As payment models change, diagnosis coding is more important than ever. Here's how to be sure your codes capture your patients' severity of illness.

As family physicians and their employers enter into risk-based contracts with payers and join accountable care organizations (ACOs), they are increasingly finding that payment depends on more than just the CPT and ICD-10 codes in their claims. Patient health status is one of several factors, including cost, utilization, and patient satisfaction, that are driving new models of physician payment. To quantify the severity of illness of patient panels, Hierarchical Condition Category (HCC) codes, long used by the Centers for Medicare & Medicaid Services to predict costs and set Medicare Advantage rates, are finding wider use.
Family physicians do not need to learn all the ins and outs of HCCs. However, understanding a few straightforward concepts and selecting ICD-10 codes that map to HCCs will contribute to a more accurate picture of patient health status and, in a growing number of practice arrangements, have a positive effect on payment.
KEY POINTS
- ICD-10 codes mapped to Hierarchical Condition Category (HCC) codes are used to determine the severity of illness of patient panels.
- New payment models include risk-adjustment factors for patient health status.
- Physicians should report not only the diagnosis codes that describe why a patient was seen but also any diagnosis codes associated with chronic conditions that affect treatment choices.
- Patient risk scores are reset each year, so physicians should comprehensively code chronic conditions at annual visits.
HOW RISK ADJUSTMENT WORKS
First it may be helpful to briefly review the connection between coding, risk adjustment, and payment. Risk-adjustment models assign each patient a risk score based on demographics and health status. Demographic variables may include age, gender, dual Medicare/Medicaid eligibility, whether the patient lives at home or in an institution, and whether the patient has end-stage renal disease. Health status is based on the diagnosis codes submitted on inpatient, outpatient, and professional claims in a calendar year. Certain diagnosis codes map to disease groups (HCCs). Demographics and HCCs are weighted and used to calculate a risk-adjustment factor (RAF) score.
The risk score is reset each contract year for individual patients, and only diagnoses reported within that year are used to calculate the score. Individual claims are paid at the contracted rate, but payers use the group's overall risk score to calculate future payment rates and bonuses. (For more information, see “HCC Coding, Risk Adjustment, and Physician Income: What You Need to Know,” FPM, September/October 2016.)
DIAGNOSIS CODING FOR RISK
Specific and systematic diagnosis coding is the foundation of accurate risk adjustment. There are three key concepts that family physicians need to keep in mind.
1. Select not only the diagnosis codes that describe why the patient was seen but also codes for any chronic conditions that affected treatment choices. Consider these examples:
- A patient with diabetes presents with severe poison ivy. The physician discusses the diabetes with the patient in deciding whether to use prednisone and documents it in the assessment. The physician should report poison ivy first and diabetes second.
- A patient followed by nephrology for chronic kidney disease (CKD) is seen by his family physician for hypertension, which is not well controlled. The physician considers and documents the CKD when selecting hypertension treatment, and should report hypertension first and CKD second.
- A patient with multiple chronic diseases presents for an annual exam. The physician reviews and documents the status of chronic diseases treated within the practice and by other providers.
The physician should document the status of each chronic condition reported. Even if the status hasn't changed, it is important to convey that the code you report is for an active diagnosis.
2. If a patient has a serious chronic condition with a manifestation or complication that has its own code, use that code rather than an unspecified code. For example, you would code “Type 2 diabetes with retinopathy” instead of “Type 2 diabetes, uncomplicated” or “Varicose veins with inflammation or ulcer” rather than “Varicose veins, unspecified.”
