Am Fam Physician. 2026;113(4):313-314B
Author disclosure: No relevant financial relationships.
Safe drinking water is essential to human health, yet it is often overlooked in routine clinical care. As trusted front-line clinicians, family physicians are uniquely positioned to ask patients about their water sources and provide practical counseling. A brief inquiry can uncover hidden risks and prevent acute and chronic illness, and addressing access to safe drinking water is a worthwhile addition to preventive care conversations.
Approximately 85% of the US population receives drinking water from regulated public water systems, whereas about 15% rely on private wells.1 Oversight under the Safe Drinking Water Act provides protection, but contamination and infrastructure failures continue to occur.2,3 Flooding, water main breaks, or lapses in treatment can allow bacteria and chemicals to reach household water taps. The water crisis in Flint, Michigan, remains a stark reminder of a change in source water leading to widespread lead contamination, elevated blood lead levels in children, and at least a dozen deaths from Legionnaires disease.3,4 Even after expensive remediation and legal settlements, many residents remain distrustful of their tap water.3,4
Private wells receive no federal oversight; this lack of regulation affects 43 million people in the United States who rely on well water.1 Unless homeowners test their own water supply, no monitoring occurs.1 Geographic risks vary: Nitrates are common in agricultural areas, arsenic is found in parts of the Midwest and Southwest, and per- and polyfluoroalkyl substances (PFAS) are found near industrial or military sites.5–7 Microbial contamination is common after flooding or well damage.
