
As part of the Future of Family Medicine project, the specialty put itself under a glaring spotlight to see where it currently stands.
Fam Pract Manag. 2003;10(10):43-47
In 2001, recognizing the need to take action to transform and renew the specialty, leaders of the seven family medicine organizations together initiated the Future of Family Medicine project. As a first step, the project leaders hired a national market research firm to provide them with an objective understanding of the current state of family medicine. The research produced a wealth of interesting and sometimes eye-opening findings and engendered a great deal of reflection and debate among those involved with the project. It also identified several key challenges that lie ahead for the specialty. With the work of the Future of Family Medicine project now complete and the final report forthcoming this spring, we thought you’d like to know what the public and other physicians had to say about family doctors.
Tough questions, honest answers
“I think many family physicians share the same anxieties and concerns,” says Richard Roberts, MD, JD, a past president of the AAFP who chaired one of the Future of Family Medicine project task forces. “For example, do patients know what I do? Do they value it and respect it? Do other clinicians know what I do? Do they value it and respect it? These were just some of the questions we needed answered at the outset of the project.” (To learn more about the Future of Family Medicine project, see page 46.)
Other specialties that have undertaken efforts similar to the Future of Family Medicine project have looked inward for answers, but doing market research seemed the most logical approach for family medicine. “Of the 25 major specialties, only family medicine was created out of social need. Choosing to do market research reflects our origins,” says Norman Kahn, MD, the AAFP staff executive for the project. “The approach was a bit risky,” says James Martin, MD, AAFP board chair and chair of the Future of Family Medicine project leadership committee. “We had to prepare ourselves to get answers we might not really want to hear.”
In all, nearly 2,000 interviews were conducted with, among others, patients of family physicians, patients of other specialists, practicing family physicians, academic family physicians, medical students, residents, other specialists and non-physician providers (for more information, see “About the research”).
ABOUT THE RESEARCH
To determine public perception toward family medicine, Roper ASW conducted more than 1,000 telephone surveys using a national random-digit sampling of the general public. Greenfield conducted 13 focus groups with patients, including those from a variety of geographic and ethnic backgrounds, those who were chronically ill, those who had a family physician, those who did not and parents of children 17 years and under.
To determine how family physicians and other specialists perceived family medicine, 17 focus groups and approximately 700 telephone surveys were conducted using AAFP and AMA samplings of practicing family physicians, academic family physicians, non-FP specialists, medical students, family medicine residents and residents in other specialties. The interviews were conducted during June and July 2002. Siegel & Gale (formerly Siegelgale) then analyzed the Roper and Greenfield findings. A portion of the market research findings are available at http://www.futurefamilymed.org/x19431.html.
The good news
“We could have learned that what family physicians do is unwanted, unnecessary and irrelevant,” Martin says. “What we learned was quite the contrary: From multiple perspectives, there is still need and desire for family physicians.”
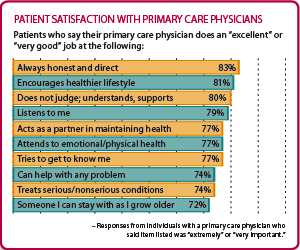
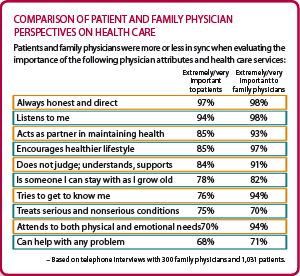
Even though patients and physicians are frustrated by the health care system, the research showed that patients seem to want the same things family physicians want to deliver. According to the research, the primary drivers of patient satisfaction include having a physician who listens, is nonjudgmental, honest and direct and who encourages a healthy life style (see “Patient satisfaction with primary care physicians”). More than 80 percent of patients and more than 90 percent of family physicians said that these were “extremely” or “very” important physician attributes (see “Comparison of patient and family physician perspectives on health care”).
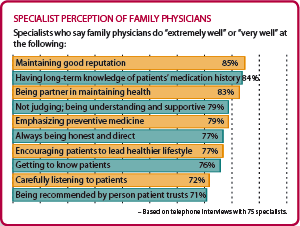
“The research findings also confirm there is support for family medicine within the medical profession, particularly among community-based sub-specialists,” says Larry Green, MD, director of the Robert Graham Center for Policy Studies in Family Practice and Primary Care and chair of one of the Future of Family Medicine project task forces. More than 80 percent of non-FP specialists surveyed said that family physicians do “well” or “extremely well” at maintaining a good reputation, knowing patients’ history and acting as a health care partner (see “Specialist perception of family physicians”).