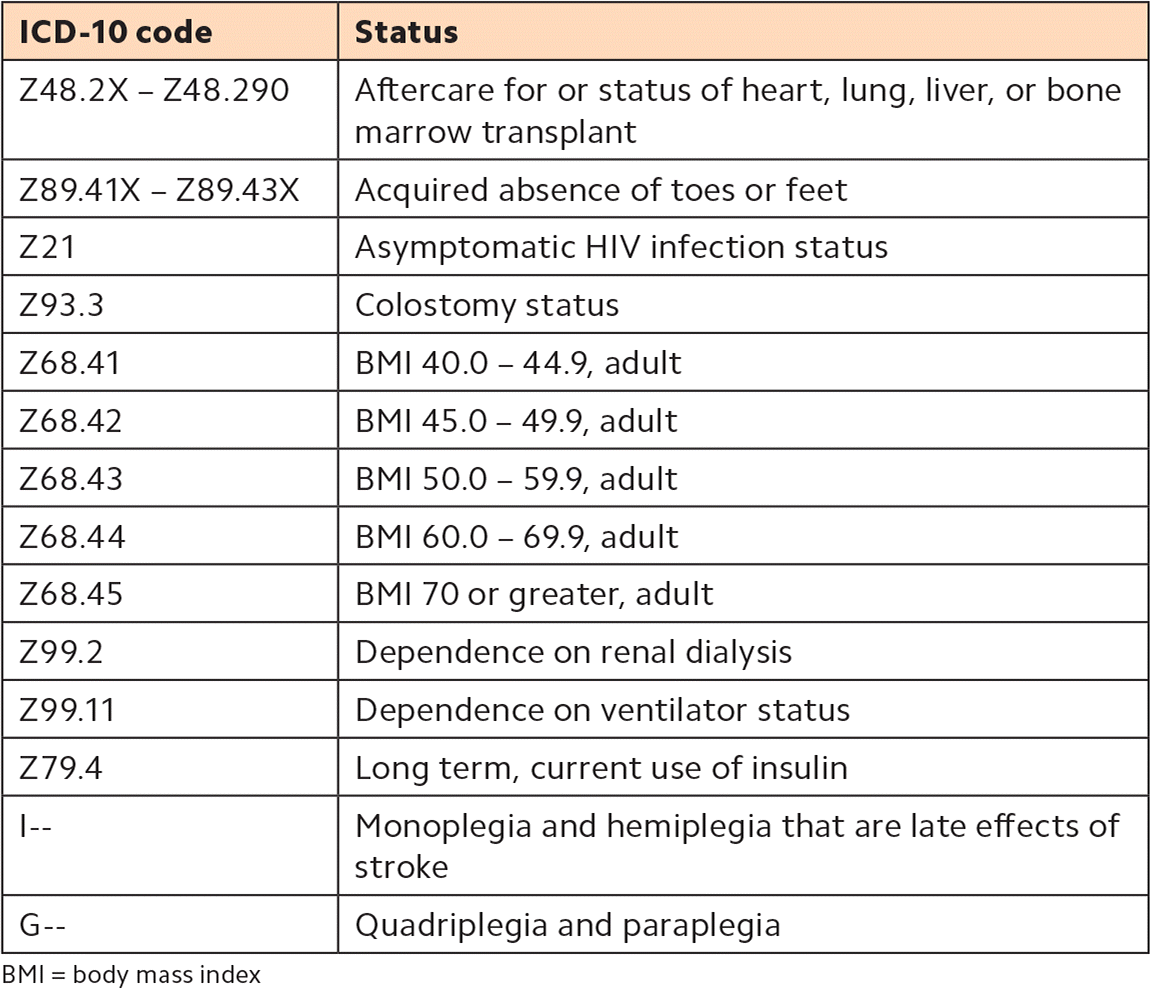
3. Report diagnosis codes annually. Because risk scores reset each year, you must report these diagnoses every year, ideally the first time you see the patient in the calendar year. Note that some “status codes” carry a risk-adjustment factor, or HCC weight, as well. (See “Status codes that contribute to risk scoring.”) Reporting these codes at the patient's annual exam is a good way to make sure they are captured.
STATUS CODES THAT CONTRIBUTE TO RISK SCORES
| ICD-10 code | Status |
|---|---|
| Z48.2X – Z48.290 | Aftercare for or status of heart, lung, liver, or bone marrow transplant |
| Z89.41X – Z89.43X | Acquired absence of toes or feet |
| Z21 | Asymptomatic HIV infection status |
| Z93.3 | Colostomy status |
| Z68.41 | BMI 40.0 – 44.9, adult |
| Z68.42 | BMI 45.0 – 49.9, adult |
| Z68.43 | BMI 50.0 – 59.9, adult |
| Z68.44 | BMI 60.0 – 69.9, adult |
| Z68.45 | BMI 70 or greater, adult |
| Z99.2 | Dependence on renal dialysis |
| Z99.11 | Dependence on ventilator status |
| Z79.4 | Long term, current use of insulin |
| I-- | Monoplegia and hemiplegia that are late effects of stroke |
| G-- | Quadriplegia and paraplegia |
BMI = body mass index
COMMON CONDITIONS AND HOW TO CODE THEM
Family physicians can increase the accuracy of risk-adjustment scoring by focusing on capturing diagnosis codes for the conditions they see frequently. Electronic health record (EHR) systems can help by identifying diagnosis codes that carry an HCC weight, but most do not. A related article in this issue includes a reference tool that physicians can use to keep HCC codes and RAF scoring in mind when selecting diagnosis codes. (See the article “Diagnosis Coding for Value-Based Payment: A Quick Reference Tool.”)
