
Doctors have several options to cope with the impending July 1 payment reduction.
Fam Pract Manag. 2008;15(5):19-21
Kent Moore is the AAFP's manager for health care financing and delivery systems and is a contributing editor to FPM. Author disclosure: nothing to disclose.

At the time this article went to press, the federal government was still trying to figure out what, if anything, to do about a 10.6 percent Medicare fee cut scheduled to go into effect for physician services beginning on July 1, with an additional cut scheduled for Jan. 1. As with past years, a number of proposals have been developed to block the fee cut, but there's no guarantee that the cut will be averted this summer. (The seemingly annual battle that family physicians and other doctors fight against Medicare fee cuts can be blamed in part on the sustainable growth rate formula, which is addressed in “Medicare's (Un)sustainable Growth Rate,” an Opinion piece by Steven Wilk, MD, and Robert L. Phillips Jr., MD, MSPH.) If Congress does not intervene in the interim, here are some suggestions about how to prepare for and cope with the impending cut.
STEP 1: Evaluate the impact
The first step is to determine how big an impact the cut in Medicare fees would have on your practice. Part of this is knowing what percentage of your practice income is tied to traditional Medicare patients. In the typical family medicine practice, about 22 percent of patients are Medicare beneficiaries.1 Thus, a 10.6 percent cut in Medicare fees translates into about a 2.3 percent cut in practice income for the typical family physician. Given the margin at which many family medicine practices operate, that's a significant cut. Of course, this doesn't take into account the fact that private payers may also reduce their payment rates, based on Medicare's rates.
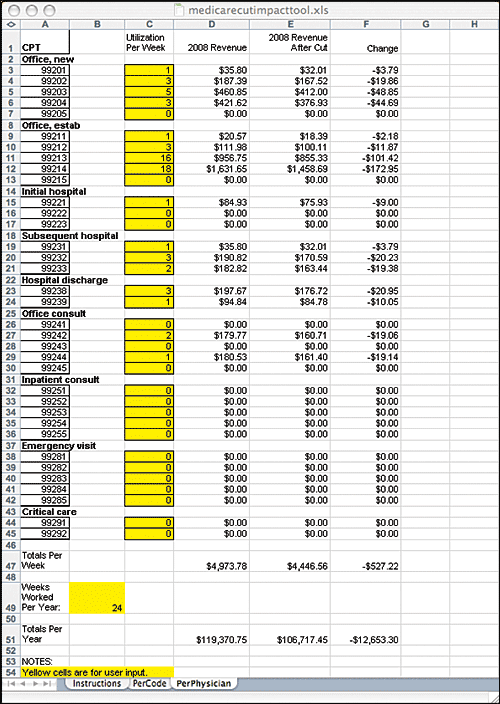
The fee and revenue analysis tool can be downloaded as an Excel spreadsheet and used to help you evaluate the impact of the cut.
MEDICARE CUT IMPACT TOOL
By plugging in the average number of services your practice performs weekly for the codes listed below, you can estimate the impact a 10.6 percent Medicare fee cut would have on your practice. Click below to download the tool as a Microsoft Excel file.
STEP 2: Know your options
The next step is reviewing your options as a practice, which include the following:
Opt out of Medicare and privately contract with Medicare patients. Opting out, also known as private contracting, allows a physician to enter into a private contract with a Medicare beneficiary for any item or service, if certain conditions are met. One of those conditions is that the physician must agree not to submit any Medicare claims or receive any payment from Medicare for items or services provided to any Medicare beneficiary for two years. Note that if you opt out, not only will Medicare and Medicare Advantage plans not pay you, but they also will not pay any entity to whom you might reassign your right to receive payment for services, unless the services are for emergency care or urgent care. Additionally, those Medicare patients who do not want to privately contract with you will have to find a new physician. On the upside, you will no longer be limited to collecting what Medicare allows (if you are a participating physician) or Medicare's limiting charge (if you are a nonparticipating physician), so you will be able to charge more for the services you provide to your privately contracted Medicare patients. (For more on opting out, see “How to Opt Out of Medicare,” FPM, November/December 2003. In addition, look for an updated article on the subject in the June issue of FPM.)
Refuse to treat Medicare patients after June 30, 2008, except on an emergency basis. Medicare is a voluntary program, and nothing requires you to treat Medicare patients in your practice if you do not wish to do so. Closing your practice to existing and new Medicare patients may eliminate a substantial portion of your current patient panel, which can significantly reduce your practice income until or unless you can find new patients without Medicare to fill the void. On the other hand, if your impact analysis indicates that you are losing money on each Medicare encounter anyway, closing your practice to Medicare patients may benefit you in the end.
Limit your practice to existing Medicare patients only; accept no new Medicare patients. This is a less radical option than closing your practice to all Medicare patients. It allows you to maintain existing Medicare patient relationships without exposing you to the potential negative financial consequences posed by adding new Medicare patients to your practice.
Reduce the number of Medicare patients in your practice. This option falls somewhere in between closing your practice to all Medicare patients and leaving it open to all existing Medicare patients, and it may depend on the percentage of your patient base that has Medicare as a primary insurer. For example, if 50 percent of your patients are on Medicare, you may not be able to simply close your practice to them all in the short run (because of the sudden disruption to your cash flow), and you may not be able to keep your practice open to all of them in the long run (because that is unsustainable financially, given practice expenses and decreasing Medicare fees). This option allows you to move in a direction that may make your practice more financially viable in the long run while minimizing disruptions in the short run.
Change your Medicare participation status. The Centers for Medicare & Medicaid Services has indicated that it does not intend to allow a change in physician Medicare participation status due to a mid-year reduction in physician fees, so this option does not exist with respect to the scheduled Medicare cuts in July. However, you will have the opportunity to change your participation status effective Jan. 1, 2009. Going from “participating” to “nonparticipating” is one way to attempt to offset the Medicare cuts scheduled in the meantime.
Nonparticipating Medicare physicians may collect up to the limiting charge from Medicare beneficiaries, which is, effectively, 109.25 percent of the Medicare participating physician allowance. So, for example, if the Medicare participating physician allowance for a service drops from $100 to $90, the new limiting charge for that service is $98.33. That means becoming nonparticipating would allow you to charge and collect almost as much as you did previously as a participating physician. The downside to nonparticipation, of course, is that you would need to collect a greater amount from your Medicare patients. (For more information on this option, see “Medicare Participation Options for Physicians” at https://www.aafp.org/online/en/home/practicemgt/mcareoptions.html.)
STEP 3: Devote extra attention to collections
Another step you can take is to review your practice's cash flow over the last year and the outstanding charges. Careful attention to accounts receivable indicators, such as the average age of unpaid claims, denied claims not resubmitted and repeated claim submission errors, might lead to better and steadier income. Some practices might benefit from a concentrated effort to collect outstanding charges after June 30. As is always the case, collection of deductibles and other patient balances at the time of service would likely provide a significant improvement in cash flow for many practices. Adopting more strict collection of past due balances or use of a collection agency may also help to alleviate pressures brought on by the Medicare reduction. (For more on improving your collections, see “Getting Off the Collections Treadmill,” FPM, June 2006, or “Patient Balances: Getting to the Root of the Problem,” FPM, March 2006.)
Always be prepared
In the end, how you cope with Medicare cuts, if they happen, will depend on the particular financial and other parameters of your practice. That said, now is the time to begin preparing for Medicare cuts, so that if they occur, you and your practice will be ready for them.