Water that looks, smells, or tastes normal can still be unsafe to drink. Without testing, families may consume water linked with increased risks of cancer, cardiovascular disease, or adverse pregnancy outcomes. Family physicians screen for hypertension, diabetes, and cancer; we can also ask about safe drinking water. Unsafe water poses a silent risk with profound health consequences.
Certain groups are particularly vulnerable to adverse health effects from unsafe drinking water. Pregnant patients exposed to nitrates face an increased risk of preterm birth and poor outcomes. Lead crosses the placenta and has been associated with miscarriage and impaired infant neurodevelopment. Arsenic exposure is linked to infant mortality and low birth weight, and PFAS are associated with hypertensive disorders of pregnancy and reduced birth weight.6–10 Infants are especially susceptible to nitrate-induced methemoglobinemia and microbial illness, particularly when formula is prepared with unsafe water. Immunocompromised patients may require extra precautions, such as boiling water or using certified microbial-reduction filters during boil water alerts and advisories.
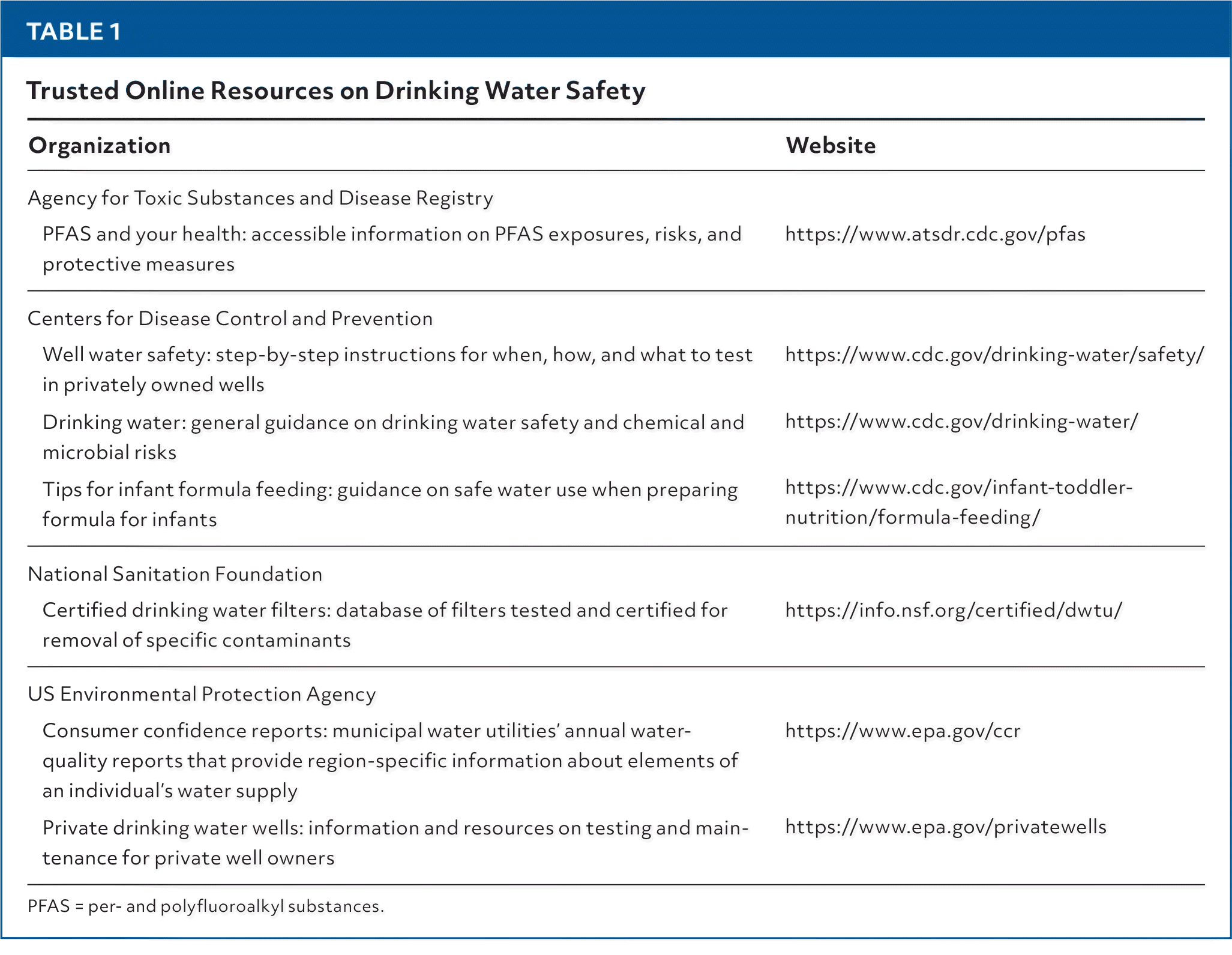
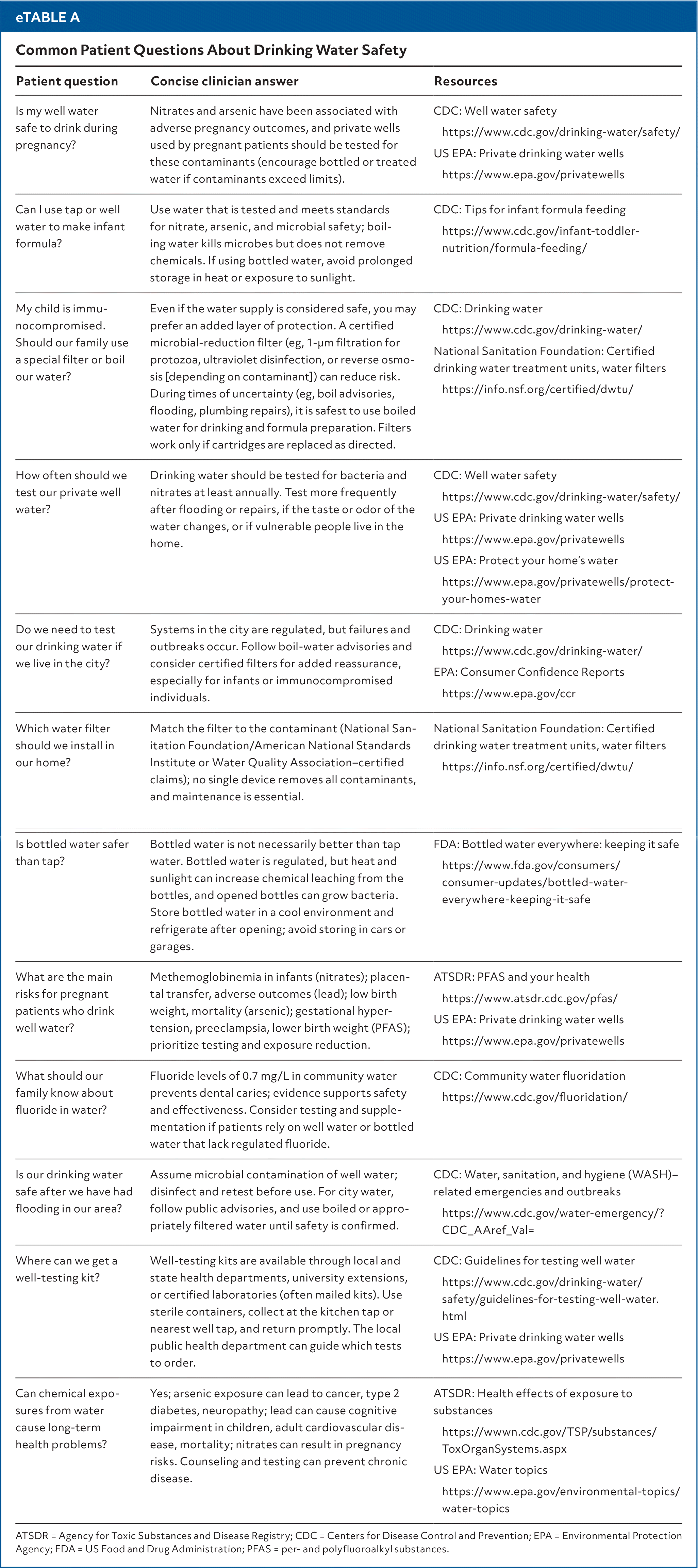
Some physicians may hesitate to address safe drinking water, concerned that counseling is too technical or time consuming. Asking about a patient's drinking water source, acknowledging potential risks, and suggesting reliable resources can make a meaningful difference. In less than a minute, physicians can ask where a patient's drinking comes from, advise testing if it is from a private well, and direct patients to appropriate guidance. Table 1 provides links to guidelines from the Centers for Disease Control and Prevention, US Environmental Protection Agency, and other organizations. The granular details (eg, when to test wells, which filters to use, how to respond to boil advisories) are detailed in eTable A. These tools allow clinicians to offer accurate advice without memorizing contaminants or standards.
