
Even with a laudable goal, such as reducing physicians' administrative burdens, it can be difficult to implement change. These real-world lessons can help.
Fam Pract Manag. 2017;24(6):10-15
Author disclosures: This study was funded by AHRQ, contract #HHSA290201000034I. The views expressed are those of the authors and are not endorsed by AHRQ. No other relevant financial affiliations disclosed.
It's hard to change. Practice settings, workflows, individual characteristics, and time constraints all affect our will and capacity to try something new even when the status quo is not working for us.
Penobscot Community Health Care (PCHC) is a federally qualified health center located in rural Maine. It serves more than 60,000 patients across 15 practice sites, including nine primary care practices, and it employs 700 people, including 200 providers. In January 2014, we attempted a major change across our primary care sites – implementing a “delegate model,” a team-based approach to care featuring an enhanced medical assistant (MA) role.1
Under this model, MAs are trained to take on additional administrative tasks thereby reducing the burden on primary care providers. The model combines two primary care providers and their MAs to form a team with a shared panel of patients and adds a full-time “care team MA” (CTMA) as a fifth team member. The CTMA, after approximately 30 hours of training, can then take on a range of responsibilities. These include previsit planning, standardized prescription renewals, schedule management, provider in-box management, and identification of patients for routine auxiliary testing and referrals (e.g., mammograms, behavioral health, and care management) using an expanded set of standing orders.
Three goals drove our interest in the delegate model:
Reduced provider burnout,
Improved access to care,
Improved quality of care.
Our change team's initial strategy was to identify teams in five of our larger primary care practices that would champion the new model and share their experience with their peers. As others observed and heard about the success of the model, they too would want to participate. After two or three years, the new model would become the new norm – or so we thought.
In this article, we will share what really happened, as well as the lessons we learned at the three critical stages of change – adoption, implementation, and sustaining change.
Adoption: getting people on board
To encourage adoption of the new practice model, we needed to “sell” it to everyone. Staff and leaders at every level had different expectations for the model and prioritized our three goals differently. Organizational leadership thought all three goals – reduced provider burnout, improved access, and improved quality – were important, but they stressed that the model also had to pay for itself through increased visits to be sustainable. Practice leadership also agreed with all three goals but thought there might be ways to achieve them instead of using the delegate model (they wanted to retain their autonomy and not be pressured into adopting a standard model). Providers endorsed the focus on burnout and improved quality of care but were adamant that they could not improve access by seeing more patients. They felt that current productivity demands were already unachievable and contributing to time pressure, low levels of job satisfaction, and burnout.
Because transparency is an organization-wide value, we wanted to be forthright with providers that this model was intended to improve efficiency, which in turn would enable them to see more patients over time. We calculated that if the new two-provider team could see on average two additional patients per day (one per provider), this would be sufficient to cover the cost of the CTMA in a fee-for-service payment environment. In discussions with providers, we acknowledged the pressure they work under and the fact that administrative tasks related to their jobs were slowing them down and invading their evenings and weekends. We emphasized that this was a pilot project and only after its completion would we be able to see the extent to which it reduced their administrative burden, as well as their job stress. However, we knew we also needed to do something immediately to address their concerns about productivity demands, so we dropped provider productivity penalties, moving from an incentive-based compensation model to a salary model. Although this change in the compensation model had been under consideration for some time, implementation of the delegate model was an important consideration in our leadership's decision to finally change the policy.
Showing a good faith effort through this organization-wide change helped with recruitment of the initial championship team, but it didn't convince everyone to get on board. Some providers just weren't interested; for the most part, they had long tenure and a practice style they had no desire to change. Other providers simply weren't right for these new teams because of performance issues; we wanted high-performing providers to be champions with the rationale that they would be most likely to succeed and most in need of the relief that the new model could provide. We ended up targeting providers who were new to practice and did not already have established practice patterns. Often, we paired a high-performing provider and a new provider to form a team. Among our MAs, many were interested in assuming the new CTMA role, but some were reluctant to change their routines or not interested in having a largely administrative position. Additionally, not all MAs and providers seemed to have the intangibles we thought were important for the model to work. (See “Characteristics to look for in a change champion.”)
