Clinical Question
Does the use of a peanut ball in pregnant patients with an epidural improve labor outcomes?
Evidence-Based Answer
In pregnant patients laboring with epidural anesthesia, the use of a peanut ball with regular position changes decreases the duration of first-stage labor by 87 minutes compared with usual care (Figure 1). (Strength of Recommendation [SOR]: A, meta-analysis of randomized controlled trials [RCTs].) The effect may be more pronounced in primiparous patients. (SOR: B, single RCT.) A patient safety bundle that includes several improvements in labor support, including the use of a peanut ball, is associated with a reduction in cesarean deliveries. (SOR: B, cross-sectional cohort study.)
FIGURE 1.
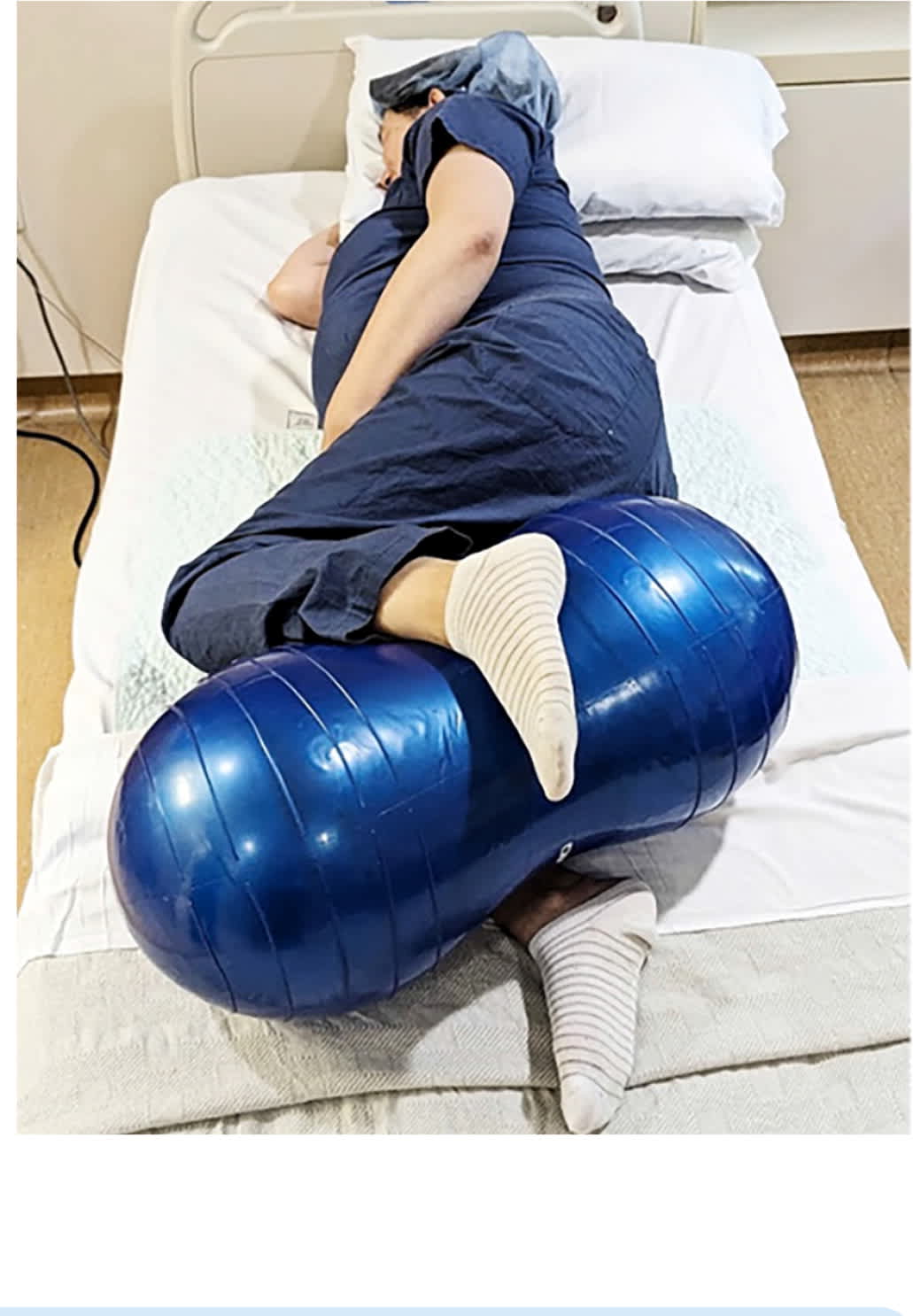
Use of a peanut ball in the knee-to-knee position.
