Your work is worth more than you think. You just need to document and code it better.

Family physicians lose perhaps 10 percent to 20 percent of reimbursement each year because of incorrect coding. The problem is not that we aren’t doing enough work. It’s that we aren’t properly documenting and coding the work we do.
For this reason, it’s important to take the time to study the CPT manual and the documentation guidelines for evaluation and management (E/M) services. You probably use 25 codes for about 95 percent of the visits you do every day, so it’s especially important to be familiar with those codes and the documentation guidelines that apply to them. For the typical family physician, 80 percent of visits are established patient office visits, which involve five codes (99211–99215); 10 percent are new patient office visits, which involve five more codes (99201–99205); and 5 percent are hospital visits, which involve 15 codes (99217–99239). The other 5 percent of the visits will involve any number of codes for procedures, lab, etc. Carefully studying these codes once isn’t enough. You’ll need to order an updated CPT manual each year and review it to find the new, revised and deleted codes. For family physicians, it’s particularly important to study the first 30 pages or so, which cover the E/M services, and to look at the laboratory and immunization codes, which frequently change from year to year.
In this article, I’ll review the general criteria for selecting a level of E/M service and then explain how you can use those and other criteria to ensure that you are properly coding and documenting for the services you do every day. Remember: You are responsible for correct CPT coding – not your nurse, not your office assistant, not your front-office staff, not your insurance staff. Nobody can code correctly but the physician or other provider who’s interacting with the patient. If you are allowing someone on your staff to code for you, whether it be for office visits or hospital visits, you are setting yourself up for lost income or trouble in an audit or both.
KEY POINTS
- If you don’t personally have a good working knowledge of CPT coding, you may be foregoing 10 percent or more of your reimbursement.
- The 1997 documentation guidelines are tedious but well worth learning.
- Family physicians bill Medicare for too many 99212s and not enough 99211s and 99214s.
Selecting a level of E/M service
For now, while the future of the documentation guidelines is unclear (see “The status of the documentation guidelines”), the best course is to learn and use the 1997 guidelines. Although they are a bit more detailed and tedious than the 1995 guidelines, they are more objective and hence more useful in case of an audit. (For a copy of the 1997 guidelines, go to www.cms.gov/medlearn/emdoc.asp.)
The key components in selecting a level of E/M service for most categories of service include the history, examination and medical decision making. When selecting the appropriate E/M level of service for a visit, the number of key components required is not always the same. Generally, for new patient visits and initial care in a hospital or nursing facility, all three key components are required, while only two are required for subsequent care (see “Counting key components”).
Note also that the levels of service are not the same for new and established patients. For example, a level-IV new patient visit requires a comprehensive history and exam while a level-IV established patient visit requires a detailed history and exam. An established patient is one who has been seen by the physician – or, in a group practice, by a physician of the same specialty – for a professional service in the last three years, and a new patient is one who has not. For example, if a family physician colleague in your practice saw a patient a year ago and you’re seeing that patient now, the patient is established. But if it’s been more than three years since you or your colleagues provided the patient a professional service, which is defined by Medicare and CPT as face-to-face service, the patient is considered new. Even if you’ve had 20 phone contacts with the patient during that time period, it doesn’t count as a professional service because you did not see the patient face-to-face.
THE STATUS OF THE DOCUMENTATION GUIDELINES
The documentation guidelines as we know them are likely to change. Someday. The CPT Editorial Panel, which is the body charged with proposing a revised set of guidelines or replacing them entirely with a new system, appears to be working on a revamped set of descriptors for the evaluation and management CPT codes. They are also working on a greatly expanded collection of vignettes designed to depict situations in which the various codes would be appropriate. When, and even whether, this new system will be made final is uncertain. Changes certainly won’t take effect before 2004, and given the speed at which changes in the guidelines have taken place in the past, they may take longer to appear. In the meantime, there is plenty of reason to master the 1997 guidelines.
