Am Fam Physician. 2024;109(1):online
Author disclosure: No relevant financial relationships.
Case Scenario
A 33-year-old woman presents with symptomatic anemia. She reports a long history of abnormal uterine bleeding and is currently menstruating. On admission, her blood pressure is 105/90 mm Hg, and her heart rate is 113 beats per minute. She reports lightheadedness when standing and dyspnea on exertion. Her hemoglobin (Hb) is 4.9 g per dL (49.0 g per L), with a mean corpuscular volume of 61.0 μm3 (61.0 fL), which indicates severe iron deficiency. I recommend transfusion of two units of packed red blood cells; however, she tells me that she and her husband are practicing Jehovah's Witnesses, and she provides a blood-refusal advance directive card.
What is my role as a physician when a patient refuses a potentially lifesaving blood transfusion? Are there any circumstances in which physicians have an ethical responsibility to prioritize lifesaving treatment over the requests of a patient or their family members?
Commentary
Critically anemic patients who refuse blood transfusions have an inverse relationship between Hb levels and morbidity and mortality, particularly for Hb levels less than 5.0 g per dL (50.0 g per L).1–3 For every 1 g per dL (10.0 g per L) drop in Hb below 8 g per dL (80.0 g per L), the risk of death increases 2.5-fold.4 Blood transfusions are a foundational component of treating severe anemia and are considered a lifesaving therapy.5 This makes caring for patients with severe anemia who refuse blood transfusions challenging. Physicians are bound by the four principles of medical ethics: autonomy, beneficence, nonmaleficence, and justice.6 To honor a patient's autonomous decision, a physician may face violating the other principles they have sworn to uphold. Respecting a patient's autonomy generally outweighs the other principles when treatment is refused.7 Importantly, declining a specific treatment modality does not imply refusal of all medical care and should not require patients to sign documentation of declining treatment against medical advice.5
Patients may refuse blood transfusions for several reasons, including fear of contracting a bloodborne pathogen, previous adverse transfusion reactions, financial constraints, or the desire to discontinue life-prolonging therapies in a terminal illness; one well-known scenario is refusal on religious grounds, particularly by Jehovah's Witnesses.
Ethical and moral convictions leading patients to avoid blood products have stimulated the development of medical strategies, appropriately termed “bloodless medicine and surgery.” Recommendations have been created collaboratively by organizations, physicians, and patients that are designed to optimize medical outcomes without the use of blood transfusion therapies.5
Some physicians may disagree or are significantly uncomfortable with a patient's choice to refuse blood transfusions. These situations place a heavy emotional toll on health care professionals, especially when the patient risks dying from a “preventable” medical condition or complications of untreated anemia. In these circumstances, it is reasonable for a physician in a nonemergent setting to refer the patient to another health care professional who is aware of the patient's medical preferences and who is willing to assume health care.
