Using these brief interventions, you can help your patients make healthy behavior changes.

Effectively encouraging patients to change their health behavior is a critical skill for primary care physicians. Modifiable health behaviors contribute to an estimated 40 percent of deaths in the United States.1 Tobacco use, poor diet, physical inactivity, poor sleep, poor adherence to medication, and similar behaviors are prevalent and can diminish the quality and length of patients' lives. Research has found an inverse relationship between the risk of all-cause mortality and the number of healthy lifestyle behaviors a patient follows.2
Family physicians regularly encounter patients who engage in unhealthy behaviors; evidence-based interventions may help patients succeed in making lasting changes. This article will describe brief, evidence-based techniques that family physicians can use to help patients make selected health behavior changes. (See “Brief evidence-based interventions for health behavior change.”)
KEY POINTS
- Modifiable health behaviors, such as poor diet or smoking, are significant contributors to poor outcomes.
- Family physicians can use brief, evidence-based techniques to encourage patients to change their unhealthy behaviors.
- Working with patients to develop health goals, eliminate barriers, and track their own behavior can be beneficial.
- Interventions that target specific behaviors, such as prescribing physical activity for patients who don't get enough exercise or providing patient education for better medication adherence, can help patients to improve their health.
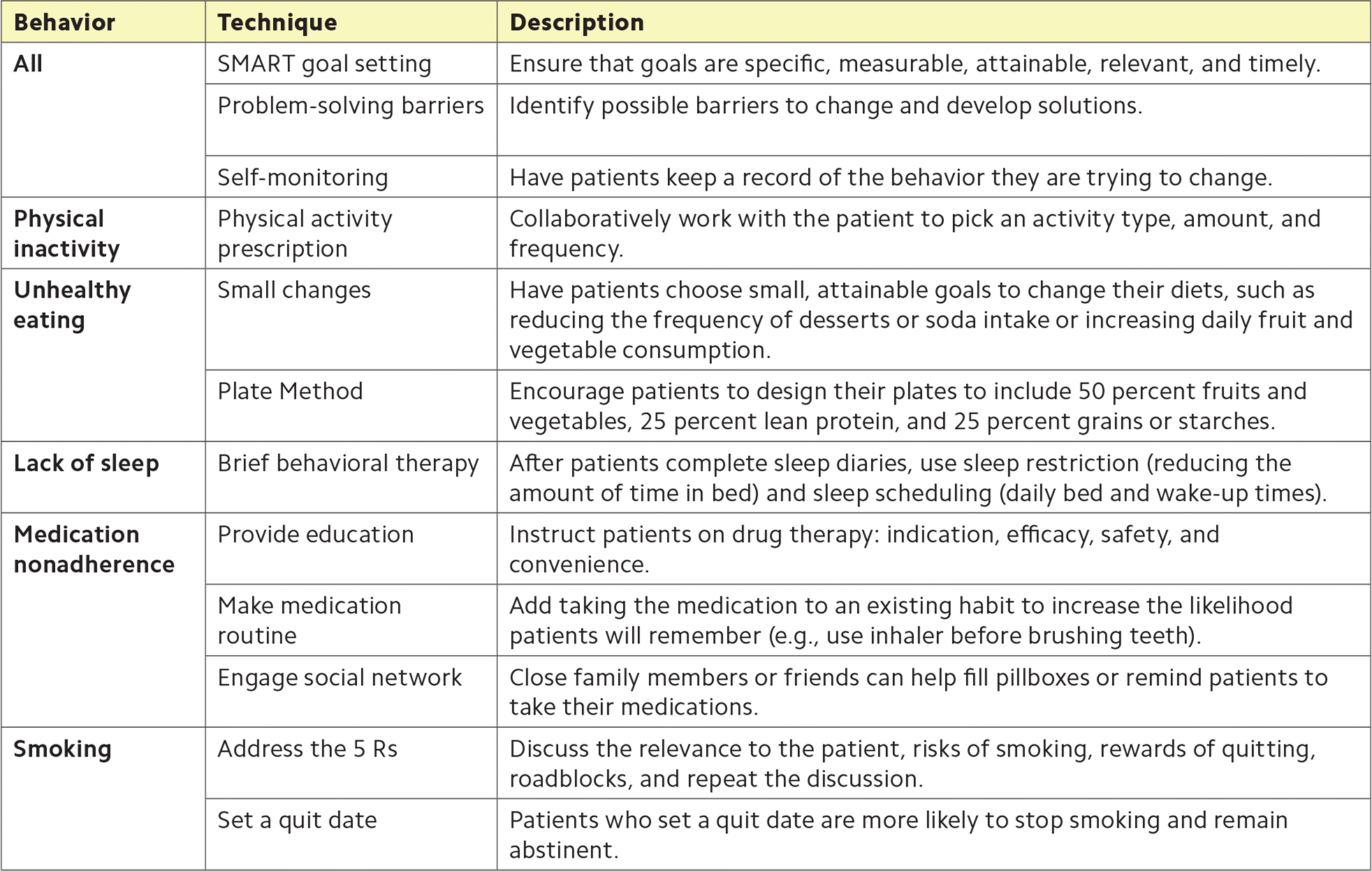
BRIEF EVIDENCE-BASED INTERVENTIONS FOR HEALTH BEHAVIOR CHANGE
| Behavior | Technique | Description |
|---|---|---|
| All | SMART goal setting | Ensure that goals are specific, measurable, attainable, relevant, and timely. |
| Problem-solving barriers | Identify possible barriers to change and develop solutions. | |
| Self-monitoring | Have patients keep a record of the behavior they are trying to change. | |
| Physical inactivity | Physical activity prescription | Collaboratively work with the patient to pick an activity type, amount, and frequency. |
| Unhealthy eating | Small changes | Have patients choose small, attainable goals to change their diets, such as reducing the frequency of desserts or soda intake or increasing daily fruit and vegetable consumption. |
| Plate Method | Encourage patients to design their plates to include 50 percent fruits and vegetables, 25 percent lean protein, and 25 percent grains or starches. | |
| Lack of sleep | Brief behavioral therapy | After patients complete sleep diaries, use sleep restriction (reducing the amount of time in bed) and sleep scheduling (daily bed and wake-up times). |
| Medication nonadherence | Provide education | Instruct patients on drug therapy: indication, efficacy, safety, and convenience. |
| Make medication routine | Add taking the medication to an existing habit to increase the likelihood patients will remember (e.g., use inhaler before brushing teeth). | |
| Engage social network | Close family members or friends can help fill pillboxes or remind patients to take their medications. | |
| Smoking | Address the 5 Rs | Discuss the relevance to the patient, risks of smoking, rewards of quitting, roadblocks, and repeat the discussion. |
| Set a quit date | Patients who set a quit date are more likely to stop smoking and remain abstinent. |
CROSS-BEHAVIOR TECHNIQUES