Evidence Summary
A 2022 systematic review and meta-analysis of four randomized or quasirandomized clinical trials (n = 818) compared the effect of using a peanut ball with usual care for laboring patients with epidural analgesia.1 In the intervention groups, researchers encouraged primiparous and multiparous patients 18 to 35 years of age with a singleton fetus in vertex position to use a peanut ball soon after epidural placement for at least 15 minutes every hour until reaching full cervical dilation. Patients changed position every 0.5 to 2 hours while using the peanut ball. Compared with patients receiving usual care, those laboring with a peanut ball had a shorter first stage of labor (two trials; n = 272; mean difference [MD] = 87.5 minutes; 95% CI, 80.3 to 94.5; high-certainty evidence based on the GRADE system) and a shorter second stage of labor (one trial; n = 201; MD = 22.2 minutes; 95% CI, 20.8 to 23.5; moderate-certainty evidence). The use of a peanut ball as a single intervention did not significantly change the risk of cesarean delivery (three trials; n = 669; relative risk = 0.75; 95% CI, 0.57 to 1.00; low-certainty evidence).
The two RCTs used in this meta-analysis did not consistently demonstrate a decrease in the duration of first stage of labor for all patients. The larger of the two trials, a 2015 RCT (n = 201) conducted at an inner-city teaching hospital, analyzed the effects of a peanut ball vs. position changes (deemed usual care) in patients who received an epidural.2 Researchers defined the primary outcomes as the length of labor and vaginal delivery rates. The control group changed position every 1 to 2 hours, whereas the intervention group received a peanut ball to use after epidural administration and then made position changes. Researchers enrolled patients with a mean age of 27 years; 56% were nulliparous, and an equal number of Hispanic and non-Hispanic White patients participated. In the raw data, the group using the peanut ball in addition to position changes had a shorter first stage (269 vs. 356 minutes; P < .01) and second stage (21 vs. 44 minutes; P < .001) of labor and a lower cesarean delivery rate (10% vs. 21%; P < .05) than patients in the usual care group. However, after the authors controlled for differences in parity and cervical dilation between the groups, there was no difference in the duration of the first stage of labor (MD = 29 minutes; P = .053), but the second stage of labor was significantly shorter (MD = 11 minutes; P < .001). After parity adjustment, use of the peanut ball was associated with fewer cesarean deliveries (odds ratio = 0.41; P = .04). Researchers identified no harms from use of the peanut ball.
A 2016 RCT (n = 149) from the previous systematic review (but not part of the meta-analysis due to incomplete outcome reporting) sought to determine whether the peanut ball would decrease the duration of labor in patients with epidurals.3 Patients had a mean age of 31 years, 30% were primiparous, and 76% were White. Patients assigned to the intervention group had a peanut ball placed between their knees within 30 minutes after epidural administration with lateral position rotation every 30 minutes. Patients in the control group used one pillow between their knees (if desired) and followed a similar rotation protocol. Overall, no decrease was shown for multiparous patients. However, in a subanalysis of patients given oxytocin, the peanut ball shortened the first-stage of labor for primiparous patients by 177 minutes and lengthened it by 32 minutes in multiparous patients (between groups; P = .018). There was no difference in either group in the duration of second-stage labor. This study's small number of primiparous patients limited its certainty (n = 45). Researchers did not track cesarean delivery rates.
A pre- and postguideline implementation study compared cesarean delivery rates among nulliparous women with term, singleton, and vertex presentation pregnancies at three hospitals before (n = 434) and after (n = 401) initiating a system-wide patient safety bundle that included peanut ball use as part of standardized labor support.4 Use of the safety bundle resulted in increased use of peanut balls (16% to 45% of labors; P < .001) and maternal position changes (79% to 88% of labors; P = .001). Although the duration of labor was not measured and the protocol used many interventions in addition to peanut balls, the overall cesarean delivery rate in the health system significantly decreased (28% to 20%; P = .006).
Recommendations From Others
In 2018, the Council on Patient Safety in Women's Health Care (which included representatives from the American Academy of Family Physicians and the American College of Obstetricians and Gynecologists) recommended implementing maternity safety bundles to decrease the number of primary cesarean deliveries.5 The Council referenced a toolkit recommending that all maternity care units provide education to support “freedom of movement in labor, upright and ambulatory positioning, techniques and tools (such as the peanut ball) that facilitate fetal rotation, flexion, and descent for women with epidural anesthesia, and maternal exercises and positioning that facilitate fetal rotation in women with and without epidural anesthesia.”6
Copyright © Family Physicians Inquiries Network. Used with permission.

