
Your peers have been coding more 99214s. Is it time to review your coding habits?
Fam Pract Manag. 2007;14(4):39-43
Betsy Nicoletti is the author of The Field Guide to Physician Coding and is a speaker and consultant with expertise in coding, billing and accounts receivable. She lives in Springfield, Vt. Author disclosure: nothing to disclose.
When you decided to become a family physician, you likely made your choice because you wanted to provide excellent care to a diverse group of patients – not because you wanted to become an expert in Current Procedural Terminology. However, in today's health care environment, accurate coding is critical for reducing your audit risk and claiming the reimbursement you deserve.
How do you know whether you have good coding habits? Two important exercises will help you to answer this question and target areas where you need to improve. The first exercise is to analyze your coding on a macro level by comparing it to normative data, including specialty-specific evaluation and management (E/M) coding distributions and a list of the codes billed most frequently by family physicians. The second exercise is to audit a sample of charts to ensure that your coding accurately reflects the services you documented. This article will provide information and tools to help you perform these analyses.
Comparing your coding pattern to benchmarks
To assess your coding habits, you'll need to create your own coding profile. To begin, you'll need a breakdown of the codes you reported during a specified period of time and the number of times you reported each one. Most computerized billing systems can produce a report that includes this data.
E/M coding distribution. You can use the information in this report to calculate your E/M coding distribution (e.g., the percentage of your established patient office visits that were level-III, level-IV and so on) and compare it with the norm.
Medicare benchmark data is available from the Centers for Medicare & Medicaid Services (CMS), which publishes the number of E/M services physicians reported by specialty (see the box). Although this data represents only the Medicare portion of your patient population, it is the most comprehensive data available at this time.
I've used the latest Medicare data to calculate coding distributions across service categories, as shown in the graphs. You can compare your coding distribution to these Medicare norms by using a spreadsheet like the one shown in "E/M coding profiles: One clinic's example."
The CMS data is not meant to be prescriptive; however, keep in mind that carriers compare physician profiles at the national and local levels and target outliers for audits. If you find that your profile varies significantly from the CMS data, consider the reasons for the disparity. The following are potential explanations for billing more low-level visits than the norm:
You see many younger patients with acute rather than chronic illnesses.
You cover a walk-in clinic.
You handwrite your notes, which may produce documentation that supports a lower level of service.
You have a high-volume practice, which may result in less thorough documentation and lower-level codes.
If you bill more high-level visits than the norm, you might relate to the following:
You are new to your practice and are billing higher levels of service as you get to know your patients.
You use an electronic health record system, which may produce documentation that supports a higher level of service.
You see a relatively high number of elderly patients with chronic illnesses.
Another reason that your profile might fall outside the CMS benchmark has less to do with your patient demographics and practice environment than it does your familiarity with Medicare's Documentation Guidelines for Evaluation and Management Services. Without a fundamental understanding of E/M coding, you will not be prepared to document a visit accurately and select the appropriate code based on your documentation.
CHANGES IN FAMILY MEDICINE CODING FREQUENCY BETWEEN 2001 AND 2005
Coding for office visits, both new and established, has shifted to higher levels of service for many specialties, including family medicine. The graphs below illustrate shifts in codes reported to Medicare for new patient visits, established patient visits, hospital admissions, subsequent hospital visits, outpatient consultations, inpatient consultations and emergency department visits.
In almost every category of E/M service, family physicians billed higher levels of service overall in 2005 versus 2001. For example, in 2001, about 14 percent of all established patient visits billed to Medicare by family physicians were reported as 99212. In 2005, only about 7 percent of established patient visits were reported as 99212 – a decrease of almost 50 percent. During the same four-year period, the use of 99213 decreased by about 7 percent and the use of 99214 increased by about 60 percent.
The increased use of electronic health records (EHRs) and template-driven documentation may have contributed to this shift. A better understanding of coding and documentation rules, which has developed in response to mounting pressure to increase revenue, may help account for the change as well. The growing prevalence of chronic diseases may also play a role, since caring for patients with diabetes, heart disease and obesity often necessitates higher levels of service.
