Yes | Focus on patient-oriented outcomes |
| Yes | Clear and actionable recommendations |
| Yes | Relevant patient populations and conditions |
| Yes | Based on systematic review |
| Yes | Evidence graded by quality |
| Yes | Separate evidence review or analyst in guideline team |
| Yes | Chair and majority free of conflicts of interest |
| Yes | Development group includes most relevant specialties, patients, and payers |
| Overall – useful |
Note: See related editorial, Where Clinical Guidelines Go Wrong, at https://www.aafp.org/afp/gtrust.html.
G-TRUST = guideline trustworthiness, relevance, and utility scoring tool.
Copyright © 2017 Allen F. Shaughnessy, PharmD, MMedEd, and Lisa Cosgrove, PhD. Used with permission.
The views expressed are those of the authors and do not necessarily reflect the official policy or position of the U.S. Department of Veterans Affairs or the U.S. government.
Editor's Note: There are few recent guidelines for the treatment of major depression, and many, like the British National Institute for Health and Care Excellence (NICE) guidelines, are vague in their recommendations. The VA/DoD guidelines may be the most useful, with their recommendation for monotherapy with counseling or medication for uncomplicated (formerly “mild to moderate”) depression and combined therapy for severe, persistent, or recurrent depression. I was impressed by the evidence for continuing treatment, whether medication or psychotherapy, during remission to prevent relapse.—Michael J. Arnold, MD, Contributing Editor
Guideline source: U.S. Department of Veterans Affairs and U.S. Department of Defense
Available at: https://www.healthquality.va.gov/guidelines/MH/mdd

