This three-step framework can help you address patients' concerns about influenza immunization.

Thousands of people are hospitalized each year due to influenza, despite it being easily preventable with vaccines.1 Patients who decline flu vaccination generally fall into two categories: the “chronic no” (those who have unequivocally refused the vaccine for years) and the “undifferentiated no” (those who have declined for reasons we have yet to explore). After eight years of working together, we have developed a team-based routine that has improved our efficiency and effectiveness in getting our patients vaccinated.
The nurse's role: Setting the stage
I (Crues) am in charge of asking patients about influenza vaccinations and informing Dr. Fogarty if they have concerns, fears, or anxiety about the flu shot. During flu season, I ask patients as part of the rooming process if they would like a flu vaccine. If a patient declines, I ask if the patient minds sharing his or her fears and concerns and then listen to the response. When appropriate, I share my own story of receiving a flu shot after years of declining and not having any problems with it. I also give the patient a flu vaccine information sheet, which the patient can review while waiting for Dr. Fogarty to come into the exam room. I work with the language interpreter or seek other help for patients who have trouble understanding the information.
In the electronic health record (EHR), I type each of the patient's chief complaints for the visit and add “Wants fluvax” or “Declines fluvax” in the last line. This makes Dr. Fogarty aware of the patient's intentions for the flu shot before entering the exam room, which saves a lot of time during the visit.
Patients who either request the flu vaccine or indicate that they received it at an outside location require little to no extra conversation. If the patient received the shot elsewhere, I request the record and enter the date into our chart. For patients who request a shot, Dr. Fogarty quickly orders it before entering the room so I can get the vaccine ready. Sometimes I can administer the vaccine before Dr. Fogarty's consultation. Overall, our team approach can reduce the total time the patient is in the office.
For the “chronic no” patients, who have generally declined the flu shot for years despite our education efforts, we don't challenge them beyond a brief check-in; we use our time to discuss other clinical concerns. It is the “undifferentiated no” patients our conversations can potentially influence.
The physician's role: Ask-Tell-Ask
I (Fogarty) handle these visits using the “Ask-Tell-Ask” framework, which was derived from the “Elicit-Provide-Elicit” model for promoting behavioral change in motivational interviewing.2,3,4 The Ask-Tell-Ask model is helpful when patients are deciding on something that may not have a “right” answer, such as screening for prostate cancer.5 It helps me better understand a patient's perspective on a recommended treatment as well as what additional information he or she may need. I use this format over and over during influenza season to pinpoint and address patients' reluctance about receiving the influenza vaccine. (See “Ask-Tell-Ask framework.”)
ASK-TELL-ASK FRAMEWORK FOR FLU VACCINATION
Ask: “I understand you don't want the influenza shot today. Can you help me understand why not? Do you mind if I share some information with you about the vaccine?”
Listen and observe the patient carefully. What is he or she telling you? What emotions is the patient showing? Responses may include, “I don't want to catch the flu from the shot” or “I got the flu shot last year.” Get the patient's permission before offering information.
Tell: Respond with information centered on the patient's belief or question.
Listen and observe the patient carefully. Listen to verbal responses and watch for nonverbal reactions to what you tell the patient. Address further questions or confusion.
Ask: “What are your thoughts now about getting a flu shot?”
If the patient agrees, have your nurse administer the vaccine. If the patient is firmly opposed to getting the vaccine, respect the patient's autonomy but welcome further conversation.
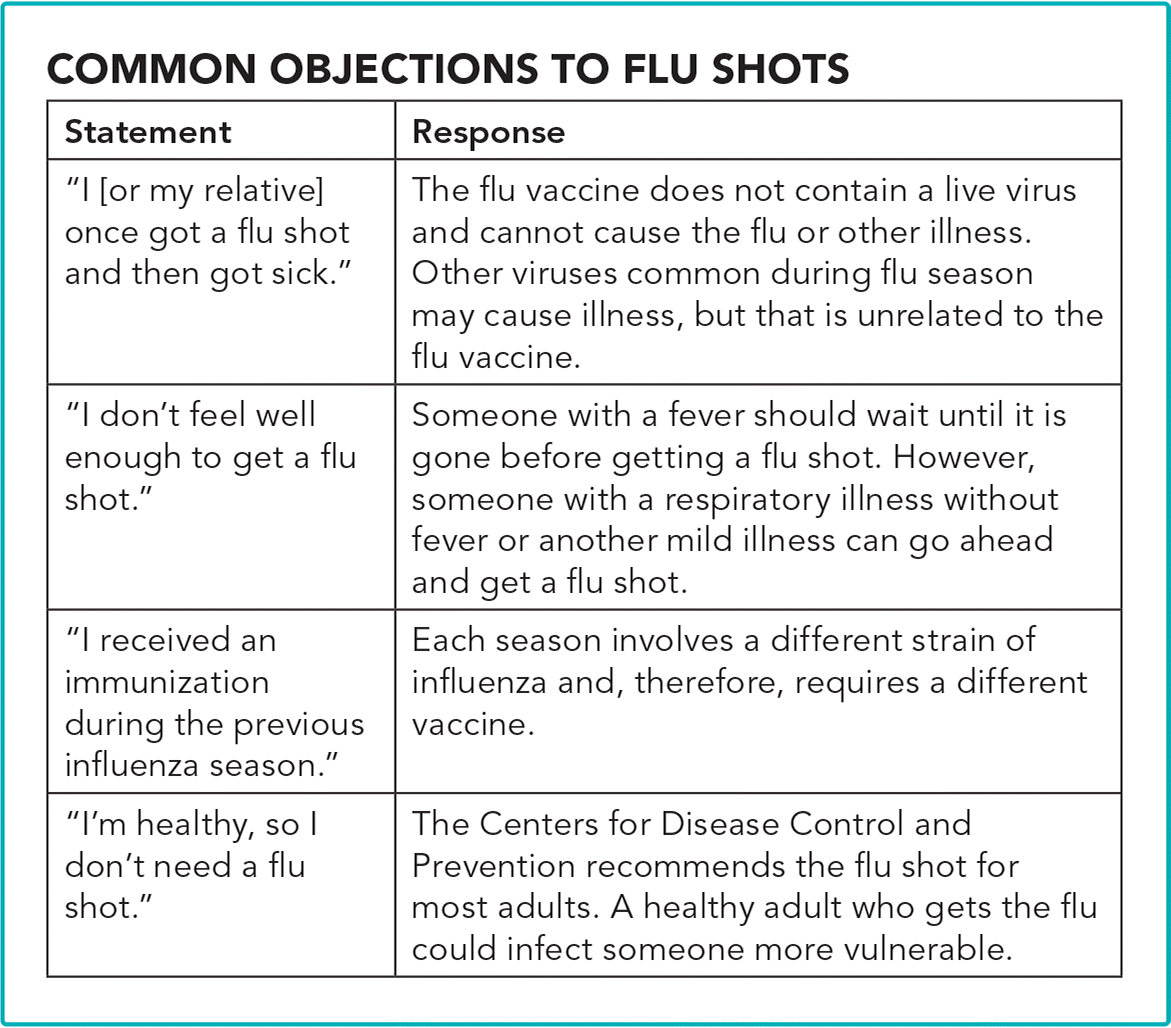