Although many interventions target specific behaviors, three techniques can be useful across a variety of behavioral change endeavors.
“SMART” goal setting. Goal setting is a key intervention for patients looking to make behavioral changes.3 Helping patients visualize what they need to do to reach their goals may make it more likely that they will succeed. The acronym SMART can be used to guide patients through the goal-setting process:
- Specific. Encourage patients to get as specific as possible about their goals. If patients want to be more active or lose weight, how active do they want to be and how much weight do they want to lose?
- Measurable. Ensure that the goal is measurable. For how many minutes will they exercise and how many times a week?
- Attainable. Make sure patients can reasonably reach their goals. If patients commit to going to the gym daily, how realistic is this goal given their schedule? What would be a more attainable goal?
- Relevant. Ensure that the goal is relevant to the patient. Why does the person want to make this change? How will this change improve his or her life?
- Timely. Help patients define a specific timeline for the goal. When do they want to reach their goal? When will you follow-up with them? Proximal, rather than distal, goals are preferred. Helping patients set a goal to lose five pounds in the next month may feel less overwhelming than a goal of losing 50 pounds in the next year.
Problem-solving barriers. Physicians may eagerly talk with patients about making changes — only to become disillusioned when patients do not follow through. Both physicians and patients may grow frustrated and less motivated to work on the problem. One way to prevent this common phenomenon and set patients up for success is to brainstorm possible obstacles to behavior change during visits.
After offering a suggestion or co-creating a plan, physicians can ask simple, respectful questions such as, “What might get in the way of your [insert behavior change]?” or “What might make it hard to [insert specific step]?” Physicians may anticipate some common barriers raised by patients but be surprised by others. Once the barriers are defined, the physician and patient can develop potential solutions, or if a particular barrier cannot be overcome, reevaluate or change the goal. This approach can improve clinical outcomes for numerous medical conditions and for patients of various income levels.4
For example, a patient wanting to lose weight may commit to regular short walks around the block. Upon further discussion, the patient shares that the cold Minnesota winters and the violence in her neighborhood make walking in her area difficult. The physician and patient may consider other options such as walking around a local mall or walking with a family member instead. Anticipating every barrier may be impossible, and the problem-solving process may unfold over several sessions; however, exploring potential challenges during the initial goal setting can be helpful.
Self-monitoring. Another effective strategy for facilitating a variety of behavioral changes involves self-monitoring, defined as regularly tracking some specific element of behavior (e.g., minutes of exercise, number of cigarettes smoked) or a more distal outcome (e.g., weight). Having patients keep diaries of their behavior over a short period rather than asking them to remember it at a visit can provide more accurate and valuable data, as well as provide a baseline from which to track change.
