
Stressed from within and without, family practice could flourish or fade in the coming years.
Fam Pract Manag. 2001;8(8):43-48

As family practice enters its fourth decade, some family physicians have begun to wonder whether the specialty is suffering a sort of midlife crisis. That may seem surprising. After all, family practice – established in direct response to public need for accessible health care – has not only survived, but thrived. In 1999 (the last year for which data are available), family physicians provided 171 million of the 757 million visits to office-based physicians, 35 million more than any other specialty.1 In 2000, family practice had more residency programs than any other specialty2 and more board-certified physicians than any other specialty except for internal medicine.3 Just as its founders had envisioned, family practice has become the primary-care foundation for the entire U.S. health care system.
And yet primary care match numbers are down for a fourth consecutive year. Midlevel providers, hospitalists and subspecialists continue to chip away at family physicians’ scope of practice, while more and more family physicians willingly give up areas of practice once considered sacred. And comprehensive, continuing patient care – the hallmark of family practice – is becoming increasingly difficult to provide in a fragmented health care system where external productivity pressures, increasing rules and regulations, and concern for short-term profits threaten to compromise the patient-physician relationship. Moreover, focus groups sponsored by the AAFP found no clear indication that consumers even know who family physicians are or what they can provide.
While you may not be aware of it, there’s currently a lively discussion going on among your colleagues about the state of the specialty and how it should evolve in the changing health care environment to best meet the needs of patients and society.
KEY POINTS
Many family physicians are feeling frustrated as they try to provide quality patient care in a fractured health care system.
There is also concern within the specialty about what a family physician should be, how future FPs are being trained and how technology is impacting patient care.
Most family physicians agree that the specialty needs to be proactive if it is going to continue to play a major role in meeting the needs of patients and society.
Keystone III
One major locus of that discussion was the recent Keystone III conference. Last October, the “family” of family medicine organizations (the AAFP, the American Academy of Family Physicians Foundation, the American Board of Family Practice, the Association of Departments of Family Medicine, the Association of Family Practice Residency Directors, the North American Primary Care Research Group and the Society of Teachers of Family Medicine) convened the conference to discuss family practice in the United States and to consider its status after 30 years of development. [The formal discussion papers from Keystone III were published in the April 2001 issue of Family Medicine, available online at www.stfm.org/fmhub/fmhub.html.]
Like Keystone I (1984) and II (1988), Keystone III was not intended to create an action plan but, rather, to hold a structured conversation about key issues facing the specialty. This time, the 82 Keystone attendees came away from the conference with a general sense that some action is needed to ensure a bright future for the specialty.
The system is broken, not the specialty
“This is another of those tumultuous times in all of medicine,” says Larry Green, MD, director of the Robert Graham Center for Policy Studies in Family Practice and Primary Care in Washington, D.C., and one of the organizers of Keystone III. “Most disciplines, not just medicine, and most specialties, not just family practice, are being confronted with having to reconsider their values, their purpose, their methods and the best way to organize themselves to do their work.”
According to Green, family medicine is particularly stressed by the current health care system. “It’s extremely difficult to accomplish the objectives of primary care because the system doesn’t support doing it. Primary care’s salutatory effects depend in part on a trusting, sustained partnership between doctors and patients, but the system constantly thwarts this. Insured lives are bought and sold and the ‘best’ doctor is the one who can crank the most patients through in the shortest time. The business model of medicine doesn’t work anymore.”
This notion of family physicians battling against a health care system that hinders their best efforts was one common theme among Keystone attendees. “Here’s what worries me,” says William Phillips, MD, MPH, a family physician from Seattle, a member of the FPM board of editors and a Keystone presenter, “I hear more and more family physicians saying, ‘You know, I wasn’t able to do my best for Mrs. Jones today. The system wouldn’t let me.’
“What has always kept us going has been the fulfillment that comes from knowing, ‘I did something special for Mrs. Jones today.’ I hear family doctors saying that less often,” says Phillips. “We need to understand and protect what makes family doctors feel good about being family doctors. Otherwise, there’s not much motivation to continue to put up with what is a very hard job with relatively low pay and a lot of frustration.”