CHARACTERISTICS TO LOOK FOR IN A CHANGE CHAMPION
For providers:
Willing to delegate,
Willing to work as part of a team,
High-performing or new to practice and not attached to a practice style.
For CTMAs:
Critical thinker,
Independent,
Competent,
Trustworthy,
Comfortable speaking up,
Skilled with the electronic health record.
Although the long-term vision is that this staffing model will become the new norm, we decided early on not to concentrate on practices that were resistant to change. The effort and cost of engaging those who were reluctant did not seem worth it. Instead, we screened for characteristics amenable to the model when recruiting new providers and MAs. Rather than stick to our initial strategy of spreading within our five largest practices, we also took advantage of the organic spread in smaller practices. This generally occurred when providers or MAs who had been involved in the model transferred to other practices within our network.
Practice and provider autonomy proved to be another stumbling block during the adoption phase. They definitely wanted the extra set of hands that the CTMA could provide, but they wanted to determine how to best use the extra team member rather than have the role prescribed for them. Although being able to adapt the intervention to various contexts is important, we were adamant about protecting two core elements: 1) Teams should not use the CTMA as a “floating” MA (used to cover other MA absences), as this would work against the CTMA's primary purpose of reducing providers' administrative tasks, and 2) Teams had to implement the core function of previsit planning, which we felt was essential to efficient, effective care.2 If providers or practice leadership were unwilling to accept these two elements, we did not implement the model within that team.
Lessons learned. The key lessons we learned about adoption are as follows:
Be transparent about what you are trying to accomplish, but use messaging that speaks to the different priorities people may have.
Back up these messages with actions that show good faith, sincerity, and a willingness to listen (e.g., following through on changes to the compensation model).
Choose champions who are willing to engage, committed to working through setbacks, seen as leaders, and willing to act as ambassadors for the intervention.
Don't waste valuable resources on converting resisters. Leverage those who are eager.
Identify which components of the intervention are negotiable and which are essential and nonnegotiable.
Implementation: putting the plan into action
We underestimated the level of effort needed to get our new teams up and running. We had planned to provide significant training to our MAs to ensure they were well prepared to carry out the CTMA role, along with two weeks of observation and support to the new team in the practice setting. However, once we started implementing the model within a practice, we inevitably encountered operational, managerial, and administrative barriers and had to change our implementation strategy accordingly. Teams needed more than just observation and supervision during initial implementation; they also needed technical assistance. Because we only had one person providing this assistance, other team start-ups and training sessions were delayed. Given the significant training time required for MAs, it was not unusual for turnover to occur at some point, requiring us to identify a new staff member for the new team, and the whole process started anew. Additionally, it proved challenging to pull MAs from their practices for the approximately 30 hours of training. Their duties had to be covered by other staff, which was not always possible. This led to further delays in implementation.
We needed to come up with strategies to reduce the long lead time for teams to go live. One strategy was to open the CTMA training to all MAs who would be part of these new teams, regardless of their role. This cross-training meant that other MAs were aware of and could perform the CTMA role, which yielded a number of benefits. Teams did not fall apart when a CTMA shifted positions, went on leave, or left the organization. It also increased knowledge, understanding, and buy-in of the model by all MAs, whereas previously the lack of understanding around the new CTMA role sometimes created uncertainty and stress for the other MAs on the team. Another unexpected and positive benefit of opening training to all MAs was that, as they moved between our various practices, they took this new knowledge and way of doing things and advocated for the model in their new environments.
Cross-training MAs also led to some teams adapting the model to make it more appealing. Some CTMAs wanted to maintain their patient interaction responsibilities, rather than be entirely devoted to administrative tasks. Thus, cross-trained teams were able to rotate CTMA responsibilities among the MAs, allowing them to continue working with patients directly.
We also prioritized certain training modules that proved to be most helpful. For example, providers were most enthusiastic about previsit planning, and it seemed to offer the greatest opportunity to improve care quality. Teams could start the model once the MAs completed this initial training, without having to wait for the full CTMA training to be completed. Rather than trying to change multiple work-flows simultaneously, they could focus just on those related to previsit planning.
For providers and MAs to work well together with maximum delegation, they needed to build trust, become comfortable with reorganized roles and responsibilities, and learn how to communicate with one another more effectively. Team building required more effort, took longer than we expected, and in some cases did not work out. We selected the teams carefully, but should have offered more team-building training and support.
