To better handle challenging patients or situations, try modifying the way you view them.

Let's face it. Some patient visits are frustrating, and if you aren't careful, a difficult patient can ruin your whole day. You also have to contend with frustrations such as insurance hassles, electronic health records, running late, and unfortunate patient outcomes. When frustrations mount, the technique of reframing can help reduce stress so you can better connect with your patient or resolve a problem. Reframing involves modifying your thoughts about a challenging person or difficult situation, and thus reducing frustration and increasing empathy.
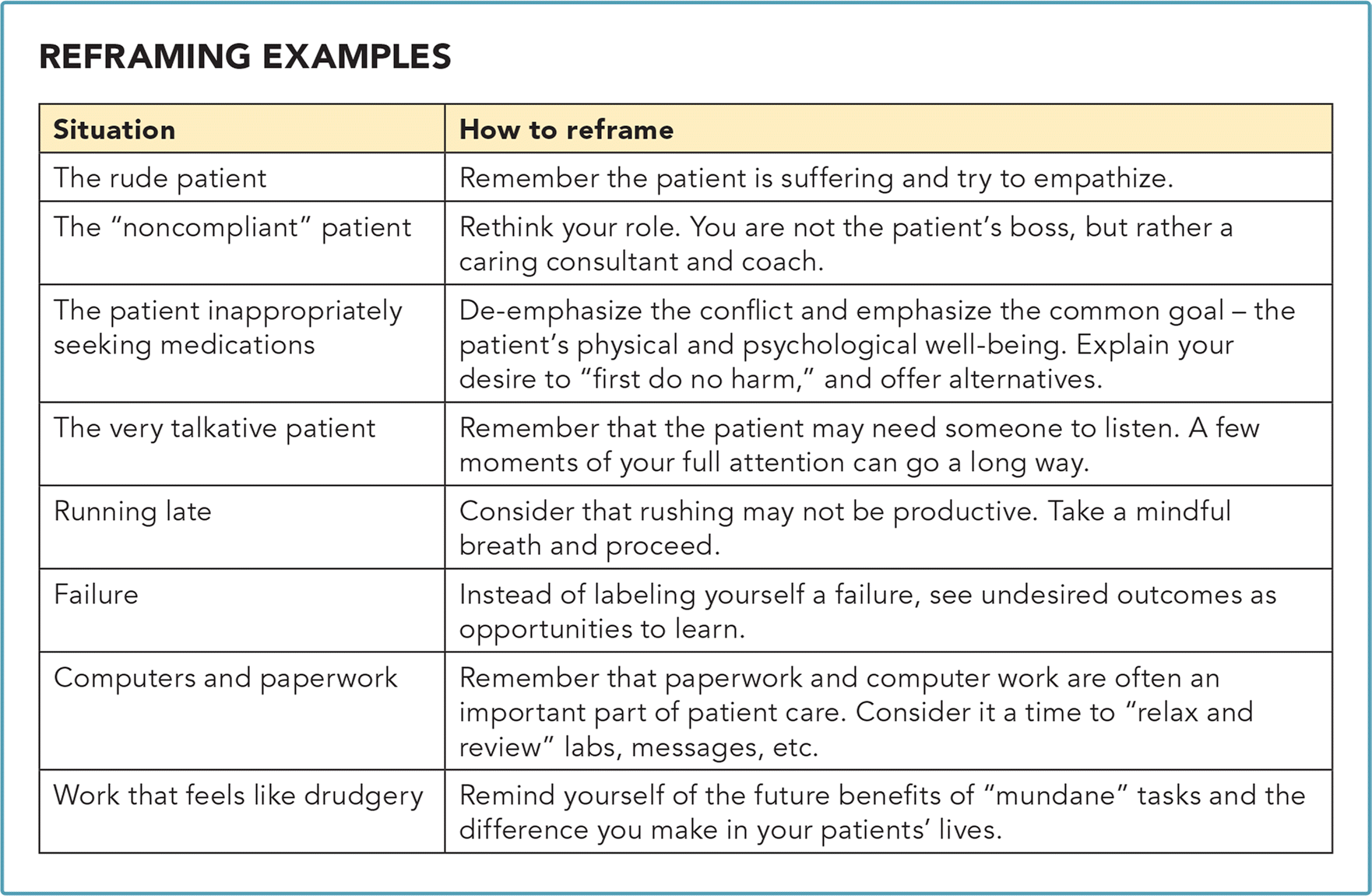
In this article, we will look at several common frustrations in medical practice and how reframing can help. (See “Reframing examples.” See also part one in this series, “Reducing Frustration and Increasing Fulfill-ment: Mindfulness,” FPM, July/August 2017.)
The rude patient
You enter the exam room to find Mrs. Jones scowling and sitting with her arms crossed. She just snapped at your nurse for having to repeat her blood pressure reading, and she immediately makes a snide comment about the quality of your staff.
