
Using the correct codes can mean the difference between getting paid and getting audited.
Fam Pract Manag. 2013;20(1):11-16
Dr. Fox is a family physician who has limited his practice exclusively to skin diagnosis and treatment since 2005 at the Mercy Defiance Clinic in Defiance, Ohio. Laura McCann is the information services director at Mercy Defiance Clinic. Author disclosure: no relevant financial affiliations disclosed.
Coding and billing for diagnosing and treating skin lesions is rife with potential pitfalls that could lead to delayed payments at best and increased insurer scrutiny or investigation for fraud at worst. Because skin procedure codes take into account the type of removal, the size and location of the lesion, your intent, and pathologic results, documenting your service and selecting the right code can be confusing. This article explains how to avoid some of the most common mistakes in skin procedure coding and provides an encounter form that can help you to more rapidly and accurately report skin-related diagnoses and associated procedures.
1. Know the difference between an excision and a biopsy
An excision is a procedure intended to fully remove a lesion. The specimen should include the lesion and the surgical margins. To qualify as an excision, the procedure must be full thickness, which means entirely through the reticular dermis to fat. For example, let's say a lesion appears to be a 4 mm nodular basal cell carcinoma (BCC) or a nevus. An 8 mm punch is used to excise the visible portion of the lesion with apparent 2 mm margins in all directions with the punch carried full thickness. The lesion has been excised. The excision code includes anesthesia and straightforward, simple closure. If the procedure required extensive undermining, a two-layer closure, and removal of excess skin, a separate code for a moderately complex closure should be used.
SKIN CARE ENCOUNTER FORM
By contrast, a biopsy is a procedure that samples anything less than a full lesion, even if full thickness (“incisional” rather than “excisional”). For example, sampling a 1 cm suspected squamous cell carcinoma (SCC) at full thickness into subcutaneous fat with a 4 mm punch instrument centrally should be coded as a biopsy. A biopsy code might also be used when sampling one or more of a group of lesions for diagnosis, even if these sample lesions are completely excised, or when taking samples of a dermatitis.
Complete removal does not necessarily mean that an excision code should be used. When the intent is to entirely remove the pathology by anything less than a full thickness technique, a shave code may be appropriate, even if the pathology report confirms complete removal of the lesion. For example, trying to completely remove a nevus or suspected melanoma via a “scoop” or “saucerization” technique that extends into the deep dermis and not the fat should be coded as a shave removal, not an excision.
2. Don't overbill for excisions or underbill for re-excisions
A primary excision should be billed based on the largest diameter of the lesion plus the narrowest lateral margins. For example, a round 4 mm lesion placed centrally in an 8 mm punch has a lesion diameter of 4 mm and 2 mm margins all around. The excision length for this lesion is 8 mm: 4 mm (lesion) plus 2 mm (one narrowest margin) plus 2 mm (other narrowest margin). For an ovoid lesion measuring 8 mm by 4 mm, removed with 2 mm margins across the short diameter and greater margins at the apices to fashion a fusiform excision closer to the traditional length-to-width ratio of 3:1, the calculation would be 12 mm: 8 mm (lesion) plus 2 mm (narrowest margins counted twice) (see the photo illustration on the next page).
The lesion should be measured preoperatively because tissue tends to change shape or shrink in formalin, which causes pathologic measurement to be generally smaller than the clinical measurement, and some dermapathology laboratories include that information in their reports.
A re-excision is a procedure on any lesion that has been previously biopsied or undergone an initial excision by you or anyone else. When billing for a re-excision, use the total closed length of the excision to guide your code selection. When a patient presents for a scheduled re-excision, you should bill for the procedure but not the office visit, unless significant, separately identifiable services are provided, in which case you could submit a code for the evaluation and management service with modifier 25.
If re-excision shows no residual malignancy, you should still bill the malignant lesion diagnosis codes, because that was the purpose of the re-excision.
3. Know the difference between biopsy and shave
When there is a dermatitis, such as suspected psoriasis, contact dermatitis, or Grover's disease, specimens you obtain for pathology should be classified as biopsies even if the sampled lesions are entirely removed using a shave technique. List your suspected diagnosis in your clinical notes, but you should bill using diagnosis code 709.9 for unspecified disorder of skin and subcutaneous tissue. If you use the code for psoriasis, for example, the insurer may reject the claim and ask why you did a biopsy if you already knew the diagnosis.