Many specialists saw family physicians and general internists as equal on a number of performance measures. Those who saw a difference thought family physicians perform better in these areas: their concern with doctor/patient relationships, the ease with which patients can relate to them and their responsiveness to patients’ concerns. As one specialist explained, “Family doctors have better communication skills. They tend to translate medical terms to human terms. Internists tend to use more Latin words in their interactions with patients, where family doctors talk to patients in their own language.”
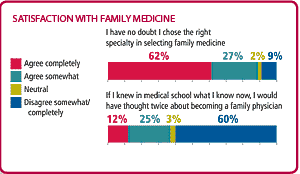
The research also showed that the family physicians surveyed are happy in their practices. Almost 75 percent said they felt the specialty gives them the opportunity to use their full range of skills. Sixty-two percent reported having no doubt that they chose the right specialty (see “Satisfaction with family medicine”). And about three-fourths said they would also be “very likely” or “fairly likely” to recommend family medicine to medical students; the most common reasons were for the satisfaction and variety it brings.
The other side of the coin
The research also suggested that while many people value the attributes of family medicine, some don’t really know what family medicine is. For example, one-third of patients whose primary care provider is a family physician aren’t aware they’re going to a family physician. Moreover, when asked to identify primary care specialists, only one in 10 patients named family physicians. And, as those responses might lead you to expect, patients in the focus groups weren’t aware of the unique training and mandatory recertification the specialty demands. According to one patient, “Everyone is a general practitioner or family doctor first and then they specialize.”
While many of family medicine’s core attributes are valued, the research also showed pockets of skepticism, particularly about comprehensive care. Although almost three-fourths of patients surveyed like the idea of having someone who could care for the majority of their basic needs, approximately one-third strongly agreed with the statement “These days it is impossible for an individual doctor to have adequate knowledge of all treatments.” Some were concerned that trying to do it all could result in a physician who was a jack-of-all-trades and master of none. Keeping up-to-date with so much medical information “asks way too much of a person,” one patient said. “They’ll be overworked.”
While patients appreciate family physicians for what one described as “their human being care versus health care” approach to medicine, they also value the use of technology in medicine. Seventy-three percent of patients with a primary care physician said that state-of-the-art equipment was “extremely” or “very” important to them. If focus group discussions are an indication, patients don’t seem to find enough technology in family physicians’ offices. “They’re more like the old-fashioned Norman Rockwell doctor,” one said.
Patients are also practical. While they want to have a personal physician, someone to coordinate their care and someone with whom they can have a good relationship, 24 percent said they base their choice of physician on location and 22 percent said they base it on whether the physician is on their insurance plan. Availability is also key. “Even if he’s the greatest doctor in the world, it doesn’t matter if you can’t get in to see him,” one patient said.
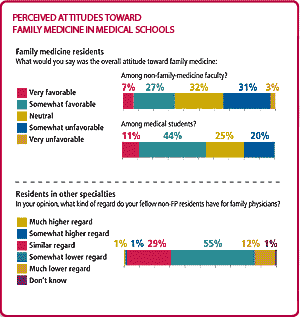
The research findings also confirmed what most, if not all, family physicians already know: Family medicine does not have strong support in academic settings. Thirty-four percent of family medicine residents surveyed reported that non-family-medicine faculty have a “somewhat unfavorable” or “very unfavorable” attitude toward the specialty (see “Perceived attitudes toward family medicine in medical schools”). They attributed the negative attitudes to their perceptions that family medicine was looked down on by other specialties, that students who choose family medicine were not as smart and that the specialty required less training and competence. Sixty-seven percent of non-FP residents responded that their fellow non-FP residents had a “somewhat lower” or “much lower” regard for family physicians than for other primary care physicians. They cited “too much to cover” and “not enough in-depth training” as the primary drawbacks to going into family medicine. “It’s easier to be the best in a very specific field,” one resident explained. “I don’t know if I could be the best family doctor. And even if I were, would people care?”
Medical students were also concerned about the extensive knowledge base required of family physicians and put income at the top of the list of drawbacks for going into family medicine today.
THE FUTURE OF FAMILY MEDICINE PROJECT
Several years ago, realizing that something had to be done if the specialty was going to remain healthy, leaders of seven family medicine organizations together initiated the Future of Family Medicine project (FFM), charging it with a tremendous task:
“To develop a strategy to transform and renew the specialty of family medicine to meet the needs of people and society in a changing environment.”
The organizations behind this landmark effort include the AAFP, the American Academy of Family Physicians Foundation, the American Board of Family Practice, the Association of the Departments of Family Medicine, the Association of Family Practice Residency Directors, the North American Primary Care Research Group and the Society of Teachers of Family Medicine. The FFM project is a collaborative effort. One elected leader and the CEO from each of the seven organizations sit on the project leadership committee (PLC), which manages the project.