We eventually realized that we needed to involve practice directors, clinical coordinators, and providers in training and team meetings rather than focusing almost exclusively on the MAs. Broad involvement was essential to secure understanding of the model's intent, clarity about roles and responsibilities, and support for team building. Practice leaders became important advocates for the model. They developed budget requests that included funding for CTMAs, recruited new staff with qualities that would contribute to successful team dynamics, and managed operational issues to facilitate implementation of the model.
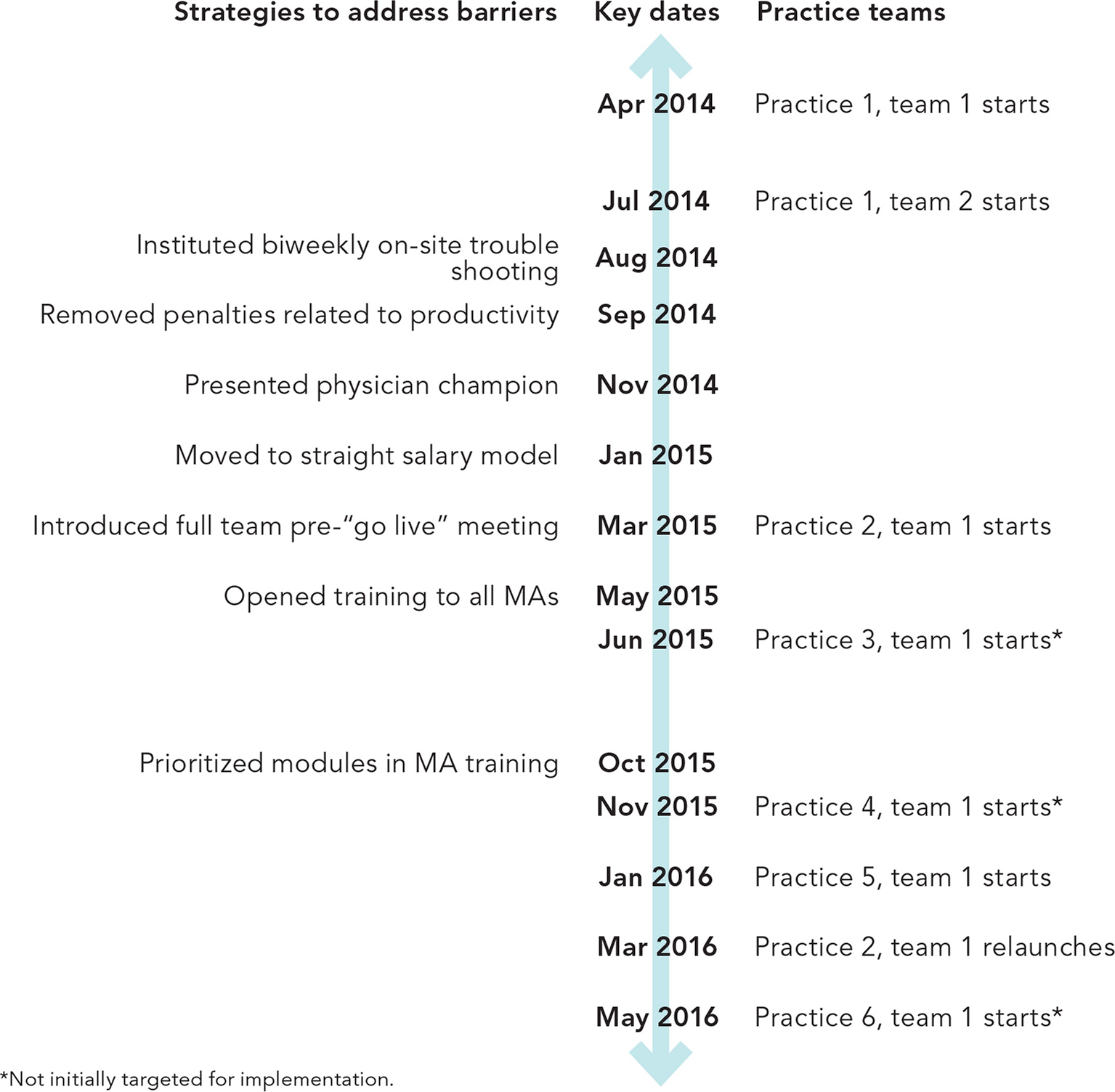
Although our implementation did not go according to plan and was slower than we had hoped, we did eventually establish seven teams at six of our nine primary care practices. (See “Implementation timeline and strategies.”)