When facing a patient who is rude, it is easy to be defensive, indignant, and even angry. Although your negative feelings toward a rude patient might be justified, they aren't necessarily helpful. How can you respond in a way that will lessen your stress and create a more successful visit? Start by honestly answering two questions:
1. Have you ever been rude?
2. When you have been rude, did it occur when you were happy and feeling your best?
If you're like most people, your answers are “yes” and “no,” respectively. In general, when people are rude, they are suffering. In fact, it's a wonder that we don't encounter more rude patients in our practices, given that most of them are suffering in some way – in pain, depressed, anxious, frustrated that they aren't getting better, etc. If you can remember that, then reactions such as “How dare she treat me and my staff that way” will be replaced with “I wonder what's going on with Mrs. Jones” or “She must really be suffering.” This type of reframing reduces our indignation, stress, and anger, and it increases our empathy, satisfaction, and ability to connect with our patients.
The “noncompliant” patient
At Dan's last visit, you spent 40 minutes carefully reviewing his history, providing patient education, discussing smoking cessation, and recommending medications, exercise, and dietary changes. Now, at his follow-up visit, Dan is still smoking, has gained weight, is not exercising, and has not started on any of the medications you prescribed. No one would blame you for feeling frustrated. However, you don't want to stay frustrated, become jaded, or let these issues get in the way of treating and connecting with your patient. Reframing can help.
Consider the term “noncompliant.” Compliance assumes that you are the boss and your patient is your subordinate. But that's not really the case. Your patient is paying you not to be the boss but to be a caring consultant and coach. If you consider yourself a coach, it can help you reframe the patient interaction. Instead of being disappointed or frustrated that your patients did not comply, you can empathize and brainstorm with them about why they did not follow through with your recommendations. This can help you better connect with them and provide more effective care so that eventually they will be more likely to make healthier choices.
The patient inappropriately seeking medications
Mr. Smith wants a narcotic prescription, and you suspect he is trying to satisfy an addiction rather than appropriately addressing pain. This type of visit is uncomfortable for most family physicians. To reframe this situation, try de-emphasizing the conflict and emphasizing, to yourself and to your patient, the common goal: the patient's physical and psychological well-being. If appropriate, discuss with the patient how, based on your medical experience and education, prescribing more narcotics will not provide long-term benefit but, rather, will likely cause harm. Explain also that a doctor's prime directive is to “first do no harm.” Then, if appropriate, you can discuss the risks of addiction and opioid-induced hyperalgesia and offer to refer the patient to a pain management specialist or an addiction specialist. Finally, offer the patient alternative types of treatment and next steps that are more appropriate and less likely to cause harm. Even if your patient is angry, you can be empathetic to his suffering and use your best judgment to act in his best interest.
The very talkative patient
You're running late, and next on your schedule is your most talkative patient, Jan. Her tendency toward conversational tangents makes getting a straight answer almost impossible. Before the visit even begins, you feel a knot in your stomach. To reframe this visit, think of Jan as someone who has waited a long time for this visit and just needs to describe what has been building up in her mind. With this type of visit, a little listening goes a long way. Yes, you should redirect the conversation as needed. However, if you're able to let these patients talk for just a few minutes and give them your full attention, they usually appreciate it.
Sometimes, talkative patients just need to be heard. They may be going on and on describing all their symptoms to you because they want reassurance that they do not have a serious disease. Lending an empathetic ear often does more for them than you realize.
REFRAMING EXAMPLES
| Situation | How to reframe |
|---|---|
| The rude patient | Remember the patient is suffering and try to empathize. |
| The “noncompliant” patient | Rethink your role. You are not the patient's boss, but rather a caring consultant and coach. |
| The patient inappropriately seeking medications | De-emphasize the conflict and emphasize the common goal – the patient's physical and psychological well-being. Explain your desire to “first do no harm,” and offer alternatives. |
| The very talkative patient | Remember that the patient may need someone to listen. A few moments of your full attention can go a long way. |
| Running late | Consider that rushing may not be productive. Take a mindful breath and proceed. |
| Failure | Instead of labeling yourself a failure, see undesired outcomes as opportunities to learn. |
| Computers and paperwork | Remember that paperwork and computer work are often an important part of patient care. Consider it a time to “relax and review” labs, messages, etc. |
| Work that feels like drudgery | Remind yourself of the future benefits of “mundane” tasks and the difference you make in your patients' lives. |
Running late
When you're running late in clinic, your blood pressure tends to rise. Knowing that others are waiting on you, how can you calmly connect with the patient in front of you? First, if you often run late, try adjusting the way you schedule your patients. However, no matter how well you schedule, there will be times when you run late. If your staff regularly keeps waiting patients up to date with how late you are running, they will be more understanding.