| Organization | Website |
|---|---|
| Agency for Toxic Substances and Disease Registry | |
| PFAS and your health: accessible information on PFAS exposures, risks, and protective measures | https://www.atsdr.cdc.gov/pfas |
| Centers for Disease Control and Prevention | |
| Well water safety: step-by-step instructions for when, how, and what to test in privately owned wells | https://www.cdc.gov/drinking-water/safety/ |
| Drinking water: general guidance on drinking water safety and chemical and microbial risks | https://www.cdc.gov/drinking-water/ |
| Tips for infant formula feeding: guidance on safe water use when preparing formula for infants | https://www.cdc.gov/infant-toddler-nutrition/formula-feeding/ |
| National Sanitation Foundation | |
| Certified drinking water filters: database of filters tested and certified for removal of specific contaminants | https://info.nsf.org/certified/dwtu/ |
| US Environmental Protection Agency | |
| Consumer confidence reports: municipal water utilities' annual water-quality reports that provide region-specific information about elements of an individual's water supply | https://www.epa.gov/ccr |
| Private drinking water wells: information and resources on testing and maintenance for private well owners | https://www.epa.gov/privatewells |
| Patient question | Concise clinician answer | Resources |
|---|---|---|
| Is my well water safe to drink during pregnancy? | Nitrates and arsenic have been associated with adverse pregnancy outcomes, and private wells used by pregnant patients should be tested for these contaminants (encourage bottled or treated water if contaminants exceed limits). | CDC: Well water safety https://www.cdc.gov/drinking-water/safety/ US EPA: Private drinking water wells https://www.epa.gov/privatewells |
| Can I use tap or well water to make infant formula? | Use water that is tested and meets standards for nitrate, arsenic, and microbial safety; boiling water kills microbes but does not remove chemicals. If using bottled water, avoid prolonged storage in heat or exposure to sunlight. | CDC: Tips for infant formula feeding https://www.cdc.gov/infant-toddler-nutrition/formula-feeding/ |
| My child is immunocompromised. Should our family use a special filter or boil our water? | Even if the water supply is considered safe, you may prefer an added layer of protection. A certified microbial-reduction filter (eg, 1-μm filtration for protozoa, ultraviolet disinfection, or reverse osmosis [depending on contaminant]) can reduce risk. During times of uncertainty (eg, boil advisories, flooding, plumbing repairs), it is safest to use boiled water for drinking and formula preparation. Filters work only if cartridges are replaced as directed. | CDC: Drinking water https://www.cdc.gov/drinking-water/ National Sanitation Foundation: Certified drinking water treatment units, water filters https://info.nsf.org/certified/dwtu/ |
| How often should we test our private well water? | Drinking water should be tested for bacteria and nitrates at least annually. Test more frequently after flooding or repairs, if the taste or odor of the water changes, or if vulnerable people live in the home. | CDC: Well water safety https://www.cdc.gov/drinking-water/safety/ US EPA: Private drinking water wells https://www.epa.gov/privatewells US EPA: Protect your home's water https://www.epa.gov/privatewells/protect-your-homes-water |
| Do we need to test our drinking water if we live in the city? | Systems in the city are regulated, but failures and outbreaks occur. Follow boil-water advisories and consider certified filters for added reassurance, especially for infants or immunocompromised individuals. | CDC: Drinking water https://www.cdc.gov/drinking-water/ EPA: Consumer Confidence Reports https://www.epa.gov/ccr |
| Which water filter should we install in our home? | Match the filter to the contaminant (National Sanitation Foundation/American National Standards Institute or Water Quality Association–certified claims); no single device removes all contaminants, and maintenance is essential. | National Sanitation Foundation: Certified drinking water treatment units, water filters https://info.nsf.org/certified/dwtu/ |
| Is bottled water safer than tap? | Bottled water is not necessarily better than tap water. Bottled water is regulated, but heat and sunlight can increase chemical leaching from the bottles, and opened bottles can grow bacteria. Store bottled water in a cool environment and refrigerate after opening; avoid storing in cars or garages. | FDA: Bottled water everywhere: keeping it safe https://www.fda.gov/consumers/consumer-updates/bottled-water-everywhere-keeping-it-safe |