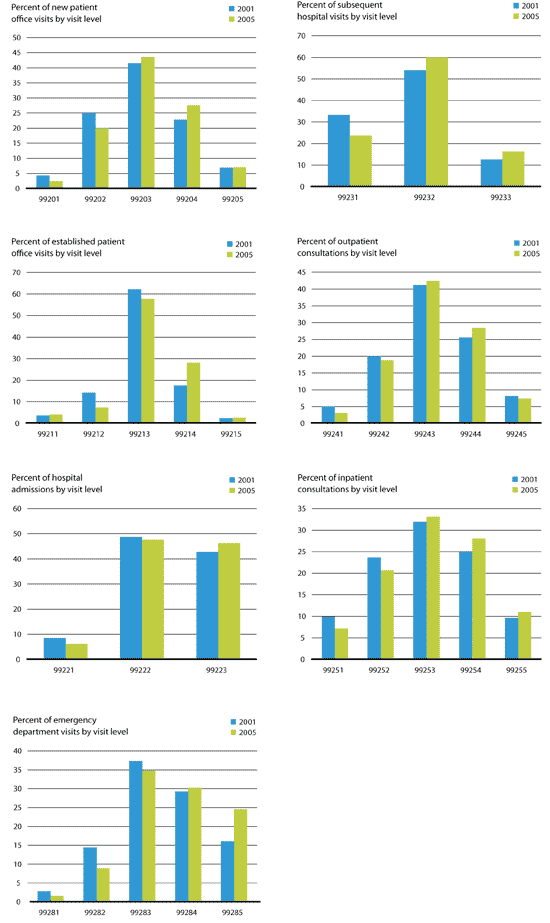
Source: Centers for Medicare & Medicaid Services. Raw data available at: https://www.cms.gov/research-statistics-data-and-systems/statistics-trends-and-reports/medicarefeeforsvcpartsab/medicareutilizationforpartb. Scroll to the bottom of the page and look for "Evaluation and Management (E/M) Codes by Specialty."
The top 25 codes. The second set of normative data you'll need for your analysis is the list of codes family physicians bill to Medicare most frequently. You should compare your top 25 codes with these. Again, this process is meant to be informative, not prescriptive. Because coding errors involving services that you perform hundreds or thousands of times a year are far more costly than errors involving services that you perform once or twice a year, it's especially important to ensure that you are documenting and coding these more common services correctly.
Note that of the top 25 codes, 11 represent E/M services: all five established patient office codes, four hospital care codes and two nursing facility care codes. Of the remainder, seven represent medications or injections – two areas especially worth reviewing.
Injection coding can be tricky because the code descriptions have changed repeatedly over the past three years. Also, different injections follow different rules. For some injections, you should bill one code for multiple injections (e.g., 95115 for one allergy injection but 95117 for multiple injections). Other injections require an add-on code for each additional injection (e.g., 90471 for the first intramuscular immunization and 90472 for each additional intramuscular immunization on that date).
Medications are difficult because you need to know how many units of each medication were administered. Be sure to keep an up-to-date version of the Healthcare Common Procedure Coding System (HCPCS) manual so you can determine how a medication is described and whether to bill for one unit or multiple units.
As you review the top 25 codes, it is also useful to look for services that you provide but are not billing for – and any that you're not providing that could generate additional revenue if you were to offer them.
THE TOP 25 CODES BILLED MOST FREQUENTLY TO MEDICARE BY FAMILY PHYSICIANS IN 2005
| CPT Code | Description | |
|---|---|---|
| 1. | 99213 | Office/outpatient visit, established |
| 2. | 99214 | Office/outpatient visit, established |
| 3. | Q9944* | IVIG non-lyophil, 10 mg |
| 4. | 99232 | Subsequent hospital care |
| 5. | Q9942* | IVIG lyophil, 10 mg |
| 6. | 99212 | Office/outpatient visit, established |
| 7. | 90658 | Influenza virus vaccine, age 3 & over, intramuscular |
| 8. | J1564* | Immune globulin, 10 mg |
| 9. | 99312* | Subsequent nursing facility care |
| 10. | 99231 | Subsequent hospital care |
| 11. | 99211 | Office/outpatient visit, established |
| 12. | G0008 | Administration, influenza virus vaccine |
| 13. | 85610 | Prothrombin time |
| 14. | 85025 | Complete blood count with automated differential white blood cell count |
| 15. | 95004 | Percutaneous allergy skin tests |
| 16. | 99311* | Subsequent nursing facility care |
| 17. | 99233 | Subsequent hospital care |
| 18. | 93000 | Electrocardiogram, with interpretation and report |
| 19. | 99238 | Hospital discharge day |
| 20. | 80053 | Comprehensive metabolic panel |
| 21. | 80061 | Lipid panel |
| 22. | G0351 | Therapeutic/diagnostic injection |
| 23. | 99215 | Office/outpatient visit, established |
| 24. | 71020 | Chest X-ray |
| 25. | 80048 | Basic metabolic panel |
Conducting a chart audit
The second exercise every practice should perform is a chart audit. Conducting a chart audit is one of the best ways to uncover gaps between what you document and what you code. Poor results are an indicator that it's time to review the E/M documentation guidelines.