The following examples illustrate how diagnosis coding can affect risk adjustment for patients with diabetes, obesity, depression, and other chronic conditions. Note: All HCC weights are based on community-based, noninstitutionalized, aged patient rates.
Diabetes
Conditions within the same HCC category are counted only once:
ICD-10 code
HCC
HCC weight
Type 2 diabetes with diabetic nephropathy
E11.21
18
0.318
Type 2 diabetes with diabetic peripheral angiopathy without gangrene
E11.51
18
0.318
Total diagnostic risk score
0.318
Note in the following two examples that using a specific code for diabetes complications raises the risk score. The documentation should describe decreased kidney function as well as evidence of kidney damage and the stage of CKD:
ICD-10 code
HCC
HCC weight
CKD, stage 5
N18.5
136
0.237
Type 2 diabetes, uncomplicated
E11.9
19
0.104
BMI 42
Z68.41
22
0.273
Total diagnostic risk score
0.614
CKD, stage 5
N18.5
136
0.237
Type 2 diabetes with diabetic nephropathy
E11.21
18
0.318
BMI 42
Z68.41
22
0.273
Total diagnostic risk score
0.828
Note in the following example how coding for peripheral vascular disease and including a status code for acquired absence of the toe adds significantly to the HCC weight and the risk score. Long-term use of insulin is not credited because there is a diabetes code with a higher score. Document signs and symptoms of peripheral vascular disease, including any abnormal results (from Doppler, ultrasound, computed tomography, and magnetic resonance angiography), decreased peripheral pulses, delayed capillary refill, venous stasis changes, varicose veins, ulcers, claudication, and ankle-brachial index of less than 0.9.
ICD-10 code
HCC
HCC weight
Type 2 diabetes with other circulatory complications
E11.59
18
0.318
Long-term (current) use of insulin
Z79.4
19
0.104
Peripheral vascular disease, unspecified
I73.9
108
0.298
Acquired absence of left great toe
Z89.412
189
0.588
Total diagnostic risk score
1.204
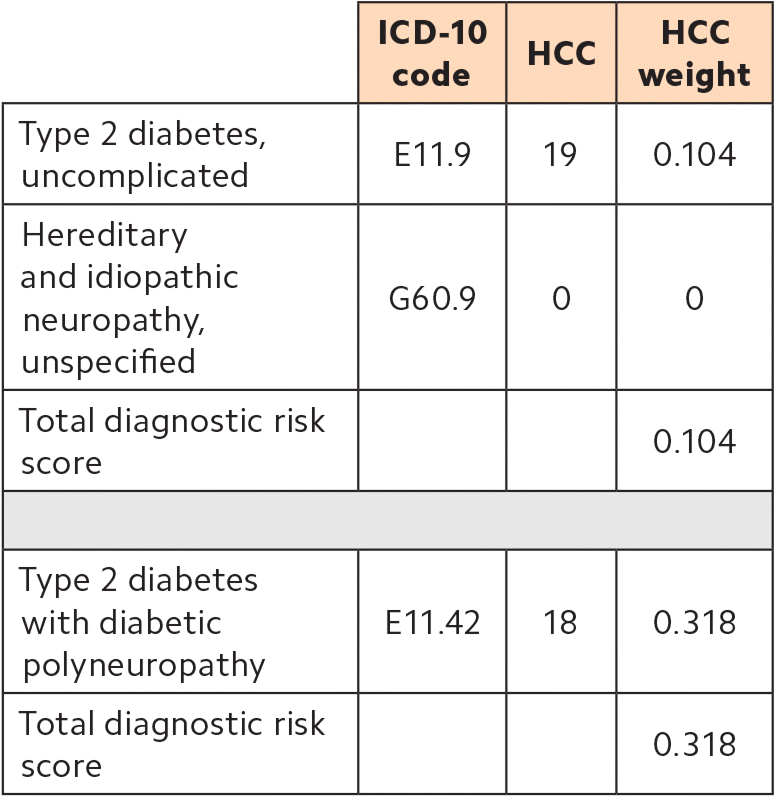
The following example describes two approaches to diagnosis coding for a patient with Type 2 diabetes and related neuropathy. Note that the more specific code E11.42 has a higher risk score. Documentation should include signs and symptoms of neuropathy and neurological exam findings.