If you remove and “cure” a symptomatic seborrheic keratosis via a shave technique, that can be appropriately billed as a shave. If you cannot determine whether a lesion is a seborrheic keratosis or a melanoma and you do a full thickness excision because of concern about melanoma, it is legitimate to bill for excision. It is almost always inappropriate to excise seborrheic keratoses when you are certain of the diagnosis. It is often appropriate to remove them because of symptoms, but only via the shave technique. Note that for smaller lesions, biopsy codes may provide greater reimbursement than shave codes.
Lines can be blurred. For example, let's say a person has a single papulosquamous plaque, and the differential diagnosis includes SCC and superficial BCC. An attempt to completely remove the lesion via a shave technique is documented. The histology report indicates psoriasis. Because the intent was to evaluate for a suspected malignancy and the lesion was completely removed, documentation would support billing a shave code. A biopsy code also would have been appropriate, but the shave code is legitimate and the reimbursement is greater. It is okay to get paid for what you do!
My research suggests that most dermatologists tend to use the diagnosis code for neoplasm of uncertain behavior of skin (238.2) when biopsying or shaving a lesion of uncertain etiology because of concern about malignancy and billing before the histopathology is known. This remains the appropriate code after histology has returned for dysplastic nevi, sebaceous nevi, and other lesions of uncertain biologic behavior. The other option is to submit the diagnosis code for neoplasm of uncertain nature (239.2). Some coding authorities emphatically recommend this code rather than 238.2, but if you have been using 238.2 without difficulty I wouldn't recommend switching. I have used 238.2 exclusively for years with good results.
4. Don't upcode destruction of benign lesions or undercode destruction of malignancies
Molluscum and verrucae are epidermal lesions. On palms and soles, verrucae can be very deep and invaginate the epidermis and even make radiographic impressions on bone. However, even if you inject anesthesia and curette a deep wart on a plantar surface or use any of a variety of methods of removing molluscum, the appropriate code is either 17110 (destruction of benign lesions, 14 or fewer lesions) or 17111 (15 or more lesions), because the billing should be based on what is medically necessary.
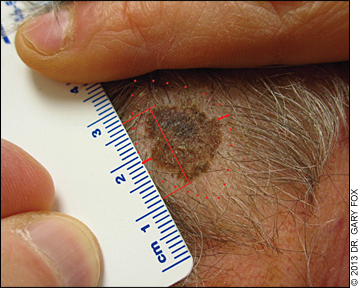
HOW TO MEASURE AN EXCISION LENGTH FOR PROPER CODING
This macular lesion is suspicious for melanoma. Many authorities recommend a 2 mm margin, full thickness, primary excision for diagnosis and initial pathologic staging to guide subsequent re-excision and management. Here, the excision length for billing for the initial excision would be the largest diameter of the lesion, 16 mm (long red arrow), plus the narrowest margins across the narrow diameter of the ellipse (clusters of dots at margins across short axis of ellipse), 2 mm on each side or 4 mm total, for a billed excision length of 2.0 cm (16 mm plus 4 mm ). Note that if the lesion needs to be re-excised, the re-excised length for billing will be the final closed length of the suture line. Pathology confirmed this as a melanoma. Thus, malignancy excision codes are appropriate both for the initial excision and re-excision, along with the ICD-9 code for melanoma, scalp (172.4).
When dealing with a malignancy that is curable by cryotherapy alone or by curettage with or without electrodessication or cryotherapy, the procedure often starts with a shave followed by the destructive procedure. You can only bill for one procedure in this case, and the codes for destruction of malignancies pay more than those for shaves or biopsies. For example, Medicare's median nongeographically adjusted payment rate for destroying a 2.5 cm scalp lesion (code 17273) is $208.31 versus $123.90 for a shave (code 11308) and $103.81 for a biopsy (code 11100). So when histology confirms malignancy, don't cheat yourself – bill for the destruction of the malignancy.
5. Don't submit claims prematurely
Codes – and payment amounts – may differ depending on whether the pathologic result is benign or malignant. Biopsies and shave removals should be coded and billed immediately because it makes no difference in code selection whether the lesion is benign or malignant. However, for excisions when the differential diagnosis includes malignancy, the claim should be held until you've reviewed the pathology report. Sometimes the pathology is equivocal, such as a dysplastic nevus or atypical junctional melanocytic hyperplasia. Such claims should be billed using diagnosis code 238.2 (neoplasm of uncertain behavior of skin) and a CPT code for an excision with benign findings.
When an obviously benign lesion is being excised because it is causing irritation (e.g., nevus catching during shaving), you could hold the claim until the pathology is known. I usually go ahead and submit the claim with a diagnosis code that indicates it is benign (e.g., 216.3, benign nevus of face) and the appropriate CPT excision code.
