If you're not coding and billing for these services, you might be leaving money on the table.

Recent changes to CPT codes for structured screenings and brief assessments have led some payers to expand coverage for these services. If you are not billing for these services, you may be losing out on valuable revenue. Quality initiatives may include incentives for performing and reporting recommended screenings and assessments, which provides an additional reason to familiarize yourself with these codes. In this article, we will review the documentation and billing requirements necessary for getting paid.
Correct coding and documentation
Four codes are used to report structured screening and assessments:
- 96110, “Developmental screening (e.g., developmental milestone survey, speech and language delay screen), with scoring and documentation, per standardized instrument,”
- 96127, “Brief emotional/behavioral assessment (e.g., depression inventory, attention-deficit/hyperactivity disorder scale), with scoring and documentation, per standardized instrument,”
- 96160, “Administration of patient-focused health risk assessment instrument (e.g., health hazard appraisal) with scoring and documentation, per standardized instrument,”
- 96161, “Administration of caregiver-focused health risk assessment instrument (e.g., depression inventory) for the benefit of the patient, with scoring and documentation, per standardized instrument.”
Codes 96110, 96160, and 96161 are typically limited to developmental screening and the health risk assessment (HRA). However, code 96127 should be reported for both screening and follow-up of emotional and behavioral health conditions.
The purpose of the screening or assessment should guide code selection. To see a description of each code and examples of standardized instruments that may be used for each, see “Quick reference: Screening and assessment codes.” CPT Assistant has described a standardized instrument as a “previously validated test that is administered and scored in a consistent or ‘standard’ manner.” Validated structured instruments have been shown through study to provide consistent and reliable results.
These codes do not represent physician work. For payment purposes, each screening and assessment code was valued based on practice expense and professional liability only, which includes the cost of furnishing instruments (when applicable) and staff time to administer and/or score an instrument for the physician or other qualified health care professional's review. The physician's interpretation of the score in light of the patient presentation is considered part of the evaluation and management (E/M) service, which would be billed in addition to the screening or assessment code.