Phase one: Questions
In 2002, the FFM project leaders hired Siegel & Gale (formerly Siegelgale), a national strategic branding consulting firm based in New York City, to develop an objective understanding of the current state of family medicine in the United States. In all, nearly 2,000 interviews and 30 focus groups were conducted (see “About the research”). Those findings as well as Siegel & Gale’s analysis and recommendations were provided to five project task forces, each of which sought to answer a critical question:
Task Force 1: What are the core attributes of family practice, how can family practice best meet people’s expectations and what systems of care should be delivered by the specialty?
Task Force 2: What are the training needs for family physicians to deliver the core attributes and services expected by people and the health care delivery system?
Task Force 3: How can we ensure that family physicians continue to deliver the core attributes of family practice and the services the system expects throughout their careers?
Task Force 4: What strategies should be employed to communicate the role of family physicians within medicine and health care, as well as to payers and patients?
Task Force 5: What is family practice’s leadership role in shaping the future health care delivery system?
The realization that reimbursement models must be developed to sustain and promote family practice led the project leadership committee to add a sixth task force and charge it with addressing reimbursement and financial issues.
Phase two: Answers
Late this summer, the five original task forces submitted their findings and recommendations to the project leadership committee. The committee then reviewed the recommendations and presented a summary report to the leaders of the seven family medicine organizations. The recommendations from the sixth task force are expected in early 2004. At press time, the summary report was being reviewed for approval by the boards of directors of the seven organizations.
Phase three: Implementation
The implementation phase of the FFM project will begin with publication of the project’s final report in the March/April issue of the Annals of Family Medicine (http://www.annfammed.org). The final recommendations will also be summarized in an upcoming issue of FPM. The data collected as part of the project will be made available for future study and will be maintained at the Robert Graham Center for Policy Studies in Family Practice and Primary Care in Washington, D.C. (https://www.graham-center.org). More information on the Future of Family Medicine project can be found at http://www.futurefamilymed.org.
Key challenges
With the market research in hand, the researchers analyzed the findings and identified five challenges influencing family medicine’s ability to maintain viability in the U.S. health care system:
Promoting a more accurate and widely held under standing of the specialty among the public.
Focusing on communicating and delivering what people can expect in a specialty that has a wide scope and variance in practice type.
Winning respect for the specialty in academic circles.
Making family medicine a more attractive career option.
Dealing with the public’s perception that family medicine is not solidly grounded in science and technology.
The Future of Family Medicine project’s final report will be published in the March/April issue of the Annals of Family Medicine (http://www.annfammed.org). It will provide a re-articulated vision of the specialty and numerous recommendations for bringing about changes within the discipline, including methods of health care delivery that will better meet public expectations. The final recommendations will be summarized in an upcoming issue of FPM.
“I think family physicians are going to need to buy into the six aims outlined in the [Institute of Medicine’s] Crossing the Quality Chasm1 report,” Martin says. “We are going to have to set up new systems that provide safe, timely, efficient, effective, equitable and patient-centered care to patients.” Two ways to accomplish this will be to bring more science and technology into the physician office and provide patients with better service.
“When we talk about service, we aren’t only talking about having open appointments,” Kahn says. “It means offering patients a basket of services so they know exactly what to expect when they walk through the door of a family physician’s office. We have to do a better job of communicating how we will deliver what people expect.” He points to quality as another component of service. “We want to provide patients with a medical home, a similar goal to that of the specialty of pediatrics. We want people to think of a family practice as somewhere they can safely go to get what they need.” Along with a new model of practice, the report will also offer recommendations for revisions in residency training programs and new approaches to lifelong learning that will enable family physicians to continue to deliver the core attributes of family medicine throughout their careers.
Yet the project leaders also realize that little can be accomplished without some fundamental changes in the U.S. health care system, specifically in reimbursement and financing mechanisms. “The current system doesn’t allow family physicians to do what they want with their practices,” Martin says. “Sure they want to idealize their practices and bring in electronic health records, but they can’t do that if we don’t develop reimbursement models that sustain and promote what they do. Skeptics have already said, ‘Show me the money.’ We’re working on it. Right now, what we’re hearing from payers is that if we can do what we say, they’ll come on board.”
Next steps
If all goes as planned, the Future of Family Medicine report should usher in a period of active experimentation within the specialty. “It will be an ongoing process over the next five to 10 years,” Roberts says. “As a result, I think you’ll see changes in daily work flows, changes in how doctors group themselves, more training in systems care and more use of technology, among other things.” It may also serve to reconnect both physicians and patients to the specialty. “In 10 years, I think it will be viewed as a potentially landmark report,” says Larry Green. “Something that punctuated the next major transition for family medicine in the United States.”