Typical office visits
The CPT codes used most commonly by family physicians are established patient office visit codes (99211–99215). Medicare data on the distribution of these codes for family physicians in 2000 is shown in the blue bars of the graph. I would suggest that the distribution shown by the red bars is more reasonable. We should be billing 99211 and 99214 about twice as often as we now do, and we should cut back on the other codes, especially 99212, which we should use about half as often. Here’s why:
99211. Consider this scenario: A patient comes into the office thinking she has an acute urinary tract infection, drops off a urine sample and leaves. Your nurse gives the patient instructions for leaving a urine sample, but the patient doesn’t see you. When UTI is confirmed, you have your nurse phone in a prescription, and she adds a note to the patient’s chart. Do you submit a claim? You should. That’s a 99211. A 99211 does not require a physician’s presence, and the presenting problems are usually very minimal. Every 99211 you fail to code is $10 to $18 you’re failing to collect. And the only documentation needed is a brief note saying why the patient was there and what happened.
You do have to use some common sense, though. You could take this to the extreme and code a 99211 every time you have a patient come in between four-month visits to have blood pressure checked. But you probably don’t want to do that, because it’s not very good public relations to charge for that every single time.
99212 and 99213. The CPT requirements for these two codes are shown side by side. As you can see, the difference between the two can be slight. If you don’t fully document the work you do in a visit, you’ll often end up coding 99212s for visits that are easily 99213s. For example, a four-year-old male presents with a fever and ear pain; you do a minimal exam and diagnose acute otitis media; the plan is straightforward. How many times do you see such a patient and document no more than this? It sounds like a 99212. But should it be a 99213? You’re likely getting into some ROS, so the problem-focused history becomes an expanded problem-focused history. (Actually, chances are you’re going even beyond that, asking about lymphadenopathy, cough and abdominal pain and perhaps about previous medications, but a brief HPI and a review of the affected system are all you need for an expanded problem-focused history.) And you’re probably also doing at least six elements in the exam –taking vital signs, making an assessment of appearance (e.g., ill, not ill, cachectic), looking at tympanic membranes, the external auditory canal and the oropharynx, and listening to the chest. Remember that three vital signs (e.g., weight, temperature and blood pressure) constitute one element, and your nurse does this before you even get there. The difference in reimbursement between 99212 and 99213 can be quite significant and requires doing just a little bit of additional documentation for work that you always do but rarely give yourself credit for.
COUNTING KEY COMPONENTS
The setting and nature of a visit determine whether two or three of the key components (history, exam and medical decision making) are required to establish the level of service.
| Setting | Three key components required | Two key components required |
|---|---|---|
| Office | New patient visit | Established patient visit |
| Consultation | ||
| Home or domiciliary facility | New patient visit | Established patient visit |
| Nursing home | Comprehensive assessment | Subsequent care |
| Hospital | Initial hospital care | Subsequent care |
| Initial inpatient consultation | Follow-up inpatient consultation | |
| Hospital observation services | ||
| Emergency department | All E/M services |
99214. A 99214 requires two of the following:
- Detailed history (an extended HPI, an extended ROS and one element of the PFSH),
- Detailed examination (at least 12 exam elements from at least two systems),
- Moderate-complexity medical decision making (two of the following: multiple diagnoses, moderate amount and complexity of data and moderate level of risk).
An extended HPI is four elements about the present illness or a statement about the status of three chronic active or inactive conditions. The extended ROS only takes a review of at least two systems. For pertinent PFSH, any single item applies, and you’re always going to ask about allergies and medications. For moderate-complexity medical decision making, “multiple” diagnoses means at least one new problem. And two or more ongoing chronic conditions or one chronic condition with acute exacerbation and prescription drug management each constitutes moderate risk.
Since 12 exam elements are required, history and medical decision making – not the exam – will often be what makes a visit a 99214. For example, let’s say you see a 60-year-old, non-Medicare patient for a routine, four-month follow-up visit. The patient has hypertension, type 2 diabetes and osteoarthritis and is stable. That’s automatically an extended HPI. You also note that the patient has no chest pain, no shortness of breath and no joint pain. So, you’ve touched on at least two systems relative to ROS. You’re automatically at moderate medical decision making because you’ve got three diagnoses and moderate risk. Since you can’t identify 12 elements of the examination, it’s not a detailed exam, but that doesn’t matter. Like all established patient office visit codes, 99214 requires only two of the three components. Of course, the exam may be clinically important for any number of reasons. But it’s not critical for the purpose of determining the code in this case.