Lessons learned. The key lessons we learned about implementation are as follows:
Remain flexible, willing to adapt, and prepared to bring in additional resources if needed, because implementing change never goes completely according to plan.
Be broad in involving others in training and model implementation. The more people who are aware of what you are trying to accomplish, the better; they can serve as advocates for the model, resulting in more staff who understand it and can support implementing teams.
Approach team building, developing trust, and learning how to work together as a process. It may require more time, training, and resources to accomplish.
Understand that staff turnover is to be expected, and work out a proactive implementation strategy that takes turnover into account.
Sustainability: keeping it going
Looking at our initial three goals of reduced provider burnout, improved quality, and improved access, we found neutral to modest results. Although a survey of provider burnout showed no statistically significant changes between providers engaged versus not engaged in the new model, anecdotal evidence found that involved providers and MAs appreciated the model. For our longest engaged practice, we did see modest statistically significant increases in three quality measures (blood pressure control, breast cancer screening, and cervical screening). There was also a gradual but statistically significant increase in cycle time (the time from patient check-in to checkout), likely reflecting the time for screening and other care management tasks. However, our data on encounters did not show any change in the average number of patients seen per day (our proxy measure for access). We suspect that even though providers did not see more patients overall, the use of previsit planning and delegation likely made their services more comprehensive, contributing to higher quality. Perhaps, as teams become more comfortable with the model, patients seen per day will eventually increase.
We did not consider the training costs associated with the model as particularly high. We estimated that it cost between $4,047 and $5,812 in staff time to train the MA and team to implement the new model. (The latter amount takes into account turnover of MAs or providers during implementation.) The largest cost, however, is the additional salary of a third MA for the two-provider team. In a fee-for-service environment, we would have to recoup this through seeing additional patients (an average of two per day for the team or one per provider). As noted, our initial encounter data did not show this increase in productivity.
Three years after starting our efforts, the delegate model persists in four of the seven teams, most notably those with the longest experience with the model. It has not been sustained in the sites that implemented it more recently, due entirely to financial pressures related to the additional cost of a third MA. However, other innovations have stemmed from the model (e.g., a senior MA role and revised standing orders) and are well established.
For now, perhaps the greatest benefit of our experiment is readying our staff for a team-based approach to care and shared panel management. As screening, preventive care, and chronic disease management guidelines proliferate, the only way we will be able to fulfill these expectations is to shift to a team-based approach where everyone works at the top of their license and shares responsibility and accountability for their patients. We know that value-based payments will eventually become the norm and the delegate model with its focus on previsit planning and population health will put us in good position to thrive under these new reimbursement models. This may be the way we ultimately recoup the CTMAs' salaries. Additionally, through simply engaging in the experiment, we learned valuable lessons about change management and implementation that will carry over to other endeavors.
Lessons learned. The key lessons we learned about sustainability are as follows:
Be open to other outcomes that will support sustainability beyond simply covering costs. For example, providing additional training to MAs increased their knowledge and skills and helped establish a career ladder within the organization to recognize those with high proficiency. This benefits not only the MAs but also the organization. Additionally, improving clinical quality became as important as cost in considering whether to sustain the model, as this was the factor that providers valued most.
Recognize the importance of organizational learning that comes from experimentation – not only the knowledge related to the intervention itself but also the growth that comes from attempting something new.
Accept that outcomes from experimentation are rarely entirely clear and that decisions about how to move forward must generally be made with this “gray” information.
Applying lessons learned
The concept of spreading change has three phases: adoption, implementation, and sustainability. Although planning for each of these phases is important, things rarely go as anticipated. Keeping an eye on progress, being flexible, and addressing challenges as they arise are essential. Even if you do everything right, change will be hard and will come with unknowns, but drawing on these lessons learned will give you a jump start as you implement change in your setting.