Reframing can also help reduce the stress of running late. In the novel House of God by Samuel Shem, 13 “laws” are given to new interns. Although many of the laws are sarcastic and cynical, law number three has some utility. It states, “At a cardiac arrest, the first procedure is to take your own pulse.” In other words, to handle an emergent situation effectively, you have to be calm. So, even though you're feeling rushed, it can be helpful to pause and take a full, mindful, diaphragmatic breath.
We tend to rush through our patients when we are running late. However, most patients would prefer to wait the extra couple of minutes for their visit if it means they will get your full attention when it is their turn.
Failure
As a family doctor, you will have patients who are diagnosed with serious illnesses and patients who die. You will second guess yourself. You may even have others second guess your decisions and call their attorney.
When things go wrong, we tend to look back at our decisions with 20/20 hindsight and call ourselves failures. A better mindset is to look forward, to reframe our mistakes not as failures but as sources of knowledge, and to see if there is something to learn for the future.
Famed physicist Niels Bohr once said, “An expert is a man who has made all the mistakes which can be made in a very narrow field.” And when Thomas Edison didn't succeed in his first attempt at inventing the incandescent light bulb, he said, “Every wrong attempt discarded is another step forward.”
Years ago, one of my patients was so angry about her visit that she switched doctors. With some reflection, I realized what I could have done better. At our last visit, I was a bit annoyed because she was late and I wanted to make the visit faster. I didn't bother reviewing her chart before going into the room. Normally, her urologist was good about sending consult reports, but this time he had not, and I entered the room totally unaware of her newly diagnosed bladder cancer. I could have left that experience feeling defensive, but instead I made it a learning experience. Since that time, I always review the patient's electronic chart before going into a visit. I also make a point to let go of any annoyance about patients being late and give them my full attention. Perhaps I won't be able to cover everything in that visit, but for the matters I do discuss, my goal is to connect and be fully present.
Emotionally recovering from a bad patient outcome can be complicated, and doctors may need time to grieve and process the event. Focusing on learning from a bad outcome, instead of second-guessing, will help in this recovery. Support from an empathetic colleague can also be helpful. All physicians have made errors and had bad patient outcomes; many just don't talk about them.
Computers and paperwork
For many doctors, their biggest stressors are not patient visits, but paperwork and computer work. Workflow solutions can help, such as delegating work to staff and using team documentation. But in addition to optimizing workflow, reframing paperwork and computer work can reduce your stress and frustration. Instead of thinking, “I hate computer work” or “I hate paperwork,” try reframing these tasks. For example, realize that communicating lab results electronically, answering messages via the computer, and completing patient forms are in fact part of patient care. I like to have small photos of my patients in their electronic chart to serve as reminders that I am connecting with my patients. I am not just doing computer work. Additionally, look for potentially positive aspects of what you are doing. For me, a positive side of doing some patient care via the computer is that I can listen to music or work from another location.
I've learned that the day before returning from a week-long vacation should include at least three hours of computer catch-up time. On one of these days, I found myself starting to dread the three-hour stint, so instead of thinking of it as “computer work,” I renamed it “relax and review time.” I sipped a cup of tea as I listened to some relaxing music and, believe it or not, for the most part enjoyed reviewing lab results, consult reports, and messages. When I rename it “relax and review time,” the work takes no more time; it is just much more pleasant.
Also, remember that most of the stress of paperwork and computer work occurs when it hangs over your head. When you can stay on top of this work, it is generally not so bad.
Work that feels like drudgery
As family medicine doctors, we might at times view our jobs as a series of mundane tasks and forget the importance of the work we do. For example, we try to make sure that our patients have their colonoscopies, that their blood pressure and cholesterol are under control, and that they make efforts to quit smoking. Because we don't know about the stroke or cancer death that didn't occur, we don't always realize the big differences we make for our patients.
Increase your fulfillment by reframing this “mundane” work and viewing it as the essential groundwork for making a difference in your patients' lives. When you see Mrs. Jones, whom you have treated for hyperlipidemia and hypertension for the past five years, take a moment to realize that, if not for your treatment, she might have had a stroke or a heart attack. When you see Mr. Smith, remember that you made sure he had the colonoscopy that found an adenomatous polyp, perhaps preventing colon cancer. Remembering all the good work you do will help you feel more fulfilled.
An essential skill
We can't always change our circumstances or the people around us, but we can change the way we view them. Reframing is an essential skill for family physicians. It can reduce our stress and frustration, help us approach difficult patients and circumstances more effectively, and ultimately create more joy, satisfaction, and fulfillment in our profession. The more this skill is practiced, the greater its benefit.
The next time you find yourself feeling frustrated at work, don't give in to that feeling. Instead, try to reframe the person or situation, and see what happens.