The approach to caring for patients refusing blood products can be complex. Individualized, patient-centered interviewing and shared decision-making are essential. First and foremost, the patient must exhibit the capacity to refuse any lifesaving treatment.8 To possess capacity, the patient must be able to understand the information being provided to them at a fundamental level, appreciate the gravity of the situation and the risks and benefits of proposed treatment options and their likely outcomes, evaluate these options through a rational thought process, and clearly and consistently communicate their choice after demonstrating the ability to meet these criteria.9 Autonomous refusal of treatment must be respected, despite the consequences, if a patient is determined to have capacity.7
After capacity is established, important factors in caring for patients refusing blood products include the following:
Determining the unequivocal indication for blood transfusion
Recognizing risks associated with blood-product transfusions
Understanding the ethical, moral, and religious beliefs of the patient
Limiting further blood loss, such as through venipuncture (average blood loss for patients in the intensive care unit is greater than 0.5 g per dL [5.0 g per L] per day during the first three days)10
Negotiating agreement on potential alternative treatment options; this should be conducted in private to avoid external influence (e.g., opinions of friends, family, clergy)
Maintaining rapport and ensuring confidentiality and trust
Having contingency plans for emergencies or adverse developments
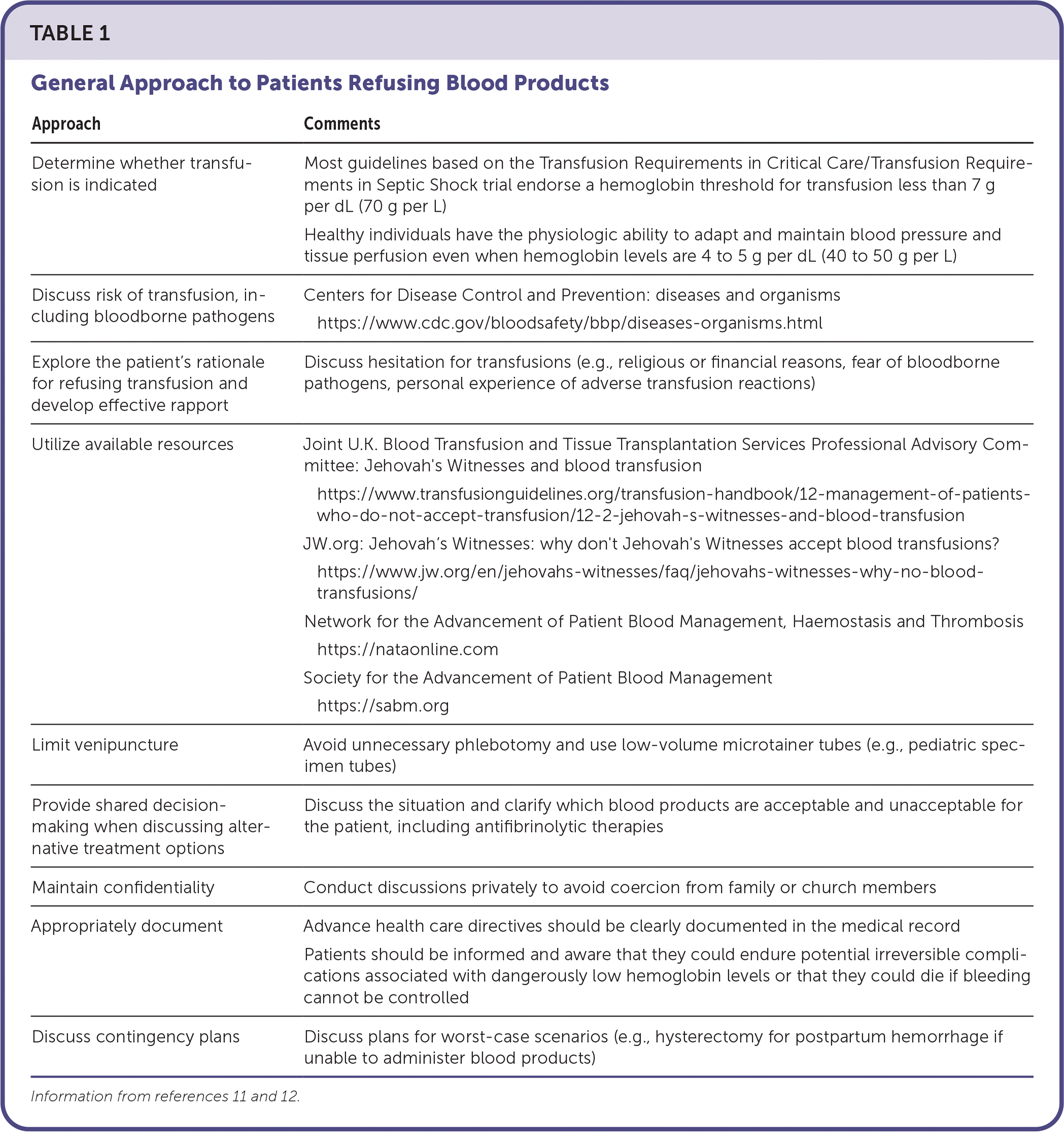
| Approach | Comments |
|---|---|
| Determine whether transfusion is indicated | Most guidelines based on the Transfusion Requirements in Critical Care/Transfusion Requirements in Septic Shock trial endorse a hemoglobin threshold for transfusion less than 7 g per dL (70 g per L) Healthy individuals have the physiologic ability to adapt and maintain blood pressure and tissue perfusion even when hemoglobin levels are 4 to 5 g per dL (40 to 50 g per L) |
| Discuss risk of transfusion, including bloodborne pathogens | Centers for Disease Control and Prevention: diseases and organisms https://www.cdc.gov/bloodsafety/bbp/diseases-organisms.html |
| Explore the patient's rationale for refusing transfusion and develop effective rapport | Discuss hesitation for transfusions (e.g., religious or financial reasons, fear of bloodborne pathogens, personal experience of adverse transfusion reactions) |
| Utilize available resources | Joint U.K. Blood Transfusion and Tissue Transplantation Services Professional Advisory Committee: Jehovah's Witnesses and blood transfusion https://www.transfusionguidelines.org/transfusion-handbook/12-management-of-patients-who-do-not-accept-transfusion/12-2-jehovah-s-witnesses-and-blood-transfusion JW.org: Jehovah's Witnesses: why don't Jehovah's Witnesses accept blood transfusions? https://www.jw.org/en/jehovahs-witnesses/faq/jehovahs-witnesses-why-no-blood-transfusions/ Network for the Advancement of Patient Blood Management, Haemostasis and Thrombosis https://nataonline.com Society for the Advancement of Patient Blood Management https://sabm.org |
| Limit venipuncture | Avoid unnecessary phlebotomy and use low-volume microtainer tubes (e.g., pediatric specimen tubes) |
| Provide shared decision-making when discussing alternative treatment options | Discuss the situation and clarify which blood products are acceptable and unacceptable for the patient, including antifibrinolytic therapies |
| Maintain confidentiality | Conduct discussions privately to avoid coercion from family or church members |