Beware of 99215s. You shouldn’t be coding many 99215s because it is rare that an established patient will come in for a visit that requires a comprehensive history or a comprehensive examination – and a patient who does require these things is usually sick enough for hospital admission instead. 99215 is not the code to use for an annual physical examination. There’s a separate set of codes that relate to the annual physical examination. Be very cautious about using 99215 because of the issue of medical necessity and the audit process. It’s not worth the hassle.
AVERAGE AND RECOMMENDED CODE DISTRIBUTIONS
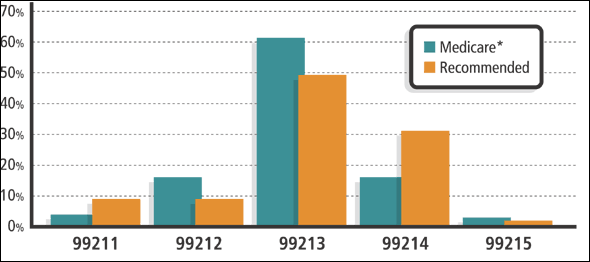
*Medicare Part B Physician/Supplier National Data, Calendar Year 2000, Evaluation and management codes. Available at: http://www.cms.gov/statistics/feeforservice/emcd00xls.zip. Accessed Dec. 6, 2002.
Other coding and documentation pearls
Following are some other coding and documentation basics you need to know to increase the reimbursement you receive for the care you provide in the office and the hospital:
Coding and time. Generally, the amount of time you spend with patients is much more important for the quality of care than it is for coding purposes. You should focus instead on how you take a history, what type of history you perform, what type of exam you perform and what degree of medical decision making is involved. That said, there are situations, such as with counseling and coordination of care, in which time counts for coding purposes. If you counsel or coordinate care with a patient or the patient’s family for more than 50 percent of the time you spend in the office visit and document it accordingly (i.e., document the total visit time, the total time spent counseling and the nature of the counseling or other activities), the level of service can be determined from the total time. When you’re in the office, the time that counts is face-to-face time. When you’re in the hospital or the nursing home, the time that counts is the time you spend on the floor reviewing the medical record, talking to the nurse and spending time with the patient or the family.
Say an elderly patient whom you’ve been seeing for 15 years comes into the office with dementia and brings a family member. After five minutes of reviewing the history, performing an exam and talking about medications, you enter into a 20-minute discussion with the family member about coordination of care in the home and coping with dementia. If you don’t take the 20-minute conversation into account and instead code only based on the limited encounter or limited history and exam, the visit may just be a 99212 or 99213. But, according to CPT, since the 20 minutes you spent counseling and coordinating care with the family member made it a 25-minute visit and 20 out of 25 minutes is more than 50 percent of the visit, it automatically becomes a 99214. Although you may want to document a SOAP note for the visit to remind yourself or a partner about it for next time, it’s not necessary for coding purposes in this case.
THE FINE LINE BETWEEN 99212 AND 99213
When you look closely, the requirements for 99213 are low enough that 99212s should be fairly rare.
| Key elements (2 of 3 required) | 99212 | 99213 | The margin of difference |
|---|---|---|---|
| History | 1–3 HPI elements | 1–3 HPI elements Review of affected system | Review of 1 system |
| Examination | 1–5 elements | 6–11 elements | 1 or more exam elements |
| Decision making | 1 self-limited or minor problem | 2 self-limited or minor problems or 1 new problem plus low risk (e.g. OTC medication) | 1 problem and, for instance, OTC medication |
Keep in mind that counseling for E/M services involves a discussion with the patient or family about one or more of the following: diagnostic results or recommended tests, prognosis, risks/benefits of treatment, instruction for management or follow-up, importance of compliance, or risk factor reduction/patient education. It does not include psychotherapy. For that, you would use the time-based psychotherapy codes (90804–90857).