Documentation of a structured screening or assessment should include the date, patient's name, name and relationship of the informant (when information is provided by someone other than the patient), name of the instrument, score, and name and credentials of the individual administering the instrument. In addition, the physician must document that he or she reviewed the score in the context of the patient presentation and discussed the results with the patient/family as part of the related E/M service. A few payers do indicate that a report (separate from the E/M service documentation) is required. This is based on CPT guidance for central nervous system assessments that states, “It is expected that the administration of these tests will generate material that will be formulated into a report.” Verify your payers' documentation requirements prior to providing these services.
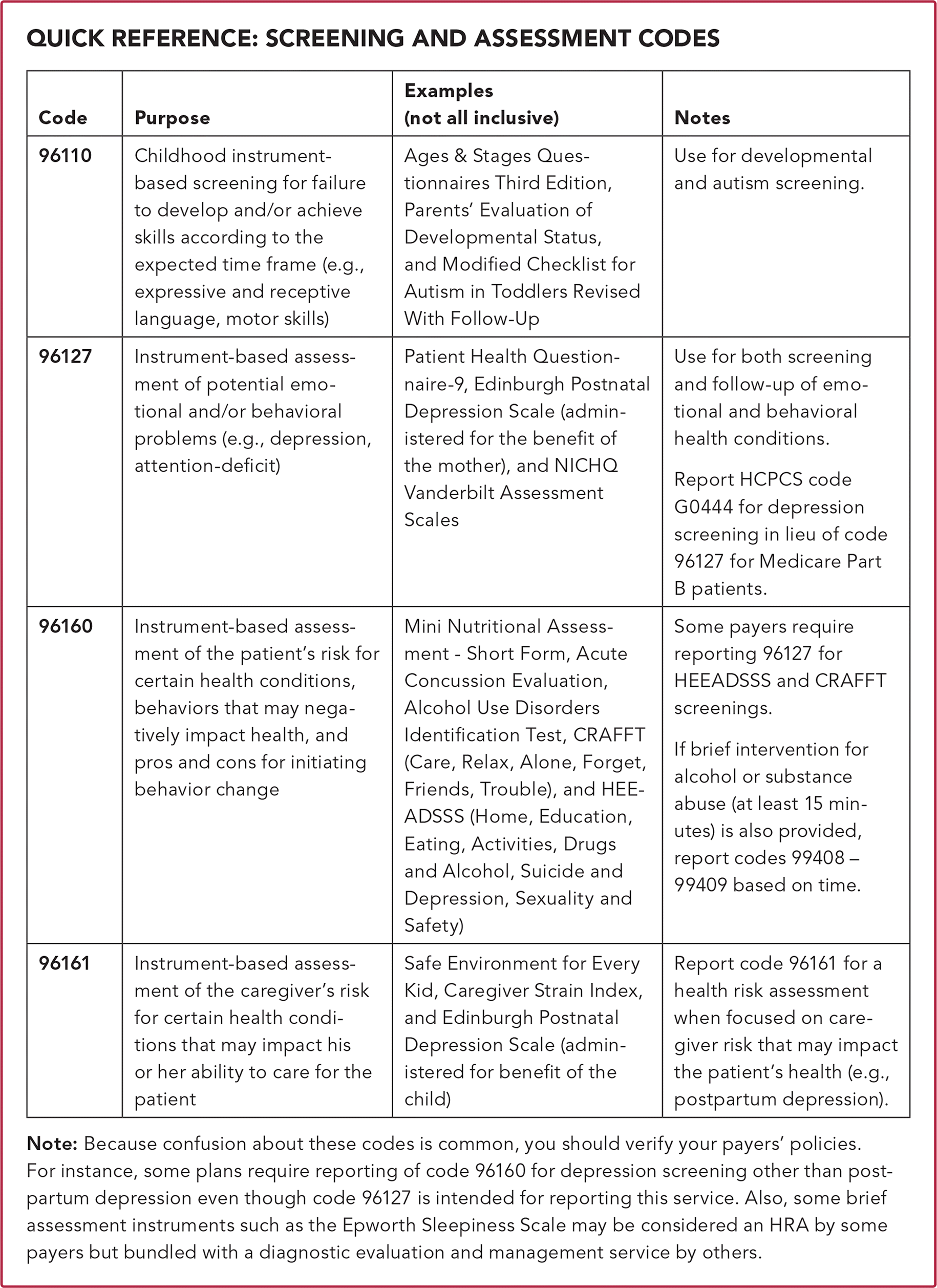
QUICK REFERENCE: SCREENING AND ASSESSMENT CODES
| Code | Purpose | Examples (not all inclusive) | Notes |
|---|---|---|---|
| 96110 | Childhood instrument-based screening for failure to develop and/or achieve skills according to the expected time frame (e.g., expressive and receptive language, motor skills) | Ages & Stages Questionnaires Third Edition, Parents' Evaluation of Developmental Status, and Modified Checklist for Autism in Toddlers Revised With Follow-Up | Use for developmental and autism screening. |
| 96127 | Instrument-based assessment of potential emotional and/or behavioral problems (e.g., depression, attention-deficit) | Patient Health Questionnaire-9, Edinburgh Postnatal Depression Scale (administered for the benefit of the mother), and NICHQ Vanderbilt Assessment Scales | Use for both screening and follow-up of emotional and behavioral health conditions. Report HCPCS code G0444 for depression screening in lieu of code 96127 for Medicare Part B patients. |
| 96160 | Instrument-based assessment of the patient's risk for certain health conditions, behaviors that may negatively impact health, and pros and cons for initiating behavior change | Mini Nutritional Assessment - Short Form, Acute Concussion Evaluation, Alcohol Use Disorders Identification Test, CRAFFT (Care, Relax, Alone, Forget, Friends, Trouble), and HEE-ADSSS (Home, Education, Eating, Activities, Drugs and Alcohol, Suicide and Depression, Sexuality and Safety) | Some payers require reporting 96127 for HEEADSSS and CRAFFT screenings. If brief intervention for alcohol or substance abuse (at least 15 minutes) is also provided, report codes 99408 – 99409 based on time. |
| 96161 | Instrument-based assessment of the caregiver's risk for certain health conditions that may impact his or her ability to care for the patient | Safe Environment for Every Kid, Caregiver Strain Index, and Edinburgh Postnatal Depression Scale (administered for benefit of the child) | Report code 96161 for a health risk assessment when focused on care-giver risk that may impact the patient's health (e.g., postpartum depression). |
Note: Because confusion about these codes is common, you should verify your payers' policies. For instance, some plans require reporting of code 96160 for depression screening other than post-partum depression even though code 96127 is intended for reporting this service. Also, some brief assessment instruments such as the Epworth Sleepiness Scale may be considered an HRA by some payers but bundled with a diagnostic evaluation and management service by others.