Ask. After greeting the patient, I review the agenda that the nurse and the patient set for the visit. If the patient declined the nurse's offer of the flu vaccine, I confirm the patient's decision and then make my first “Ask”: Would you tell me more about why you do not want a flu shot? This is similar to the nurse's question during rooming, but I am asking the patient to expand on it. I listen carefully to the patient's words and watch for nonverbal communication. Often I discover fear of the vaccine based on the experience of a friend or relative or the patient's own past experience. (See “Common objections to flu shots.”)
COMMON OBJECTIONS TO FLU SHOTS
| Statement | Response |
|---|---|
| “I [or my relative] once got a flu shot and then got sick.” | The flu vaccine does not contain a live virus and cannot cause the flu or other illness. Other viruses common during flu season may cause illness, but that is unrelated to the flu vaccine. |
| “I don't feel well enough to get a flu shot.” | Someone with a fever should wait until it is gone before getting a flu shot. However, someone with a respiratory illness without fever or another mild illness can go ahead and get a flu shot. |
| “I received an immunization during the previous influenza season.” | Each season involves a different strain of influenza and, therefore, requires a different vaccine. |
| “I'm healthy, so I don't need a flu shot.” | The Centers for Disease Control and Prevention recommends the flu shot for most adults. A healthy adult who gets the flu could infect someone more vulnerable. |
The second part of this “Ask” usually revolves around the need to correct misperceptions about the flu vaccine. For example, I will ask, “Do you mind if I share some information with you?” The motivational interviewing model highly recommends asking permission to provide advice when attempting to change health behavior. This is also important to maintaining a patient-centered approach. If the clinician provides what the patient perceives as a lecture, the patient is more likely to dismiss the recommendation. Asking permission also demonstrates respect for the patient by conveying that the clinician will not waste the patient's time providing information the patient does not want. In my experience, no patient has ever declined the offer of more information.
Tell. Next comes the “Tell.” In this phase, it is important for me to be brief and convey information specific to the patient's belief or fear. For example, if the patient is worried about catching the flu because a family member once developed a cough shortly after getting the flu shot, I explain that the flu vaccine is made of killed virus, not live, and cannot make the patient sick. (See “Resources.”)
As I speak to the patient, I carefully watch for nonverbal cues of understanding, doubt, or other reactions. Then, I pause for a moment. If the patient appears to be following what I'm saying, I continue by acknowledging that such concerns are common. I might go on to explain that because we typically administer the flu shot in the fall and winter when other viruses are in the community, people may get sick from these other, unrelated viruses but believe the flu shot caused it. Again, I'm careful to watch the patient's body language or expression to detect unspoken questions, comprehension, or emotion. If the patient has questions, I try to answer them, again focusing on the key concerns.
Ask. Eventually, I make the final “Ask”: What are your thoughts now about getting a flu shot? After hearing the information, many patients agree to the vaccine. Of course, many others continue to say “no.” I'm careful to provide a clear medical recommendation for the vaccine, but I also respect their autonomy to choose. I tell them that if they want more information about flu vaccination or if they change their mind in the future to let myself or the nurse know. This leaves the door open for more conversation in the future.
Getting to “yes”
We are continually surprised by the number of reluctant patients who change their mind and agree to a flu shot when we use the Ask-Tell-Ask framework. This simple tool has successfully moved the needle on prevention in our practice, helping us get more of our patients immunized, especially those who are most vulnerable.