| ICD-10 code | HCC | HCC weight | |
|---|---|---|---|
| Type 2 diabetes, uncomplicated | E11.9 | 19 | 0.104 |
| Hereditary and idiopathic neuropathy, unspecified | G60.9 | 0 | 0 |
| Total diagnostic risk score | 0.104 | ||
| Type 2 diabetes with diabetic polyneuropathy | E11.42 | 18 | 0.318 |
| Total diagnostic risk score | 0.318 | ||
- If a patient's A1C is greater than 7 on a recent test, use E11.65, “Type 2 diabetes with hyperglycemia.”
- If a patient's blood glucose is less than 70, use E11.649, “Type 2 diabetes with hypoglycemia.”
- If a patient has diabetes and hyperlipidemia, use E11.69, “Type 2 diabetes with other specified complication.” Add a code for the lipid condition.
Obesity
Code for morbid obesity using E66.01 if a patient's BMI is 35 to 39.9 and the patient has two or more comorbidities, such as hypertension, dyslipidemia, coronary artery disease, chronic obstructive pulmonary disease (COPD), or obstructive sleep apnea:
ICD-10 code
HCC
HCC weight
Morbid obesity due to excess calories
E66.01
22
0.273
Obstructive sleep apnea
G47.33
0
0
COPD
J44.9
111
0.328
Total diagnostic risk score
0.601
Depression
Depression is one of the most frequently reported diagnoses in family medicine, and the most frequently reported depression code is F32.9, “Major depressive disorder, single episode, unspecified.” In many EHR systems, this is listed simply as “depression” or “primary depression.” However, code F32.9 does not map to an HCC code, so it does not contribute to risk scoring. More specific depression codes do. Codes in the range F32.0 – F32.5, any code from category F33, “Major depressive disorder, recurrent,” and all codes in category F31, “Bipolar disorder,” have an HCC weight and factor into risk-adjustment scores. The following examples show two approaches to diagnosis coding for a patient with a long history of depression who presents with moderate exacerbation and whose medication list includes an antidepressant:
ICD-10 code
HCC
HCC weight
Depression (major depressive disorder, single episode, unspecified)
F32.9
0
0
Total diagnostic risk score
0
Major depressive disorder, recurrent, moderate
F33.1
58
0.395
Total diagnostic risk score
0.395
Other chronic conditions
Chronic conditions with complications typically have a higher HCC weight than chronic conditions without complications. In some instances, the chronic condition without a complication does not have an HCC weight:
ICD-10 code
HCC
HCC weight
Atherosclerotic heart disease of native coronary artery without angina pectoris
I25.10
0
0
Atherosclerotic heart disease of native coronary artery with angina pectoris with documented spasm
I25.111
88
0.140
However, it is important to remember that the unspecified codes for some chronic conditions do have HCC weights:
ICD-10 code
HCC
HCC weight
All conditions for congestive heart failure
I50.-
85
0.323
All conditions for COPD
J44.-
111
0.328
The following example describes diagnoses for a patient seen for a prothrombin time and international normalized ratio check. Long-term use of anticoagulants is not weighted for risk-adjustment, but atrial fibrillation is:
ICD-10 code
HCC
HCC weight
Long-term use of anticoagulants
Z79.01
0
0
Personal history of pulmonary embolism
Z86.711
0
0
Chronic atrial fibrillation
I48.2
96
0.268
BARRIERS AND FINANCIAL IMPLICATIONS
Accurate diagnosis coding can be thwarted by incorrect or abbreviated code descriptions in the EHR. Physicians may not have access to the complete code description without leaving the EHR program and opening another window – which slows down completion of the chart. Numerous mobile apps can provide ICD-10 codes if needed. Some software programs may limit the number of codes submitted on a claim. In that case, be sure to list the HCC-weighted codes first.
Diagnosis coding that is informed by an awareness of HCC codes and risk adjustment will benefit medical practices that are part of an ACO, an alternative payment model, or other risk-based arrangement, as their payment is adjusted in future contract years.