Getting paid for screenings and assessments
Although the fee-for-service payment for screening and assessments may be small, it can add up to significant income across a patient panel. In addition, most are recommended preventive services, and some may also be factored into performance ratings and quality initiatives.
Screening and assessment services should be reported unless a payer's written policy restricts doing so. Because most payment policies are regional rather than national and accessible only through secure provider portals, providing a comprehensive list is beyond the scope of this article. It is worth the effort to determine which payers in your area pay for these services. For example, Aetna clearly encourages and pays for depression screening reported with code 96127 and ICD-10 code Z13.89, “Encounter for screening for other disorder.” Cigna has a national policy that provides separate coverage of developmental screening (96110), brief behavioral health assessment (96127), and depression screening reported with HCPCS code G0444.
Payment policies and claims edits are constantly changing and should be systematically monitored. Many payers and clearinghouses offer code edit simulators for use in determining whether codes for services such as screenings and assessments are bundled or separately paid.
Developmental screening
Developmental screening reported with code 96110 is paid for by 45 state Medicaid programs with rates varying from approximately $5 to $60.1 Many private insurers also provide preventive benefits for code 96110 for developmental screening at nine months, 18 months, and 30 months, and autism screening at 18 months and 24 months in addition to the recommended preventive medicine E/M services (e.g., well-child visits). Developmental surveillance without use of a structured screening instrument is included in the preventive medicine service and not separately reported. Most payers allow two “units” (i.e., instruments) per date of service for code 96110.
Developmental screening performed at the time of a well-child exam is reported with ICD-10 codes Z00.121, “Encounter for routine child health examination with abnormal findings,” or Z00.129, “Encounter for routine child health examination without abnormal findings.” If developmental screening is provided at an encounter other than a well-child exam, report code Z13.4, “Encounter for screening for certain developmental disorders in children.” Watch for payer policies that may require reporting of both codes (Z00.121 or Z00.129 and Z13.4) even though ICD-10 indicates separate codes are not required.
Example: An 18-month-old established patient is seen for a well-child exam. Staff administer and score two structured screening instruments for development and autism. The physician completes the age- and gender-appropriate history and exam, including a review of the scores of the screening instruments, and provides counseling/anticipatory guidance and/or identifies the need for diagnostic testing as indicated. The physician reports code 99392 for the preventive service and two units of code 96110 for the administration of the structured screening instruments. No modifier is necessary because the commercial payer does not bundle 96110 with 99392 and allows two units per date of service as the maximum allowable for code 96110. Diagnosis code Z00.129, “Encounter for routine child health examination without abnormal findings,” is linked to each service reported as this code includes an encounter for developmental screening.
Emotional and behavioral health assessments
Depression screening, reported with 96127, is typically a covered preventive service for adolescents age 12 to 18 and is a quality measure in many pediatric quality initiatives. This code may also be reported for depression screening in adult patients other than Medicare beneficiaries. For instance, Aetna has a long-standing policy to cover depression screening in primary care when the service is performed using the Patient Health Questionnaire-9 (PHQ-9) tool and is reported with code 96127.
An annual depression screening of up to 15 minutes is covered for Medicare beneficiaries in primary care settings that have staff-assisted depression care supports in place to assure accurate diagnosis, effective treatment, and follow-up. (For more information, see “Screening Your Adult Patients for Depression,” FPM, March/April 2016.) Code G0444 should be reported to Medicare Part B administrative contractors for this purpose instead of code 96127, and the time spent on screening and discussing results and recommendations should be documented. Depression screening is not separately reported in conjunction with a Medicare initial preventive physical examination (IPPE, “Welcome to Medicare” exam) or an initial Medicare annual wellness visit (AWV).