Perry A. Pugno, MD, MPH, director of the AAFP division of medical education, believes the stresses family physicians are feeling have little to do with their specialty and everything to do with economics. “You can’t spend that little bit of extra time with that individual patient who periodically needs it because profit margins are now so narrow that it may make the difference between whether you make your bottom line or not,” he says. “Physician dissatisfaction is not with the core concepts of the discipline. It’s dissatisfaction with the economic system and how the system has encroached on the patient relationship.” (For more information on physician satisfaction, see the box.)
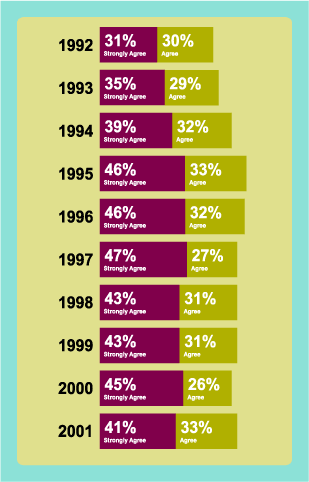
WOULD YOU WANT TO BE A FAMILY PHYSICIAN AGAIN?
Family practice may not be a bed of roses in today’s health care environment, but it’s not all doom and gloom either. Asked whether they would do it over again if they could, almost 74 percent of family physicians agree or strongly agree that they would.
Scope of practice is changing
One of the defining characteristics of family practice has always been the special relationship family physicians have with their patients. Family physicians often mention providing cradle-to-grave care for a community of patients as a source of their deepest satisfaction. Yet, within the context of the current health care system, this kind of care has become more difficult to provide. Hospitals and health plans increasingly frustrate family physicians’ attempts to practice a full scope, for example by mandating use of hospitalists, refusing to pay for certain procedures performed in family physicians’ offices or offering little or no financial incentive (or a disincentive) to practice a broad scope. And of course, some family physicians have purposely decided to limit their scope for a variety of personal reasons, including a desire for a fuller life outside of medicine. The decision to self-limit scope of practice is creating some concern and much discussion within the specialty.
“When I was first in practice, the 80-hour weeks and the 16-hour days were expected of us,” says Robert Avant, MD, executive director of the American Board of Family Practice and a Keystone attendee. “But we’re hearing from younger physicians that they don’t want that lifestyle. I think they’re smart, and I think we have to recognize and respect their desire to pay more attention to their personal and family lives instead of getting frustrated by it.” [For more on scope of practice issues, see “Are the Edges of Family Practice Being Worn Away?” FPM, February 2000, page 35.]
Demographics are changing
Thirty years ago, the medical profession was dominated by older white males who cared for a population of Americans who looked up to them and shared their culture. The face of America looks much different now. There’s increasing racial and ethnic diversity, the gender balance is shifting and the population is aging. And it has had its effect on family practice. For example, ethnic groups bring their own set of culture-specific problems and health beliefs to the family physician’s office, and aging brings more chronic disease care.
Compounding this is the realization that concepts of family and community have also changed. “We’re not really dealing with the nuclear family anymore,” says Terrence Steyer, MD, assistant professor of family medicine at the Medical University of South Carolina, Charleston, and a Keystone attendee. “We’ve got high divorce rates, single-parent households, same-gender partnerships with children and so on. Our traditional notion of what makes a family or what makes a community no longer really exists.”
Steyer believes that technology has had a major impact on our sense of community. “It used to be that a patient might say to me, ‘I talked to my neighbor across the street about my high blood pressure,’ but now they’re coming in saying, ‘I got this information from an Internet chat room about high blood pressure or some other condition, and this is what this guy in California or Washington is saying. What do you think?’ It’s really changed the way I view community and people’s support systems,” Steyer says.
Technology is a double-edged sword
Information technology has given family physicians more access to scientific information and more resources to support comprehensive practice, but it has also changed both patient and physician expectations about just how comprehensive family physicians need to be. “We have professors telling students that because of the information explosion, 50 percent of what they learn in medical school will be obsolete by the time they finish residency,” Steyer says. “Search the Internet for health-related Web sites and you find something like a million sites. Turn on your television and there’s almost always something medically related on the evening news. There’s just no way to keep track of all the information. It’s overwhelming to students.”