Consultations. Although family physicians do a lot of consultations, they don’t code for a lot of consultations. And consultations generally pay much higher than routine office visits and routine initial hospital care codes or subsequent hospital care codes. Any request you receive, either written or verbal, from another health care professional to see a patient, assess a patient or engage in treatment of a patient and to return a report constitutes a request for a consultation and must be documented in your note if you wish to code it as such. According to CPT, although consultations can be requested by a non-physician health care provider, such as a psychologist, they must be performed and recorded in the note by a physician. If you’re performing the consultation in your office, you must also send a letter back to the person who requested the consult. Consults may occur anywhere in the outpatient or inpatient setting, and there are separate codes for each setting (99241–99245 for office or outpatient consultations and 99251–99255 for initial inpatient consultations).
Prolonged services. CPT’s prolonged services codes (99354–99359) can be used when the time you spent providing a service is beyond the usual time for that service. The time can be face-to-face time or time before or after face-to-face time:
- For face-to-face time in the office, use 99354 for the first 30–74 minutes of prolonged service and 99355 for each additional 30 minutes. An example of this would be a child with acute asthma who does not require hospitalization.
- For face-to-face time in the hospital, use 99356 for the first 30–74 minutes and 99357 for each additional 30 minutes. An example of this would be maternal/fetal monitoring for a high-risk delivery.
- For prolonged services without face-to-face contact, use 99358 (30–74 minutes) and 99359 (each additional 30 minutes). These last two codes should only be used rarely – when, for example, review of very extensive medical records or prolonged communication with other professionals is necessary.
These codes can be submitted in addition to the visit code without attaching a modifier. Medicare won’t reimburse for them, but other insurers may.
The “Medicare physical.” Most clinical guidelines indicate that Medicare patients should have an annual “update” physical at least every 18 months, depending on how ill they are. But the annual physical is a service not covered by Medicare, which means it has nothing to do with the Medicare fee schedule. Therefore, if you code for it properly, you can charge your Medicare patients what you would normally charge your non-Medicare patients for a physical exam. However, most family physicians don’t code this correctly. Many use 99215, which doesn’t represent this type of visit, or the preventive medicine services code 99397, which is correct but probably not complete, since Medicare patients almost always have multiple chronic conditions that need follow-up at the same visit. Instead, you should almost always submit a preventive medicine services code and 99214 (or 99213, whichever code would apply to the visit if the patient had not also come in for the physical) with modifier -25 appended to show that the 99214 service was significant and separately identifiable from the preventive medicine service.
Here’s how the reimbursement works: For simplicity, let’s say the Medicare fee schedule is $50 for a 99214 under most usual circumstances and you charge $100 for an annual physical. Say your visit with the patient justifies coding 99397 for the physical and 99214–25 for following up on his chronic conditions. You should automatically collect $50 from the patient when he checks out (i.e., the difference between the Medicare fee schedule amount for the 99214 and your normal charge for a physical). Then submit a claim to Medicare for the $50 that applies to the 99214 service. If the patient hasn’t met his Medicare deductible, you’ll have to collect the other $50 from the patient as well. However, if the patient has met his deductible, Medicare will pay 80 percent of the $50 claim you submit ($40), and the patient will pay 20 percent of the claim ($10). With the $60 you collect from the patient and the $40 Medicare will send you, you’ll collect your $100 annual-physical fee.
Concurrent care. Family physicians often deal with concurrent care (primarily when providing subsequent hospital care), which occurs when similar E/M services are provided by two physicians on the same date. For example, if a 50-year-old male comes in with an acute myocardial infarction and you admit the patient to the critical care unit on that first day, you’ll submit either a critical care code or an initial hospital care code and, on subsequent days, a subsequent hospital care code. You’ll probably also consult a cardiologist, who will code for an initial consultation in the hospital and, each day after that, a subsequent hospital care code. So now you’ve got two physicians both coding for subsequent hospital care of a patient with an acute MI. What happens when you send your claim to the payer? Whoever gets it there first will get paid. It’s as simple as that. To make sure your claim gets there first, call your office from the hospital immediately or do it first thing in the morning. Tell your insurance office to electronically submit a claim that day for that service.