Payer guidance for reporting postpartum depression screening also varies. Many Medic-aid plans have adopted code 96161 for screening for postpartum depression at well-baby visits (some may allow up to six screenings before the child is 13 months old).
Code 96127 is also applicable to assessments for conditions such as anxiety, attention-deficit disorders, and generalized psychosocial symptoms (e.g., pediatric symptom checklist). Report ICD-10 code Z13.89, “Encounter for screening for other disorder,” in conjunction with depression screening services. Use of structured instruments for assessing attention deficit should be linked to the ICD-10 code for the diagnosis or symptoms that prompted the assessment.
Example A: An adult established patient with opioid addiction, currently in remission, is seen for a routine physical examination. Clinical staff administer and score a structured screening instrument for depression with positive results. The physician provides the age- and gender-appropriate history and examination and briefly discusses the positive depression screening result with the patient. The patient expresses a feeling of hopelessness related to relationships lost during opioid use and sexuality issues. The patient is reluctant to take any medication due to her addiction. The physician recommends a consultation with a psychologist for management of moderate major depression, and a staff member arranges the appointment for later in the week. The physician reports preventive medicine E/M code 99395 with ICD-10 code Z00.01, “Routine adult medical examination with abnormal findings,” and F32.1, “Major depressive disorder, single episode, moderate.” Also reported to the patient's health plan is code 96127 for the depression screening with ICD-10 diagnosis code Z13.89 “Encounter for screening for other disorder.” If a significant, separately identifiable E/M service was rendered for depression or another health problem, an established patient office or other outpatient service code would be separately reported with modifier 25 appended.
Example B: Imagine the same scenario as in example A, but the patient has a different health plan. Because the depression screening does not require an interpretation and report, it is not separately paid by this payer. Only the preventive medicine E/M service code, reported with ICD-10 codes Z00.01, F32.1, and Z13.89, is reimbursed.
Health risk assessment
Medicaid plans often allow payment for adolescent HRAs using tools such as the HEE-ADSSS (Home, Education, Eating, Activities, Drugs, Sexuality, Suicide/Depression, Safety) assessment or the CRAFFT (Care, Relax, Alone, Forget, Friends, Trouble) screening tool. For example, Texas Health Steps pays for adolescent mental health screening using specified structured instruments reported with code 96160 when completed by the patient, and 96161 when completed by a caregiver.
Although an HRA is bundled in the AWV under Medicare Part B, code 96160 may be billed separately in Medicare Advantage plan quality initiatives. For instance, one plan in Tennessee has paid between $150 and $250 for code 96160 when a specific HRA is completed in conjunction with the IPPE or AWV.
ICD-10 codes for routine health examinations (Z00.0-, Z00.1-) should be reported in conjunction with recommended HRAs performed at the same encounter. For assessments of specific risks such as caregiver strain, report code Z13.89.
Modifiers needed
Several scenarios require use of a modifier when billing for screening and assessment services, including the following:
- Modifier 25 may be required to indicate a significant, separately identifiable preventive or other E/M service was provided on the same date.
- Modifier 33 may be required to indicate a service that may be preventive or diagnostic was provided as a preventive service.
- HCPCS modifiers such as modifier EP may be required by Medicaid plans to indicate a service was provided as part of a Medicaid early periodic screening diagnosis and treatment program, or they may require other state-defined modifiers.
- When reporting multiple units of the same or different screening instruments, modifier 59, XE, XP, XS, or XU may be required to indicate distinct services. Be sure that your billing staff is aware of National Correct Coding Initiative and other payer edits that may bundle or limit the units of service for screening and assessment codes. In most cases, modifiers will override the edits when clinically appropriate.
Though screening and assessment services require verification of benefits and of coding and documentation requirements, these services may be beneficial to both the patient and the practice. Collaboration between practice managers, coding and billing staff, and physicians is needed to provide and be appropriately paid for these services.