6. Know when to bill the patient rather than the insurer
When a patient asks for removal of a lesion for cosmetic reasons, Medicare, Medicaid, and most other insurance plans do not cover the service. Billing insurance for cosmetic removal of lesions could be deemed fraudulent. Tell the patient before the procedure that it may result in an out-of-pocket expense. Medicare requires an Advance Beneficiary Notice, signed by the patient before the procedure, or beneficiaries cannot be billed for the noncovered service. Consider using a separate encounter form – or even a separate visit – for cosmetic removals. Annotate these forms so that your billing staff knows not to bill insurance.
For benign lesions that are symptomatic or have functional significance, such as skin tags that catch on clothing or seborrheic keratoses that catch on combs, document the reason for removal and bill insurance. I add the secondary diagnosis code of disturbance of skin sensation (782.0) when removing known benign symptomatic lesions. This code is not precise, but I have found no better ICD-9 code to indicate irritancy from skin tags and seborrheic keratoses caused by clothing and other outside factors.
7. Know the global periods
Excisions have a global period, often 10 days, so suture removal and other routine follow-up care is included in the payment and should not be separately reported. Biopsies and shaves, on the other hand, have no global period, so you can bill for follow-up visits.
8. Know when to use multiple codes – or a single code for multiple lesions
If treating or destroying multiple benign lesions of the same type, such as verrucae or molluscum (or a combination of both), it does not matter for coding and billing purposes whether you use different methods. For example, you could remove some with shaving, some with cryotherapy, and others with cantharidin or an injection of Candida antigen. The important point is whether there were 14 or fewer lesions (code 17110) or 15 or more (code 17111).
If you biopsy three different lesions, or three different areas of a dermatosis, then the code is 11100 for the first biopsy and +11101 for each additional biopsy. However, if you do shaves and curettage with curative intent, wait for the pathology to return to verify BCC. Then bill for destruction of three BCCs, using a separate code for each one. Code selection will depend on the size and location of the lesion (codes 17260-17286). If you remove multiple lesions in a single visit by shave or full thickness excising, each should be reported separately with modifier 59 to indicate that these are distinct procedural services provided on the same day.
When treating more than one lesion of the same type on the same area, document well and include a note to the billing staff that these are separate lesions.
9. Know when to do two-layer closures – and bill for them
Tension on a skin closure suture line not only influences the likelihood of wound dehiscence but also is a factor influencing “railroad tracking” later. Surgeons who incise the skin for deeper procedures are not removing skin. When skin is removed, it needs to be pulled back together, which increases tension at the wound edges. Even with subcutaneous undermining, often the width of excisions is such that there will be significant tension on skin sutures unless absorbable subcutaneous sutures are placed. When a two-layer closure is appropriate, document its rationale and necessity in the dictation and surgical procedural paperwork – and bill for it. Append modifier 59 to the appropriate code for a moderately complex (two-layer) closure based on the site and excision length.
10. Don't overlook medical necessity
It is not medically necessary to do a full thickness excision to remove a symptomatic seborrheic keratosis, which is a superficial process, or to cure lesions of molluscum contagiosum, which is an epidermal viral process. Even if you perform excisions of these lesions, it is not appropriate to bill these as excisions.
11. Send everything for histopathology
You never want to be in a situation where a patient develops metastatic melanoma, has no obvious primary symptoms, and is asked whether he or she has had anything removed (especially anything “pigmented”) that was not sent for histopathology. Your word that it was a seborrheic keratosis may not protect you, because sometimes even the world's greatest experts cannot make that differentiation with complete assurance. Histology is your ally and your defense. Skin tags that are soft and absolutely typical, as well as typical verrucae in younger patients, can be exceptions.
12. Don't have documentation? Don't bill
Many of us have heard the expression, “If it isn't documented, it wasn't done.” Although we all know that saying isn't true, if you don't have documentation to support the medical necessity of a service, then you probably shouldn't bill for it.
Photography is an excellent documentation tool. You can capture location and size, provided you include a centimeter ruler in the photo next to the lesion. It also helps to support the medical necessity of the procedure (e.g., demonstrating an ulcerated, pearly lesion with telangiectasia). Of course, photos can also document history of recent onset, change, growth, bleeding, crusting, irritancy, etc.
Be careful
In one of my former jobs, I reviewed insurance claims for skin procedures. As one example of erroneous billing, a primary care physician billed more than $7,000 for excision of molluscum on a single claim. This was eventually recoded to destruction of benign lesions (17111), which typically pays about 2 percent of that amount. In situations like this, the insurer may go back and audit all your recent claims in this category and flag you for auditing going forward. When billing involves a government-sponsored insurance plan, you could also be investigated for waste, fraud, and abuse. You've worked too hard and too long for that.
