Medicare spending slows; leaders call for more
Medicare spending growth slowed to 1.5 percent in 1998, the smallest rate of growth since the program's creation in 1965. Over the past decade, Medicare spending has increased at an average rate of 10 percent annually. As recently as 1997, Medicare spending grew at a rate of 7.2 percent.
Likely explanations for the record-setting low growth include cuts in payments to hospitals, physicians and other providers under the 1997 Balanced Budget Act (BBA) as well as the government's crackdown on health care fraud and abuse. In addition, delays in Medicare payments may have shifted small amounts of Medicare spending from 1998 to 1999.
Meanwhile, a bipartisan group of health care leaders, including three former HCFA administrators, is asking Congress and the Clinton administration to increase HCFA's funding so it can carry out the regulatory duties it received under the Health Insurance Portability and Accountability Act of 1996, the 1997 BBA and the Children's Health Insurance Program, as well as administer Medicare and Medicaid.
Site offers one-stop shopping for clinical policies
In January, the federal government officially launched its web-based National Guideline Clearinghouse (NGC), http://www.guideline.gov.
The NGC is an online repository of evidence-based clinical policies (also known as practice guidelines or parameters) that makes comparing individual policies much easier. The policies are presented with standardized abstracts and tables that highlight areas of agreement and disagreement.
The NGC was developed by the Agency for Health Care Policy and Research in partnership with the AMA and the American Association of Health Plans. Currently, the clearinghouse includes information on about 400 clinical policies.
For more information on the NGC and other sources of clinical policies, see “Where to Look for Good Clinical Policies.”
How much are you paying your management staff?
A 1998 survey from the Health Care Group, a consulting firm based in Plymouth Meeting, Pa., reports these average salaries for key office-management positions:
- Office managers, $39,600;
- Administrators, $56,400;
- Business managers, $42,600.
The survey found that salaries generally increased based on practice size, manager's level of education and the number of employees supervised. Years of experience seemed to have “no relationship at all to the salary received.”
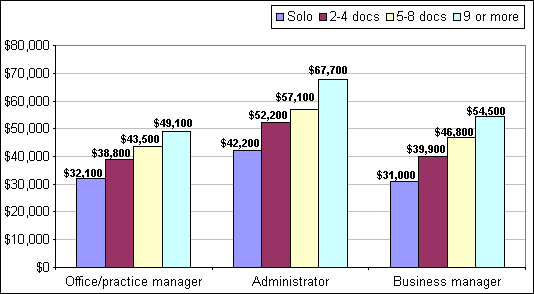
Source: The Health Care Group. “Manager/Administrator Compensation Package Survey,” On Managing newsletter. Plymouth Meeting, Pa: Health Care Publishing; 1998:2.
Doctors fleeing HMOs?
Citing low reimbursement, administrative headaches and intrusions on the doctor-patient relationship, several physician groups have recently turned their backs on managed care organizations.
- The San Francisco Chronicle reports that 600 doctors belonging to the San Mateo Independent Practice Association have rejected a contract from Aetna U.S. Healthcare that would have covered 20,000 patients. It is reportedly the largest contract any physician group has walked away from in California.
- The Journal of Commerce reports that “a small but growing number of Southern California physicians are bolting from the fold of managed care organizations and going on their own.” Among them are the physicians of Memorial Prompt Care in Westminster, Calif., who recently decided to sever their managed care ties, which represent more than 1,000 patients for the practice.
- The New York Times reports that while there is hardly a mass exodus, a “startling” number of physicians in New York are scaling back or withdrawing altogether from managed care plans. Over the past three months, 10 percent of physicians associated with New York Presbyterian Hospital have quit their managed care plans; 50 percent have cut back the number of plans with which they participate.
HMOs sued over compensation methods
The state of Texas recently sued six HMOs for “illegally compensating doctors who limited patients' medical care and penalizing those who didn't,” says the AP/ Kansas City Star.
At issue, according to Texas' then- Attorney-General Dan Morales, is the HMO practice of offering financial incentives to physicians for limiting treatment. “We cannot allow the accountants and lawyers at the HMOs to make decisions about what is proper medical care for patients,” he said. “That is a decision reserved for patients' doctors, and those doctors should not be manipulated by the HMOs.”
The HMOs deny any illegal activity and say Texas and federal regulators had approved their compensation policies, which they say are designed to encourage efficiency.
Reference(s)
- 1.Texas takes aim at HMOs' policies. Kansas City Star. Dec. 17, 1998:A-7.
Studies find increasing numbers of uninsured
The number of Americans lacking health insurance is increasing and likely to keep rising over the next few years, according to three recent reports.
A study in the January issue of the American Journal of Public Health finds that one of six Americans lacks health insurance, up from one in seven at the end of the 1980s (an increase of about 10 million). The authors note that this increase has come during a period of healthy national economic growth.
The proportion of uninsured Americans is higher in the nation's largest cities. A study released by the UCLA Center for Health Policy Research in December reported that almost one-fifth of nonelderly people in America's 85 largest cities lack health coverage. The study found that areas with high numbers of uninsured people tend to have more small employers, which are less likely to offer health coverage to their workers.
A third study, released in December by the Health Insurance Association of America, projects that more than one-fifth of all nonelderly Americans will be without health coverage by 2007 if current economic conditions continue. If the economy takes a downturn and if health care costs increase more than anticipated, the study estimates that the proportion might be almost 25 percent.
Reference(s)
- 1.Carrasquillo O, Himmelstein DU, Woolhandler S, Bor DH. Going bare: trends in health insurance coverage, 1989 through 1996. Am J Pub Health. 1999;89(1):36-42.
Quote. End quote.
“I don't believe anyone in the Federal Bureau of Investigation or the Department of Justice thinks most physicians are crooks. We realize it's a small percentage. Unfortunately, that small percentage takes a fairly significant amount of the money — money that should be going into the pockets of legitimate providers.”
Joanne Madden, a special agent with the FBI, speaking to representatives of medical societies in HCFA's Kansas City region.
HCFA ‘increasingly optimistic’ about Y2K deadline
Although the General Accounting Office in September pronounced it “severely behind schedule” in becoming year 2000 compliant, HCFA says it's now on its way to meeting the federal government's March 31 deadline for working the millennium bug out of its systems.
The agency's 25 most critical computer systems have been validated by external Y2K consultants, and Medicare's contractors have completed Y2K-compliance work on 95 percent of their software code. “I'm increasingly optimistic that we are going to not only meet the March 31 deadline but beat it,” says HCFA Administrator Nancy-Ann Min DeParle.
HCFA now is turning its attention to developing up to 60 backup plans for potential Y2K problems, including how to reroute claims if a contractor's computers or telephones fail.
Estimates of the cost of HCFA's Y2K compliance range from $632 to $755 million.
Reference(s)
- 1.Barr S. Hurdles in Medicare's race for Y2K fix. The Washington Post. Jan. 4, 1999:A-17.