Not to mention practicing physicians. But technology also provides the opportunity to practice more evidence-based medicine and improve patient relationships.
“In a way, it’s what we’ve always been looking for,” says Deborah McPherson, MD, assistant director of the AAFP’s division of medical education and a Keystone attendee. “For example, I see a patient with Bell’s palsy. I know he has it. He knows he has it. In fact, he probably knows more about it than I do because he’s done so much research on the Internet. There’s really no treatment for it. We both know that, and it started me thinking, ‘Why is he coming to see me?’ So I asked him. He said, ‘Because I need to know how this is going to affect my life and I need you to help me figure that out.’ That’s what family doctors do. Technology really can help us build a better relationship with our patients.”
While technology may be helpful in many ways, the struggle to implement and adapt to new technologies is currently increasing physicians’ burdens, according to Douglas E. Henley, MD, AAFP executive vice president: “In the long run, technology is a very good thing. Technologies like e-mail and electronic medical records systems are going to help us work smarter, not harder. But what’s hurting us right now is that we’ve been so slow to adapt to it, so it’s adding frustration.”
Student interest is declining
Students haven’t been immune to the frustration within the specialty. During the early 1990s, student interest in family practice thrived as managed care organizations competed for family physicians, driving up their salaries and embracing them as the “gatekeepers” of the health care system. But as the managed care backlash grew in strength, and as family physicians became more and more identified with the much-maligned role of gatekeeper – ironically, a role most family physicians never liked in the first place – students watched the aftermath from front-row seats.
“We physicians are unsettled about the future, and it’s bleeding over into how we communicate the specialty,” Pugno admits. “As a practicing physician, you can feel really good inside about the kinds of things you do for your patients, but if you just hung up the phone after a frustrating conversation with a Medicare representative and some students walk into your office, they’re probably going to hear about that. And because students don’t yet have a clear picture of family practice, they can’t really balance a comment like that.”
Long hours, low reimbursement and high medical school debt don’t add to the specialty’s appeal, and students have begun to turn to other specialties that provide better pay and more control over lifestyle choices.
“We’ve let the hassles of managed care – which are very real – overshadow the immense satisfaction that we receive from being in direct contact with our patients,” says Avant. “We’ve somehow got to change that.”
Physicians are frustrated
According to the 2001 AAFP Member Attitude Survey, 95 percent of Academy members feel that outside regulations and rules are making it more and more difficult to practice. And 83 percent surveyed agreed that “adequate systems within my practice to handle paperwork would relieve some of my frustrations with the practice of medicine.” But discussion at the Keystone conference revealed that frustration runs deeper than complaints about low reimbursement and managed care hassles.
One of the goals of Keystone was to unite members of the founding generation (Generation 1), the first wave of residency-trained physicians (Generation 2) and the emerging generation of family physicians (Generation 3) for an intergenerational sharing of ideas and concerns.
“One of the feelings I left Keystone with, is that Generation 2 – my friends and myself – are the most frustrated,” Phillips says. “We’re still out there working hard. We’ve, by and large, been successful in our practices and we’re frustrated because we proved that the model of family practice that our founders envisioned works. Yet somehow it’s not seen as enough by people around us. A lot of people in my region, the Pacific Northwest, work in salaried environments. Every week, administrators come in and tell them, ‘We’re losing money.’ No one ever comes in and says, ‘You did a good job with Mrs. Jones’ or ‘We think our breast cancer rates are lower because of your commitment to prevention.’ We are bumping into people and systems that don’t really understand or care about the value of a family physician. And that’s frustrating.”
At the same time, younger physicians are somewhat frustrated with the model of family practice that has been handed down to them: “I think I can speak for Generation 3 when I say I’m thankful to Generation 1 and Generation 2 for the struggles they went through to establish family practice as an academic discipline and to get us board certification,” says Steyer. “We respect them. We believe in the same core values they do, but I think we struggle with their assertion that the traditional model of family physician is the model. In the traditional model, being a family doctor means having to be in your office and being a doctor all the time. Teaching or doing advocacy or public policy or whatever else is done on the side. We see the family physician in a wider variety of roles. Some of us have chosen to go into academics or research or public policy or part-time practice, and we still consider ourselves ‘real’ family doctors. Some members of the other generations seem to question that.”