| Appropriately document | Advance health care directives should be clearly documented in the medical record Patients should be informed and aware that they could endure potential irreversible complications associated with dangerously low hemoglobin levels or that they could die if bleeding cannot be controlled |
| Discuss contingency plans | Discuss plans for worst-case scenarios (e.g., hysterectomy for postpartum hemorrhage if unable to administer blood products) |
JEHOVAH'S WITNESSES
Worldwide, more than 8.5 million people are practicing Jehovah's Witnesses, with more than 1.2 million people practicing in the United States.14 Practicing Jehovah's Witnesses are by far the largest group of patients who refuse blood transfusions, and treatment of anemia in this population has been extensively researched.
When approaching a patient who is a Jehovah's Witness and who refuses a potentially lifesaving blood transfusion, it is important to clarify which blood products they are willing to accept because a wide variation of practices exists among Jehovah's Witnesses. The Hospital Liaison Committees for Jehovah's Witnesses was formed to help bridge the gap between members of the religion and the medical community. This organization provides a reference outlining which blood components are prohibited, those that may be acceptable, and others that are subject to personal choice for members of the faith15 (Table 216).

| Unacceptable treatments |
| Allogenic whole blood transfusions |
| Autologous blood transfusions |
| Red blood cells, white blood cells, platelets, plasma transfusions |
| Acceptable treatments |
| Hematopoietic growth factors (e.g., intravenous iron; albumin-free erythropoietin [e.g., darbepoetin alfa, epoetin alfa]; folate; vitamins B12 and C) |
| Immediate discontinuance of anticoagulation drugs (e.g., direct oral anticoagulants, warfarin) and use of appropriate reversal agent |
| Medications that promote hemostasis (e.g., desmopressin, tranexamic acid, aminocaproic acid, vitamin K [if taking warfarin]) |
| Nonblood volume expanders (e.g., lactated ringers, normal saline, hydroxyethyl starches) |
| Oxygen carriers (e.g., hemoglobin-based oxygen carriers, perfluorochemicals) |
| Recombinant clotting factors |
| Personal choice within the religion's guidelines |
| Acute normovolemic hemodilution |
| Minor blood fractions (e.g., immunoglobulins, fibrinogen, cryoprecipitate, serum albumin, recombinant activated factor VIIa, prothrombin complex concentrates) |
Patients who are Jehovah's Witnesses show significant heterogeneity regarding the acceptance of blood components and blood-sparing procedures (e.g., blood cell salvage, acute normovolemic hemodilution).14 Discussions about blood transfusions should be confidential and take place independent of family or church members to avoid coercion or guilt. An anonymous survey revealed that 10% to 12% of Jehovah's Witnesses would accept blood products in life-threatening situations.14 If a patient opts to receive blood anonymously, the physician must ensure complete confidentiality; a patient who is a Jehovah's Witness who accepts a blood transfusion may face serious consequences from the religious community, including being dismissed from that community (i.e., “disfellowshipped”). If a patient resolutely refuses blood products, physicians are strongly discouraged from debating the ethical principles of transfusion refusal with the patient. Further discussion is likely to be considered adversarial and could result in a compromised physician-patient relationship.