The Department of Health and Human Services Office of Inspector General (OIG) recommends that practices review at least five notes per government payer, or 10 notes selected at random, per physician per year. An audit can be simple or elaborate. At its simplest, it should compare the documentation with the codes submitted on the claim form: Does the documentation support the procedure and diagnosis codes submitted? If not, carefully review the discrepancy and take note so that it does not happen again.
Also, be sure to note unusual patterns. For example, if you find you're billing all hospital admissions as level-IIIs or all subsequent hospital visits as level-IIs, it's time to review the code descriptions. Such uniformity of service level is unlikely, and in any case, billing all services in any category at a single level significantly increases your risk of being audited.
Fortunately, there are many resources available to help you improve your E/M coding skills (see the resources list and E/M coding articles from FPM).
E/M CODING PROFILES: ONE CLINIC'S EXAMPLE
The sample spreadsheet below shows one practice's E/M coding profile for office visits (OV) for its three physicians. You can download a copy of this spreadsheet in Microsoft Excel and use it to calculate your own code distribution. (Note: This tool has been updated since its original publication date; you will be downloading the most current version.)
| Dr. A | Dr. B | Dr. C | Practice Totals | Benchmark1 | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| CPT Code | # of Times | % | # of Times | % | # of Times | % | # of Times | % | % | |
| 99201 OV, new, straightforward | 5 | 2.76% | 0 | 0.00% | 3 | 1.06% | 8 | 1.06% | 2.28% | |
| 99202 OV, new, expanded | 98 | 54.14% | 8 | 2.79% | 17 | 5.99% | 123 | 16.36% | 19.90% | |
| 99203 OV, new, low | 72 | 39.78% | 197 | 68.64% | 255 | 89.79% | 524 | 69.68% | 43.43% | |
| 99204 OV, new, moderate | 6 | 3.31% | 82 | 28.57% | 6 | 2.11% | 94 | 12.50% | 27.46% | |
| 99205 OV, new, high | 0 | 0.00% | 0 | 0.00% | 3 | 1.06% | 3 | 0.40% | 6.93% | |
| Totals | 181 | 100.00% | 287 | 100.00% | 284 | 100.00% | 752 | 100.00% | 100.00% | |
| 99211 OV, est., minimal | 68 | 2.88% | 116 | 4.35% | 133 | 6.47% | 317 | 4.48% | 4.09% | |
| 99212 OV, est., straightforward | 1655 | 70.16% | 257 | 9.64% | 226 | 10.99% | 2138 | 30.18% | 7.35% | |
| 99213 OV, est., low-expanded | 475 | 20.14% | 2046 | 76.72% | 1542 | 74.96% | 4063 | 57.36% | 57.75% | |
| 99214 OV, est., mod.-detailed | 125 | 5.30% | 224 | 8.40% | 128 | 6.22% | 477 | 6.73% | 28.17% | |
| 99215 OV, est., high-comp. | 36 | 1.53% | 24 | 0.90% | 28 | 1.36% | 88 | 1.24% | 2.64% | |
| Totals | 2359 | 100.00% | 2667 | 100.00% | 2057 | 100.00% | 7083 | 100.00% | 100.00% | |
Get in the habit
Comparing your coding profile with Medicare benchmarks is a valuable exercise when performed regularly, along with a self-audit. It can alert you to coding trends within your practice that you might not be aware of, and it can indicate when it's time to brush up on your coding skills. Your effort may reduce your audit risk or be rewarded in your bottom line.
CODING RESOURCES FOR FAMILY PHYSICIANS
FPM Coding Tools. FPM's coding resources include the FPM Pocket Guide to the 1997 E/M Documentation Guidelines and the level-four reference card.
FPM ARTICLES ON E/M CODING