The public is frustrated
“The public has been unhappy with the health care system for a long time,” says Green. “They’ve felt like they’re not getting what they need and what they are getting isn’t very satisfying. And since family practice is positioned squarely between the public and the rest of medicine, it’s no wonder that family physicians are early observers of it.”
Access to health information on the Internet has helped to create a public that’s better educated and more proactive about their health care. And just as public need helped to create family practice 30 years ago, public need is once again affecting the health care system. Aging baby boomers are demanding easier access and better service. And in some instances, they’re getting it.
“There’s no doubt in anyone’s mind that we’ve got a consumer-driven health care system,” says Henley. “The question now becomes how do we as a specialty identify and meet the public’s wants, needs and expectations?”
Pugno believes family medicine’s core values are what the public really wants and needs, “even though significant portions of them don’t know yet that they want and need them,” he says. “We’re on the right track. It’s just a matter of increasing our visibility.”
Increasing visibility may be a bigger task than the specialty ever imagined. “My own husband didn’t realize that family physicians are recertified every seven years,” says McPherson. “The public doesn’t know we were the first group and, for some time, the only group required to take a proctored exam for recertification. They don’t know that when they take their child to the pediatrician, that pediatrician was certified at one point but may or may not have been recertified since he or she finished residency. Maybe that’s where family practice really needs to change. We’ve done a good job at what we do, and I think we’ve always believed that by virtue of that people will recognize us, but that really hasn’t happened to the extent we’d like.”
An action-packed future
Given all the concerns present in the specialty today, the big question is “Is anyone going to roll up their sleeves and do something?” Actually, work has already begun:
• The AAFP has commissioned the University of Arizona to conduct a study to assess the factors associated with declining student interest in family practice. Preliminary results are expected shortly.
• The Society of Teachers of Family Medicine is currently under contract with the Health Resources and Services Administration’s Bureau of Health Professions Division of Medicine and Dentistry to examine the medical school curriculum and identify new competencies so that family physicians will be better prepared to meet future public health care needs. A family medicine curriculum resource manual will also be developed.
• Last February, in response to member concerns, the Academy launched a national public awareness campaign to build recognition and respect for the specialty. Advertisements with the tag line “Our doctor is a specialist in us” run regularly in USA Today and the Washington Post and during National Public Radio’s top news programs, “Morning Edition” and “All Things Considered,” of which the Academy is a current sponsor. While the campaign was created to make sure that policymakers and elected officials know about family physicians and their vital role in the health care system, consumers are noticing.
• This spring, leaders of the seven national family practice organizations that convened Keystone III got together again to determine how best to respond to the specialty’s concerns. They’ve created an initiative called the Future of Family Medicine Project. While still in its infancy at press time, the project is intended to provide direction to the specialty with regard to its educational programs, research enterprise, clinical care and business practices. According to Henley, it will also offer tools to help get family physicians to where they need to go. “This re-examination of the discipline is not occurring because all of a sudden there’s a feeling that family practice is outdated or losing its value,” he says. “It’s coming from a proactive perspective, a sense that the specialty needs to listen and to better respond to our patients’ wants, needs and expectations concerning their health care.”
One of the first steps of the initiative will be to survey the public to determine exactly what they want, need and expect from physicians. “This may represent the first time that any specialty organization has gone directly to the public to ask them about what they value,” says Henley, who is chairing the project. “Once we understand that, we can respond in a way that’s more evidence-based, more efficient for the practicing physician and more enjoyable for both the patient and the physician. And we need to incorporate technology into the process so that we work smarter, not harder.”
Avant, who’s also working on the project, says, “I wish we had something great to give the specialty right now, but maybe just the understanding and the hope that things are changing and that we’re trying to do what’s best to support them will help. Family physicians have had a tough, tough time and they do an excellent job. They need to be recognized for that.”