A simple medication list updated at each visit can prevent errors – and make your job easier.
Medication errors, such as prescribing contraindicated medicines or prescribing the wrong medicine dose, are the number one source of error in family practices in the United States.1 A number of these errors could be prevented if patients’ medication records were more accurate, up-to-date and accessible; however, maintaining such records is a challenge. Patients change their medications frequently, often visit more than one physician and use undocumented over-the-counter medications.
One of the best methods available for managing patients’ medication data is a simple medication list displayed in each patient’s chart and updated at each visit. The list quickly conveys all medications the patient is currently taking, all past medications and the exact combination of medications being taken at the time of each patient visit. If used properly, the medication list can become a vital part of the chart and make the physician’s job much easier. More important, it can help physicians provide higher quality care and minimize medication errors and adverse drug interactions.
How to get started
The first step in developing a medication list is for all the physicians in your office to agree on the need for careful medication monitoring and then to express this concern to the entire office staff. Having their support will make it easier to tackle the details, such as deciding how your medication list should be organized and printed and who will be involved in updating the form. Your receptionist can help by reminding patients to bring all of their medication bottles to each visit for review. And your nurse or medical assistant can help with updating the forms during each visit. You will want to remain closely involved in the medication review process as well.
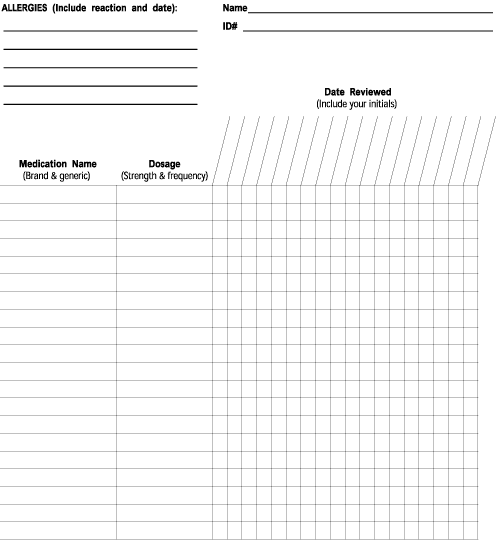
In designing your medication list, choose whatever format is most workable for your group. A copy of the medication list I use in my office can be viewed and downloaded below. I recommend that the medication list be used for all chronic medications, with acute medications recorded elsewhere in the chart (e.g., in the progress note for each visit).
To use the sample form, interview each patient at each visit regarding all medications he or she is currently using. Commonly overlooked medications include birth control pills, inhalers, eye drops, patches, herbal medicines and medications prescribed by other physicians. As you gather this information, write each drug’s brand name, generic name, strength and frequency in the appropriate fields, listing one drug per row. Then, write the current date in the “Date Reviewed” section and place a check mark in the appropriate box next to each medication to indicate that it was reviewed on that date. Finally, place your initials next to the current date.
At subsequent visits, if the patient indicates that he or she is still taking a certain medication, simply place a check mark in the box under the current date and initial that column. If a medication has changed in dosage, mark the old entry as discontinued (by writing “Discontinued [date] because of dosage change” immediately to the right of the last checked box) and start a new entry for the new dosage. If a medication is no longer being taken, mark that entry as discontinued as well. The old entry should not be used again even in the event that the medication is restarted at a later time. If the medication is restarted, create a new entry on a new line. Avoid crossing out a medication name or dosage or in any way modifying information previously entered on the medication list. Such markings will make it difficult to understand the patient’s medication history and identify when changes were made.
When deciding on the appearance of your medication list, choice of paper is important. Paper of 60-pound weight is recommended, as it is durable and extends the effective lifetime of the form. Printing on both the front and back of the form will also allow you to use it longer and will help minimize the thickness of your charts.
MEDICATION LIST
Simple tool; countless benefits
With consistent and proper use, a simple medication list can become a very powerful part of the chart providing countless benefits, such as the following:
Efficient charting. Because the medication list can be updated via a few check marks, it makes documentation quicker and easier. Reviewing it at each visit requires less time than documenting each medication in the progress note. The physician can simply refer to the medication list in the note (“the medication list is reviewed today with the patient”), thus saving time and money in dictation costs.
Safer refills. When patients require prescription refills, the medication list makes it easy to check that the patient is receiving the correct prescription. Physicians and nurses do not have to search through pages of progress notes, as the information is clearly displayed at the front of the chart.
Communication with other physicians. The medication list can easily be photocopied and sent to other doctors involved in the patient’s care so they can see the patient’s medication history. This improved information-sharing between physicians can prevent dangerous medication errors.
Information recall. A patient’s medication list is often a snapshot of his or her medical history. Reviewing the medication list with the patient helps the physician recall past treatments. This is particularly helpful when a patient presents with a recurring problem.
Allergy documentation. Ideally, allergies should be documented in one place in the chart. What better place than the medication list? The allergy list should describe the reaction and include the date.
An effectively maintained medication list makes practicing medicine easier and more enjoyable and can facilitate improvements in the quality of patient care. Is it time to change the way you document medications?