Patients who are practicing Jehovah's Witnesses and who need a blood transfusion following trauma may present particularly complex challenges. The trauma may render them incapacitated or incapable of making their own medical decisions. Many Jehovah's Witnesses carry a blood-refusal advance medical directive/release document outlining their refusal of blood products; this directive is considered a legally binding document.8 Nevertheless, courts have ruled both in support of and against physicians who have transfused Jehovah's Witnesses with critical anemia despite possession of blood-refusal cards.17 In almost all instances, a physician is liable for violating the religious belief of a Jehovah's Witness patient with capacity if a blood transfusion is administered either without consent or against the patient's request.17 Physicians treating incapacitated patients who are Jehovah's Witnesses and who require a transfusion but have no available blood-refusal directive or surrogate decision maker should transfuse blood products as a lifesaving measure.17
Another potential ethical predicament for physicians concerns a minor patient whose parents refuse a blood transfusion based on the parents own beliefs. This scenario has much more legal clarity: Based on a 1944 Supreme Court ruling (Prince v. Massachusetts), a precedent established limiting parental authority if it is not in the best interest of the child.14 Several states have laws that provide “mature minor” status for older teenagers. This allows for autonomy for older teenagers to make their own medical decisions, including refusing blood transfusions in the same manner as an adult.14 In the case of an older teenager attempting to refuse treatment, physicians should be familiar with local laws and act accordingly. It is recommended that the hospital ethics committee and medicolegal counsel should be consulted in such cases.
NONBLOOD TRANSFUSION TREATMENT OPTIONS
Alternative treatments, some of which have proven benefits, should be offered to patients with severe anemia or active bleeding who refuse blood transfusions. These treatment options include hematopoietic growth factors (e.g., albumin-free erythropoietin; intravenous iron; vitamins B12 and C; folate), minor blood fractions (e.g., prothrombin complex concentrate, fibrinogen concentrate), prothrombotic drugs (e.g., tranexamic acid, recombinant factor VIIa), and nonblood volume expanders.14 The goal is to optimize the patient's hematopoiesis while minimizing further blood loss and improving hemostasis.17 Another strategy is acute normovolemic hemodilution, which involves removing whole blood from the patient before surgery with maintenance of normovolemia using crystalloid intraoperatively (hemodilution). This process reserves blood for postoperative use and reduces the total amount of red blood cells and clotting factors lost intraoperatively.3,14 In addition to these measures, physicians should limit laboratory testing and use pediatric specimen tubes and point-of-care testing whenever possible.14
Hb-based oxygen carriers are alternatives to red blood cell transfusion.2,14 These agents have not been approved by the U.S. Food and Drug Administration and have potentially severe adverse effects, including systemic vasoconstriction, thrombosis, and increased risk of death.2 The carriers may be used as a temporizing measure to improve oxygenation in severely anemic patients who are unable to receive blood transfusions. Compassionate use of Hb-based oxygen carriers is available; however, with tight regulatory processes and preapproval from the U.S. Food and Drug Administration, it can take more than 24 hours to obtain these products, making them less useful for acute trauma.18
Case Resolution
The patient in the scenario should receive extensive education about the risk of potential complications associated with critical anemia, including the possibility of death. Before discussing transfusion of blood products with the patient, the physician should request that the patient's husband or family be excused to avoid potential coercion. Potentially helpful interventions to boost hematopoiesis, including intravenous iron, subcutaneous darbepoetin alfa, and vitamins C and B12, should be provided. Assessing and addressing the underlying cause of her blood loss should occur, for example, initiating tranexamic acid therapy and requesting gynecologic consultation. The patient can be safely discharged after her anemia symptoms improve, an increase in the Hb count is demonstrated, and no additional blood loss has occurred.
The views expressed herein are those of the authors and do not necessarily reflect the official policy of the U.S. Department of the Army, the U.S. Department of Defense, or the U.S. government.