When patients agree to self-monitor their behavior, physicians can increase the chance of success by discussing the specifics of the plan. For example, at what time of day will the patient log his or her behavior? How will the patient remember to observe and record the behavior? What will the patient write on the log? Logging the behavior soon after it occurs will provide the most accurate data. Although patients may be tempted to omit unhealthy behaviors or exaggerate healthy ones, physicians should encourage patients to be completely honest to maximize their records' usefulness. For self-monitoring to be most effective, physicians should ask patients to bring their tracking forms to follow-up visits, review them together, celebrate successes, discuss challenges, and co-create plans for next steps. (Several diary forms are available in the Patient Handouts section of the FPM Toolbox.)
A variety of digital tracking tools exist, including online programs, smart-phone apps, and smart-watch functions. Physicians can help patients select which method is most convenient for daily use. Most online programs can present data in charts or graphs, allowing patients and physicians to easily track change over time. SuperTracker, a free online program created by the U.S. Department of Agriculture, helps patients track nutrition and physical activity plans, set goals, and work with a group leader or coach. Apps like Lose It! or MyFitnessPal can also help.
The process of consistently tracking one's behavior is sometimes an intervention itself, with patients often sharing that it created self-reflection and resulted in some changes. Research shows self-monitoring is effective across several health behaviors, especially using food intake monitoring to produce weight loss.5
BEHAVIOR-SPECIFIC TECHNIQUES
The following evidence-based approaches can be useful in encouraging patients to adopt specific health behaviors.
Physical activity prescriptions. Many Americans do not engage in the recommended amounts of physical activity, which can affect their physical and psychological health. Physicians, however, rarely discuss physical activity with their patients.6 Clinicians ought to act as guides and work with patients to develop personalized physical activity prescriptions, which have the potential to increase patients' activity levels.7 These prescriptions should list creative options for exercise based on the patient's experiences, strengths, values, and goals and be adapted to a patient's condition and treatment goals over time. For example, a physician working with a patient who has asthma could prescribe tai chi to help the patient with breathing control as well as balance and anxiety.
In creating these prescriptions, physicians should help the patient recognize the personal benefits of physical activity; identify barriers to physical activity and how to overcome them; set small, achievable goals; and give patients the confidence to attempt their chosen activity. Physicians should also put the prescriptions in writing, give patients logs to track their activity, and ask them to bring those logs to follow-up appointments for further discussion and coaching.8 More information about exercise prescriptions and sample forms are available online.
Healthy eating goals. Persuading patients to change their diets is daunting enough without unrealistic expectations and the constant bombardment of fad diets, cleanses, fasts, and other food trends that often leave both patients and physicians uncertain about which food options are actually healthy. Moreover, physicians in training receive little instruction on what constitutes sound eating advice and ideal nutrition.9 This confusion can prevent physicians from broaching the topic with patients. Even if they identify healthy options, common setbacks can leave both patients and physicians less motivated to readdress the issue. However, physicians can help patients set realistic healthy eating goals using two simple methods:
- Small steps. Studies have shown that one way to combat the inertia of unhealthy eating is to help patients commit to small, actionable, and measurable steps.10 First, ask the patient what small change he or she would like to make — for example, decrease the number of desserts per week by one, eat one more fruit or vegetable serving per day, or swap one fast food meal per week with a homemade sandwich or salad.11 Agree on these small changes to empower patients to take control of their diets.
- The Plate Method. This model of meal design encourages patients to visualize their plates split into the following components: 50 percent fruits and non-starchy vegetables, 25 percent protein, and 25 percent grains or starchy foods.12 Discuss healthy options that would fit in each of the categories, or combine this method with the small steps described above. By providing a standard approach that patients can adapt to many forms of cuisine, the model helps physicians empower their patients to assess their food options and adopt healthy eating behaviors.
Brief behavioral therapy for insomnia. Many adults struggle with insufficient or unrestful sleep, and approximately 18.8 percent of adults in the United States meet the criteria for an insomnia disorder.13 The first-line treatment for insomnia is Cognitive Behavioral Therapy for Insomnia (CBT-I), which involves changing patients' behaviors and thoughts related to their sleep and is delivered by a trained mental health professional. A physician in a clinic visit can easily administer shorter versions of CBT-I, such as Brief Behavioral Therapy for Insomnia (BBT-I).14 BBT-I is a structured therapy that includes restricting the amount of time spent in bed but not asleep and maintaining a regular sleep schedule from night to night. Here's how it works:
- Sleep diary. Have patients maintain a sleep diary for two weeks before starting the treatment. Patients should track when they got in bed, how long it took to fall asleep, how frequently they woke up and for how long, what time they woke up for the day, and what time they got out of bed. Many different sleep diaries exist, but the American Academy of Sleep Medicine's version is especially user-friendly.