| What are the main risks for pregnant patients who drink well water? | Methemoglobinemia in infants (nitrates); placental transfer, adverse outcomes (lead); low birth weight, mortality (arsenic); gestational hypertension, preeclampsia, lower birth weight (PFAS); prioritize testing and exposure reduction. | ATSDR: PFAS and your health https://www.atsdr.cdc.gov/pfas/ US EPA: Private drinking water wells https://www.epa.gov/privatewells |
| What should our family know about fluoride in water? | Fluoride levels of 0.7 mg/L in community water prevents dental caries; evidence supports safety and effectiveness. Consider testing and supplementation if patients rely on well water or bottled water that lack regulated fluoride. | CDC: Community water fluoridation https://www.cdc.gov/fluoridation/ |
| Is our drinking water safe after we have had flooding in our area? | Assume microbial contamination of well water; disinfect and retest before use. For city water, follow public advisories, and use boiled or appropriately filtered water until safety is confirmed. | CDC: Water, sanitation, and hygiene (WASH)–related emergencies and outbreaks https://www.cdc.gov/water-emergency/?CDC_AAref_Val= |
| Where can we get a well-testing kit? | Well-testing kits are available through local and state health departments, university extensions, or certified laboratories (often mailed kits). Use sterile containers, collect at the kitchen tap or nearest well tap, and return promptly. The local public health department can guide which tests to order. | CDC: Guidelines for testing well water https://www.cdc.gov/drinking-water/safety/guidelines-for-testing-well-water.html US EPA: Private drinking water wells https://www.epa.gov/privatewells |
| Can chemical exposures from water cause long-term health problems? | Yes; arsenic exposure can lead to cancer, type 2 diabetes, neuropathy; lead can cause cognitive impairment in children, adult cardiovascular disease, mortality; nitrates can result in pregnancy risks. Counseling and testing can prevent chronic disease. | ATSDR: Health effects of exposure to substances https://wwwn.cdc.gov/TSP/substances/ToxOrganSystems.aspx US EPA: Water topics https://www.epa.gov/environmental-topics/water-topics |
Practical examples can frame the conversation. Individuals may believe bottled water is inherently safer, but prolonged heat or sun exposure can cause chemical leaching from plastic bottles and bacterial growth after opening.2 Some may assume that any filter is protective, when in fact filters must be matched to specific contaminants and replaced as directed. By correcting misconceptions and directing patients to certified products and local testing programs, family physicians can empower families to take manageable steps toward safer water use.
Waterborne illness is more common than many realize. Surveillance from 1971 to 2006 identified hundreds of outbreaks, and endemic gastrointestinal disease linked with water is estimated to affect millions in the United States annually.2 Beyond infections, chronic exposure to contaminants carries a heavy burden. Arsenic contributes to cancer, hypertension, type 2 diabetes, and neuropathy; lead impairs cognition in children and increases cardiovascular mortality in adults; and nitrates endanger pregnant women and infants. Family physicians already work diligently to avoid these conditions through other preventive services. Counseling about drinking safe water extends this preventive mission into an often-ignored domain.
Water safety belongs in the examination room. Physicians do not need to be experts in hydrology, but we should embrace the opportunity to identify hidden risks and connect patients with appropriate resources. Asking about sources of drinking water during prenatal visits, well-child checks, or wellness examinations can uncover hazards that patients may not suspect.
Drinking water safety is an often overlooked yet critical area where family physicians can profoundly affect their patients' health. Brief, targeted counseling helps to prevent not only acute infections but also long-term, debilitating diseases that often take years or decades to develop. By routinely inquiring about potable water sources and educating patients, we can identify hidden hazards early, connect patients with vital resources, and ultimately save lives. Integrating drinking water safety into practice is not only feasible—it is preventive medicine at its best.