Hospital observation services. For these services, there are a number of different coding scenarios to be aware of (in all cases, keep in mind that your code selection should be based on the dates of service, and the date changes at midnight):
- If you admit a patient to observation status in the hospital, use the initial observation care codes (99218–99220) instead of the initial hospital care codes (99221–99223).
- If the patient is discharged on the next date, even if it’s 12:01 a.m., use 99217 for observation care discharge instead of a hospital discharge code (99238 or 99239).
- If you admit a patient to observation at 7:00 a.m. and discharge him from observation at 5:00 p.m., use 99234–99236 for “observation or inpatient care services (including admission and discharge services).”
- Once a patient is formally admitted to inpatient status, you should use the initial hospital care codes or the subsequent hospital care codes (99231–99233) instead of the observation care codes. However, if you admit the patient to observation on Monday and then admit her to the hospital on Tuesday, you have two options. On Tuesday, you can submit a subsequent hospital care code if you think that most applies to what you’ve done to the patient that day, or you can submit an initial hospital care code, even though you submitted an initial hospital observation care code on Monday. But if you choose the latter, all three key components must be met, which requires you to address history, exam and medical decision making. A subsequent hospital care code would only require two out of three.
- If you see a patient in the office and admit him directly to observation in the hospital, you should submit only an initial observation care code for that encounter. However, if you see the patient in the office in the morning, send him home and then end up admitting him for observation later that day, you can submit an office visit code and an initial observation care code. You may want to use the -25 modifier and explain the situation to the payer.
Hospital discharge services. There are two time-based codes for hospital discharge services (99238 for 30 minutes or less and 99239 for more than 30 minutes). These codes relate to the entire amount of time you spend working on a patient’s eventual discharge before she leaves the hospital. This includes working with discharge planners, nurses and the home health agency, and planning with the family what to do at home.
If you discharge a patient and admit her to a nursing facility on the same day, you can charge for both services, even if you don’t see the patient in the nursing facility that day. Just make sure the patient’s record goes with her to the nursing facility so that it’s documented that you did the history and physical within the last several days, that you did the discharge summary that day and that you have met the requirements of the initial nursing facility assessment code (99303).
Critical care services. For critical care, there are also two time-based codes (99291 for the first hour and 99292 for each additional 30 minutes). (When you read the CPT manual carefully, you’ll find that the first “hour” is really the first 30 to 74 minutes of critical care.) Critical care, which is reimbursed at a much higher rate than an initial hospital care code, requires constant attention. You have to be with the patient the whole time – at the bedside or in the unit working with the nurses on that patient’s care. You can’t be spending time with other patients.
You can code for subsequent hospital care and critical care on the same day if, for example, you see a patient for a routine hospital visit in the morning, he crashes later on and you return for critical care in the afternoon. To ensure that you get paid for both services, send a letter (even a form letter) to your Medicare carrier or your insurance company to explain what happened. And remember, if more than one physician is providing critical care (e.g., the patient goes into cardiogenic shock and has arrhythmia in the critical care unit while you’re there with the cardiologist), submit your claim that day to avoid problems with concurrent care.
Emergency department (ED) services. ED services codes (99281–99285) apply to new or established patients. Whatever you do in the ED requires all three key components, so you should treat all patients just like new patients even if they are established patients. If you’re the only physician involved in the ED care, simply charge the ED visit codes. But if a patient of yours has gone to the ED and you’re called in to see her by the ED physician, you’ve got a decision to make. If you admit the patient, you should use the initial hospital care or observation codes. If you send the patient home after performing a consultation, you should document the consultation request in the record and use the appropriate consultation codes.
It’s up to you
Correct CPT coding can have a significant impact on reimbursement. As a physician, you, not your staff, must take control of this. Though staying up-to-date on changes to the codes and guidelines can be time-consuming and tedious, it’s well worth your time to prevent fraud-and-abuse concerns and code correctly so that you can be properly reimbursed for the work you do.