- Education. In the next clinic appointment, briefly explain how the body regulates sleep. This includes the sleep drive (how the pressure to sleep is based on how long the person has been awake) and circadian rhythms (the 24-hour biological clock that regulates the sleep-wake cycle).
- Set a wake-up time. Have patients pick a wake-up time that will work for them every day. Encourage them to set an alarm for that time and get up at that time every day, no matter how the previous night went.
- Limit “total time in bed.” Review the patient's sleep diary and calculate the average number of hours per night the patient slept in the past two weeks. Add 30 minutes to that average and explain that the patient should be in bed only for that amount of time per night until your next appointment.
- Set a target bedtime. Subtract the total time in bed from the chosen wake-up time, and encourage patients to go to bed at that “target” time only if they are sleepy and definitely not any earlier.
For example, if a patient brings in a sleep diary with an average of six hours of sleep per night for the past two weeks, her recommended total time in bed will be 6.5 hours. If she picks a wake-up time of 7 a.m., her target bedtime would be 12:30 a.m. It usually takes up to three weeks of regular sleep scheduling and sleep restriction for patients to start seeing improvements in their sleep. As patients' sleep routines become more solid (i.e., they are falling asleep quickly and sleeping more than 90 percent of the time they are in bed), slowly increase the total time in bed to possibly increase time asleep. Physicians should encourage patients to increase time in bed in increments of 15 to 30 minutes per week until the ideal amount of sleep is reached. This amount is different for each patient, but patients generally have reached their ideal amount of sleep when they are sleeping more than 85 percent of the time in bed and feel rested during the day.
Patient education to prevent medication nonadherence. Medication adherence can be challenging for many patients. In fact, approximately 20 percent to 30 percent of prescriptions are never picked up from the pharmacy, and 50 percent of medications for chronic diseases are not taken as prescribed.15 Nonadherence is associated with poor therapeutic outcomes, further progression of disease, and decreased quality of life. To help patients improve medication adherence, physicians must determine the reason for nonadherence. The most common reasons are forgetfulness, fear of side effects, high drug costs, and a perceived lack of efficacy. To help patients change these beliefs, physicians can take several steps:
- Educate patients on four key aspects of drug therapy — the reason for taking it (indication), what they should expect (efficacy), side effects and interactions (safety), and how it structurally and financially fits into their lifestyle (convenience).16
- Help patients make taking their medication a routine of their daily life. For example, if a patient needs to use a controller inhaler twice daily, recommend using the inhaler before brushing his or her teeth each morning and night. Ask patients to describe their day, including morning routines, work hours, and other responsibilities to find optimal opportunities to integrate this new behavior.
- Ask patients, “Who can help you manage your medications?” Social networks, including family members or close friends, can help patients set up pillboxes or provide medication reminders.
The five Rs to quitting smoking. Despite the well-known consequences of smoking and nationwide efforts to reduce smoking rates, approximately 15 percent of U.S. adults still smoke cigarettes.17 As with all kinds of behavioral change, patients present in different stages of readiness to quit smoking. Motivational interviewing techniques can be useful to explore a patient's ambivalence in a way that respects his or her autonomy and bolsters self-efficacy. Discussing the five Rs is a helpful approach for exploring ambivalence with patients:18
- Relevance. Explore why quitting smoking is personally relevant to the patient.
- Risks. Advise the patient on negative consequences of continuing to smoke.
- Rewards. Ask the patient to identify the benefits of quitting smoking.
- Roadblocks. Help the patient determine obstacles he or she may face when quitting. Common barriers include weight gain, stress, fear of withdrawal, fear of failure, and having other smokers such as coworkers or family in close proximity.
- Repeat. Incorporate these aspects into each clinical contact with the patient.
Many patients opt to cut back on the amount of tobacco they use before their quit date. However, research shows that cutting back on the number of cigarettes is no more effective than quitting abruptly, and setting a quit date is associated with greater long-term success.19
Once the patient sets a quit date, repeated physician contact to reinforce smoking cessation messages is key. Physicians, care coordinators, or clinical staff should consider calling or seeing the patient within one to three days of the quit date to encourage continued efforts to quit, as this time period has the highest risk for relapse. Evidence shows that contacting the patient four or more times increases the success rate in staying abstinent.18 Quitting for good may take multiple a empts, but continued encouragement and efforts such as setting new quit dates or offering other pharmacologic and behavioral therapies can be helpful.
GETTING STARTED
Family physicians are uniquely positioned to provide encouragement and evidence-based advice to patients to change unhealthy behaviors. The proven techniques described in this article are brief enough to attempt during clinic visits. They can be used to encourage physical activity, healthy eating, better sleep, medication adherence, and smoking cessation, and they can help patients adjust their lifestyle, improve their quality of life, and, ultimately, lower their risk of early mortality.

